International Journal of Anesthetics and Anesthesiology
Safety and Efficacy of Remifentanil for Single Agent Procedural Sedation: A Systematic Review
Jeppe T Jensen1*, Peter Vilmann1, Lars Konge2 and Møller3
1Department of Endoscopy, Gastro-Unit D, University Hospital Herlev, Denmark
2Centre for Clinical Education, University of Copenhagen, Denmark
3Department of Anesthesiology, University Hospital Herlev, Denmark
*Corresponding author:
Jeppe Thue Jensen, Herlev University Hospital, Gastro Unit D, Department of Endoscopy, Herlev Ringvej 75, DK-2730 Herlev, Denmark, Tel: 0045-38685245, E-mail: jeppe.thue.jensen.01@regionh.dk
Int J Anesthetic Anesthesiol, IJAA-2-033, (Volume 2, Issue 3), Review Article; ISSN: 2377-4630
Received: June 24, 2015 | Accepted: August 16, 2015 | Published: August 19, 2015
Citation: Jensen JT, Vilmann P, Konge L, Møller (2015) Safety and Efficacy of Remifentanil for Single Agent Procedural Sedation: A Systematic Review. Int J Anesthetic Anesthesiol 2:033. 10.23937/2377-4630/2/3/1033
Copyright: © 2015 Jensen JT, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: More procedures are performed in sedation alone or as an adjunct to local anesthesia. Hence, the diversity of the procedures and the patients are increasing along with the need for suitable sedative alternatives.
Objective: The purpose of this study was to assess the safety and efficacy of remifentanil monotherapy for procedure sedation.
Design: Systematic review of randomised controlled trials without meta-analyses.
Data-sources: Electronic search of Pubmed, EMBASE, The Cochrane Library, and Web of Knowledge. No date or language limitations were applied.
Eligibility criteria: Only full-text articles of remifentanil monotherapy for procedural analgesia/sedation were eligible. Remifentanil as an adjunct to local anesthesia was also considered.
Results: Twenty one randomised controlled trials (718 vs. 719 patients) were included. Sedation related mortality was zero. The rate of hypoxia was lower (26 vs 56, P<0.005) in the remifentanil group, fewer needed assisted ventilation (2 vs 15, p<0.005), there was a lower incidence of blood pressure deviation (0.2% vs 7.3%, P<0.005), less procedures were incomplete or needed rescue therapy (4 vs 12, P=0.045) and patients experienced more nausea and\or vomiting (16.5% vs 10.2%, P=0.004).
Conclusion: Remifentanil sedation can be performed with few adverse events as long as the patient is reminded to breathe firmly. Patients experience more nausea and vomiting after remifentanil sedation compared with propofol sedation, but expresses no difference in satisfaction.
Keywords
Sedation, Analgesia, Remifentanil
Introduction
Hospitals and healthcare centers are continuously pushed to deliver a better quality of care with a higher turnover. Hence, there is an increasing demand for shorter procedures and shorter time to discharge. Some of these requirements can be met if sedation is used instead of general anesthesia. Furthermore, sedation, as an alternative to nothing, has its benefits. Two recent studies have shown that sedation for endoscopies increases endoscopist satisfaction, the patient's willingness to undergo a repeat procedure, and the likelihood for successful cecal intubation [1,2].
Conventional sedation has since the beginning of the 1980s primarily consisted of benzodiazepines such as midazolam and/or opioids such as fentanyl, alfentanil or pethidine. Lately, propofol has increased in popularity. Over the last 20 years, an increasing amount of procedures have been performed in sedation only, or with sedation as an adjunct to regional or local anesthesia. This implies that a larger and more diverse patient population has been sedated. Hence, the need for suitable sedative alternatives is increasing. Preferably, the ultimate sedative preserves hemodynamic stability, respiratory function and has a short context sensitive half-life so that the desired depth of sedation can be obtained quickly without prolonged recovery [3-8]. There is no single drug with these characteristics.
Remifentanil is an ultra-short acting opioid with fast onset, no accumulation and fast offset through plasma cholinesterase metabolism independent of kidney function. It provides for analgesia and some sedative effect. The clinical effect wears off within 2 to 5 minutes, and the side-effects of remifentanil are dose-dependent and include nausea, vomiting, pruritus, muscle stiffness and cardiopulmonary depression [9]. Hence, remifentanil could provide for a controllable level of sedation and analgesia with minimal or non-sustained side effects. Furthermore, the pharmacodynamic properties should allow for a fast recovery and short time to discharge.
