International Journal of Cancer and Clinical Research
Cervical Cytology Screening - Is the Change of Policy Risk Free?
Emily H. Hertzberg, Nurit Ariel, Dalia Kaplan, Michal Markovitz and Zeev Blumenfeld*
Reproductive Endocrinology, Ob/Gyn, RAMBAM Health Care Campus, The Rappaport Faculty of Medicine, Technion - Israel Institute of Technology, Haifa, Israel
*Corresponding author:
Zeev Blumenfeld, Associate Professor, Director, Reproductive Endocrinology, Department of OB/GYN, Rambam Health Care Campus, Rappaport Research Institute, Technion-Faculty of Medicine, 8 Ha'Aliyah St, Haifa, Israel 31096, Tel: 972-4-8542577, Fax: 972-4-8543243, E-mail: bzeev@techunix.technion.ac.il, z_blumenfeld@rambam.health.gov.il
Int J Cancer Clin Res, IJCCR-2-031, (Volume 2, Issue 5), Research Article; ISSN: 2378-3419
Received: September 25, 2015 | Accepted: October 27, 2015 | Published: November 01, 2015
Citation: Hertzberg EH, Ariel N, Kaplan D, Markovitz M, Blumenfeld Z (2015) Cervical Cytology Screening - Is the Change of Policy Risk Free?. Int J Cancer Clin Res 2:031. 10.23937/2378-3419/2/5/1031
Copyright: © 2015 Hertzberg EH, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective: With the change in the cervical cancer screening guidelines, women younger than 21 will not be routinely screened and the screening interval is extended to three years. In spite of the well-received newly recommended guidelines on cervical cancer screening, how many patients will be excluded by the guidelines that may have otherwise benefited from the screening?. It is important to look at the trends in the screened population in order to answer this question. Our aim was to determine the effectiveness of the previous policy on cervical cancer screening in terms of incidence of cervical cancer and rates of dysplasia in the population of a tertiary hospital gynecology outpatient clinic.
Materials and Methods: This is a retrospective analysis conducted at Rambam Health Care Campus' gynecology outpatient clinic. Chart-review of all cytology reports of PAP smears performed between the years 2004 and 2010 were evaluated. Data were compared to measure the screening methods and changes to the screening method including the trends in PAP smear testing, results, persistence, and the trends in progression and regression in disease based on pre-determined age groups.
Results: The rate of atypical PAP smear test results was 10.92% which was broken down in a rate of atypia of 7.66%, the rate of low grade squamous intraepithelial lesion [LGSIL] was 2.93%, and high grade SIL [HGSIL] was 0.338%.The highest incidence of atypical PAP smear results was seen in the age group 21-25. The highest incidence of LGSIL was seen in under 21 years and 21-25 years. The highest incidence of HGSIL was seen under 21 years. In the under 21 y's group, there was a wide disparity between those who regressed (14%) and those who progressed (3%). On the other hand, in the 26-30 years group and the 41-50 years group, the trend was towards progression of disease (19.4% and 27%, respectively).
Conclusions: Through the results of this study, it seems that not testing women under 21 years old would result in missed diagnoses of potentially treatable precancerous cervical lesions. It is important to factor in the harms of excessive PAP smears and subsequent follow up procedures in order to get a more accurate net benefit from the screening of young women.
Keywords
Cervical cytology, PAP smear, Cervical cancer, Cervical dysplasia, Atypia, SIL, CIN, Preventative Medicine
Introduction
Cervical cancer is the most common gynecologic neoplasm and the second most frequent cancer in women worldwide [1]. According to the WHO/ICO Information Centre [1] on HPV and Cervical Cancer, Israel has 222 new cervical cancer cases diagnoses annually. Although there is a relatively low incidence of cervical cancer in Israel (crude incidence rate of 6.2, age - standardized incidence rate of 5.6), the mortality rate from cervical cancer is relatively high. Annually in Israel, there are 98 new cervical cancer deaths, a crude mortality rate of 2.8 and an age-standardized mortality rate of 2.1 making cervical cancer the 14th cause of female cancer deaths in women aged 15 - 44 years. In the United States the incidence of cervical cancer is higher/similar compared to Israel (crude rate of 7, age-standardized incidence rate of 5.7) while the mortality rate of cervical cancer related deaths is 2.4 (age - adjusted 1.7). The incidence of precancerous cervical lesions (low-grade squamous intraepithelial lesions, and high-grade squamous intraepithelial lesions) is equal in Israel and Western countries [2]. The disparity between the low incidence and the high mortality of cervical cancer in Israel may be due to problems in the screening methods.
