International Journal of Critical Care and Emergency Medicine
Albuminuria in Critically Ill Patients: A Prospective Cohort Study
Noortje Godijn1,4, Simone M Smits2 and Peter HJ van der Voort1,3*
1Department of Intensive Care, Onze Lieve Vrouwe Gasthuis, The Netherlands
2Department of Clinical chemistry, Onze Lieve Vrouwe Gasthuis, The Netherlands
3TIAS School for Business and Society, Tilburg University, The Netherlands
4Department of neurology, Leiden University Medical Center, Leiden, The Netherlands
*Corresponding author:
P.H.J. van der Voort, Professor of Health Care, TIAS school for business and society, Tilburg University, Tilburg, The Netherlands, Tel: 31 20 5993007, E-mail: p.h.j.vandervoort@olvg.nl
Int J Crit Care Emerg Med, IJCCEM-1-003, (Volume 1, Issue 1), Original Article; ISSN: 2474-3674
Received: July 28, 2015 | Accepted: August 12, 2015 | Published: August 14, 2015
Citation: Godijn N, Smits SM, van der Voort PHJ (2015) Albuminuria in Critically Ill Patients: A Prospective Cohort Study. Int J Crit Care Emerg Med 1:003. 10.23937/2474-3674/1510003
Copyright: © 2015 Godijn N. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: To establish the behaviour of albuminuria over time and its relation to APACHE II score, SOFA score, infection parameters and outcome in critically ill patients.
Methods: In a prospective cohort study, we measured albumin creatinine ratio (MACR) for all consecutively admitted patients at the ICU. We recorded the following baseline variables: gender, age, admission diagnosis, type of admission (medical, surgical), length of stay, days of follow up. The cohort was divided into two pairs of subgroups medical and surgical; diabetes and non-diabetes. Patients were followed for ten days when possible.
Results: A hundred and fifty patients were included with a median age of 68.6 yrs. The patients had a mean APACHE II score of 20.5 and a mean SOFA score of 5.0. In all patients the ACR increases in the first five days. Median ACR on day 1 was 29.2mg/mmol; median ACR on day 5 was 45.5 mg/mmol. For all subgroups except for the diabetes patients the ACR decreased after day five. Spearman rho correlation showed a significant correlation between mean ACR per patient and age (r=0.19), APACHE II (r=0.48), mean SOFA score (r=0.41) and serum creatinine (r=0.25). Only in surgical patients a relation was found between ACR and CRP.
Serum creatinine is found to have a relation with ACR and is a confounder in the relation between ACR and the SOFA score. There was no significant difference found in mean microalbuminuria at the first day between survivors versus non-survivors.
Conclusions: ACR increases in the first five days in all critically ill patients. A relation between ACR and physiologic scores of severity of disease was established, except for diabetes and medical patients.
Keywords
Albuminuria, Albumin-creatinine ratio, Critically ill, Intensive care, Severity of disease
Introduction
In the intensive care unit (ICU) physicians are challenged to predict patient outcome when patients are admitted. Over the years, several tools have been developed for this purpose. Examples are the Acute Physiology and Chronic Health Evaluation (APACHE) and Sepsis Related Organ Failure Assessment (SOFA) scoring systems.
Though useful, these tools are complex. For example, the APACHE score takes 24 hours to collect the data necessary to calculate the predictive mortality. If it would be possible to identify patients who are most at risk of serious complications and adverse outcomes earlier,it might be able to target our clinical interventions more accurately [1-3]. There is need for a non-invasive and direct method for quantification of the severity of illness, complementing the already existing scoring systems.
Microalbuminuria has been proposed as a prognostic marker in the ICU, for acute kidney injury in septic patients and in pediatric intensive care [4-9]. Critical illness is associated with endothelial dysfunction that results from a cytokine cascade following injury and /or infection. Increased capillary permeability to plasma proteins is a consequence [10]. The glomerulus will leak albumin as a reaction to increased endothelial permeability, which will cause (micro) albuminuria. Frequently, patients admitted to an ICU are coping with multiple organ failure including kidney failure. Because of this, there is a rationale for using kidney functions to score the severity of illness [11].
Few preliminary studies examined the use of albuminuria in the intensive care as a prognostic marker. In 2006, a study by Gosling concluded that urine albumin predicts ICU mortality and inotrope requirement as well as or better than APACHE II and SOFA scores [12]. A systematic review by Gopal 2006 describes that albuminuria may hold promise as a predictor of illness severity, and mortality on the intensive care. However, it was concluded that future studies need to be conducted to determine the optimal timing as well as the threshold reference value for the urine albumin creatinine ratio in the adult intensive care population [13].
