International Journal of Cancer and Clinical Research
Primitive Fallopian Tube Carcinosarcoma: Three Cases with Immunohistochemical Profiling
Mira Akiki1, Fereshteh Farkhondeh1, Virginie Fourchotte2 and Xavier Sastre-Garau1
1Institut Curie, Department of BioPathology, France
2Institut Curie, Department of Surgery, France
*Corresponding author:
Xavier Sastre-Garau, Institut Curie, Department of BioPathology, 26 rue d'Ulm, 75248, Paris, Cedex 05, France, Tel: +33-1-44-32-42-50, E-mail: xavier.sastre@curie.fr
Int J Cancer Clin Res, IJCCR-2-011, (Volume 2, Issue 1), Case Report; ISSN: 2378-3419
Received: January 13, 2015 | Accepted: January 20, 2015 | Published: January 22, 2015
Citation: Akiki M, Farkhondeh F, Fourchotte V, Sastre-Garau X (2015) Primitive Fallopian Tube Carcinosarcoma: Three Cases with Immunohistochemical Profiling. Int J Cancer Clin Res 2:011. 10.23937/2378-3419/2/1/1011
Copyright: ©2015 Akiki M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Most carcinosarcoma, formerly designed as Malignant Mixed Mullerian Tumors are found in the uterus or the ovary, but rarely in the fallopian tube. The histogenesis of this type of tumor and its place regarding serous or poorly differentiated carcinoma are discussed. We document here three typical cases primarily developed in the fallopian tube. The patients were 69, 70 and 82 years old. They all presented with abdominal pain and large unilateral adnexal mass apparently confined to the ovary. Bilateral salpingo-oophorectomy was performed in all cases. Macroscopically, the tumors were located on the fimbriae in two cases and on the fallopian tube in one. They presented cystic and solid components. In addition, in one case, vegetations were present on the serosal surface of the homolateral ovary whereas both ovaries were normal in the two other cases. Microscopically, tumors were classified as carcinocarcoma with heterologous component in two cases and as homologous carcinosarcoma in one. All tumors showed immunoreactivity for cytokeratins, p53, and CD10 and, in two cases, immunoreactivity for S100 was also observed. The tumor located in the fallopian tube was associated with p53 positive intra-epithelial neoplasia in the contralateral fimbriae. The vegetations observed on the surface of the homolateral ovary in one case corresponded to a focus of high grade serous carcinoma.
As high grade serous carcinoma, carcinosarcoma can derive from the fimbria of the Fallopian tube.
Keywords
Fallopian tube; Fimbriae; Carcinosarcoma; Malignant Mixed Mullerian Tumor (MMMT); Intraepithelial Neoplasia.
Introduction
Systematic histopathological analysis of salpingo-ovariectiomy specimens removed in the context of preventive surgery for women with familial susceptibility to ovarian cancer has led to the incidental discovery of infra-clinical neoplasia of Fallopian tubes [1]. Further studies have identified the fimbria as a site of origin for tubal intraepithelial carcinoma [2]. The Fallopian tube as a site of origin for a large proportion of high grade serous carcinoma of the pelvis is now well recognized [3]. Malignant Mixed Mullerian Tumors (MMMT)/carcinosarcoma represent a rare type of tumors, characterized by specific histology and severe outcome, most frequently encountered in the endometrium or in the ovary in elderly women. This tumor type is rarely observed in the Fallopian tube. We report here three cases of primitive Fallopian tube MMMT. The immunophenotypic profile was based on the analysis of epithelial (cytokeratin AE1/AE3) and stromal (CD10) markers. The search of heterologous mesenchymal component was performed using anti- S100, desmin, myogenin, smooth actin, cKit antibodies and that of sex-cord component with anti-inhibin antibody. P53 status was also documented as frequently altered in high grade serous carcinoma.
Cases
Case 1
A 70 year old, gravida 1, para 1, postmenopausal French woman presented with abdominal pain. Her past medical and surgical history was unremarkable. As for her family history, she had a sister who died from disseminated cancer of unknown origin. Gynecologic examination revealed right adnexal mass confirmed by computed tomography (CT) requiring bilateral salpingo-oophorectomy.