The current and historical screening method for cervical cancer is the PAP (Papanicolaou) cytology smear test. While the PAP smear test is not the gold standard for diagnosis (it has not been tested in a randomized controlled trial), observational data support its use. Large population-based studies in Iceland showed that the mortality rate declined by 80% for more than 20 years with the use of PAP smear tests, and in Finland and Sweden by 50% and 34%, respectively [3,4]. These studies also found that reduction in the incidence and mortality of cervical cancer was proportional to the intensity of screening [3,4]. In addition, poor PAP smear screening frequency was the primary factor attributable to development of invasive cervical cancer. 53.8% of invasive cervical cancer subjects had inadequate screening histories and 4.5% have never been screened [5]. Despite the wide use of the PAP smear test, it is far from being a perfect test. The PAP smear test has limited sensitivity for detecting cervical cancer and its precursors, precancerous cervical lesions. To compensate for this limited sensitivity, the test was often repeated in short intervals with low cytological threshold for additional follow up. Repetitive tests in short intervals leads to elevated costs and exposure to unnecessary follow-up tests (colposcopy) that are not without consequences [6].
In Israel, cervical cancer screening has been opportunistic and institution-specific, meaning a PAP smear test was done only if the patient was consulting a health practitioner for another purpose. For several years Rambam Health Care Campus' policy comprised the screening of all sexually active women within one year of first sexual activity. In March 2012, the United States Preventive Service Task Force [7] changed the recommendation on screening for cervical cancer. All women with a cervix, regardless of sexual history should been screened with cytology (PAP smear test) from the ages of 21 to 65 years, every 3 years. Women between 30 and 65 years of age can be screened with a combination of cytology (PAP smear test) and HPV DNA testing every 5 years. Women under 21 years of age and those after total hysterectomy (removal of the cervix) should not be screened. These recommendations exclude women who have been diagnosed with high-grade precancerous cervical lesion or cervical cancer, women with in utero exposure to diethylstilbestrol (DES), or immuno-compromised women [7]. The National Institute of Health (NIH, American College of Obstetrics and Gynecology (ACOG), and the Center for Disease Control (CDC) have adopted these new guidelines. In 2012, the Rambam Health Care Campus (RHCC) also changed its policy to adopt the new USPSTF guidelines.
With the change in the cervical cancer screening guidelines, women younger than 21 will not be routinely screened and the screening interval is extended to three years. In spite of the well-received newly recommended guidelines on cervical cancer screening, how many patients will be excluded by the guidelines that may have otherwise benefited from the screening?. It is important to look at the trends in the population at RHCC in order to answer this question. Our aim was to determine the effectiveness of the previous policy on cervical cancer screening in terms of incidence of cervical cancer and rates of dysplasia in the population of RHCC gynecology outpatient clinic.
Materials and Methods
The study is a retrospective database analysis. A database was compiled of PAP smear tests performed between the years 2004 to 2010. All PAP smear tests were performed at the RHCC gynecology outpatient clinic, a tertiary medical centre serving a population of over a million in northern Israel. This includes Israeli Jewish and Israeli Arab women from a diverse socio-economic background. The Rambam cytology laboratory read all the cytology results and diagnoses were retrieved from a computerized database with treatment procedures collected from the patient's chart. Records in all files and databases contain recipients' unique identification number. The study has been approved by the hospital's institutional review board.
A total of 1778 PAP smear tests were collected from a total of 1094 women over the span of seven years. No age cut-offs were used in order to measure all patients whether or not they would be screened under the new guidelines.