In this prospective study we record the presence of albuminuria over time and study the association between albuminuria and the conventional severity of illness scoring systems (APACHE and SOFA), infection parameters (C-reactive protein (CRP) and white blood cell count (WBC)) and outcome.
Patients and Methods
Design
A prospective cohort study was performed in a teaching hospital with a 26-bed mixed medical-surgical tertiary ICU. Consecutive intensive care patients over the age of 18 were included. Patients suffering from chronic kidney disease (creatinine more than177μmol/l) and those receiving chronic dialyses were excluded. For practical reasons the follow-up was ten days or until ICU discharge.
We recorded the following baseline variables: gender, age, admission diagnosis, type of admission (medical, surgical), length of stay, days of follow upand outcome. Outcome was extracted from the ICU and hospital database. The cohort was divided into two pairs of subgroups medical and surgical patients based on the type of admission and diabetes and non-diabetes patients based on an established diagnosis of diabetes before ICU admission. Predefined potential confounders were: diabetes mellitus, hypertension and renal function. The APACHE II score was calculated after 24 hours of ICU stay according to the original definitions and following the NICE datadictionary (www.stichting-nice.nl). From the included patients we registered daily the albumin/creatinine ratio (ACR), the Sepsis-related Organ Failure Assessment (SOFA), plasma WBC count using the XE-2100automated blood cell counter (Sysmex) and plasma CRP and creatinine levels using the ModularAnalytics Panalyzer (RocheDiagnostics).
Informed consent was waived by the ethical review board because of the observational design of the study in accordance with Dutch and European legislation.
Urine analyses
Urine samples were collected daily at 9 am. Approximately 15ml was extracted from the urinary catheter, and urine analysis was performed on the same day. Albumin and creatinine levels were analyzed on the ModularAnalytics Panalyzer (RocheDiagnostics), and the ACR was calculated. The ACR is the preferred test for diagnosis of albuminuria because it corrects for the confounding effect of variations in urine volume on the urine albumin concentration [14].
The normal rate of albumin excretion is less than 20mg/mmol; persistent albumin excretion between 30 and 300mg/mmol is in the literature defined as microalbuminuria. However, we defined albuminuria as any amount of albumin excretion in the urine.
Treatment
All patients were treated according to standard intensive care treatment according to national and international guidelines.
Statistical analyses
Statistical analyses were performed with SPSS version 17.0 (SPSS Inc., Chicago, Illinois, USA). Data are expressed as mean and standard deviation (SD) for normally distributed data and as median and interquartile range (IQR) for skewed data. However, when the data from one patient is used as a variable, the arithmetic mean for that patient is used. A p-value less than 0.05 was considered statistically significant for all analyses.
Evaluation of an association between ACR and physiologic scores, markers of inflammation, plasmacreatinine and outcome were made using the two-tailed Spearman rank correlation procedure. Spearman rank correlation was used instead of Pearson correlation because of the non-normal distribution of the ACR values. Because ACR showed a skewed distribution, medians were compared between patient groups using the Mann-Whitney nonparametric test and between time points using the Wilcoxon signed rank test.
Univariate regression analyses were performed for categorical ACR in relation to SOFA score, WBC, CRP, diabetes mellitus, hypertension and plasma creatinine. The ACR categories were chosen based on the normal value of 3.4mg/mmol. The presence of confounding for these relations was tested through logistic regression analyses. The same was done for the relation between ACR day one (ACR1) and APACHE II score.
Results
Characteristics
During a two-month period 150 patients were included. One patient was excluded because of chronic kidney failure for which he received chronic dialyses. The remaining 149 patients had a mean age 68.6 (SD 11.1) range 31-88 years. The patient group included 106 (71.2%) men and 43 (28.8%) women. All patients were treated with vasoactive medication (either noradrenalin, dopamine or enoximone) and nearly all patients were mechanically ventilated. There were no differences in ACR between men and women. Spearman rho correlation showed a significant correlation between mean ACR per patient and age (r=0.19), APACHE II (r=0.48), mean SOFA score (r=0.41) and serum creatinine (r=0.25). APACHE II score, ICU stay, ACR, SOFA and predictive mortality for the categories surgical and medical, diabetes and non-diabetes are summarized in table 1. The surgical patient group included mainly patients after heart valve replacement (76 patients). In addition, 9 patients after gastrointestinal surgery, 8 patients after major vascular surgery, and 4 miscellaneous. The medical patient group consisted of patients with respiratory failure (11 patients), cardiogenic shock (11), sepsis (9), pulmonary infection (7), after cardiac arrest (6), intoxication (2) and miscellaneous (8). Approximately 27% of the patients had diabetes and 32% had preexisting hypertension. The median admission creatinine was 83 (IQR 36 μmol/L. Nineteen percent had a pre-admission creatinine of >120μmol/L.
