International Journal of Critical Care and Emergency Medicine
Pre-Hospital Ultrasound: Current Indications and Future Perspectives
Mirko Zanatta*, Piero Benato and Vito Cianci
Emergency Department, Arzignano Hospital, Italy
*Corresponding author:
Dr. Mirko Zanatta, Emergency Department of Arzignano Hospital, ULSS 5 Ovest Vicentino, Via Parco 1, 36071, Arzignano, Vicenza, Italy, Tel: +390444479261, Email: mirko.zanatta@ulss5.it
Int J Crit Care Emerg Med, IJCCEM-2-019, (Volume 2, Issue 2), Review Article; ISSN: 2474-3674
Received: January 25, 2016 | Accepted: July 18, 2016 | Published: July 20, 2016
Citation: Zanatta M, Benato P, Cianci V (2016) Pre-Hospital Ultrasound: Current Indications and Future Perspectives. Int J Crit Care Emerg Med 2:019. 10.23937/2474-3674/1510019
Copyright: © 2016 Zanatta M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The mission of pre-hospital medical service is to provide rapid and high quality life support. The development of specific protocols, the availability of new diagnostic tools have determined a significant improvement of pre-hospital care. The use of ultrasound in the pre-hospital medical service is a new and reliable diagnostic device.
Pre-hospital ultrasound must have few and focused indications, in order to match rapidity with effectiveness. The FAST approach is extensively and effectively used worldwide and it is useful for the evaluation of either penetrating or blunt trauma of the chest and the abdomen.
Ultrasound has been introduced in the management of cardiac arrest, as assessed in the international guidelines of cardiopulmonary resuscitation.
This paper revises the most important indications and the future perspectives of pre-hospital ultrasound.
Keywords
Pre-Hospital, Ultrasound, FAST, Echocardiography, Lung, Aortic aneurism, Indications, Perspectives
Introduction
The mission of pre-hospital care is to provide rapid and high quality support and to carry the patients to the hospital while preventing complications. Emergency medicine covers pathologies that belong to many sub-specialties, like surgery, orthopedics, internal medicine, cardiology, nephrology, pediatrics, and obstetrics. The management of these conditions can start before the arrival at the hospital. The reduction of the "door to balloon time" for the treatment of ST elevated myocardial infarction (STEMI) is one of the most important examples [1].
The same advantage can be obtained in many other situations [2,3]. Specific protocols have been validated for the management of diseases in the pre-hospital setting and new, smaller, cheaper and portable medical devices are available that can be located inside the ambulance and used outside of the hospital. These include the electrocardiograph, defibrillator, ventilator and echograph (Figure 1).

.
Figure1: Medical devices in a modern ambulance. A) monitor, electrocardiograph and defibrillator; B) ventilator; C) echograph.
View Figure 1
A new generation of small, light and hand-held ultrasound appliances have been developed that produce high quality images. They are available to everybody, can be used everywhere and represent a new and interesting challenge, as well as opportunity, in emergency medical transport. "Outdoor" ultrasound was first used by the military to assist in surgical triage in many remote and austere conditions; an ultrasound system is also installed on the International Space Station [4-7].
These extreme experiences paved the way for pre-hospital ultrasound and it is one of the top five priorities in physician-provided pre-hospital critical care according to the opinion of a consensus meeting of an European expert panel [8].
In these remote settings, the indications should be more focused and goal directed than in-hospital ultrasound. This is critical to match their effectiveness with rapidity. The technical skills are the same or even simpler [9].
This review revises the available evidence and suggests some major indications and future perspectives for prehospital ultrasound.
Methods
The article is a narrative review. A literature revision was conducted both on Medline and as a focused Internet search. The search was limited to English language documents published between January 1, 1990 and January 1, 2016.
Titles and abstracts were firstly reviewed and assessed for inclusion. Then references were scrutinized for relevance and included definitevely in the study.
The selection was based on the following criteria: point of care ultrasound (or critical/portable/ bedside ultrasound), pre-hospital setting, emergency physician and paramedics, diagnostic accuracy, clinical outcome and cost effectiveness. No filters were applied for study type.
Major Indications
Trauma
FAST is the acronym of "Focused Assessment Sonography for Trauma" and represents a worldwide accepted protocol for the management of trauma. It is usually performed during the primary survey, it was introduced in the ATLS protocol and has replaced the diagnostic peritoneal lavage [10-13]. The original FAST was integrated with the Extended-FAST (EFAST) for the evaluation of pneumothorax followed by the FASTER (plus extremities and respiratory tract) and FAST-ABCDE (including breathing, circulation, disabilities, exposure) [14-16]. FAST was successfully used by the military for the management of trauma in the battlefield and is important in pre-hospital care, in car accidents, injures at work, environment disasters and crimes [4-6,17-23].
The most important indications of FAST are the management of penetrating cardiac injuries as well as chest and abdominal blunt and penetrating trauma. Walcher et al. showed that ultrasound is reliable for surgical triage, it has high sensitivity, specificity and accuracy for abdominal bleeding (93%, 99% and 99%, respectively). Some uncertainties remain regarding the management of penetrating injuries of the abdomen because ultrasound cannot identify intestinal lesions. The high sensitivity for bleeding makes FAST a precious technique even in these situations because it prioritizes the management of injured patients [23].