The PAP smear tests were performed using an endocervical brush at the transitional zone of the cervix. The smear was fixed using 96% ethanol.
The information obtained from the PAP smear test included patient's age, indication for PAP smear test, result of cytology, and treatment.
Cervical cancer screening rates/trends
The cervical cancer screening trends were calculated by the percentage of women who had PAP smear tests, calculated for age group, and indication for PAP smear test. Age was categorized into eight groups: < 21 years, 21-25 years, 36-30 years, 31-35 years, 36-40 years, 41-50 years, 51-64 years, and > 65 years.
Atypia/Precancerous Lesions/Cervical cancer prevalence trends
Cervical cancer, precancerous lesions (PCL), and other abnormal diagnoses were identified from the Rambam cytology department formal results. The prevalence rates by age group were calculated by using the total number of recipients who had a diagnosis of a degree of atypia/PCL/cervical cancer in a given age group divided the total number of PAP smear tests in that age group.
Atypia/PCL/Cervical Cancer Trends between the age groups
The population was examined by age group, especially those younger than 21 years. The data was stratified by PAP smear test result and in particular split into non-pathological findings, atypia (which included a histological diagnosis of atypia, koilocytosis, or ASCUS [atypical squamous cells of unknown significance]), and Precancerous Lesions (low-grade squamous intraepithelial lesion (LGSIL) and high-grade squamous intraepithelial lesion (HGSIL). A Pearson's Chi-Square test and Fisher's Exact test was used to determine statistical significance between the age groups. All tests were two-sided.
Persistence with PAP smear testing
Persistence with PAP smear testing among recipients was measured by calculating the total number of claims for PAP smear testing during the seven-year period. The higher the count, the greater the persistence with PAP smear testing. Testing more than once a year without an indication, was also noted. Statistical significance was calculated using an unpaired two-tailed t-test with Welch's correction.
Rates of persistence and regression of disease
Change in diagnosis was defined by any change from one visit to the subsequent visit. Persistence of disease was defined as the change in diagnosis that reflects a worsening of an atypia/PCL diagnosis. Regression of disease was defined as the change in diagnosis that reflected a regression/alleviation of atypia/PCL diagnosis. This was calculated by monitoring the index date (defined as the date of the first claim containing a diagnosis of atypia/PCL/cervical cancer) and analyzing prospective follow-up and recurrent PAP smear tests after the index date.
Results
PAP smear testing prevalence and trends
Recipient's ages ranged between 18 and 87 years (Table 1). Among the age groups, the rates of screening were mostly equally distributed, although the age-group under 21 years old is over represented considering the new guidelines that do not recommend the screening of females under 21 years of age. The most common reason for PAP smear testing was a routine screening according to the previous screening guidelines at the hospital.
![]()
Table 1: Cervical Cancer Screening (PAP smear testing) Rate (Percentage) Among Female Patients at the Rambam Gynecology Outpatient Clinic.