Gross description: A solid cystic tumor mass measuring 8 x 5 x 4cm involving the distal part of the right fallopian tube. The cut surface was solid and cystic, tannish-white with necrotic foci (Figure 1). A 0.8 cm pediculated polypoid mass was noted on the serosal surface of the right ovary. The left adnexa showed no macroscopic abnormalities. One month later, the patient was operated for hysterectomy and proctectomy. Grossly, a large tumor mass adherent to the rectum was observed. Cut section showed that the rectal mucosa was not invaded by this tumor and that the endometrial cavity was free of tumor.
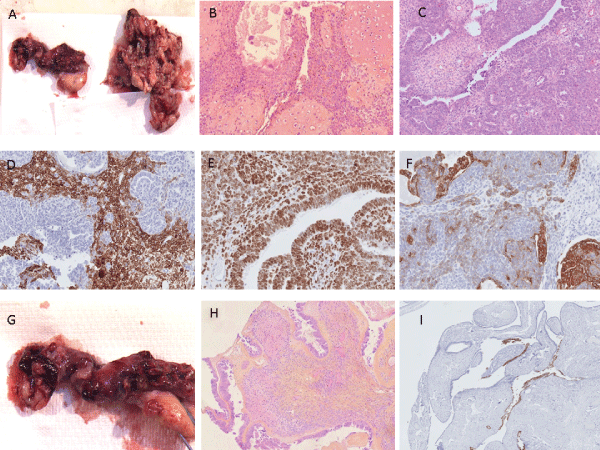
Figure 1: Malignant Mixed Mullerian Tumors (MMMT)/ Carcinosarcomas of the fallopian. A: Tumor separated from the fimbriae of the right fallopian tube,
gross description. B and C: Carcinosarcoma with epithelial and stromal components as well as a component of cartilage (_200). D: CD10 staining for the
stromal component (_200). E: P53 staining for the glandular and stromal component (_200). F: Pancytokeratine staining for the epithelial component. G, H
and I: vegetated mass noted on the serosal surface of the right ovary corresponds to a borderline non invasive papillary serous carcinoma stained strongly
positive for P53 (_200).
View Figure 1
Microscopic description: The tumor was limited to the distal part of the right fallopian tube. It consisted mostly of an epithelial component with features of moderately to poorly differentiate serous papillary carcinoma. The mesenchymal component was a large areas of chondrosarcoma admixed with undifferentiated stromal sarcoma. Lesions of serous carcinoma in situ were noted just at the distal part of the bilateral fallopian. The proximal part of the bilateral fallopian tubes showed no histological abnormalities. The vegetated mass noted on the serosal surface of the right ovary corresponds to a borderline non invasive papillary serous tumor. The axis of this vegetation was composed of an ovarian stroma. The left ovary showed no histological abnormalities. This malignant proliferation invaded the rectal wall from the outside layer until the muscularis propria. The endometrium was atrophic.
Immunohistochemical analysis revealed the epithelial component to be positive for Cytokeratin AE1/AE3 and negative for estrogen and progesterone receptors. The mesenchymal component was markedly positive for S100 in the chondrosarcomal areas and focally positive for CD10 in the undifferenciated sarcoma areas. Both components were negative for desmin, myogenin and smooth muscle antigen. The serous carcinoma in situ found on the fimbriae of the left fallopian tube and admixed to the right carcinosarcomatous mass were strongly positive for P53.
Case 2
A 69 year old, gravida 4, para 3, postmenopausal French woman presented with abdominal pain. Her past medical and surgical history was unremarkable. As for her family history, her father had colon cancer. Gynecologic examination revealed right adnexal mass confirmed by computed tomography (CT) requiring bilateral salpingo-oophorectomy.
Gross description: A solid cystic tumor mass measuring 19 x 8 x3 cm involving the distal part of the right fallopian tube. The cut surface was solid and cystic, tannish-white with necrotic foci. The right ovary and the left adnexa showed no macroscopic abnormalities (Figure 2).