The purpose of this systematic review was to compare the safety and efficacy of remifentanil monotherapy with other sedatives for procedure sedation.
Materials and Methods
This systematic review was conducted according to the Prisma guidelines [10]. The protocol was not registered.
Eligibility criterion for considering studies for this review
Randomized controlled trials of remifentanil as monotherapeutic analgosedation for procedures alone or as an adjunct to regional anesthesia and local infiltration anesthesia. There were no procedure or intervention criterions in the control group. Exclusion criteria were, pediatric and intubated patients and protocolled sedative premedication. Post-procedure pain control or labor pain was excluded due to the lack of intervention. Axial nerve blocks with spinal anesthesia or epidural anesthesia was excluded due to the expected hemodynamic side effects of the block and the subsequent effects on that outcome. We considered three types of remifentanil administration: Manually controlled infusion pump (MCI/MCA), target controlled infusion (TCI/TCA) and patient controlled infusion (PCI/PCA).
Information sources
We performed an electronic search in Pubmed. Furthermore we searched the Cochrane Central Register of Controlled Trials (CCRCT), EMBASE, and Web of Knowledge for relevant trials. We had no date or language limitations to the search. For EMBASE and Web of Knowledge, the filters: Human and Full-text were used. Mesh terms for the Pubmed search were: "sedation" AND "remifentanil". Identical wording was used for the other databases. See Appendix 1 for further information on the search results. We also searched related articles in the search databases and reference lists of identified studies. The search was conducted by first author between fifth of August 2014 and 14th of August 2014.
Study selection
Selection of studies was performed by first author who reviewed titles, abstracts and full-texts for eligibility. Only full papers compliant with in- and exclusion criterion were selected. Selected studies were pooled in groups depending on the type of control intervention as: Propofol, propofol with remifentanil (sedation or general anesthesia), benzodiazepine, opioid, benzodiazepine with an opioid, and dexmedetomidine.
Data collection process
Data collection was conducted using a data extraction sheet stating the outcomes searched for. First and second author collected the data independent of each other directly from full papers (Table 1-3).
![]()
Table 1: Risk of bias
View Table 1
![]()
Table 2: Safety and efficacy
View Table 2
![]()
Table 3: Postoperative nausea and vomiting and satisfaction
View Table 3
Data items and outcomes
Primary outcomes: Sedation related adverse events and mortality. Adverse events were hypoxia, bradypnea, apnea, hypertension, hypotension, mask ventilation and intubation. The definitions of adverse advents were as defined by the study authors.
Secondary outcomes: Procedure failure due to insufficient sedation or the need for rescue therapy, nausea or vomiting and physician and patient satisfaction with sedation as found in the author's conclusion. Transformation of results was performed to fit the study set up: Study designs with multiple interventions were simplified through interpretation of each study arm independently. Continuous outcome data were simplified and interpreted as dichotomous when possible. For example "satisfaction", which was mostly measured as a continuous outcome on various scales, was in terms simplified according to the author's conclusion of significantly "satisfied" or "not satisfied".
Risk of bias assessment
The risks of bias in individual studies were assessed using the Cochrane Collaboration Risk of Bias Tool (CCRBT) [11]. Assessment was performed by first author to assist interpretation of findings and the robustness of data. Furthermore, we wished to explore the study quality in order to address possible need for future work.
Statistics
Summary of measures for the pooled, binary data was performed using Pearson Chi-squared or Fisher's Exact Test as appropriate. We considered P<0.05 significant. We did not perform a sensitivity analysis.