View Table 1
Precancerous Lesions/Cervical cancer prevalence trends
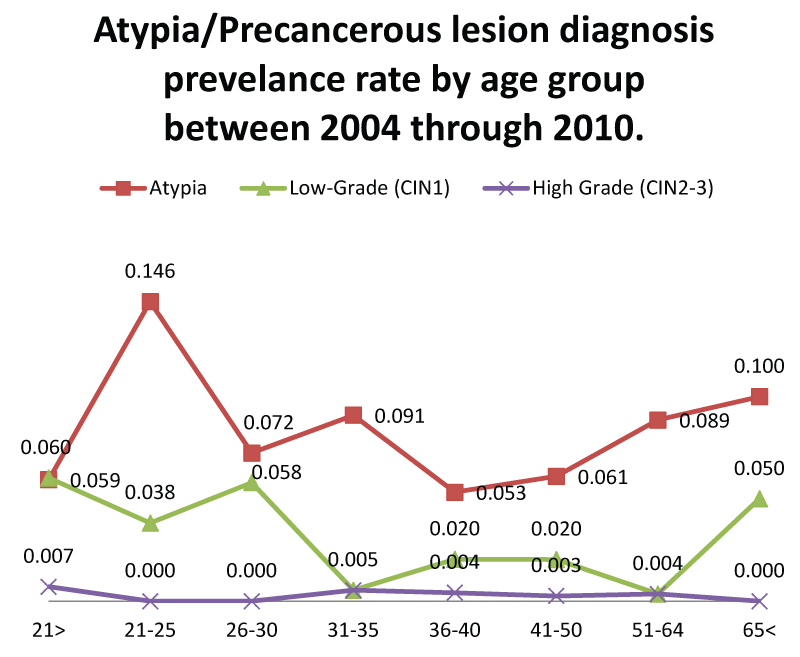
Figure 1 shows the display of the tested patients stratified by age group and result. There were no cases of cervical cancer. The highest incidence of abnormal was in the age group 21 - 25. The highest incidence of LGSIL was detected under 21 years and 21 - 25 years. The highest incidence of HGSIL was seen under 21 years. The rate of atypical PAP smear test results between 2004 and 2010 was 10.92%, which was broken down in a rate of atypia/koilocytosis/ASCUS of 7.66%, the rate of LGSIL was 2.93%, and the rate of HGSIL was 0.338%.
.
Figure 1: Cervical Atypia/Precancerous Lesion prevalence rate trends by age.
< 21, N = 262; 21-25, N = 153; 26-30, N = 198; 31-35, N = 182; 36-40, N = 238; 41-50, N = 386; 51-64, N = 274; > 65, N = 20. CIN = cervical intraepithelial neoplasia.
View Figure 1
Trends in dysplasia/PCL between the age groups
Table 2 displays that there was no statistical significance between the rate of atypical including precancerous lesions and the rate of normal PAP smear between the age groups. Because abnormal findings including atypia, koilocytosis and ASCUS was common in the age group younger than 21 and usually self-resolves, it is important to see (Table 3) that even when including a result of abnormal but non-dysplastic findings versus LGSIL and HGSIL, there still was no significant difference between the younger than 21 years old and the 21 - 25 years old groups. In table 4, we looked at the younger than 21-year-old group versus the rest of the population of PAP smear test recipients and found no significance when comparing non-pathological and pathological PAP smear test results.
![]()
Table 2: Comparison of data from the PAP smear test results of the under 21-year-old group and the 21 - 25 year old group and statistical analysis. The results are grouped by normal versus abnormal results (atypia, low grade and high grade SIL). NS = non-significant; PAP = papanicolaou test; LGSIL = low-grade squamous intraepithelial lesion; HGSIL = high-grade squamous intraepithelial lesion.
View Table 2
![]()
Table 3: Comparison of data from the PAP smear test results of the under 21 year old group and the 21 - 25 year old group and statistical analysis. The results are grouped by no pathology with dysplasia (benign/equivocal pathology including Atypia, Koilocytosis, ASCUS, usually no treatment required) versus low grade and high grade SIL. NS = non-significant; PAP = Papanicolaou test; LGSIL = low-grade squamous intraepithelial lesion; HGSIL = high-grade squamous intraepithelial lesion.
View Table 3
PAP smear testing persistence
In the seven-year period, 67.3% of the recipients have undergone only one PAP smear test. In Table 5, the average number of visits was compared by age and by past PAP smear testing history. Because one visit was the baseline in the study, only values greater than one visit were considered in the analysis. The under 21 years group received less PAP smear testing than the general population. The recipients with a history of cervical dysplasia received more PAP smear testing than those with no history of any cervical dysplasia.
![]()
Table 4: Comparison of data from the PAP smear results of the under 21-year-old group and the rest of the population (21-65 years of age) and statistical analysis. The results are grouped by non-pathological versus abnormal (cervical atypia, low grade and high grade SIL). NS = Non-significant. PAP = papanicolaou test; LGSIL = low-grade squamous intraepithelial lesion; HGSIL = high-grade squamous intraepithelial lesion.