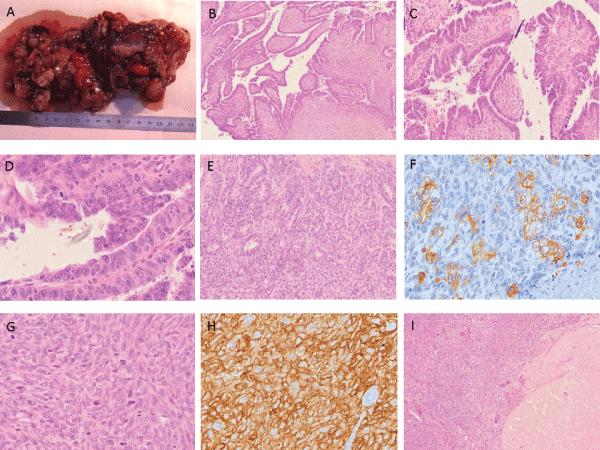
Figure 2: Malignant Mixed Mullerian Tumors (MMMT)/ Carcinosarcomas of the fallopian. A: Solid cystic tumor mass with necrotic foci involving the distal part
of the right fallopian tube. B, C and D: Intra-epithelial neoplasia of the fimbriae of the right fallopian tube (_200 for B and C, _400 for D). E and F: Glandular
component strongly positive for Cytokeratine AE1/AE3 (_200 for E,_400 for F). G and H: Stromal component strongly positive for CD10 (_400). I: Right ovary.
View Figure 2
Microscopic description: The tumor was limited to the distal part of the right fallopian tube. It consisted mostly of an epithelial component with moderately to poorly differentiated serous papillary carcinoma admixed with undifferentiated endometrial stromal sarcoma. The proximal part of the right fallopian tube, the right ovary and the left adnexa showed no histological abnormalities.
Immunohistochemical analysis revealed the epithelial component to be positive for Cytokeratin AE1/AE3 and negative for estrogen and progesterone receptors. The mesenchymal component was markedly positive for CD10. Both components were negative for desmin, myogenin, smooth muscle antigen, c-Kit, inhibine, S100, factor VIII, estrogen and progesterone receptors and c-erb B2. A diagnosis of primary right homologous MMMT with serous carcinoma and undifferentiated endometrial stromal sarcoma was done.
Case 3
An 82 year old, gravida 3, para 3, postmenopausal French woman presented with abdominal pain and distention. Her past medical and surgical history was unremarkable. As for her family history, her father had rectal cancer. Gynecologic examination revealed left adnexal mass confirmed by computed tomography (CT) requiring bilateral salpingo-oophorectomy.
Gross description: A 16 x 8 x 6cm solid cystic tumor mass, involving the distal part of the left fallopian tube. The cut surface was solid and cystic, tannish-white with necrotic foci (Figure 3). The left ovary and the right adnexa showed no macroscopic abnormalities.
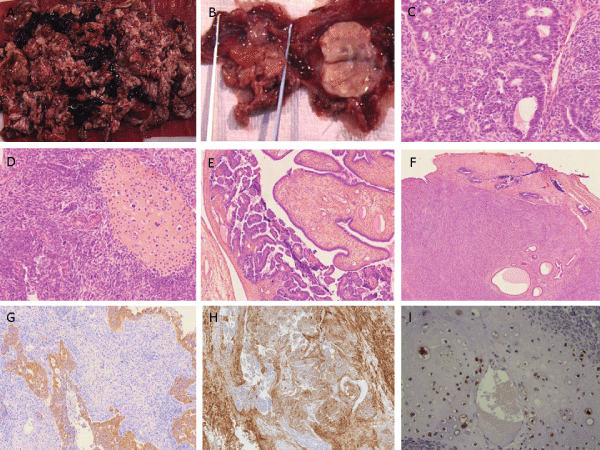
Figure 3: Malignant Mixed Mullerian Tumors (MMMT)/ Carcinosarcomas of the fallopian. A and B: Solid cystic tumor mass with necrotic foci involving the distal
part of the left fallopian tube. The homolateral ovary shows no macroscopic abnormalities. C and D: Carcinosarcoma with epithelial and stromal components as
well as a component of cartilage (_200). E: Intra-epithelial neoplasia of the left fallopian tube (_100). F: The invasive tumor extending superficially and focally
to the serosal surface of the homolateral ovary without invading the ovarian parenchyma (_100). G: Pancytokeratine staining for the epithelial component. H:
CD10 staining for the stromal component. I: PS100 staining for the cartilage component.
