Trauma Cases and Reviews
Algorithms of Flap Reconstruction in High-Voltage Electrical Injuries: 26 Years Experience
Cengiz Eser1*, Erol Kesiktas1, Eyuphan Gencel1, Omer Kokacya1, Metin Yavuz1 and Rauf Kerimov2
1Cukurova University Medical Faculty Plastic Reconstructive and Aesthetic Surgery, Turkey
2Central Hospital of Oil workers Plastic Surgery Clinic, Turkey
*Corresponding author: Cengiz Eser, Assistant Professor, Cukurova University, Medical Faculty, Plastic Reconstructive and Aesthetic Surgery Clinic, Adana, Turkey, Tel: 00905323163317, Email: cengizeser01@gmail.com
Trauma Cases Rev, TCR-1-001, (Volume 1, Issue 1), Research Article; ISSN: 2469-5777
Received: February 16, 2015 | Accepted: April 28, 2015 | Published: May 02, 2015
Citation: Eser C, Kesiktas E, Gencel E, Kokacya O, Yavuz M, et al. (2015) Algorithms of Flap Reconstruction in High-Voltage Electrical Injuries: 26 Years Experience. Trauma Cases Rev 1:001. 10.23937/2469-5777/1510001
Copyright: © 2015 Eser C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Electricity is an indispensable part of a comfortable modern life. However, multipurpose electricity use in daily life increases the risks of accidents, injury or death. High-voltage (>1000 volts) electrical burns cause the greatest tissue damage and sequelae, as well as the largest number of deaths. To minimize the functional effects caused by delayed recovery, reconstruction with skin flaps or grafts should be performed as soon as possible in a High-voltage Electrical Injury (HVEI). This study presents 156 flaps that were performed in 117 patients hospitalized with HVEI in the Cukurova University Burn Unit /Adana/Turkey between 1988 and 2014. The flap reconstruction algorithms that we suggested might help plastic surgeons perform interventions in HVEI patients that are more rapid and effective.
Introduction
Electricity is an indispensable component of comfortable modern life. Multipurpose electricity use in daily life increases the number of accidents and the risk of injury or death. The first death secondary to electricity contact occurred in 1879; since then, these injuries have gradually increased. Today, they play a role in the most devastating traumas [1].
Electrical current is delivered as high voltage (>1000 volts) or as residential voltage (220-380 volts). High-voltage electrical burns cause the greatest tissue damage and sequelae, as well as the largest number of deaths [2,3]. Functional disorders, amputations and other burn-related complications might occur because of this type of injury. To minimize the functional effects caused by delayed recovery, reconstruction with skin flaps or grafts should be performed as soon as possible in such injuries [4].
The purpose of this study is to demonstrate early (as soon as possible) debridement and reconstruction of extensive defects (secondary to a high-voltage electrical injury [HVEI] in which vital tissues are exposed) with a reliable and well-vascularized flap and to suggest a flap selection algorithm, according to the anatomical region.
This study presents 156 flaps performed in 117 patients hospitalized for HVEI in our burn unit from 1988 to 2014. The suggested reconstructive algorithms, which included all the body, might help plastic surgeons perform interventions in HVEI patients that are more rapid and effective.
Materials and methods
The study protocol was approved by the Cukurova University Research Ethics Board. One hundred and fifty six flap reconstructions performed on 117 HVEI patients hospitalized in the Cukurova University Burn Unit/Adana/Turkey from 1988 to 2014 were retrospectively analyzed. Major causes of electrical burns in present patient population were illegal usage of electricity and industrial accidents.
During each emergency evaluation, reliable vascular access, urinary catheterization, cardiac monitoring, and an advanced trauma life support algorithm were applied to all patients. In particular, patients with a history of fall from height were examined for accompanying traumas. Further examinations and treatments were performed on these patients, as necessary. Urgent fasciotomy/escharotomy (F/E) was performed for the existence or suspicion of a compartment syndrome. After the initial intervention, fluid resuscitation was started, according to the Parkland formula, to replace fluid loss and prevent hypovolemic shock. The patients were then transported to the burn unit. Debridement was performed on alternate days, as necessary. We protected vital structures, such as tendons, vessels, nerves, bones and joints, during debridement. Amputations were performed from the distal level (if possible) to conserve functionality. Lesions not necessitating amputations were closed with reliable and proper flaps soon after debridement.