John Ma et al. stressed the importance of a multiple view examinations: sensitivity, specificity and accuracy were 87%, 100% and 98%, respectively, with the standard multiple-view approach. It was 51%, 100% and 93%, respectively, with a single-view approach (Morrison's pouch) [24]. Moreover a second look improves significantly diagnostic accuracy, especially in severe trauma and when clinical conditions change. [17,23,25].
Cardiac ultrasound has 100% sensitivity, 97% specificity, and 97% accuracy for identifying hemopericardium and cardiac tamponade after a penetrating injury of the trunk [18]. In another study by Tayal et al., the specificity and sensitivity reached 100% and were correlated with the need for thoracotomy [26]. Finally lung ultrasound is more accurate than X-ray for the diagnosis of pneumothorax and pleural effusions [20,27,28].
Pre-hospital FAST remains the same as in-hospital FAST, the only difference is that it should be "faster" (Figure 2). Although there are contrasting data about the utility of clinical outcomes (see review by Jorgensen et al. [29]), ultrasound undoubtedly improves the capacity to identify hidden bleeding before hospital admission [23,29]. There are some warnings however, slow and small bleeds cannot be observed in the first 24 hours [30]. However, evaluation of the dynamics of trauma, clinical observations, and the integration with CT scan remain compulsory. Lung sliding should also be monitored, especially in ventilated patients. An occult pneumothorax can increase during ventilation, and it can cause a tension pneumothorax with rapid deterioration of respiratory function during transport if not drained.
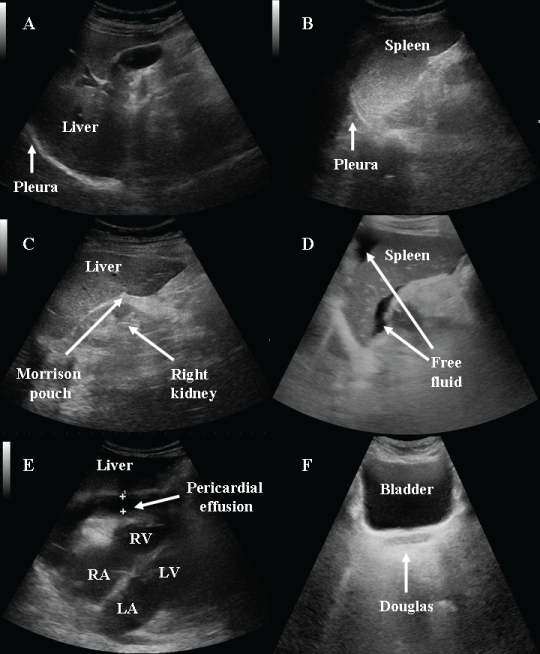
.
Figure 2: FAST. A) a free right pleura; B) left pleura; C) a free morrison pouch; D) free fluid in the perisplenic space; E) pericardial effusion (RV: right ventricle; LV: left ventricle; RA: right atrium; LA: left atrium); F) a free douglas space.
View Figure 2
The identification of severe thoracic and abdominal injuries outside of the hospital can change the patient's care [2]. Treatment can be adapted to the clinical condition of the patient and to the ultrasonographic findings, e.g., fluid therapy according with vena cava collapsibility and heart contractility. The indication to perform invasive procedures can be given such as drainage of a pleural effusion and/or pneumothorax in a patient with respiratory insufficiency and a pericardiocentesis in case of a cardiac tamponade and a pulseless electric activity [26,31,32]. Communication with the in-hospital emergency physicians can be improved including a request for rapid surgical evaluation and blood supply. Evidence of peritoneal effusion is certainly an indication for immediate surgery, but if hemodynamic conditions are stable a CT scan can be immediately prescribed skipping useless examinations. Finally, the ambulance crew can ask for medical centralization towards the nearest "trauma center". The probability of death increases by 1% for every 3 minutes of delay. Thus, faster diagnoses imply a higher probability to save and effectively treat the patient [33].
Lung ultrasound
Lung evaluation is already included within the EFAST to identify traumatic pneumothorax and hemothorax, but it can also be used for the management of non-traumatic respiratory insufficiency [14]. The international recommendations for point-of-care lung ultrasound was published in 2012 and provided important and well-documented evidence about the role of ultrasound in the diagnosis and management of many lung diseases [27].
Pre-hospital lung ultrasound might have just three indications: i) the determination of lung profile (A profile: dry lung; B profile: wet lung) (Figure 3A and Figure 3B), ii) the diagnosis of pleural effusions (Figure 3C) and iii) the identification of a spontaneous pneumothorax. Lung evaluation is very rapid, and physicians can effectively discriminate between a wet and a dry lung and rule in or rule out an interstitial syndrome or a pneumothorax in a few minutes, sometimes in less than 1 minute [9,21,33,34].