![]()
Table 1: APACHE II score, ICU length of stay, ACR, SOFA, and APACHE II predicted mortality.
View Table 1
Development of ACR over time
The ACR values for subsequent days in the ICU for all patientsof the cohort and the number of patients included each day are presented in table 2. As the data were collected at 9.00 hrs AM, only data from 8 patients admitted in the night were available.
![]()
Table 2: Median daily ACR (mg/mmol) for all patients
View Table 2
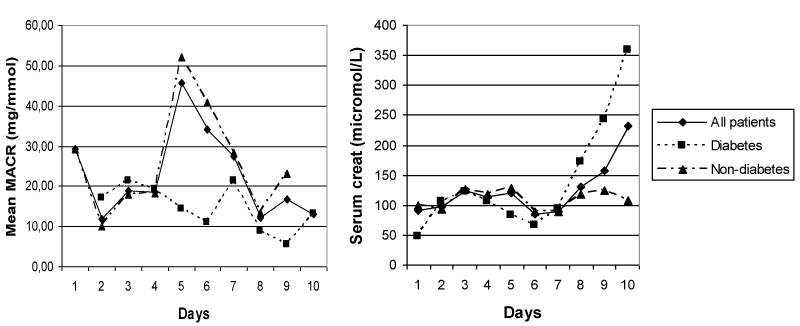
Dailyvalues for ACR and plasmacreatinine for all patients and the subgroups diabetes and non-diabetes are presented in figure 1. Figure 2 shows the daily values for all patients and the subgroups medical and surgical patients.
.
Figure 1: ACR and plasmacreatinine for all patients, diabetes and non-diabetes patients
View Figure 1
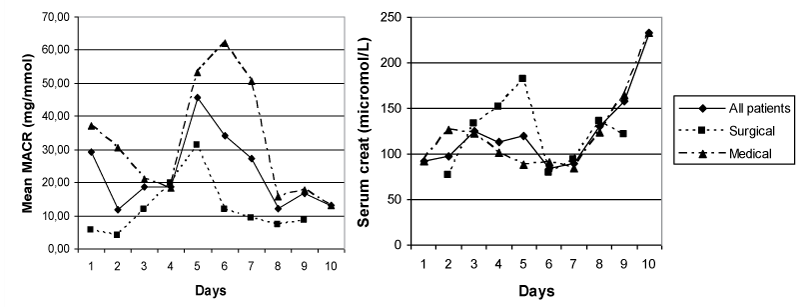
.
Figure 2: ACR and plasma creatinine for all patients, surgical and medical patients
View Figure 2
Relation ACR and physiologic scores, infection parameters
The correlation for ACR compared with SOFA, inflammatory markers and plasmacreatinine is accomplished using the arithmetic mean over the treatment time in the ICU. APACHE II score, calculated in the first 24 hours, is correlated to the first measuredACR (ACR1). Table 3 shows the spearman rho-correlation.
![]()
Table 3: Spearman rho-correlation data for: arithmetic mean of ACR per patient compared with SOFA, inflammatory markers and plasma creatinine; ACR day 1 (ACR1) is compared with APACHE II score.
View Table 3
Univariate regression analyse was conducted for categorical mean ACR (<3.4mg/mmol or >3.4mg/mmol), as the dependent factor. The mean SOFA score per patient, inflammatory markers and the predefined confounders plasma creatinine, diabetes and hypertension were entered as independent variables. We found SOFA (OR 1.3, 95% CI 1.2-1.6; p=0.001) and plasmacreatinine (OR 1.01, 95% CI 1.0-1.02; p=0.004) significantly associated with ACR.
In addition, multivariate logistic regression analyse was performed for categorical ACR as a dependent factor, SOFA score and plasmacreatinine as independent factors, table 4. Table 4 shows a decrease in the regression coefficient (B) of the SOFA score from more then 10 percent in comparison to the univariate analyses. Therefore, plasmacreatinine turns out to be a confounder for ACR in relation with the SOFA score.