The anatomical regions that we reconstructed were categorized as head and neck (21 patients, 21 flaps), upper extremity (66 patients, 103 flaps), lower extremity (28 patients, 30 flaps) or perineal region (2 patients, 2 flaps). The patients were analyzed for gender, age, total burned surface area (TBSA), length of hospital stay, accompanying traumas, F/E practice, flap types, complications and amputations. After these analyses, we aimed to algorithms for flap choices, according to the anatomical region of the injury.
Results
This study presents 156 flaps that were performed in 98 males [83.8%] and 19 females [16.2%]. Mean age of the patients was 26.7 (from 1 to 64 years). In all cases, the burn depths were second and third degree, and the TBSA ranged between 3% and 44% (mean, 15%). The hospital stays ranged from 7 to 110 days (mean, 59.3 days). In the initial emergency room (ER) evaluations, eight patients were diagnosed with head trauma, 2 with extremity fracture and 4 with vertebral trauma. Of the 117 patients, 62 (53%) received an urgent fasciotomy or escharotomy of one or more extremities.
Table 1 shows the total number of patients treated and the flap reconstructions performed.
![]()
Table 1: Flap types, according to the reconstructed regions and the number and percentage of flaps
View Table 1
We encountered 33 (21.2%) complications in 156 flaps. The flap types and complications are shown in Table 2.
![]()
Table 2: Complications according to flap types
View Table 2
Discussion
Electrical burns constitute 3-5% of all burns and are traumas with severe morbidity and mortality rates [1-3,5-7]. Previous studies report that the majority of HVEI patients are young males, with a hospital stay of 30 to 40 days and a mean TBSA of approximately 20% [2,8,9]. In our study, 83.7% of the patients were male, and the mean age was 26.7 years; the mean hospital stay was 59.3 days. Our relatively long hospital stay may have resulted from hospitalizing the patients until full recovery.
Mann et al. [10] and Nafs et al. [11] reported 19.3% and 7%, respectively, co-occurrence of head trauma and various fractures in electrical injury patients. In our series, 6.8% (n=8) of the patients were diagnosed with head trauma, 1.7% (n=2) had extremity fractures, and 3.4% (n=4) had vertebra fractures. Accompanying trauma was observed in 11.9% (n=14) of our cases. Therefore, a multi-clinical approach should be considered for HVEI patients.
The F/E ratio in electrical burn injury ranges between 9.2% and 54% in the literature [6]. In our study, the F/E ratio in HVEI patients was 53%. This high ratio may have resulted from our low F/E threshold. When HVEI defect reconstruction is performed using flaps, the aesthetic and functional results may be improved compared to other treatments and might prevent amputations and complications [12,13].
Upper extremity reconstructions in HVEI
There are numerous flap options for the reconstruction of finger defects resulting from HVEI. V-Y advancement flaps cannot be used for defects larger than 1.5cm [14]. Abdominal perforator flaps have unsatisfactory aesthetic and functional outcomes [15,16]. A Reverse Dorsal Metacarpal Artery Flap (RDMA) is a convenient flap for finger defects; however, it has a risk of distal flap necrosis and low sensation [17]. Adipofascial turnover flaps can be used for medium-sized defects [18]. Cross-finger flaps can be used for dorsal and volar defects [19]. A Superficial External Pudendal Artery (SEPA) flap can maintain the hand in a more neutral position than a groin flap; however, the aesthetic result might be unsatisfactory [20]. As experience in free flap surgery and practice in burn patients increases, free flaps from the foot to hand are being widely used.
In our study, a finger defect was treated with a reverse dorsal metacarpal artery (RDMA) flap in two patients, and two patients with finger defects were treated with a cross-finger flap. One patient with damaged surrounding tissue and a wide defect at the first finger was treated with a SEPA flap. The aesthetic and functional results were reasonable in these 5 patients. Two-stage reconstructions were performed, except for RDMA flaps. The RDMA flap is considered a convenient flap for this region. The algorithm that we constructed for finger defects (based on these findings) is shown in Table 3.