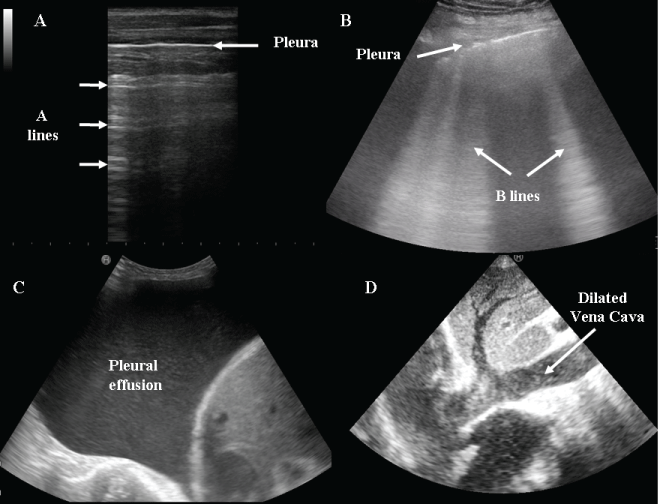
.
Figure 3: Lung ultrasound. A) dry lung: A lines; B) wet lung: multiple B lines in a patient with decompensated heart failure; C) large pleural effusion; D) a dilated inferior vena cava.
View Figure 3
Point-of-care techniques are extremely simplified in comparison to in-hospital protocols. A rapid 2-point technique (upper anterior and basal lateral area) is enough to rule in or rule out an alveolar interstitial syndrome that is characterized by bilateral homogeneous increases in B lines (Figure 3B) [27,35]. Pleural effusions are also easily evaluated (Figure 3C) [9-21].
Many studies have demonstrated the high correlation between B-lines and the diagnosis of interstitial syndrome and the superiority of ultrasound in comparison to standard X-ray for the diagnosis of both interstitial syndrome and pneumothorax [14,27]. Neesse et al. found that pre-hospital chest ultrasound was useful for the differentiation between cardiac heart failure and chronic obstructive pulmonary disease [36]. Consequently, an early diagnosis determines the appropriate pre-hospital pharmacological therapy, ventilation settings, and reduces inappropriate drugs, medical failures and intubations [9,37].
Echocardiography
The application of echocardiography in critically ill patients has been well recognized for several years, especially for the evaluation of blunt or penetrating chest trauma [38]. Pre-hospital critical care echocardiography can be also used in patients without trauma for the identification of pericardial effusions with or without tamponade, for a rapid assessment of heart contractility in patients with hypothension, heart failure and shock [39-42] as well as for the management of cardiac arrest [3,39,40,43-46].
A subxiphoid projection is often sufficient to collect all the required information [47]. An apical view is sometimes necessary in the case of obese patients, severe abdominal pain or meteorism. A sector probe is used for standard echocardiography, but a curvilinear high frequency probe is often used out-of-hospital because the concomitant evaluation of other organs is easier. Data collection is limited to the identification of free fluid in the pericardium, cardiac chamber dimensions, and general heart contractility (Figure 4). The integration of these data with the lung profile and inferior vena cava dimensions and collapsibility significantly improves the diagnostic accuracy in patients with shock and hypotension (Figure 3) [40,41].
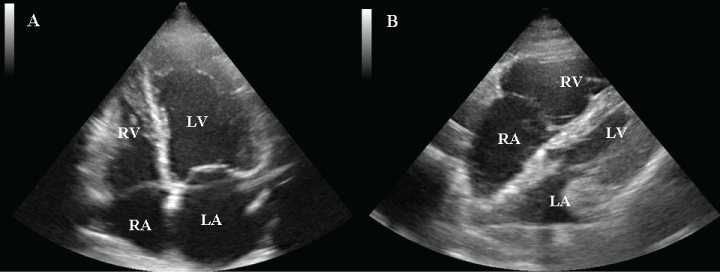
.
Figure 4: A) A dilated and hypokinetic heart; B) right ventricle overload in a patient with acute pulmonary embolism.
View Figure 4
Critical care echocardiography rapidly determines whether the cause of shock and hypotension is cardiac (severe left ventricle dysfunction, right ventricle overload, cardiac tamponade) or non-cardiac (hypovolemia or vasoplegia) (Figure 4) [39,41,42]. Ultrasound was successfully used during cardiopulmonary resuscitation and its role was mentioned in the 2015 international guidelines for cardiopulmonary resuscitation [3,39,43,44,46]. A focused ultrasound assessment should not delay resuscitative interventions but may be considered as an additional diagnostic tool. The FEER study suggested 10-second assessment of the heart during the rhythm check. It showed that no time was wasted during cardiopulmonary resuscitation [44]. Ultrasound was also used to checking the efficacy of heart compressions. It offers important information on the quality of chest compressions and collects cardiac data without stopping CPR [48]. The ability to see the heart during cardiopulmonary resuscitation identifies some reversible causes of cardiac arrest (cardiac tamponade, pulmonary embolism, pseudo-PEA) that must be treated to improve survival rate.
