International Journal of Critical Care and Emergency Medicine
Inadvertent Late Migration of Jugular Catheter and Bilateral Pleural Effusion and Pneumomediastinum
Yiheng Wang1*, Lixian He2 , Xiaoling Hu1, Zhigang Zhou1, Hong Zhou3
1Department of Anesthesiology, The First Affiliated Hospital, University of South China, China
2Department of Ophthalmology, The First Affiliated Hospital, University of South China, China
3Department of Radiology, The First Affiliated Hospital, University of South China, China
*Corresponding author:
Yiheng Wang, Department of Anesthesiology, The First Affiliated Hospital, University of South China, No.39 Chuangshan Road, Hengyang 421001, Hunan Province, P.R.China, Tel: 860-73485-78511, E-mail: biosciwyh@tom.com
Int J Crit Care Emerg Med, IJCCEM-2-010, (Volume 2, Issue 1), Case Report; ISSN: 2474-3674
Received: December 28, 2015 | Accepted: January 27, 2016 | Published: January 30, 2016
Citation: Wang Y, He L, Hu X, Zhou Z, Zhou H (2016) Inadvertent Late Migration of Jugular Catheter and Bilateral Pleural Effusion and Pneumomediastinum. Int J Crit Care Emerg Med 2:010. 10.23937/2474-3674/1510010
Copyright: © 2016 Wang Y, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The authors report an inadvertent late migration of right jugular catheter and the unexpected complications. Postoperative computed tomography reveals bilateral pleural effusion and pneumomediastinum. We speculate that the migration during the maintenance or multiple attempts of placing a guidewire damaged the wall of right brachiocephalic vein or superior vena cava, and punctured through right pleura and anterior mediastinal leading into the complications.
Keywords
Central venous catheterization, Late migration, Malposition, Complications
Introduction
Central venous catheterization is now a useful and commonly-performed procedure in the operating theater, intensive care unit and emergency room. But the insertion of central venous catheters (CVC) is not free of complications. Incorrect positioning of CVC leads to severe complications such as hematothorax or pneumothorax, chemical or bacterial thrombophlebitis, and perforation of the heart and great vessels [1]. This case report illustrates an inadvertent delayed migration of right jugular catheter and serious complications arising from it.
Case Report
A 50-year-old female patient weighing 52 kg was scheduled for radical gastrectomy due to gastric carcinoma. After induction of general anesthesia and intubation, her head was turned left in Trendelenburg position. With skin disinfection, the right internal jugular vein (IJV) was cannulated with all aseptic precautions using the Seldinger technique. On locating the right IJV with landmark and free aspiration of blood by the needle, a spring guidewire (J-shaped, 0.032 inch) was threaded without any problem, except some resistance at 6 cm depth of the internal jugular vein. A 7F double lumen catheter (Arrow International Inc., Pennsylvania, USA) was passed over the guidewire again without difficulty. The catheter was fixed at the 12 cm mark after free aspiration of blood from both the ports of the catheter. Catheter was sutured, and intravenous anesthetics and fluids were administered via IJV catheter. Surgery was done as planned. After the operation, she was transferred to the wards, and received 500 ml total parenteral nutrition via right jugular catheter.
.
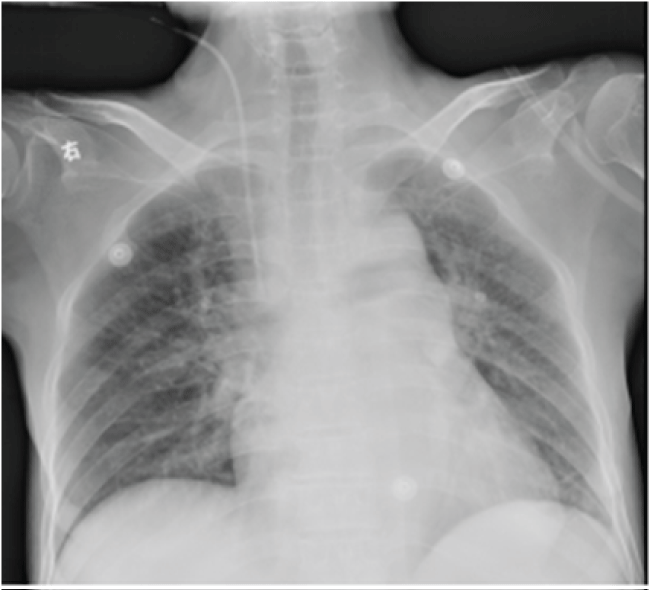
Figure1 1: The same post-operative day X-ray confirmed the safe positioning of central venous catheter.