![]()
Table 3: Algorithm of finger defects in HVEI patients
View Table 3
Local random fasciocutaneous flaps are insufficient for reconstructing large hand and wrist defects in HVEI patients. There are many distant flap reconstruction options in these regions. The most preferred options are groin and Tensor Fascia Lata (TFL) flaps. Groin and TFL flaps can be harvested with larger dimensions, and the arc of rotation secures the proper angle for many defects [21,22]. A reverse radial or ulnar forearm flap necessitates sacrificing a major artery. A reverse posterior interosseous artery flap has a risk of perfusion in the distal part [23]. Sub mammary flaps and intercostal artery perforator flaps result in severe scarring at the thorax or abdomen [24]. Abdominal fasciocutaneous or perforator flaps were previously mentioned in the finger reconstruction section.
There are numerous flaps for forearm and cubital region reconstruction; their advantages and disadvantages depend on the various flaps. Distal necrosis can occur in lateral and medial arm flaps [25,26]. Intercostal artery pedicle flaps and submammary flaps result in large scars at the donor areas [24]. For large upper extremity defects, a rectus abdominis flap can be used alone or in combination with an inguinal flap [27]. Additionally, pedicled or free Latissimus Dorsi (LD) muscle or musculocutaneous flaps can be used in the reconstruction of the cubital region as a functional transfer [28]. When selecting a flap (pedicle or free), it is important that the pedicle is away from the injury zone [22]. Rectus abdominis, LD and Anterolateral Thigh (ALT) flaps are frequently used in reconstruction of the cubital region [29,30].
Another important issue in cubital defects secondary to HVEI is impairment in the continuity of the brachial artery and the loss of soft tissue coverage over the artery. A saphenous vein interposition graft is one of the most commonly used techniques for repairing a brachial artery. Well-vascularized muscle or musculo cutaneous flaps can be used to cover the graft. For composite defects of the cubital region, when the brachial artery is affected, flow-through free flaps can be used to restore vascular continuity and soft tissue deficiency.
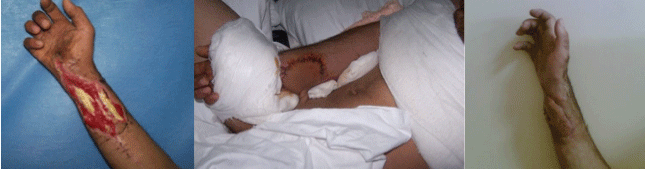
In our study, if the forearm region was intact, local fasciocutaneous flaps or adipofascial turnover flaps were used for the hand and wrist reconstruction. If the forearm was injured and the groin region was intact, a groin flap was used (Figure 1). If the groin region was also injured, then a submammary flap was used. For a patient with a radial and ulnar artery injury, a wrist defect was repaired with a flow-through free LD flap. In one patient with bilateral wrist defects and groin injuries, both wrist defects were reconstructed with a pedicled rectus abdominis myocutaneous flap that was prepared in a �y� shape.
.
Figure 1: A patient with a right wrist defect from a HVEI (left). Groin flap reconstruction of the defect (middle). Postoperative view of the right wrist (right).
View Figure 1
Of the 8 patients with large defects at the cubital region and whose brachial arteries were exposed, 2 were treated with local fasciocutaneous flaps. Four of the patients with inadequate healthy surrounding tissue and severe loss of the biceps brachii muscles received reconstruction with pedicled LD muscle flaps to the mimic biceps brachii muscle. The remaining 2 patients with inadequate healthy surrounding tissue, whose brachial arteries were defective and who had severe loss of the biceps brachii muscle, received reconstruction with saphenous vein interposition grafts (for brachial artery defect repair), and pedicled LD myocutaneous flaps were used to cover the vein grafts and restore forearm flexion.