Results
Description of studies
The database search identified 2281 items (Figure 1). One title was identified as a reference. 1550 duplicates/triplicates (title/abstract) were removed. After title and abstract screening, 69 articles were assessed for eligibility. Only full-text articles were considered. 21 randomised controlled trials of remifentanil versus other sedatives or general anesthesia were included for evaluation. The total number of participants was 1437. The remifentanil population was 718 versus 719 in the control group. The included studies used both manually controlled infusions, target controlled infusion, and patient controlled infusion. Remifentanil was compared with propofol, midazolam, other opioids, dexmedetomidine, propofol with remifentanil co-administration, and general anesthesia. A variety of procedures were studied: Fiberoptic intubation, removal of intracranial space-occupying lesion , radiofrequency treatment of atrial flutter , blepharoplasty and otoplasty, endoscopy, carotid endarterectomy, eye surgery, aortic endovascular repair, breast biopsy, second trimester abortion , shock-wave lithotripsy, operative hysteroscopy, and oocyte retrieval. See Appendix 1 for further study description.
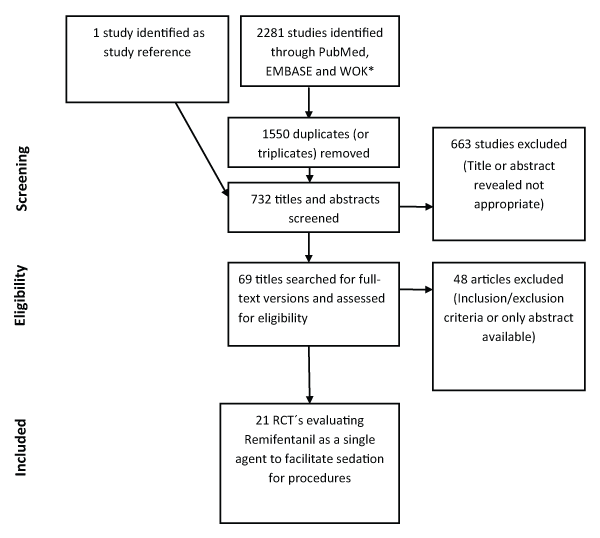
.
Figure 1: Flowchart
*Web of Knowledge, including Cochrane Centre of Registered Trials.
View Figure 1
Risk of bias
The 21 studies are all depicted in table 1. Blinding of the administrating personnel is difficult during sedation and only two studies performed blinding of all involved personnel, both studies utilizing PCI technique [12,13]. Allocation concealment was reported adequately in seven studies [12-18], leaving eight with unsure concealment and six with no allocation concealment. Five studies had an inadequate methods section, possibly allowing for unaccounted bias [3,19-22]. Furthermore, a few primary outcomes [6,12] and several of the secondary outcomes were subjective and study samples were small or not blinded, hence increasing the risk of bias. Sample size consideration or power calculations were described in 14 studies. Seven studies fully or partially accounted for eligible patients and how many were enrolled [3,12,15-17,20,23], potentially affecting generalizability or skewed results in the remaining.
Results overall
Mortality related to sedation was not reported in any of the studies included. As seen in table 2, the overall rate of hypoxia was lower in the remifentanil group (P<0.005). The overall rate of bradypnea or apnea was lower in the remifentanil group (P<0.005). Two patients in the remifentanil group needed assisted ventilation compared to 15 patients in the control group (p<0.005). There was a lower overall incidence of deviation from baseline blood pressure in the remifentanil group compared to control (P<0.005). In the 718 procedures undertaken in remifentanil sedation, 4 procedures were recorded as incomplete due to insufficient sedation or needed rescue therapy in order to complete the procedure compared with 12 in 719 procedures in the control group (P=0.045). In one study data was not available for this outcome [3]. There was no difference in patient willingness to repeat the procedure in the same type of sedation and there was no difference in what the patients favoured in terms of remifentanil or control. Sedationists or physicians favoured remifentanil or recorded no difference in terms of satisfaction with sedation or working conditions. In the remifentanil treated population 68% of the patients recalled the procedure or parts of it compared with 42% of the control population. There was a higher percentage of the remifentanil treated patients who experienced nausea and\or vomiting during or after the procedure (P=0.004). The results are shown in table 3. There were not enough studies utilizing TCI or PCI to allow for a meaningful comparison with MCI.