Abdominal ultrasound
Pre-hospital ultrasound is performed in patients with severe abdominal pain to study the abdominal aorta and to search for peritoneal effusion [6,9,17]. Aorta studies are usually very fast (less than 1 minute) even though obesity, abdominal tenderness and intestinal air can limit the examination. In these situations, lateral and/or longitudinal scans using the acoustic windows of the liver and of the left kidney should be exploited to identify the artery.
A dilated aorta is easily identified, whereas the diagnosis of dissection is more difficult. It can sometimes only be predicted by the presence of indirect signs such as free peritoneal fluid (Figure 5). The only chance for a patient with a broken aneurism is a fast diagnosis and surgical treatment: here, pre-hospital critical ultrasound can make the difference.
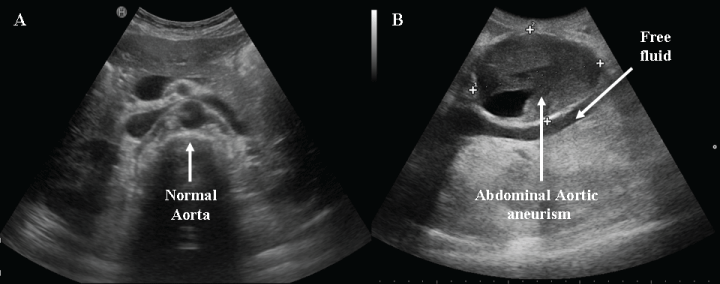
.
Figure 5: A) A normal abdominal aorta; B) a broken aneurism with free fluid behind the posterior wall.
View Figure 5
An appropriate treatment can start in the pre-hospital setting with aggressive fluid replacement, blood pressure control and the use of pain-killers that do not affect platelets activity. Moreover the identification of an aortic aneurism in a patient with abdominal pain and shock helps route the patient to the most appropriate hospital [49].
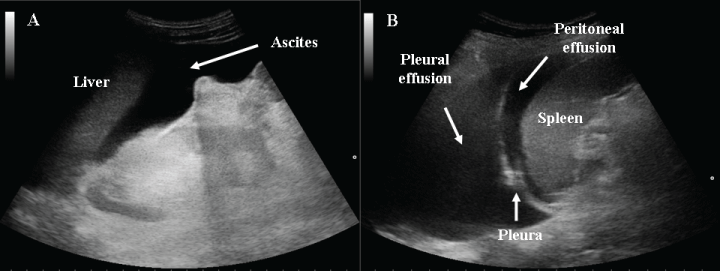
Free abdominal fluid in subjects without an aortic aneurysm, can be a complication of blunt abdominal trauma or the manifestation of many abdominal pathologies. Non-traumatic sources of intraperitoneal fluid must be carefully investigated including ascites in liver disease or peritoneal carcinomatosis, acute inflammatory bowel diseases, appendicitis, and pelvic free fluid in pregnant women or in young and healthy women (Figure 6).
.
Figure 6: A) Ascites in a patient with hepatic cirrhosis; B) peritoneal and pleural effusion in a woman with an end stage ovarian carcinoma.
View Figure 6
In all of these situations, the combination of ultrasound with patient history and clinical assessment becomes crucial for the correct interpretation of images.
Future Perspectives
Airways
Airway management is one of the most difficult challenges in emergency medicine, especially in the pre-hospital setting where diagnostic and therapeutic resources are low. Difficult airways improve the risk of respiratory insufficiency and reduce the resuscitation success rate. Ultrasound was successfully used for the diagnosis of some pathologies of the upper airway , for the evaluation of trauma of the head and the neck and for airway management [50-53].
Real-time monitoring of endotracheal intubation and the presence of bilateral lung sliding confirm the correct positioning of the tube. Standard management based on auscultation and capnography remains the gold standard, but noisy environments hamper the auscultation, and capnography is not always available [46,47,54]. Ultrasound can easily identify crico-thyroid membrane and the first tract of the trachea as well as can guide cricothyrotomy and tracheostomy [55,56]. This opportunity is extremely important in those patients with a difficult anatomy of the neck such as obese patients, those with a deviation of the trachea for masses of the neck, or severe trauma patients [55].
Cerebral diseases
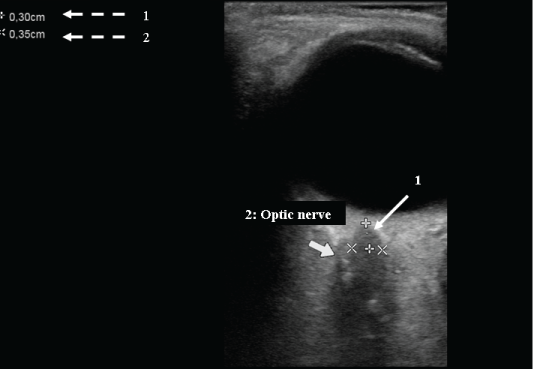
Patients with trauma of the head, severe headache, neurological impairment or persistent coma could be evaluated for intracranial hypertension with ultrasound. Intracranial pressure can be estimated by measuring the optic nerve diameter, 3 mm distal to the optic disk, with a low frequency linear probe (Figure 7). An increased intracranial pressure is supposed when the diameter of the nerve is larger than 5 mm [56,57]. Optic nerve identification and measurements are simple and reproducible. The correlation with intracranial hypertension is high but the real utility in acute patients is still under investigation. The majority of studies suggest the use of optic nerve diameters for monitoring patients inside the intensive care unit [56,57].