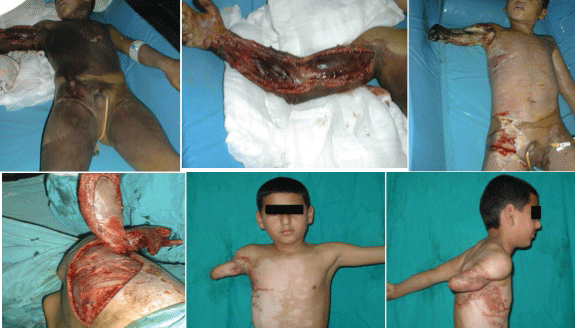
In 12 HVEI patients who required shoulder disarticulation with subtotal necrosis of the upper extremity, a trans-humeral bone stump that can host a functional prosthesis was preserved and salvaged by wrapping with a pedicle LD flap to maintain the shoulder joint (Figure 2).
.
Figure 2: A child burned by high-voltage electricity (upper left). The affected upper extremity after a fasciotomy (upper-middle). The amputated right arm (upper right). The harvested latissimus dorsi muscle for trans-humeral amputation stump coverage (lower left). One-year postoperative anterior view (lower-middle) and lateral view (lower-right).
View Figure 2
In our study, a groin flap was most frequently used in upper extremity reconstructions (n=55, 35.3%). A groin flap is easily prepared, of sufficient size, and has hairless skin; in addition, patient mobility can be restored, and joint exercises can begin in the early postoperative period. The donor area scar can be hidden by clothes and a groin flap enables further nerve or tendon repairs.
An algorithm for hand and wrist reconstruction and cubital defects from an HVEI is shown in Tables 4 and 5.
![]()
Table 4: Algorithm of hand and wrist defects in HVEI patients
View Table 4
![]()
Table 5: Algorithm of cubital defects in HVEI patients
View Table 5
Scalp reconstructions in HVEI
Whereas 0.5-1cm� scalp defects generally heal by epithelization, 1-3cm� defects should be closed with primary saturation, and larger defects should be reconstructed with flaps [31,32]. Defects with an intact periosteum can be repaired with skin grafts. Hartford advocated that preserving a devitalized, intact calvarial bone in electrical burns acts as a good in situ bone graft [33]. It is important to cover burned calvarial bone with a flap in HVEI patients.
Galea, periosteum and temporoparietal fascia flaps are local flaps for scalp defects [34]. For parieto-occipital defects, trapezius [35] and LD flaps [36] are the most appropriate among the distant flap alternatives. Successful reconstruction with well-vascularized tissue in single stage procedures can be performed with free flaps, which are frequently preferred. Various free flaps, such as LD, parascapular [37], omental, ALT, forearm and serratus anterior flaps, can be used for scalp reconstruction [32,38-40]. An omentum flap necessitates intraabdominal surgery [41]. A forearm flap is not large enough to cover large defects, and cosmetic problems result at the donor area. Dissection of the serratus anterior muscle is challenging, and it can result in a winged scapula deformity [4].
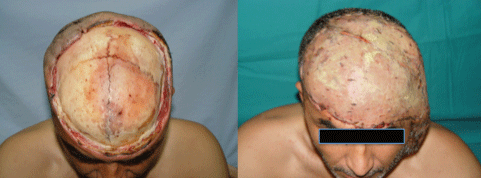
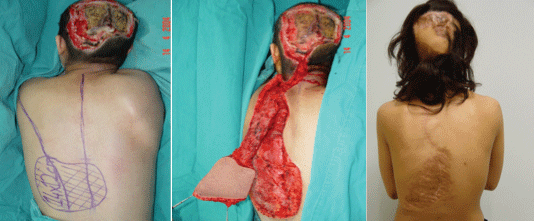
In our study, scalp or temporoparietal flaps were preferred if the defect was of small to medium size with adequate healthy surrounding scalp tissue. The reasons for this selection were perfect color-tissue matching and the ability to work at the identical operation field. Free flaps were preferred if the defect was large or if there was not sufficient surrounding scalp tissue (Figure 3). A free LD flap was our first choice because it provides wide tissue, is easily harvested and has an appropriate pedicle length and caliber that is convenient for anastomosis. In the case of a pregnant patient, reconstruction with a free flap was reasonable under the extreme circumstances; however, because the obstetricians did not approve a long operation, the defect was reconstructed with a pedicled trapezius myocutaneous flap (Figure 4).
.
Figure 3: A head-entry high-voltage electrical burn (left). Postoperative view after free latissimus dorsi flap reconstruction (right).