Results by control group
There was no significant difference in the frequency of adverse events when comparing remifentanil with propofol (229 vs. 224 patients), but the need for respiratory support with a facemask was higher in the propofol group (2 vs. 10; p=0.017) and the rate of nausea and vomiting were higher in the remifentanil group (25 vs 3; p<0.005). Physicians favoured remifentanil over propofol or recorded no difference. More patients in the midazolam with opioid group (0 vs. 21 patients) had bradypnea/apnea (p<0.005), blood pressure deviation (p<0.005), and five needed assisted ventilation compared with zero in the remifentanil group. The difference in hypoxia was not significant. Physicians favoured remifentanil. When comparing remifentanil with other opioids, the frequency of hypoxia and the need for rescue therapy was not significantly higher. Significantly more patients (p=0.022) in the propofol with remifentanil group experienced hypoxia, but the rate of nausea and vomiting was lower (p=0.002) and neither physicians nor patients favoured remifentanil. There was no difference in adverse events when comparing remifentanil with dexmedetomidine, but patients and physicians favoured dexmedetomidine.
Discussion
The frequency of adverse events was lower in the remifentanil group compared with midazolam with opioids and the frequency of hypoxia was higher in the propofol with remifentanil group. There was no difference in any of the other groups. Assisted ventilation was needed more frequently when sedating with propofol or midazolam with an opioid. However, one study contributed considerably to this result [17]. Remifentanil proved to be more efficient than propofol or opioids in terms of procedure completion rate or the need for rescue therapy and less efficient in the remifentanil versus dexmedetomidine study [14]. Overall, patients who received remifentanil experienced more nausea and vomiting compared to control groups, but only consistently when propofol was part of the control group therapy. With the exception of one study [24], where patients were asked if they remembered the subsequent intubation, patients receiving remifentanil had full recollection of the procedure, whereas the control group had varying degrees of recall. As evaluated by the authors, patients had no preferences regarding type of sedation. Authors, on behalf of sedationists or physicians, preferred remifentanil to propofol and midazolam with opioids but preferred propofol with remifentanil or dexmedetomidine to remifentanil, or were unable to detect any difference in terms of satisfaction with sedation or working conditions.
Assessment of safety
Remifentanil is safer than benzodiazepines, as safe as propofol with or without opioids, and possibly less safe than dexmedetomidine. But only consistent as long as careful attention is paid and patients are encouraged to breathe often.
As frequently seen, the overall mortality rate was zero. Safety during remifentanil sedation was therefore assessed with the most commonly used surrogate markers: Rate of hypoxia, rate of bradypnea or apnea, rate of assisted ventilation or intubation, and hemodynamic stability. Eight studies reports varying degrees of hypoxia in the remifentanil population [13,14,18,19,23,25-27]. Most studies define hypoxia as a haemoglobin saturation (SAT%) <90%, although the definition of hypoxia ranges from SAT%<90-94 %. Three studies had a considerably higher rate of remifentanil induced hypoxia. One of these studies defined hypoxia as SAT%<95% which could readily explain the hypoxia rate of 20% [26]. Furthermore, this study used MCI supplemented with PCI. The second study [27] reported a rate of hypoxia of 23% compared to the overall rate of 2.9%. The trial studied remifentanil TCI versus fentanyl TCI for shockwave lithotripsy. The target plasma concentration was 2.8ng.mL-1, which is not particularly high. There were not registered any cases of bradypnea or apnea during the procedures. Oxygen was delivered with a facemask with an oxygen/air mixture of 50%. The fentanyl treated population in this study had a hypoxia frequency of 59%. The third study used an infusion rate of 0.05mcg.kg.minute-1 with a PCI system delivering 0.5cg.kg-1 bolus every third minute. The Control group did not have any adverse events. An unconfirmed explanation for these results could be that the patients were less verbally stimulated, other than that, there is no obvious explanation to the high frequency of hypoxia in these two studies. Remifentanil is known to produce respiratory depression in terms of hypoventilation, bradypnea or apnea. Only five studies report on remifentanil induced brady- or apnea [13,14,17,20,26] and the overall rate was lower than that induced by propofol, midazolam and opioids, but not that of dexmedetomidine. In two studies [13,14] bradypnea or apnea were associated with a transient desaturation. Assisted ventilation was needed in two cases [19,26]. In the remaining studies, apnea was avoided in the remifentanil group through encouraging patients to breathe firmly. Although respiratory depression is an expected adverse event with opioid administration, the overall rate was lower in the remifentanil group as compared with the remaining control groups, apart from dexmedetomidine, which is known to maintain respiration. Two patients needed mask ventilation. No patient needed intubation or other advanced airway handling due to oversedation or aspiration. Hemodynamic stability was high in the remifentanil treated population in partial contrast with an earlier finding [28]. Only one study [25] reported a clinically significant change in blood pressure during endoscopy. Bradycardia is a well-known complication in endoscopy and was registered in eight cases in this trial. Since we did not include bradycardia as an outcome measure, we cannot conclude on this outcome. It is evident that remifentanil provides better hemodynamic stability than midazolam with an opioid, but apart from this finding, there is no significant difference in hemodynamic control in any of the trials. This finding emphasizes the advantage of sedation versus general anesthesia in terms of hemodynamic control Appendix 2.