.
Figure 7: Optic nerve diameter. 1: the diameter measured 3 mm distal to the optic disk. 2: the size of the optic nerve (0.35 cm).
View Figure 7
Transcranial Doppler is another application for the diagnosis of cerebral ischemia in traumatic brain injuries [58]. It detects an impaired cerebral perfusion that should be treated more aggressively to restore an adequate cerebral perfusion through the adjustment of blood pressure or with hyperosmotic solutions. Although it directly represents cerebral perfusion, it is not as simple as optic nerve evaluation. It requires expert hands, and the images are not often sufficiently clear.
Triage
Triage is increasingly important in high patient numbers. The ability to correctly evaluate and categorize wounded patients identifies those who need to be transported urgently to a hospital for care, to which hospital, who can be postponed, and those who do not need hospital care [11,23,59]. This is especially critical in crowded and noisy environments such as disasters or mass casualty situations.
Some papers have demonstrated the utility of portable ultrasound for the management of trauma, in the battlefield, in military setting, in austere conditions and in multi-casualty events [4-6,9,23,60]. The management of resources can be improved too such as the request of other means of transport like a helicopter or other ambulances.
Obstetrics emergencies
In 2004 a screening examination named "The Fetal Evaluation for Transport with Ultrasound (FETUS)" was introduced in the helicopter during air transport for high-risk obstetrics cases to evaluate fetal heart rate, position, movement and condition of placenta [60]. Traditional evaluation with Doppler stethoscope is not possible in noisy situations like those in a helicopter or ambulance. On the contrary, ultrasound is always available and is not influenced by the means of transport. It can be repeated easily if necessary [60].
Wireless and satellite transmission
Pre-hospital ultrasound is increasingly needed for remote image reading. The possibility to send images using wireless or satellite transmission to the hospital emergency physician for remote evaluation is under evaluation [61,62]. According to published data, the transmitted data resulted in no degradation in image quality and offers an accurate interpretation at a distance by emergency physicians [61].
Both physicians and paramedics can acquire the data. This facilitates a new and interesting opportunity for widespread ultrasound use worldwide, especially in remote and poor regions. Paramedics or technicians can be trained to learn the correct technique for the acquisition of images, which can then be sent for remote interpretation. An ultrasound system is already installed on the International Space Station, and non-physician crew acquire all target images without difficulty after a specific and rapid training [7].
Conclusion
Ultrasound is a new and interesting opportunity for pre-hospital medical service. It significantly improves the management of pre-hospital care and reduces the "door to diagnosis and therapy time", which is one of the most important factors in improving medical assistance and survival.
The first recommendation of pre-hospital ultrasound is rapidity, if used correctly, it will certainly improve the management of patients and precious time will be saved.
Therefore, the examination must be rapid, not more than 2-3 minutes. For example, pre-hospital FAST usually takes no more than 3 minutes [23]. The identification of lung sliding, the diagnosis of pneumothorax, and the evaluation of abdominal aorta usually lasts less than 1 minute [14,33]. Heart studies during cardiopulmonary resuscitation should be performed in 10 seconds during the rhythm check. Alternatively, images and video clips can be recorded and analyzed later while RCP is ongoing [44].
Technical skills are the same or even simpler than in-hospital critical ultrasound. The exam should answer specific yes/no questions, i.e., Is there a pneumothorax? Is there free fluid in the pleura, pericardium, peritoneum? Is there an aortic aneurism? Are the lungs wet or dry?
The indications must be few and well-defined to combine effectiveness and speed. Trauma, respiratory insufficiency, shock, cardiac arrest and severe abdominal pain, to rule in or rule out an abdominal aortic aneurism, are situations where pre-hospital ultrasound makes the difference [9-13,21,34,54].
There are also promising and valuable perspectives regarding some other indications, such us pre-hospital triage, airway management, obstetric emergencies and in wireless and satellite transmission [7,9,17-23,54-56,60-62]. Some studies evaluated the possibility to extend the use of ultrasound to paramedics, with few and well defined indications. Paramedics were able to obtain adequate images and to perform examinations as accurate as those performed by physicians. However, further researches are necessary to confirm these findings [13,63].
The rapid spread of critical ultrasound has focused attention on training [16]. In the last decade, specific recommendations were published for lung ultrasound, critical care echocardiography, and ultrasound-guided central venous catheterization [13,16,27,47,64]. Moreover critical ultrasound has evolved from an "organ-based" to a "problem-based approach" (aortic aneurism, pneumothorax, and hydroneprhosys) to a "syndrome based approach" (hypotension, cardiac arrest, respiratory insufficiency, and trauma). Finally, global patient management has emerged as theorized by Neri et al. in the FAST-ABCDE [16]. Therefore, technical capabilities must be integrated with a good knowledge of anatomy, physiopathology and pathology. A tighter link among these elements increases the effectiveness of point-of-care critical ultrasound.