View Figure 3
.
Figure 4: A pregnant patient with a head-entry high-voltage electrical burn (left). Left pedicled trapezious flap harvesting (middle). One-year postoperative view (right).
View Figure 4
An algorithm for the repair of scalp defects resulting from HVEI is shown in Table 6.
![]()
Table 6: Algorithm of scalp defects in HVEI patients
View Table 6
Lower extremity reconstructions in HVEI
Reconstruction of the distal 1/3 lower extremity is highly challenging. Skin grafts, local cutaneous and fascial and fascioadipous flaps, first dorsal metatarsal artery flaps, distal and proximal pedicled fasciocutaneous/fascioneurocutaneous muscle flaps, cross-leg flaps and free flaps can be used for reconstruction in this region [7,42-46]. When reconstructing foot defects, the calcaneal region is of particular importance because of the pressure point of the foot, which must be covered with thick textured tissue.
In some cases, early reconstruction of electrical burn injuries has the disadvantage of resulting in a tendency to thrombosis because of intimal damage of the vessels, particularly in regions closer to the defect and regions needing a vein graft [47]. In this instance, reconstruction can be achieved with distant pedicled or free flaps with the help of the vascular system of the contralateral lower extremity. If the arteries of the distal lower extremity are injured, flow-through free flaps can be used [48,49].
In our study, fascial, fasciocutaneous, adipofascial turnover or sural flaps were preferred for the patients with adequate local tissue. The sural flap was predominantly preferred because it is a reliable flap, with a constant pedicle and wide arc of rotation; it also provides a sufficiently large tissue area. Local fasciocutaneous flaps were applied if the sural flap could not be used. An adipofascial turnover flap was used as the last option because of the high rate of partial necrosis. Cross-leg sural or fasciocutaneous flaps were used if there was not enough surrounding tissue for local flaps. Two patients with extremely large defects or whose contralateral extremities lacked adequate tissue for flap harvesting were treated with cross-leg free LD flaps.
The algorithm for lower leg and foot defects caused by HVEI is shown in Table 7.
![]()
Table 7: Algorithm of lower leg and foot defects in HVEI patients
View Table 7
Genital reconstructions in HVEI
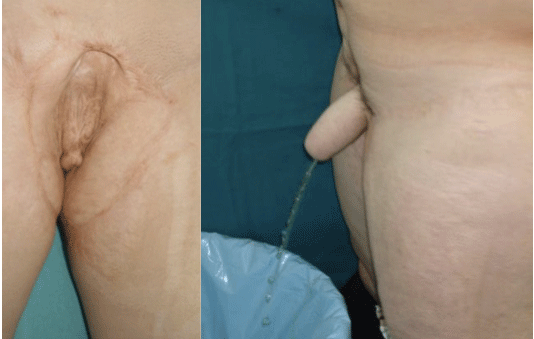
Penis loss secondary to HVEI is rare [50]. We treated two patients with necrosis of the penis caused by HVEI. In one patient, the penis was reconstructed with a free fasciocutaneous radial forearm flap that enclosed 2 silicon rod pieces. Except for the urethral stricture and hair growth in the urethra, no problems were observed in the postoperative period. Sufficient penile sensation occurred at postoperative year 1, and at the 5-year follow up, the patient did not show negative effects on micturition and sexual intercourse. The other patient underwent penile reconstruction with an osteocutaneous free fibula flap (Figure 5). A sufficient skin island, sufficient pedicle length, sufficient penile stiffness by the bone and the capability of harvesting a sensate flap were the most important reasons that this flap was preferred. No problems were observed in the postoperative period; however, the patient had a loss of sexual function, as well as burned and debrided testes.
.
Figure 5: A patient with penile loss resulting from a high-voltage electrical burn after debridement and skin grafting (left). Postoperative view two years after penile reconstruction with an osteocutaneous fibula flap (right).