Assessment of working conditions and completion rate
Remifentanil provides for a high degree of patient co-operation, none or little sedation and a high completion rate.
Five studies favoured remifentanil to control [16,21,29-31]. Three of these trials examined remifentanil sedation for fiberoptic intubation. The authors' reports of good intubation conditions, even without topical anesthesia, are in accordance with earlier findings [9,32,33]. The remaining two studies [16,31] investigates remifentanil sedation as an adjunct to infiltration analgesia for endovascular repair of an abdominal aortic aneurysm and blepharoplasty and otoplasty. Three trials favour control to remifentanil: Propofol with remifentanil sedation for shockwave lithotripsy [13], eye surgery [22] and dexmedetomidine for fiberoptic intubation. Three studies [12,15,30-35] used rescue therapy with propofol, midazolam or general anesthesia due to insufficient sedative effect of remifentanil. One study [13] reports of rescue therapy due to insufficient analgesia of remifentanil during shockwave lithotripsy.
Assessment of nausea, vomiting and patient satisfaction with sedation
Nausea and vomiting is a common side effect of remifentanil, but has little influence on patient satisfaction with sedation. Patients seem to prefer sedation compared to general anesthesia, but are indifferent to the type of sedation and magnitude of recall.
Three studies report of no remifentanil induced nausea and vomiting. In one study anti-emetics were administered as premedication [30], one study used a low infusion rate [16]. Data were not available in eight studies. The incidence of nausea and vomiting in the remaining studies ranged from 3-43%, but without affecting the willingness to repeat. Patient satisfaction with sedation in terms of pain, comfort, and overall experience differed in favour of control when propofol combined with remifentanil was administered as PCI for shock-wave lithotripsy [13] or dexmedetomidine for fiberoptic intubation [14]. Dexmedetomidine provided a higher degree of amnesia compared to remifentanil, but other than that, there is no apparent explanation for this finding. During hysteroscopy patients favoured remifentanil compared to general anesthesia [15]. This could correlate with the fear of general anesthesia or the longer recovery. These three studies [13,15] all found the study drug better than the control. In the remaining studies, with available data, there was no difference in preference. In terms of recall, almost all remifentanil treated patients remembered the procedure without affecting the level of satisfaction, possibly with the exception of the dexmedetomidine study [14]. All patients would repeat the procedure in the same type sedation with no difference between the groups or between types of procedure.
Assessment of administration method and type of procedure
It seems that MCI provides for more reliable dose-dependent side effects. On the other hand, TCI provides for less hands-on dose adjustments and more attention can be paid to auditory stimulation of the patient, but this is not evident. In terms of procedure type, shockwave lithotripsy was associated with the highest frequency of hypoxia, possibly due to a need for deeper sedation.
Strengths and limitations
The strength of this study is the relatively large population who received remifentanil as monotherapy. This eases interpretation without having to adjust for the effects of co-administration. The limitation of this study is the large heterogeneity of the included trials. Different procedures, control groups, and patient categories necessitated simplification and transformation of data in order to achieve comparability. The variety of procedures could possibly confound the outcome and simplification of data increases the risk of losing information. The low number of included studies in some comparison groups warrants more data. Bradycardia was not included as an outcome measure, although retrospectively, it would have been relevant.
Conclusion
Remifentanil sedation can be performed with few adverse events as long as the patient is reminded to breathe firmly. It is feasible and efficient for a range of procedures, particularly fiberoptic intubation, and can be administered equally safe with a manually controlled infusion pump or a target controlled infusion. The use of dexmedetomidine for fiberoptic intubation provides good working conditions and warrants further studying along with target controlled infusion of remifentanil.