Pre-hospital ultrasound still has some limitations. First, international guidelines and a specific training are still lacking. There is no worldwide agreement on pre-hospital ultrasound yet. Also, diagnostic capability is well known, but some doubts remain regarding the real impact on outcome and survival. Moreover there isn't any relevant evidence regarding the cost-effectiveness of pre-hospital ultrasound.
There are also some technical limitations such as adverse environmental conditions (luminosity with no possibility to obscure the area of the screen and rainy/snowy weather) and narrow/confined spaces inside the ambulance or the helicopter that can limit the number of scans and the possibility to move the patient. There are also patients with specific needs for assistance or with a reduced available "body surface" such as those trapped inside a vehicle or with severe injuries including crushed, degloved or mangled extremities or active bleeding.
Finally the study design of this revision has some limitations: it doesn't consider some important confounders, such us study settings, type of patients, quality of ultrasound appliances, expertise of physicians and paramedics.
References
-
McNamara RL, Wang Y, Herrin J, Curtis JP, Bradley EH, et al. (2006) Effect of door-to-balloon time on mortality in patients with ST-segment elevation myocardial infarction. J Am Coll Cardiol 47: 2180-2186.
-
Gomes E, Araujo R, Carneiro A, Dias C, Costa-Pereira A, et al. (2010) The importance of pre-trauma centre treatment of life-threatening events on the mortality of patients transferred with severe trauma. Resuscitation 81: 440-445.
-
Nolan JP, Soar J, Cariou A, Cronberg T, Moulaert VR, et al. (2015) European Resuscitation Council and European Society of Intensive Care Medicine 2015 guidelines for post-resuscitation care. Intensive Care Med 41: 2039-2056.
-
Brooks AJ, Price V, Simms M (2005) FAST on operational military deployment. Emer Med J 22: 263-265.
-
Peoples GE, Gerlinger T, Craig R, Burlingame B (2005) Combat casualties in Afghanistan cared for by a single Forward Surgical Team during the initial phases of Operation Enduring Freedom. Mil Med 170: 462-468.
-
Nelson BP, Melnick ER, LI J (2011) Portable ultrasound for remote environments, part II: current indications. J Emerg Med 40: 313-321.
-
Sargsyan AE, Hamilton DR, Jones JA, Melton S, Whitson PA, et al. (2005) FAST at MACH 20: clinical ultrasound aboard the International Space Station. J Trauma 58: 35-39.
-
Fevang E, Lockey D, Thompson J, Lossius HM, Torpo Research Collaboration (2011) The top five research priorities in physician-provided pre-hospital critical care: a consensus report from a European research collaboration. Scand J Trauma Resusc Emerg Med 19-57.
-
Zanatta M, Cianci V, Benato P, De Battisti S (2014) Pre-hospital critical ultrasound: utility, indications and limitations.
-
Wherrett LJ, Boulanger BR, McLellan BA, Brenneman FD, Rizoli SB, et al. (1996) Hypotension after blunt abdominal trauma: the role of emergent abdominal sonography in surgical triage. J Trauma 41: 815-820.
-
Rozycki GS, Feliciano DV, Ochsner MG, Knudson MM, Hoyt DB, et al. (1999) The role of ultrasound in patients with possible penetrating cardiac wounds: a prospective multicenter study. J Trauma 46: 543-552.
-
Scalea TM, Rodriguez A, Chiu WC, Brenneman FD, Fallon WF Jr, et al. (1999) Focused Assessment with Sonography for Trauma (FAST): results from an international consensus conference. J Trauma 46: 466-472.
-
Heegaard W, Hildebrandt D, Spear D, Chason K, Nelson B, et al. (2010) Prehospital ultrasound by paramedics: results of field trial. Acad Emerg Med 17: 624-630.
-
Kirkpatrick AW, Sirois M, Laupland KB, Liu D, Rowan K, et al. (2004) Hand-held thoracic sonography for detecting post-traumatic pneumothoraces: the Extended Focused Assessment with Sonography for Trauma (EFAST). J Trauma 57: 288-295.
-
Dulchavsky SA, Henry SE, Moed BR, Diebel LN, Marshburn T, et al. (2002) Advanced ultrasonic diagnosis of extremity trauma: the FASTER examination. J Trauma 53: 28-32.
-
Neri L, Storti E, Lichtenstein D (2007) Toward an ultrasound curriculum for critical care medicine. Crit Care Med 35: S290-304.
-
Hoyer HX, Vogl S, Schiemann U, Haug A, Stolpe E, et al. (2010) Prehospital ultrasound in emergency medicine: incidence, feasibility, indications and diagnoses. Eur J Emerg Med 17: 254-259.
-
Bush M (2006) Portable ultrasound in pre-hospital emergencies: a feasibility study. Acta Anaesthesiol Scand 50: 754-758.