![]()
Table 4: Multivariate logistic regression analyse for categorical average MACR (<3.4 mg/mmol or >3.4 mg/mmol).
View Table 4
The analysis was also conducted for categorical ACR measured on day 1 as a dependent factor. APACHE II score and the predefined confounders were entered as independent variables. We found APACHE II (OR 1.1, 95% CI 1.0-1,2; p=0.002) significant correlated to ACR day 1.
ACR and outcome
During our study period ten people did not survive the ICU. We measured a non-significantly higher ACR1 in the non-survivors compared to the survivors (30.08; 95% CI -5,7-65,8 vs. 12.35; 95% CI 6,2-18,5; p= 0,081).
Discussion
This study showed that the ACRof the cohort decreases between the first and the second day but increases until day 5 of ICU treatment in all patient groups. This is followed by a decrease in all patients except for the patients suffering from diabetes mellitus. ACR may be a marker of endothelial dysfunction caused by the primary insult and the subsequent inflammation. This inflammation wanes in several days resulting in a decreased ACR. The observation of an increasing ACR until day 5 is in conflict with a conclusion drawn by Gosling et al. [12]. This author concluded that the ACR decreases significantly after four to six hours. This contradiction may in part be explained by the differences in baseline characteristics between these study populations. Our study was different in two respects. First, the mean age in the Gosling study is 55.5 years versus 68.6 years in our study. We did confirm the finding in the Gosling study that showed that urine albumin on ICU admission increased significantly with patient age. Second, patients in the Gosling study had lower median APACHE scores then in our study, 18.0 versus 20.5. The current study established a significant relation between ACR and APACHE II score. This could be an explanation for the higher ACR values in the current study.
The highest ACR values were found in the diabetic patients. This observation is consistent with the Thorevska [14] study, which found that diabetes was an independent predictor of increased ACR.
The pathogenesis of albuminuria in patients with diabetic ketoacidoses requiring ICU admission is multifactorial. Diabetic ketoacidosis has been shown to cause acute tubular proteinuria and reduced tubular resorption of filtered albumin, which may resolve when acid base status is restored to normal. Also hyperglycemia causes glomerular hyperfiltration, which will contribute to albuminuria and which will resolve with the restoration of blood glucose concentrations toward normal [16]. In our study the median ACR in the diabetes group did not decrease at all over time. However, only one patient was admitted because of ketoacidosis. The diabetes patient group only reflects a small group of patients (41), on day nine and ten respectively three and two patients were available for analysis, which limits further conclusions.
ACR was significantly related to prognostic scores (APACHE II and SOFA). Between ACR and the SOFA score a significant but moderate correlation was found for all patient groups. A significant but relatively weak correlation was found between ACR and APACHE II score except for medical and diabetes patients. Gosling et al. [17] suggests that ACR is an early marker of the systemic inflammatory response to an acute insult, and the effect of an acute event on a pre-existing medical condition that leads to ICU admission will be variable. The ACR in medical and diabetes patients on admission is higher then in surgical a non diabetic patients. This could be an explanation for the non-significant association between ACR and APACHE II score for medical and diabetes patients.
Many of the causes of critical illness are associated with intense inflammatory responses. The cascade of events, triggered by the release of interleukins and other inflammatory mediators, results in widespread endothelial dysfunction [18,19]. The degree of albuminuria is dependent, in part, on the intensity of the inflammatory responses [15]. In surgical patients a significant correlation was found between ACR and CRP. However, in none of the groups a correlation was found between ACR and WBC.
The current study has methodological flaws. From patients admitted in the weekend the first MACR was measured on Monday. As a result, the mean ACR per day is calculated from the available urine samples only. The study failed to establish a statistical significant increase in ACR during the follow up days. The failure to reach statistical significance may be explained in part by the decreasing number of patients followed until day ten. However the 18 patients left on day 6 show the same distribution of ACR and serum creatine over the ten day period (data not shown).
ACR is influenced by many factors, an increase in protein excretion may be seen with fever and exercise, perhaps mediated by angiotensin II or norepinephrine-induced alterations in glomerular permeability, as well as with symptomatic urinary tract infection [14]. We did not record the medication the patients received; this could have been an important confounder.
