International Journal of Diabetes and Clinical Research
Type 2 Diabetes and Lifestyle- A Prospective Population-Based Cohort Study among Rural Men
Anders Thelin1* and Sara Holmberg1,2
1Department of Public Health and Caring Sciences, Family Medicine and Clinical Epidemiology Sections, Uppsala University, Sweden
2Research and Development Centre, Kronoberg County Council, Sweden
*Corresponding author:
Anders Thelin, Department of Public Health and Caring Sciences, Family Medicine and Clinical Epidemiology Sections, Uppsala University, Gatugard, SE-355 94 Wedersl�f, Sweden, Tel: +46-470-778000; E-mail: athelin@wgab.se
Int J Diabetes Clin Res, IJDCR-1-010, (Volume 1, Issue 2), Research Article; ISSN: 2377-3634
Received: September 24, 2014 | Accepted: November 13, 2014 | Published: November 16, 2014
Citation: Thelin A, Holmberg S (2014) Type 2 Diabetes and Lifestyle- A Prospective Population-Based Cohort Study among Rural Men. Int J Diabetes Clin Res 1:010. 10.23937/2377-3634/1410010
Copyright: © 2014 Thelin A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The risk of type 2 diabetes (T2D) is related to lifestyle but less is known about how lifestyle factors interact and how they impact the risk when combined. This study was performed to analyze how lifestyle factors relate to the cumulative incidence of T2D in a Swedish rural population. Outcomes were generated from national registers and from two surveys. Two hundred sixty men (11%) with diabetes were found in the registers, and 193 men with T2D were identified in the surveyed population (9.8%). Physical activity (OR for high physical activity=0.55 (95% CI 0.31-0.97) and meal quality (OR for high meal quality=0.58 [95% CI 0.35-0.99] were significantly related to T2D in the adjusted analyses. Other lifestyle factors had no significant relationship with T2D in this study. An interaction between physical activity and meal quality was revealed, indicating that a healthy lifestyle in one of the aspects does not compensate for an unhealthy choice in the other.
Keywords
Diabetes type 2, diet, meal quality, physical activity, rural population, prospective cohort study
Introduction
The number of people suffering from type 2 diabetes (T2D) is rapidly increasing worldwide [1,2]. T2D has a significant impact on morbidity and mortality and gives rise to extensive medical interventions related to medical complications. The treatment and prevention of T2D is a challenging task, especially for physicians in primary health care.
In Western industrialized countries, the prevalence ofT2D is strongly influenced by socioeconomic status [3,4]. High frequencies of the metabolic syndrome, which is strongly related to diabetes, are reported from different countries [5], including countries with a less westernized lifestyle [6,7], and for different occupational groups [8].
Lack of exercise, poor diet, smoking and low or no alcohol consumption were all associated with a significantly increased risk of T2D among female nurses [9]. Nine of ten new cases of T2Dcould be attributed to five lifestyle factors (physical activity, diet, smoking, alcohol habits and adiposity) in a recent analysis [10].
However, few studies have been conducted to analyze the risk or frequency of diabetes in occupational groups. A Polish study [11] reports a high risk of diabetes among road transport drivers and in Japan, fire-fighters and policemen have an increased risk of T2D [12]. In both studies, the risk was related to high body mass index (BMI). Blue-collar occupations were associated with a high prevalence of diabetes mellitus in another Japanese study [13]. We have found a low cumulative incidence of T2D among Swedish farmers, which is related to high physical capacity and high meal quality [14].
The aim of this study was to analyze how the risk of T2D is associated with lifestyle in a male rural population and to analyze whether and how these factors interact and impact the cumulative incidence of T2D.
Methods
Study population
A prospective study cohort with farmers and rural non-farmer referents was established in 1989 with the intention to study health-promoting factors related to farming and lifestyle. All male farmers born between 1930 and 1949 in nine rural municipalities in Sweden were identified from the Swedish National Farm Register. The areas were chosen taking into consideration known east-west and north-south cardiovascular disease gradients in the Swedish population [15], and with the objective to be representative of a variety of farm types and geographical variation across the country. Farmers were defined as men who owned or rented a farm and who spent at least 25 hours per week farming. The occupational activity was checked with local representatives from the Federation of Swedish Farmers. Farm laborers were not included. To each farmer, a rural referent, matched by age, sex and residential area, was sampled from the National Population Register. The rural referents should be active in an occupation other than farming, according to the most recent census. Due to limited non-farming populations in some of the districts included, the non-farmers were somewhat fewer than the farmers.
Altogether, 1,220 farmers and 1,130 rural non-farmers were eligible and included in the cohort. The farmers and the rural referents (n=2,350) were invited to an extensive health survey in 1990/91, including questionnaires, interviews, physical examinations and laboratory tests. The participation rate was 75.8 % with 1,782 men attending the baseline survey [16-18]. A second survey was performed in 2002-03 and the same, still available individuals were invited. At this time, 67.6% of the base population, which was 72.1 % of the available population, attended the survey. Altogether 1,963 individuals participated at least once (83.5% of the study population) (Table 1). The whole study population has been followed in national registers.