-
Taylor J, McLaughlin K, McRea A, Lang E, Anton A (2014) Use of Prehospital ultrasound in North America: a survey of emergency medical services medical directors. BMC Emerg Med 14: 6.
-
Knudsen L, Sandberg M (2011) Ultrasound in pre-hospital care. Acta Anaesthesiol Scand 55: 377-378.
-
Neesse A, Jerrentrup A, Hoffmann S, Sattler A, Gorg C, et al. (2012) Prehospital chest emergency sonography trial in Germany: a prospective study. Eur J Emerg Med 19: 161-166.
-
Mazen J El Sayed, Elie Zaghrini (2013) Prehospital emergency ultrasound: a review of current clinical applications, challenges, and future implications. Emerg Med Int.
-
Walcher F, Weinlich M, Conrad G, Schweigkofler U, Breitkreutz R, et al. (2006) Prehospital ultrasound imaging improves management of abdominal trauma. Br J Surg 93: 238-242.
-
Ma OJ, Kefer MP, Mateer JR, Thoma B (1995) Evaluation of hemoperitoneum using a single-vs multiple-view ultrasonographic examination. Acad Emerg Med 2: 581-586.
-
Miller MT, Pasquale MD, Bromberg WJ, Wasser TE, Cox J (2003) Not so FAST. J Trauma 54: 52-59.
-
Tayal VS, Beatty MA, Marx JA, Tomaszewski CA, Thomason MH (2004) FAST (focused assessment with sonography in trauma) accurate for cardiac and intraperitoneal injury in penetrating anterior chest trauma. J Ultrasound Med 23: 467-472.
-
Volpicelli G, Elbarbary M, Blaivas M, Lichtenstein DA, Mathis G, et al. (2012) International evidence-based recommendations for point-of-care lung ultrasound. Intensive Care Med 38: 577-591.
-
Volpicelli G, Boero E, Sverzellati N, Cardinale L, Bussi M, et al. (2014) Semi-quantification of pneumothorax volume by lung ultrasound. Intensive Care Med 40: 1460-1467.
-
Jorgensen H, Jensen CH, Dirks J (2010) Does prehospital ultrasound improve treatment of the trauma patient? A systematic review. Eur J Emerg Med 17: 249-253.
-
Byhahn C, Bingold TM, Zwissler B, Maier M, Walcher F (2008) Pre-hospital ultrasound detects pericardial tamponade in pregnant victim of stabbing assault. Resuscitation 76: 146-148.
-
Heegaard W, Hildebrandt D, Reardon R, Plummer D, Clinton J, et al. (2009) Pre-hospital ultrasound diagnosis of traumatic pericardial effusion. Acad Emerg Med 16: 364.
-
Calrke JR, Trooskin SZ, Doshi PJ, Greenwald L, Mode CJ (2002) Time to laparotomy for intra-abdominal bleeding from trauma does affect survival for delays up to 90 minutes. J Trauma 52: 420-425.
-
Lyon M, Walton P, Bhalla V, Shiver SA (2012) Ultrasound detection of the sliding lung sign by prehospital care provider. Am J Emerg Med 30: 485-488.
-
Zechner PM, Aichinger G, Riguad M, Wildner G, Prause G (2010) Prehospital lung ultrasound in the distinction between pulmonary edema and exacerbation of chronic obstructive pulmonary disease. Am J Emerg Med 28: 389.
-
Copetti R, Soldati G, Copetti P (2008) Chest sonography: a useful tool to differentiate acute cardiogenic pulmonary edema from acute respiratory distress syndrome. Cardiovasc Ultrasound 6: 16.
-
Neesse A, Jerrentrup A, Hoffmann S, Sattler A, Gorg C, et al. (2012) Prehospital chest emergency sonography trial in Germany: a prospective study. Eur J Emerg Med 19: 161-166.
-
Ferrari G, Esquinas AM (2015) Lung ultrasound in prehospital acute cardiac pulmonary edema: a new practical toll for CPAP assessment. Eur J Emerg Med 22: 146-147.
-
Jimenez E, Martin M, Krukenkamp I, Barret J (1990) Subxiphoid pericardiotomy versus echocardiography; a prospective evaluation of the diagnosis of occult penetrating cardiac injury. Surgey 108: 676-679.
-
Perera P, Mailhot T, Riley D, Mandavia D (2010) The RUSH exam: Rapid Ultrasound in SHock in the evaluation of the critically III. Emerg Med Clin North Am 28: 29-56.
-
Volpicelli G, Lamorte A, Tullio M, Cardinale L, Giraudo M, et al. (2013) Point-of-care multiorgan ultrasonography for the evaluation of undifferentiated hypotension in the emergency department. Intensive Care Med 39: 1290-1298.
-
D Lichtenstein (2013) FALLS-protocol: lung ultrasound in hemodynamic assessment of shock. Heart Lung Vessel 5: 142-147.
-
Haydar SA, Moore ET, Higgins GL 3rd, Irish CB, Owens WB, et al. (2012) Effect of bedside ultrasonography on the certainty of physician clinical decision making for septic patients in the emergency department. Ann Emerg Med 60: 346-358.