View Figure 5
Complications
Saint-Cyr et al. [8] observed total flap loss in 3 of 15 cases of free flap administration in 14 patients with HVEIs. Their free flap success rate was 80%. Ofer et al. [29] showed an 85% success rate in flap reconstruction in 26 patients with electrical burns. They encountered a hematoma in 2 (7.7%) cases, partial flap necrosis in 1 (3.8%) case and a fistula in 1 (3.8%) case. Zhu et al. [51] demonstrated 1 total flap necrosis case and 2 partial flap necrosis cases in 398 flaps that were applied in 155 electrically burned patients. We encountered 33 (21.2%) complications in 156 flaps, which included 3 (18.8%) cases of total free flap loss in 16 free flap administrations and 19 (12.2%) cases of partial flap loss among all the flaps. We encountered 6 cases of infection and 1 hematoma under the flaps (Table 2). After prompt debridement, the remaining defects were repaired with saturation and flap advancement operations. The infections observed under the flaps were managed by debridement on alternate days, and local and parenteral antimicrobial therapy was performed with respect to the wound cultures and antibiograms. Hematomas were evacuated, and, eventually, the flaps healed spontaneously. In our patients, there were 29 finger amputations, 34 above/below big joint amputations and 7 disarticulations.
Limitations
An important limitation of this study was that perforator flaps were not discussed. Some authors have successfully used perforator flaps, particularly in defects after burn contracture release. However, there have been no large series using perforator flaps during the early injury period after HVEI. Another limitation is the limited number of patients with perineal HVEI defects; therefore, we could not construct a perineal flap reconstruction algorithm. In this study, we were not clarified the metabolic responses for fluid formulas and morbidity and mortality rates of HVEI patients as Sara�oglu et al. [52] described.
Conclusion
After clinical evaluation, the treatment of HVEI defects should include urgent F/E, serial debridement and reconstruction with a reliable flap. The flap reconstruction algorithms that we suggest might aid plastic surgeons in rapidly and effectively treating HVEI patients.
References
-
Kempn� T, Lipov� B, Hokynkov� A, Lorenz L, Klosov� H (2012) Wrap-around flap in urgent thumb reconstruction after high-voltage electrical injury. Burns 38: 20-23.
-
Luz DP, Millan LS, Alessi MS, Uguetto WF, Paggiaro A, et al. (2009) Electrical burns: a retrospective analysis across a 5-year period. Burns 35: 1015-1019.
-
Kym D, Seo DK, Hur GY, Lee JW (2014) Epidemiology of electrical injury: Differences between low- and high-voltage electrical injuries during a 7-year study period in South Korea. Scand J Surg.
-
Dalay C, Kesiktas E, Yavuz M, Ozerdem G, Acarturk S (2006) Coverage of scalp defects following contact electrical burns to the head: a clinical series. Burns 32: 201-207.
-
Kumar S, Ali W, Verma AK, Pandey A, Rathore S (2013) Epidemiology and mortality of burns in the Lucknow Region, India--a 5 year study. Burns 39: 1599-1605.
-
Handschin AE, Vetter S, Jung FJ, Guggenheim M, K�nzi W, et al. (2009) A case-matched controlled study on high-voltage electrical injuries vs thermal burns. J Burn Care Res 30: 400-407.
-
Azzena B, Tiengo C, Salviati A, Mazzoleni F (2007) Combined use of free and pedicled skin flaps for the reconstruction of extremities in high voltage electrical injury. Burns 33: 382-386.
-
Saint-Cyr M, Daigle JP (2008) Early free tissue transfer for extremity reconstruction following high-voltage electrical burn injuries. J Reconstr Microsurg 24: 259-266.
-
Koul AR, Patil RK, Philip VK (2008) Early use of microvascular free tissue transfer in the management of electrical injuries. Burns 34: 681-687.
-
Mann R, Gibran N, Engrav L, Heimbach D (1996) Is immediate decompression of high voltage electrical injuries to the upper extremity always necessary? J Trauma 40: 584-587.
-
Nafs FJE, Aromir FC, Carreira IS, Olaso PSC (1993) High tension electrical burns. Eur J Plast Surg 16: 84�8
-
Stefanacci HA, Vandevender DK, Gamelli RL (2003) The use of free tissue transfers in acute thermal and electrical extremity injuries. J Trauma 55: 707-712.
-
Hallock GG (2002) The utility of both muscle and fascia flaps in severe upper extremity trauma. J Trauma 53: 61-65.