View Table 4
![]()
Table 5: The mean and statistical analysis of the number PAP smear tests for female recipients between 2004 and 2009 based on age and history of cervical dysplasia. Those who received only one PAP smear tests in this time period were not included in the interval calculation.
View Table 5
Rates of persistence and regression of disease
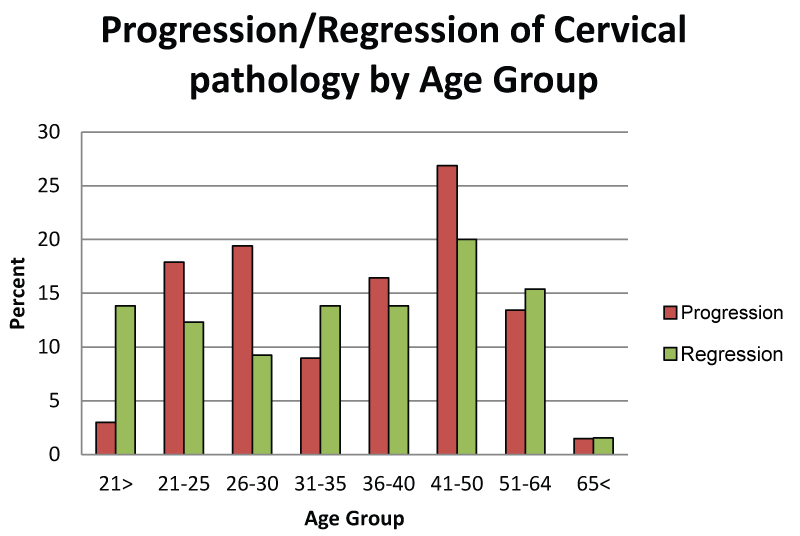
Figure 2 shows the trends of progression and regression of cervical cytological results by age group. Of those recipients who changed PAP smear test diagnosis from one PAP smear to the next, there was a difference between age groups. In the under 21 years of age group, there was a wide disparity between those who regressed (14%) and those who progressed (3%). On the other hand, in the 26 - 30 years group and the 41 - 50 years group, the trend was towards progression of disease (19.4% and 27%, respectively).
.
Figure 2: Progression and regression of cervical pathology by age group between 2004 and 2010. Includes only recipients of more than one PAP smear test between 2004 and 2010. No change, N = 554 (not included in figure); Progression, N = 67; Regression, N = 65.
View Figure 2
Discussion
One thousand, seven hundred and seventy-eight PAP smear tests were performed between 2004 and 2010 at RHCC Gynecology Outpatient Unit. The rate of atypical PAP smear test results was 10.92%, including 7.66% with findings of atypia, koilocytosis, or ASCUS, 2.93% with LGSIL (histological diagnosis of CIN1), and 0.338% with HGSIL (histological diagnosis of CIN2 or CIN3). The highest incidence of LGSIL was seen in the under 21 years and the 21-25 year old group. Surprisingly, the highest incidence of HGSIL was seen in the under 21 group. These results are higher than expected given the literature on similar age population. A larger study performed by Clalit medical services [2], one of the largest HMOs (Health Maintenance Organization) in Israel, examined 199, 259 PAP smear tests between 2005 and 2009 and found a rate of 3.7% atypical PAP smear results [2]. The other major Israeli HMO, Maccabi, conducted a similar retrospective analysis of 297, 849 PAP smear tests from 1991 through 1999 which showed the incidence of LGSIL and HGSIL to be 0.69% and 0.29%, respectively. The highest incidence of LGSIL was between the ages 20-24 and the highest incidence of HGSIL was between 30-39 years old [8]. A possible explanation to the differences in incidences between our study and the larger HMO studies is the population. Rambam is located in the Northern district of Israel and serves a smaller, more homogenous population. The population is very mixed with Jewish Israelis, Arabs, and Russian immigrants with a wide variation in socioeconomic status. There should be further investigation into how race, religion, immigration status, and socioeconomic status impact that rate of screening as well as the incidence of cervical pathology. Another possible explanation for the higher rates of dysplasia is that the population served by RHCC is more secular than in Israel as a whole. A more secular population means less strict views on premarital sex and earlier exposure to HPV infection.