Aknowledgements
Assistance with the study: None. Financial support: Thanks to Arvid Nilsson's foundation for financial aid in this study. The founders did not have any saying in the objective, conduction, or presentation of the study.
Funding
This study was supported by Arvid Nilssons Foundation. The funders had no saying in the objective or the conduction of this study.
References
-
Amornyotin S, Lertakayamanee N, Wongyingsinn M, Pimukmanuskit P, Chalayonnavin V (2007) The effectiveness of intravenous sedation in diagnostic upper gastrointestinal endoscopy. J Med Assoc Thai 90: 301-306.
-
Radaelli F, Meucci G, Sgroi G, Minoli G; Italian Association of Hospital Gastroenterologists (AIGO) (2008) Technical performance of colonoscopy: the key role of sedation/analgesia and other quality indicators. Am J Gastroenterol 103: 1122-1130.
-
Avramov MN, Smith I, White PF (1996) Interactions between midazolam and remifentanil during monitored anesthesia care. Anesthesiology 85: 1283-1289.
-
Subramanian S, Liangpunsakul S, Rex DK (2005) Preprocedure patient values regarding sedation for colonoscopy. J Clin Gastroenterol 39: 516-519.
-
Lauwers MH, Vanlersberghe C, Camu F (1998) Comparison of remifentanil and propofol infusions for sedation during regional anesthesia. Reg Anesth Pain Med 23: 64-70.
-
Mingus ML, Monk TG, Gold MI, Jenkins W, Roland C (1998) Remifentanil versus propofol as adjuncts to regional anesthesia. Remifentanil 3010 Study Group. J Clin Anesth 10: 46-53.
-
Rai MR, Parry TM, Dombrovskis A, Warner OJ (2008) Remifentanil target-controlled infusion vs propofol target-controlled infusion for conscious sedation for awake fibreoptic intubation: a double-blinded randomized controlled trial. Br J Anaesth 100: 125-130.
-
Berkenstadt H, Ram Z (2001) Monitored anesthesia care in awake craniotomy for brain tumor surgery. Isr Med Assoc J 3: 297-300.
-
Bürkle H, Dunbar S, Van Aken H (1996) Remifentanil: a novel, short-acting, mu-opioid. Anesth Analg 83: 646-651.
-
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, et al. (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol 62: e1-34.
-
Higgins JP, Altman DG, Gøtzsche PC, Jüni P, Moher D, et al. (2011) The Cochrane Collaboration's tool for assessing risk of bias in randomised trials. BMJ 343: d5928.
-
Orbach-Zinger S, Paul-Keslin L, Nichinson E, Chinchuck A, Nitke S, et al. (2012) Tramadol-metoclopramide or remifentanil for patient-controlled analgesia during second trimester abortion: a double-blinded, randomized controlled trial. J Clin Anesth 24:28-32.
-
Joo HS, Perks WJ, Kataoka MT, Errett L, Pace K, et al. (2001) A comparison of patient-controlled sedation using either remifentanil or remifentanil-propofol for shock wave lithotripsy. Anesth Analg 93: 1227-1232.
-
Hu R, Liu JX, Jiang H (2013) Dexmedetomidine versus remifentanil sedation during awake fiberoptic nasotracheal intubation: a double-blinded randomized controlled trial. J Anesth: 27: 211-217.
-
Majholm B, Bartholdy J, Clausen HV, Virkus RA, Engbæk J, et al. (2012) Comparison between local anaesthesia with remifentanil and total intravenous anaesthesia for operative hysteroscopic procedures in day surgery. Br J Anaesth 108: 245-253.
-
Bonfreschi V, Giuliani E, Malagnino FC, Navi A, Coppi G, et al. (2009) Analgesia during abdominal aortic aneurysm endovascular repair: remifentanil vs. fentanyl-midazolam--a randomized controlled trial. Eur J Anaesthesiol 26: 782-787.
-
Lee HM, Sakong J, Jee DL (2013) The comparison of feasibility and safety on fiberoptic guided intubation under conscious sedation with remifentanil and propofol. Korean J Anesthesiol 65: 215-220.
-
Fanti L, Agostoni M, Gemma M, Rossi G, Azzolini ML, et al. (2013) Two dosages of remifentanil for patient-controlled analgesia vs. meperidine during colonoscopy: a prospective randomized controlled trial. Dig Liver Dis 45: 310-315.