View Figure 1
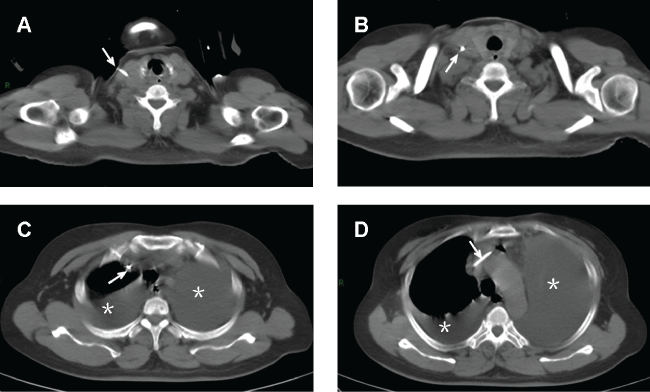
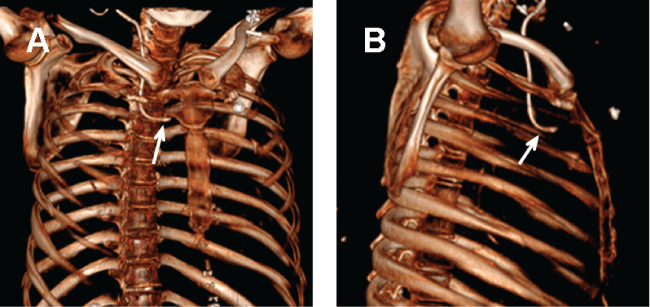
At the first post-operative day, she complained of mild pain at incision site. The patient have a same day post central venous catheterization X-ray with normal chest radiography (Figure 1). On the morning of postoperative day 2, she was in respiratory distress with tachypnoea, mucosa cyanosis and began to report chest pain during the inspiration phase. The extremities were clammy. Arterial blood gas showed severe hypoxia, with sudden fallen of arterial oxygen pressure (PaO2 123 mmHg to 31 mmHg). A suspicion of pulmonary embolism or acute heart failure raised. N-terminal Pro-Brain Natriuretic Peptide and cardiac troponin I were immediately determined but without elevation. An emergent lung spiral computed tomography (CT) scan was performed. No thrombus was obtained but an unexpected malposition of the catheter tip that was complicated with severe bilateral pleural effusion and mild pneumomediastinum (Figure 2). By tracking the position of catheter from IJV till subclavian vein, catheter was found intravascularly located at the entire route of IJV (Figure 2A and Figure 2B) and segment of subclavian vein (Figure 2C and Figure 2D). However, the catheter tip did not proceed to superior vena cava as expected, but distorted and bent forward, and rotated leftward as depicted by the images taken from three-dimensional CT (Figure 3), which clearly illustrated the entire journey of the CVC. During the stay in intensive care unit, intermittent thoracentesis and chest drainage, along with continuous oxygen therapy, analgesia, were immediately implemented. The catheter was gently removed under ultrasound guidance. The vital parameters were monitored. Care was taken to prevent vascular rupture and detachment of thrombosis. All the drainage tubes were removed and the patient was safely transferred to the wards at postoperative day 7.
.
Figure 2: Lung spiral CT scan revealed severe bilateral pleural effusion and mild anterior pneumomediastinum caused by malposition of catheter. Cather was correctly located at the entire route of IJV and segment of subclavian vein (arrow). Approximate 90% of right thorax and less than 50% of left thorax were effused with mixture of blood and total parenteral nutrition demonstrated by drainage analysis (asterisk). No thrombus sign was obtained.
View Figure 2
.
Figure 3: Three-dimensional CT images showing the detail of catheter tip malposition. The catheter tip (arrow) bends upward to the anterior mediastinal (A) and rotates leftward to left pleura (B).
View Figure 3
Discussion
Malposition of catheter is a well-known complication during central venous catheterization. It common occurs after subclavian and left jugular vein cannulation. On the contrary, the incidence of misplacement after right jugular puncture is very low (5.3%) [1]. The incorrect positioning of the catheter via IJV mentioned in the literature including contralateral IJV [2], internal mammary vein [3], azygos arch [4]. These events commonly developed at the moment of placement, and occasionally reported during the long-term maintenance.