-
Kojima T, Kinoshita Y, Hirase Y, Endo T, Hayashi H (1994) Extended palmar advancement flap with V-Y closure for finger injuries. Br J Plast Surg 47: 275-279.
-
Yamada N, Ui K, Uchinuma E (2001) The use of a thin abdominal flap in degloving finger injuries. Br J Plast Surg 54: 434-438.
-
Gao W, Yan H, Li Z, Li X, Jiang L, et al. (2011) The free dorsoradial forearm perforator flap: anatomical study and clinical application in finger reconstruction. Ann Plast Surg 66: 53-58.
-
Wang P, Zhou Z, Dong Q, Jiang B, Zhao J (2011) Reverse second and third dorsal metacarpal artery fasciocutaneous flaps for repair of distal- and middle-segment finger soft tissue defects. J Reconstr Microsurg 27: 495-502.
-
Cil Y, Eski M, Isik S (2008) First dorsal metacarpal artery adipofascial flap for thenar burn contracture releasing. Burns 34: 127-130.
-
Feng SM, Gu JX, Liu HJ, Zhang NC, Pan JB, et al. (2013) Treatment of distal fingertip degloving injuries using a cross-finger flap based on the dorsal branch of the proper digital artery at the middle phalanx. J Reconstr Microsurg 29: 623�30
-
Dias AD (2010) Remember S.E.P.A. flap? Indian J Plast Surg 43: 119-120.
-
Goertz O, Kapalschinski N, Daigeler A, Hirsch T, Homann HH, et al. (2012) The effectiveness of pedicled groin flaps in the treatment of hand defects: results of 49 patients. J Hand Surg Am 37: 2088-2094.
-
Fankhauser G, Klomp A, Smith A, Rececca A, Casey W 3rd (2010) Use of the pedicled tensor fascia lata myocutaneous flap in the salvage of upper extremity high-voltage electrical injuries. J Burn Care Res 31: 670�3
-
Biswas D, Wysocki RW1, Fernandez JJ, Cohen MS2 (2014) Local and regional flaps for hand coverage. J Hand Surg Am 39: 992-1004.
-
Oki K, Murakami M, Tanuma K, Ogawa R, Ozawa H, et al. (2009) Anatomical study of pectoral intercostal perforators and clinical study of the pectoral intercostal perforator flap for hand reconstruction. Plast Reconstr Surg 123: 1789-1800.
-
Morrison CS, Sullivan SR, Bhatt RA, Chang JT, Taylor HO (2013) The pedicled reverse-flow lateral arm flap for coverage of complex traumatic elbow injuries. Ann Plast Surg 71: 37-39.
-
Uygur F, Sever C, Evin� R, Ulk�r E, Duman H (2008) Reverse flow flap use in upper extremity burn contractures. Burns 34: 1196-1204.
-
Hu XH, Qin FJ, Chen Z, Shen ZY, Shen YM (2013) Combined rectus abdominis muscle/paraumbilical flap and lower abdominal flap for the treatment of type III circumferential electrical burns of the wrist. Burns 39: 1631-1638.
-
Germann G, Steinau HU (1995) Functional soft-tissue coverage in skeletonizing injuries of the upper extremity using the ipsilateral latissimus dorsi myocutaneous flap. Plast Reconstr Surg 96: 1130-1135.
-
Ofer N, Baumeister S, Megerle K, Germann G, Sauerbier M (2007) Current concepts of microvascular reconstruction for limb salvage in electrical burn injuries. J Plast Reconstr Aesthet Surg 60: 724-730.
-
Oni G, Saint-Cyr M, Mojallal A (2012) Free tissue transfer in acute burns. J Reconstr Microsurg 28: 77-84.
-
Beasley NJ, Gilbert RW, Gullane PJ, Brown DH, Irish JC, et al. (2004) Scalp and forehead reconstruction using free revascularized tissue transfer. Arch Facial Plast Surg 6: 16-20.
-
Newman MI, Hanasono MM, Disa JJ, Cordeiro PG, Mehrara BJ (2004) Scalp reconstruction: a 15-year experience. Ann Plast Surg 52: 501-506.
-
Hartford CE (1989) Preservation of devitalized calvarium following high-voltage electrical injury: case reports. J Trauma 29: 391-394.