Conclusion
This observational study was conducted to describe the trend of microalbuminuria over time. It is shown that the mean ACR increased in all patients until day 5, in contradiction to previously performed studies. ACR is significantly correlated with the APACHE II score, except for diabetes and medical patients. In surgical patients a significant relation was found between ACR and CRP. Plasmacreatinine has been established to be a confounder in the relation between ACR and SOFA. There was no significant difference found in mean albuminuria at the first day between survivors versus non-survivors. The ACR in the urine is associated with severity of disease but cannot be used as a routine prognostic marker.
Ethical Statement
Informed consent was waived by the ethical review board because of the observational design of the study in accordance with Dutch and European legislation. All patients were treated and the study was executed according to the Helsinki Statement.
References
-
Knaus WA, Draper EA, Wagner DP, Zimmerman JE (1985) APACHE II: A severity of disease classification system. Crit Care Med 13: 818-829.
-
Vincent J, Moreno R, Takala J, Willatts S, De Mendonça A et al. (1996) The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure. On behalf of the Working Group on Sepsis-Related Problems of the European Society of Intensive Care Medicine. Intensive Care Med 22:707-710.
-
Mackinnon KL, Molnar Z, Lowe D, Watson ID and Shearer E (2000) Use of microalbuminuria as a predictor of outcome in critically ill patients. BR J Anaesth 84: 239-41
-
Omar A, Sun Q, Sugimoto K, Mercan D, Vincent J (2001) Predictive value of microalbuminuria in medical ICU patients: results of a pilot study. Chest 120: 1984-1988.
-
Molnar Z, Szakmany T, Heigl P (2003) Microalbuminuria does not reflect increased systemic capillary permeability in septic shock. Intensive Care Med 29:391-395.
-
Gosling P, Shearman CP, Gwynn B, Simms MH (1988) Microproteinuria: response to operation. Br Med J (Clin Res Ed) 296: 338-389.
-
Neyra JA, Manllo J, Li X, Jacobsen G, Yee J, Yessayan L, et al. (2014) The association of de novo dipstick albuminuria with severe acute kidney function in critically ill septic patients. Nephron ClinPract 128: 373-380.
-
Din AH, Frew Q, Smailes ST, Dziewulski P (2015) The utility of microalbuminuria measurements in pediatric burn injuries in critical care. J Crit Care 30:156-161.
-
Anil AB, Anil M, Yildiz M, Kamit Can F, Bal A, et al. (2014)The importance of microalbuminuria in predicting patient outcome in a PICU. Pediatr Crit Care Med 15:e220-225.
-
Fleck A, Raines G, Hawker, Trotter J, Wallace PI, et al. (1985) Increased vascular permeability: A major cause of hypoalbuminaemia in disease and injury. Lancet 1:781-784.
-
Dubaybo BA (2001) Microalbuminuria: simple, inexpensive, and dynamic marker of critical illness. Chest 120: 1769-1771.
-
Gosling P,Czvz J, Nightingale P, Manji M (2006) Microalbuminuria in the intensive care unit: Clinical correlates and association with outcomes in 431 patients. Crit Care Med Aug 34: 2158-2166.
-
Gopal S, Carr B, Nelson P (2006) Does microalbuminuria predict illness severity in critically ill patients on the intensive care unit? A systematic review. Crit Care Med 34: 1805-1810.
-
Rose BD, Fletcher SW (2008) Evaluation of isolated proteinuria in adults.
-
Thorevska N, Sabahi R, Upadya A, Manthous C, Amoateng-Adjepong Y (2003) Microalbuminuria in critically ill medical patients: Prevalence, predictors, and prognostic significance. Crit Care Med 31; 1075-1081.
-
Miltenyi M, Szabo A, Tulassay T, Körner A, Kenesei E, et al. (1990) Reduced glomerular filtration and elevated urinary protein excretion in diabetic ketoacidose. Acta Paediatr Scand 79: 444-447.
-
Gosling P, Brudney S, McGrath L, Riseboro S, Manji M (2003) Mortality prediction at admission to intensive care: A comparison of microalbuminuria with acute physiology scores after 24 hours. Crit Care Med 31: 98-103.
-
Stehouwer CD, Lambert J, Donker AJ, van Hinsbergh VW (1997) Endothelial dysfunction and pathogenesis of diabetic angiopathy. Cardiovasc Res 34: 55-68.
-
Pedrinelle R, Dell'Omo G, Penne G, Mariani M (2001)Non-diabeticmicroalbuminuria, endothelialdysfunction and cardiovasculardisease. Vasc Med 6: 257-264.