-
Bouvet L, Allaouchiche B, Duflo F, Debon R, Chassard D, et al. (2004) Remifentanil is an effective alternative to propofol for patient-controlled analgesia during digestive endoscopic procedures. Can J Anaesth 51: 122-125.
-
Krenn H, Deusch E, Jellinek H, Oczenski W, Fitzgerald RD (2002) Remifentanil or propofol for sedation during carotid endarterectomy under cervical plexus block. Br J Anaesth 89: 637-640.
-
Puchner W, Obwegeser J, Pühringer FK (2002) Use of remifentanil for awake fiberoptic intubation in a morbidly obese patient with severe inflammation of the neck. Acta Anaesthesiol Scand 46: 473-476.
-
Holas A, Krafft P, Marcovic M, Quehenberger F (1999) Remifentanil, propofol or both for conscious sedation during eye surgery under regional anaesthesia. Eur J Anaesthesiol 16: 741-748.
-
Lier MC, Douwenga WM, Yilmaz F, Schats R, et al. (2015) Patient-Controlled Remifentanil Analgesia as Alternative for Pethidine with Midazolam During Oocyte Retrieval in IVF/ICSI Procedures: A Randomized Controlled Trial. Pain Pract 15: 487-495.
-
Puchner W, Egger P, Pühringer F, Löckinger A, Obwegeser J, et al. (2002) Evaluation of remifentanil as single drug for awake fiberoptic intubation. Acta Anaesthesiol Scand 46: 350-354.
-
Manolaraki MM, Theodoropoulou A, Stroumpos C, Vardas E, Oustamanolakis P, et al. (2008) Remifentanil compared with midazolam and pethidine sedation during colonoscopy: a prospective, randomized study. Dig Dis Sci 53: 34-40.
-
Lena P, Mariottini CJ, Balarac N, Arnulf JJ, Mihoubi A, et al. (2006) Remifentanil versus propofol for radio frequency treatment of atrial flutter. Can J Anaesth 53: 357-362.
-
Cortinez LI, Muñoz HR, De la Fuente R, Acuña D, Dagnino JA (2005) Target-controlled infusion of remifentanil or fentanyl during extra-corporeal shock-wave lithotripsy. Eur J Anaesthesiol 22: 56-61.
-
Noseir RK, Ficke DJ, Kundu A, Arain SR, Ebert TJ (2003) Sympathetic and vascular consequences from remifentanil in humans. Anesth Analg 96: 1645-1650, table of contents.
-
Zhang X, He W, Wu X, Zhou X, Huang W, et al. (2012) TCI remifentanil vs. TCI propofol for awake fiber-optic intubation with limited topical anesthesia. Int J Clin Pharmacol Ther 50: 10-16.
-
Lallo A, Billard V, Bourgain JL (2009) A comparison of propofol and remifentanil target-controlled infusions to facilitate fiberoptic nasotracheal intubation. Anesth Analg 108: 852-857.
-
Ferraro GA, Corcione A, Nicoletti G, Rossano F, Perrotta A, et al. (2005) Blepharoplasty and otoplasty: comparative sedation with remifentanil,propofol, and midazolam. Aesthetic Plast Surg 29: 181-183.
-
Vennila R, Hall A, Ali M, Bhuiyan N, Pirotta D, et al. (2011) Remifentanil as single agent to facilitate awake fibreoptic intubation in the absence of premedication. Anaesthesia 66: 368-372.
-
Mingo OH, Ashpole KJ, Irving CJ, Rucklidge MW (2008) Remifentanil sedation for awake fibreoptic intubation with limited application of local anaesthetic in patients for elective head and neck surgery. Anaesthesia 63: 1065-1069.
-
Girard F, Moumdjian R, Boudreault D, Chouinard P, Bouthilier A, et al. (2009) The effect of sedation on intracranial pressure in patients with an intracranial space-occupying lesion: remifentanil versus propofol. Anesth Analg 109: 194-198.
-
Akgül A, Aydin ON, Dayanir V, Sen S, Ugur B, et al. (2007) Usage of remifentanil and fentanyl in intravenous patient-controlled sedo-analgesia. Agri 19: 39-46.