This is the first experience of late migration of right IJV catheter in our department. Bending of the catheter is very rare because the right internal jugular vein is the straight route for catheterization to the right atrium. In the present case, the initial position of the catheter is corrected located, which was confirmed by the catheter that was functioning well with blood aspiration and as a canule for anesthetics infusion. Drug effect was obtained intraoperative through administration of sedation/analgesia through this catheter. Central venous pressure monitoring showed no other abnormal findings. The chest X-ray at the same day of post central venous catheterization confirmed the safe positioning of the catheter, but the images reveals that the catheter is inserted very proximal to the mediastinal structures through the jugular (Figure 1), that makes the peri-IJV structure vulnerable to mechanic injuries.
Several factors may contribute to the complications and the catheter late migration. Firstly, encountering early resistance during guidewire insertion could be a clue that the guiderwire is entering the vessel at a steep angle or taking an acute change in course, or maybe the manipulator introduces the wire deeply. Multiple attempts of guidewire insertion may damage the wall of right brachiocephalic vein or superior vena cava, and puncture through right pleura and anterior mediastinal. Blood from the impaled vessels, and drugs/nutrient fluids entered leading into severe pleural effusion and pneumomediastinum. Secondly, positioning change or activities such as weight lifting that require extreme Valsalva maneuvers may lead to catheter migration [5]. Thirdly, spontaneous migration of the soft silastic catheter may be related to its inherent flexibility, which makes catheter displacement when there are sudden changes of central venous pressure during coughing or cardiac arrhythmia [6]. Furthermore, the patient's venous morphology or anatomical variation plays a role in the migration, in that migration is more likely to occur in large caliber jugular veins or if jugular vein forms an obtuse angle with the subclavian vein. Collectively, the violent guidewire threading and catherization, and late migration caused by positioning change or Valsalva maneuvers, along with anatomical variation of vessels could cause these devastating mechanic complications.
Recently, ultrasound-guided catheter placement is demonstrated to be a easiest method for acknowledging the direction of catheter tip, needle and guide wire during the entire catheterizing process [7]. The malposition of the catheter can be prevented by avoiding the left internal jugular/subclavian vein cannulation, limiting the depth of insertion of the guidewire and corrent using of J-shaped guidewire [7,8]. If well trained and properly utilized, ultrasound guidance can increase the success rate, shorten the procedure time and decrease the complication.
In summary, CVC may late migrate and lead to severe complications though initially correct placed. Careful review of early post-catheterization chest radiography and communication with the physician can prevent such an unfortunate event. If there is any problem during the central venous catheterization, ultrasonography can be used for optimal catheter placement and prevention of complications.
Authors' Contributions
Yiheng Wang conceived, researched, and drafted the manuscript. Lixian He performed the literature review and postoperative follow-up. Xiaoling Hu and Zhigang Zhou took charge of anesthetic task. Hong Zhou provided the relevant radiographic images. All authors read and approved the final manuscript.
References
-
Ruesch S, Walder B, Tramer MR (2002) Complications of central venous catheters: internal jugular versus subclavian access--a systematic review. Crit Care Med 30: 454-460.
-
Singh GP, Prabhakar H, Reddy BK (2012) Malposition of internal jugular vein catheter into contralateral internal jugular vein: An uncommon position. Indian J Anaesth 56: 205-207.
-
Sandroni C, Pirronti T, Tortora F, Santangelo S, Rinaldi P, et al. (2003) Unusual central venous catheter malposition into the left internal mammary vein: a case report. Intensive Care Med 29: 2338-2339.
-
Bankier AA, Mallek R, Wiesmayr MN, Fleischmann D, Kranz A, et al. (1997) Azygos arch cannulation by central venous catheters: radiographic detection of malposition and subsequent complications. J Thorac Imaging 12: 64-69.
-
Jahagirdar SM, Laxmimani, Athiraman U, Ravishankar M (2013) Migration of subclavian venous catheter tip: Patient positioning in ICU makes a difference. Indian J Crit Care Med 17: 193-194.
-
Rasuli P, Hammond DI, Peterkin IR (1992) Spontaneous intrajugular migration of long-term central venous access catheters. Radiology 182: 822-824.
-
Denys BG, Uretsky BF, Reddy PS (1993) Ultrasound-assisted cannulation of the internal jugular vein. A prospective comparison to the external landmark-guided technique. Circulation 87: 1557-1562.
-
Wu SY, Ling Q, Cao LH, Wang J, Xu MX, et al. (2013) Real-time two-dimensional ultrasound guidance for central venous cannulation: a meta-analysis. Anesthesiology 118: 361-375.