One of the major concerns with adapting the U.S. Preventive Service Task Force (USPSTF) recommendation on beginning screening women at 21 years of age is how many diagnoses of precancerous cervical lesions will be missed in this age group?. The Israel Society of Obstetrics and Gynecology recommends screening all women every 3 years from ages 25-65 years of age, making the group that may be missed in Israel even larger. The USPSTF admits that there is a lack of publications evaluating the age at which to begin screening. The reasoning behind excluding these young women is that the rates of HGSIL and cervical cancer are markedly low in this group. The prevalence of CIN3 among women younger than 20 years is 0.2% [9]. The analyses performed by the USPSTF found that varying the start age for cytology screening from 15 years to 18 years to 21 years shows cervical cancer death rates of 1.54, 1.54, and 1.55 per 1000 women, respectively [10]. This evidence cannot be interpreted without understanding a few important things. It has been seen in other studies that low-grade precancerous lesions regress spontaneously in younger women. One study found that 62% of women with LGSIL regressed to normal in a 39-month follow up [11]. In our study of the 11 recipients that had received more than one PAP smear test under the age of 21 and had some degree of abnormality, 14% regressed and only 2.5% progressed to a more severe diagnosis.
When attempting to determine whether to screen women under 21 years old, the possible risks and complications must also be discussed. Excessive PAP smears done at young ages (under 21) when the prevalence of HPV is highest leads to additional diagnostic procedures and a false-positive cytology rate of 3.1% [7]. Colposcopies, even though considered a safe diagnostic procedure can lead to immediately higher reports of pain, bleeding, and or discharge over those who just underwent surveillance of the lesions [12]. Treatment of high-grade precancerous lesions involved cervical conization or loop electrosurgical excision, with specific short and long-term consequences. Short-term consequences are similar to those from colposcopy but the long-term consequences include higher rate of preterm delivery, and low birth weight, possibly affecting perinatal mortality [13].
It should be mentioned that a prospective study was almost impossible to perform due to the changed practice of PAP smear routine testing in light of the 2012 recommendations. This study is retrospective and the data set was collected for clinical evaluation and not as part of a research protocol. Therefore it must be assumed there is variation in materials and methodology used during the PAP smear test and documentation. Similarly, the Bethesda system was not used in the reporting of cytology reports by the Rambam cytology laboratory and therefore was inconsistent and unstandardized. There was no set time interval between testing of healthy patients and of those patients with cervical pathology. This was a challenge when trying to compare intervals of screening time for patients because there was no standard model to follow for short or long screening interval times. As discussed previously, there was a higher frequency of high-grade squamous intraepithelial lesions in the younger than 21 years group compared to previous reports. In future studies it would be beneficial to examine other factors such as sexual activity, pregnancy history, smoking status, and oral contraception use should be noted and analyzed. Lastly, low patient compliance for follow-up PAP smear tests may skew the data.
Anecdotally, after the collection of all the PAP smear tests performed between 2004 and 2010 there were two 19 year-old patients seen in the Rambam clinic diagnosed with HGSIL (CIN3). One patient had previously been diagnosed with ASCUS which was followed by a colposcopy compatible with CIN and koilocytosis. The second patient was diagnosed by a screening PAP smear test and underwent conization. With the current guidelines, these women would have had to wait two more years before their first PAP smear tests. For these patients, the risk of waiting and possibly progression of disease severity outweighs the risk of unnecessary procedures. Despite the results of this study, it is fair to assume and speculate that the consequences of early screening for cervical cancer with subsequent, excessive follow-up tests outweigh the benefits of early detection of low-grade lesions that will most likely regress [14-19]. It is necessary for future work to account for other factors that may predispose young women to earlier high-grade lesions.
References
-
(2010) WHO/ICO Information Centre on HPV and Cervical Cancer (HPV Information Centre). Human Papillomavirus and Related Cancers in Israel. Summary Report.