View Figure 3
Microscopic description: The invasive tumor was limited to the distal part of the left fallopian tube, extending superficially and focally to the serosal surface of the proximal part of the same fallopian tube and to the serosal surface of the left ovary without invading the ovarian parenchyma. The tumor consisted mostly of an epithelial component with moderately differentiated serous papillary carcinoma admixed with undifferentiated endometrial stromal sarcoma and areas of chondrosarcoma. The right adnexa showed no histological abnormalities.
Immunohistochemical analysis revealed the epithelial component to be positive for Cytokeratin AE1/AE3. The mesenchymal component was markedly positive for CD10. The areas of chondrosarcoma were positive for S100. Both components were negative for desmin, myogenin, smooth muscle antigen, c-Kit and inhibine. A diagnosis of primary left heterologous MMMT with serous carcinoma, undifferentiated endometrial stromal sarcoma and chondrosarcoma was done.
Discussion
MMMT/Carcinosarcoma is a mixed tumor composed of malignant glands and malignant mesenchyme. The annual incidence of about 0.25 cases per million women [4]. It may be found anywhere along the female genital tract, and, although much more common in the endometrium and ovary, some cases have been reported in the fallopian tube [5-9. This tumor was traditionally divided into “homologous” and “heterologous” based on the absence or presence of the mesenchymal component that was intrinsic or extrinsic of the primary site. Previously, it was believed that heterologous carcinosarcomas carried a worse prognosis, but recent evidence suggests that this histological feature does not significantly alter the prognosis. The histogenesis of carcinosarcoma has been a matter of speculation and debate [10]. Uterine MMMTs are currently considered as metaplastic carcinomas because of the expression of epithelial markers such as keratins and EMA by the mesenchymal component [11]. The term of carcinosarcoma is now preferred. Compared with tubal adenocarcinomas, primary MMMTs arising in the fallopian tube are extremely rare malignancies, accounting for fewer than 4 % [12]. MMMTs of the fallopian tube frequently occur in post-menopausal women and generally the presenting symptoms are variable and non-specific, but most commonly include abdominal pain and distention, abnormal vaginal bleeding or discharge. Carcinosarcomas of the tube are often relatively small when diagnosed. Larger tumors are difficult to distinguish from ovarian primaries. They appear grossly as polypoid growths filling the lumen of the tube, often with areas of hemorrhage and necrosis. Microscopically, carcinosarcoma discloses a malignant epithelial element which may or may not have the pattern of a serous adenocarcinoma, together with a mesenchymal element. As in the endometrium and ovary, together with a mesenchymal element may be homologous, containing elements indigenous to the endometrium, ovary and the fallopian tube, or heterologous, containing elements foreign to the endometrium, ovary and the fallopian tube such as cartilage and striated muscle.
The first and the third cases were diagnosed as heterologous carcinosarcoma of the fallopian tube with moderately to poorly differentiated serous papillary carcinoma, chondrosarcoma and undifferentiated endometrial stromal sarcoma. The second case was diagnosed as homologous carcinosarcoma of the fallopian tube with moderately to poorly differentiated serous papillary carcinoma and endometrial stromal sarcoma. In the first case, intraepithelial neoplastic lesions were noted on the distal part of the contralateral fallopian tube and were strongly positive for p53. Furthermore, the identification of the same mutations in p53 tumor suppressor gene in both epithelial and mesenchymal elements implies a common derivation from a multipotent stem cell of the mullerian system differentiating towards the epithelium and mesenchyme [13,14].Strong overexpression of p53 protein was observed in both epithelial and mesenchymal cells, including carcinoma in situ in the same fallopian tube and in the fimbriae of the controlateral fallopian tube. This suggests that the p53 mutation is an early event in carcinogenesis. The expression of CD10 in the present cases is consistent with previous reports that propose it as a characteristic of mullerian system derived neoplastic mesenchymal cells [8]. This represents the main phenotypic difference of homologous MMMT with serous carcinoma whereas p53 staining is a common feature between the two tumor types.