-
Ozerdem OR, Anlatici R, Sen O, Yildirim T, Bircan S, et al. (2003) Prefabricated galeal flap based on superficial temporal and posterior auricular vessels. Plast Reconstr Surg 111: 2166�75
-
Lynch JR, Hansen JE, Chaffoo R, Seyfer AE (2002) The lower trapezius musculocutaneous flap revisited: versatile coverage for complicated wounds to the posterior cervical and occipital regions based on the deep branch of the transverse cervical artery. Plast Reconstr Surg 109: 444�50
-
Jeong WS, Roh JL, Kim EK (2014) Extensive scalp reconstruction after repeated failure of free tissue transfer with a pedicled latissimus dorsi flap. J Craniofac Surg 25: 1103-1105.
-
Herrera F, Buntic R, Brooks D, Buncke G, Antony AK (2012) Microvascular approach to scalp replantation and reconstruction: a thirty-six year experience. Microsurgery 32: 591-597.
-
Bailey JK, Park C, Yakuboff KP (2011) Fourth-degree burn of the brain from friction burn of scalp: an unusual injury from a golf cart. J Burn Care Res 32: e146-148.
-
Lee JW, Hsueh YY, Lee JS (2010) Composite skull and dura defect reconstruction using combined latissimus dorsi musculocutaneous and serratus anterior muscle-rib free flap coupled with vascularized galea transfer: a case report. Microsurgery 30: 632�5
-
Chicarilli ZN, Ariyan S, Cuono CB (1986) Single-stage repair of complex scalp and cranial defects with the free radial forearm flap. Plast Reconstr Surg 77: 577-585.
-
Kalra GS, Goil P, Chakotiya PS1 (2013) Microsurgical reconstruction of major scalp defects following scalp avulsion. Indian J Plast Surg 46: 486-492.
-
Grishkevich VM (2014) Proximally based sural adipose-cutaneous/scar flap in elimination of ulcerous scar soft-tissue defect over the achilles tendon and posterior heel region: a new approach. J Burn Care Res 35: e143-150.
-
Li Y, Xu J, Zhang XZ (2013) Lowering the pivot point of sural neurofasciocutaneous flaps to reconstruct deep electrical burn wounds in the distal foot. Burns 39: 808-813.
-
Hallock GG (2014) The First Dorsal Metatarsal Artery Perforator Propeller Flap. Ann Plast Surg .
-
Tajsic N, Winkel R, Husum H (2014) Distally based perforator flaps for reconstruction of post-traumatic defects of the lower leg and foot. A review of the anatomy and clinical outcomes. Injury 45: 469-477.
-
Russo A, Delia G, Casoli V, Colonna MR, Stagno d'Alcontres F (2014) Dorsalis pedis adipofascial perforator flap for great toe reconstruction: anatomical study and clinical applications. J Plast Reconstr Aesthet Surg 67: 550�4
-
Banic A, Wulff K (1987) Latissimus dorsi free flaps for total repair of extensive lower leg injuries in children. Plast Reconstr Surg 79: 769-775.
-
Kesiktas E, Yavuz M, Gencel E, Dalay C, Acart�rk S (2006) Use of cross-leg latissimus dorsi free flap for repair of extensive lower leg electrical injury in a child. Burns 32: 507-510.
-
Koshima I, Fujitsu M, Ushio S, Sugiyama N, Yamashita S (2005) Flow-through anterior thigh flaps with a short pedicle for reconstruction of lower leg and foot defects. Plast Reconstr Surg 115: 155-162.
-
Santanelli F, Paolini G (2003) Glans, urethra, and corporeal body reconstruction by free osteocutaneous forearm flap transfer. Ann Plast Surg 50: 545-549.
-
Zhu ZX, Xu XG, Li WP, Wang DX, Zhang LY, et al. (2003) Experience of 14 years of emergency reconstruction of electrical injuries. Burns 29: 65-72.
-
Saracoglu A, Kuzucuoglu T, Yakupoglu S, Kilavuz O, Tuncay E, et al. (2014) Prognostic factors in electrical burns: a review of 101 patients. Burns 40: 702-707.