-
Schejter E, Bornstein J, Siegler E (2013) Cervical cancer screening, human papillomavirus vaccination practices and current infrastructure in Israel. Vaccine 31: 142-145.
-
Laara E, Day NE, Hakama M (1987) Trends in mortality from cervical cancer in the Nordic countries: association with organised screening programmes. Lancet 1: 1247-1249.
-
Sigurdsson K (1993) Effect of organized screening on the risk of cervical cancer. Evaluation of screening activity in Iceland, 1964-1991. Int J Cancer 54: 563-570.
-
Spence AR, Goggin P, Franco EL (2007) Process of care failures in invasive cervical cancer: systematic review and meta-analysis. Prev Med 45: 93-106.
-
Schiffman M, Solomon D (2013) Clinical practice. Cervical-cancer screening with human papillomavirus and cytologic cotesting. N Engl J Med 369: 2324-2331.
-
Kjaer SK. Frederiksen K. Munk C. Iftner T (2010) Long-term absolute risk of cervical intraepithelial neoplasia grade 3 or worse following human papillomavirus infection: role of persistence. J Natl Cancer Inst 102: 1478-1488.
-
Insinga RP, Glass AG, Rush BB (2004) Diagnoses and outcomes in cervical cancer screening: a population-based study. Am J ObstetGynecol 191: 105-113.
-
Kulasingam SL, Havrilesky L, Ghebre R, Myers ER (2011) Screening for cervical cancer: a decision analysis for the U.S. Preventive Services Task Force. Rockville, MD: Agency for Healthcare Research and Quality: AHRQ Publication No 11-05157-EF-1.
-
Nasiell K, Roger V, Nasiell M (1986) Behavior of mild cervical dysplasia during long-term follow-up. ObstetGynecol 67: 665-669.
-
Sharp L, Cotton S, Cochran C, Gray N, Little J, et al. TOMBOLA (Trial Of Management of Borderline and Other Low-grade Abnormal smears) Group (2009) After-effects reported by women following colposcopy, cervical biopsies and LLETZ: results from the TOMBOLA trial. BJOG 116: 1506-1514.
-
Arbyn M, Kyrgiou M, Simoens C, Raifu AO, Koliopoulos G, et al. (2008) Perinatal mortality and other severe adverse pregnancy outcomes associated with treatment of cervical intraepithelial neoplasia: meta-analysis. BMJ 337: a1284.
-
Munoz N, Bosch FX, de Sanjose S, Herrero R, Castellsague X, et al. (2003) International Agency for Research on Cancer Multicenter Cervical Cancer Study Group. Epidemiologic classification of human papillomavirus types associated with cervical cancer. N Engl J Med 348: 518-527.
-
Nadpara PA, Madhavan SS, Khanna R, Smith M, Miller LA (2012) Patterns of cervical cancer screening, diagnosis, and follow-up treatment in a state Medicaid fee-for-service population. Popul Health Manag 15: 362-371.
-
Raz R, Shavit O, Stein M, Cohen R, Schejter E, et al. (2012) Uptake of pap smears among women in a large Israeli HMO between 2006 and 2008. Public Health 126: 594-599.
-
Sawaya GF, McConnell KJ, Kulasingam SL, Lawson HW, Kerlikowske K, et al. (2003) Risk of cervical cancer associated with extending the interval between cervical-cancer screenings. N Engl J Med 349: 1501-1509.
-
Shavit O, Raz R, Stein M, Chodick G, Schejter E, et al. (2012) Evaluating the epidemiology and morbidity burden associated with human papillomavirus in Israel. Appl Health Health Policy 10: 87-97.
-
Siegel R, Naishadham D, Jemal A (2013) Cancer statistics, 2013. CA Cancer J Clin 63: 11-30.
-
Blatt AJ, Kennedy R, Luff RD, Austin RM, Rabin DS (2015) Comparison of cervical cancer screening results among 256, 648 women in multiple clinical practices. Cancer Cytopathol 123: 282-288.