On the whole, our observations show that MMMT and serous carcinoma may derive from the same site of origin.
Treatment and Prognosis
Recommended treatment is by surgery, followed by radiotherapy and/or chemotherapy. The prognosis is poor, the 5-year survival rate being about 15% and the mean survival only 16-20 months. Early stage disease is associated with a better prognosis, and several long-term survivals are recorded [4].
References
-
Carcangiu ML, Peissel B, Pasini B, Spatti G, Radice P, et al. (2006) Incidental carcinomas in prophylactic specimens in BRCA1 and BRCA2 germ-line mutation carriers, with emphasis on fallopian tube lesions: report of 6 cases and review of the literature. Am J Surg Pathol 30: 1222-1230.
-
Kindelberger DW, Lee Y, Miron A, Hirsch MS, Feltmate C, et al. (2007) Intraepithelial carcinoma of the fimbria and pelvic serous carcinoma: Evidence for a causal relationship. Am J Surg Pathol 31: 161-169.
-
Jarboe EA, Folkins AK, Drapkin R, Ince TA, Agoston ES, et al. (2008) Tubal and ovarian pathways to pelvic epithelial cancer: a pathological perspective. Histopathology 53: 127-138.
-
Stanley J. Robboy, George L. Mutter, Jaime Prat, FRCPath, Rex Bentley et al. (2009) Robboy's Pathology of the Female Reproductive Tract, 2nd Edition. In: Elsevier: 28.
-
Carlson JA Jr, Ackerman BL, Wheeler JE (1993) Malignant mixed müllerian tumor of the fallopian tube. Cancer 71: 187-192.
-
Hanjani P, Petersen RO, Bonnell SA (1980) Malignant mixed Mullerian tumor of the fallopian tube. Report of a case and review of literature. Gynecol Oncol 9: 381-393.
-
Imachi M, Tsukamoto N, Shigematsu T, Watanabe T, Uehira K, et al. (1992) Malignant mixed Müllerian tumor of the fallopian tube: report of two cases and review of literature. Gynecol Oncol 47: 114-124.
-
Kuroda N, Moriki T, Oguri H, Maeda N, Toi M, et al. (2005) Malignant müllerian mixed tumor (carcinosarcoma) of the fallopian tube: an immunohistochemical study of neoplastic cells. APMIS 113: 643-646.
-
Yang Sun, Lin Lv, Zhi-lan Peng, Kai-xuan Yang, Jiang-yan Lou (2009) Malignant mixed Müllerian tumor of the fallopian tube in a patient with irregular vaginal bleeding. Lab Med 40: 401-403.
-
McCluggage WG (2002) Malignant biphasic uterine tumours: carcinosarcomas or metaplastic carcinomas? J Clin Pathol 55: 321-325.
-
Alvarado-Cabrero I, Cheung AF, Caduff R (2003) Tumours of the fallopian tube and uterine ligaments. In: Tavassoli F.A. DPE, ed. Pathology and Genetics: Tumours of the Breast and Female Genital Organs. Lyon, France: IARC Press: 203-216.
-
Bicher A, Levenback C, Silva EG, Burke TW, Morris M, et al. (1995) Ovarian malignant mixed müllerian tumors treated with platinum-based chemotherapy. Obstet Gynecol 85: 735-739.
-
Costa MJ, Vogelsan J, Young LJ (1994) p53 gene mutation in female genital tract carcinosarcomas (malignant mixed müllerian tumors): a clinicopathologic study of 74 cases. Mod Pathol 7: 619-627.
-
Kounelis S, Jones MW, Papadaki H, Bakker A, Swalsky P, et al. (1998) Carcinosarcomas (malignant mixed mullerian tumors) of the female genital tract: comparative molecular analysis of epithelial and mesenchymal components. Hum Pathol 29: 82-87.