-
Hernandez C, Shuler K, Hannan H, Sonyika C, Likourezos A, et al. (2008) C.A.U.S.E.: Cardiac arrest ultra-sound exam-a better approach to managing patients in primary non-arrhythmogenic cardiac arrest. Resuscitation 76: 198-206.
-
Breitkreutz R, Walcher F, Seeger FH (2007) Focused echocardiographic evaluation in resuscitation management: concept of an advances life support-conformed algorithm. Crit Care Med 35: S150-161.
-
Aichinger G, Zechner PM, Prause G, Sacherer F, Wildner G, et al. (2012) Cardiac movement identified on pre-hospital echocardiography predicts outcome in cardiac arrest patients. Prehosp Emerg Care 16: 251-255.
-
Neumar RW, Shuster M, Callaway CW, Gent LM, Atkins DL, et al. (2015) Part 1: Executive Summary: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 132: S315-67.
-
Price S, Via G, Sloth E, Guarracino F, Breitkreutz R, et al. (2008) Echocardiography practice, training and accreditation in the intensive care: document for the World Interactive Network Focused on Critical Ultrasound (WINFOCUS). Cardiovasc Ultrasound 6: 49.
-
Zanatta M, Benato P, Cianci V (2015) Ultrasound guided chest compressions during cardiopulmonary resuscitation. Resuscitation 87: e13-e14.
-
Mazur SM, Sharley P (2007) The use of point of care ultrasound by critical care retrieval team to diagnose acute abdominal aortic aneurysm in the field. Emerg Med Australas 19: 71-75.
-
Kristensen MS (2011) Ultrasonography in the management of the airway. Acta Anaesthesiol Scand 55: 1155-1173.
-
Ko DR, Chung YE, Park I, Lee HJ, Park JW, et al. (2012) Use of bedside sonography for diagnosing acute epiglottitis in the emergency department: a preliminary study. J Ultrasound Med 31: 19-22.
-
Bisetti MS, Segala F, Zappia F, Albera R, Ottaviani F, et al. (2009) Non-invasive assessment of benign vocal folds lesions in children by means of ultrasonography. Int J Pediatr Otorhinolaryngol 73: 1160-1162.
-
Jakubowska A, Zawadzka-Glos L, Brewski M (2011) Usefulness of ultrasound examination in larynx traumas in children. Pol J Radiol 76: 7-12.
-
Brun PM, Besserau J, Cazes N, Querrelou E, Chenaitia H (2012) Lung ultrasound associated to capnography to verify correct endotracheal tube positioning in prehospital. Am J Emerg Med 30: 2080.e5-6.
-
Siddiqui N, Arzola C, Friedman Z, Guerina L, You-Ten KE (2015) Ultrasound improves Cricothyrotomy Success in Cadavers with Poorly Defined Neck Anatomy: A Randomized Control Trial. Anesthesiology 123: 1033-1041.
-
Dubourg J, Javouhey E, Geeraerts T, Messerer M, Kassai B (2011) Ultrasonography of optic nerve sheath diameter for detection of raised intracranial pressure: a systematic review and meta-analysis. Intensive Care Med 37: 1059-1068.
-
Rajajee V, Fletcher JJ, Rochlen LR, Jacobs TL (2012) Comparison of accuracy of optic nerve ultrasound for the detection of intracranial hypertension in the setting of acutely fluctuating vs stable intracranial pressure: post-hoc analysis of data from a prospective, blinded single center study. Crit Care 16: R79.
-
Tazarourte K, Atchabahian A, Tourtier JP, David JS, Ract C, et al. (2011) Pre-hospital transcranial Doppler in severe traumatic brain injury: a pilot study. Acta Anaesthesiol Scand 55: 422-428.
-
Tazarourte K, Dekadjevi H, Sapir D, Desmettre T, Libert N, et al. (2010) Ultrasound and pre-hospital triage: a tool for limiting the undertriage. J Trauma 69: 997.
-
Polk JD, Merlino JI, Kovach BL, Mancuso C, Fallon WF Jr (2004) Fetal evaluation for transport by ultrasound performed by air medical teams: a case series. Air Med J 23: 32-34.
-
Strode CA, Rubal BJ, Gerhardt RT, Bulgrin JR, Boyd SY (2003) Wireless and satellite transmission of prehospital focused abdominal sonography for trauma. Prehosp Emerg Care 7: 375-379.
-
Su MJ, Ma HM, Ko CI, Chiang WC, Yang CW, et al. (2008) Application of tele-ultrasound in emergency medical services. Telemed J E Health 14: 816-824.
-
Brooke M, Walton J, Scutt D (2010) Paramedics application of ultrasound in the management of patients in the prehospital setting: a review of the literature. Emerg Med J 27: 702-707.
-
Lamperti M, Bodenham AR, Pittiruti M, Blaivas M, Augoustides JG, et al. (2012) International evidence-based recommendations on ultrasound-guided vascular access. Intensive Care Med 38: 1105-1117.