![]()
Table 1: Description of the study population
View Table 1
The study was approved by the Research Ethics Committee at the Karolinska Institute in Stockholm, Sweden, and by the Regional Ethics Board, Uppsala, Sweden. All men who participated in the health surveys gave their informed consent.
Outcomes
The number of fatalities and causes of death from 1989 through 2009 were obtained from the National Cause of Death Register. The diagnoses were in accordance with the International Classification of Diseases (ICD), 9th edition, Swedish version, from 1989 through 1996, and the 10th edition, Swedish version, from 1997 through 2009 [19,20].
Diagnoses for admission to hospital for the years 1989-2009 were obtained from the Hospital Patient Register, which registers all hospital admissions in Sweden with a main diagnosis and up to seven additional diagnoses. We used all available diagnoses and counted the number of individuals who were given a diabetes diagnosis at least once. Diabetes was defined as ICD-9 code 250 and ICD-10 codes E10- E14 [19,20].
Diagnoses for outpatients were retrieved from the Patient Register, which registers all visits to attending physicians at hospitals in Sweden for the years 2001-2009. Diagnoses were retrieved and patients included in the same way as for the Hospital Patient Register.
A team of doctors, nurses, and physiotherapists visited the nine rural districts during a 12-month period in 1990-1991. The selected population was invited to the investigation and those who did not show up were reminded by telephone. The surveys included structural and elaborate interviews concerning previous health problems and contacts with health care suppliers, as well as current medical drug consumption including insulin. Questionnaires were answered on site and different tests were performed and blood samples drawn. The second survey in 2002/03 was conducted in the same way, but some tests were excluded and some new questionnaires included.
Individuals with diabetes taking insulin who were identified in the 1990-91 survey were regarded as having type1 diabetes and were excluded from further analyses. Individuals with diabetes not taking insulin in 1990-91, as well as all those who acquired diabetes during the follow-up period were regarded as having T2D.
Lifestyle
A number of living conditions and habits (lifestyle factors) are related to T2D [5]. In this study we have included physical activity, meal quality, smoking, alcohol consumption, stress, occupation and educational level.
The level of physical activity has been estimated in three ways. Physical workload was assessed in a structured interview by an experienced physician as the reported average number of hours working in a sitting or standing position, with a moderate, heavy or very heavy workload during an average working day, according to Edholm�s activity scale [21]. Physical activity during leisure time was assessed in interviews on a four-grade scale (sedentary, low, moderate or rigorous activity). The physical work capacity was determined using a sub-maximal work test on a bicycle ergometer [22]. The three parameters of physical workload, physical activity during leisure time, and physical work capacity were used to generate a general physical activity indicator (Table 2).
![]()
Table 2: General physical activity indicator.
View Table 2
In addition to the dietary components, eating habits, meal design and meal structure throughout the day may be of relevance [23]. The baseline survey included a meal quality index, which estimated the daily meal schedule and the different types of meals during an ordinary day, assessed in a structured interview. The day was split into six periods of three hours each, from early morning to late afternoon, and the participant was asked what kind of food was consumed during each three-hour period. Only something to drink generated one point and a full cooked meal generated 5 points. The points were summarized and the sum was used as a meal quality index (Table 3).
![]()
Table 3: Description of the meal quality index with an illustrative example. Meal data from six periods of the day, three hours each, assessed in structural interviews.
View Table 3
Tobacco and alcohol consumption were assessed in a structured interview. Tobacco consumption was analyzed as a dichotomous variable: current daily smoking, yes or no. Average alcohol intake, computed as grams of pure alcohol consumed per week, was based on the frequency of alcohol intake, type of beverage consumed and amount consumed on each occasion.
Stress was operationalized as experienced work demand and perceived work control and was assessed in a questionnaire according to Karasek and Theorell [24]. Occupation was included as farming versus non-farming according to the design of the base project. Educational level was measured on a five-grade scale from compulsory to university level.
Baseline characteristics
Weight and height were measured with standard procedures at the baseline survey and BMI was calculated as weight in kilograms divided by height in meters squared. The waist/hip ratio was calculated after measuring the waist and hip using a standard tape measure. Blood pressure was measured twice with mechanical blood pressure equipment (Trim line LIC�) after five minutes of supine rest, and the average was recorded. The diastolic blood pressure has been used in the analyses.
Non-fasting blood samples were drawn, centrifuged, and refrigerated at 4�C at the examination site and all samples were transported to the same laboratory in Uppsala for analysis within three days.
Statistical analyses
The survey in 1990-91 was regarded as baseline. Those who only took part in the second survey in 2002-03 did not generate any baseline data. The internal non-response rate was very low for almost all items (less than 2%). Physical work capacity testing had more dropouts, due to clinical precautions in permitting testing, and the missing rate for the Karasek-Theorell questionnaire was 9 %.
The statistical analyses were conducted using the SPSS� version 16.0. Comparisons between farmers and non-farmers regarding baseline factors were made using at test for continuous variables and a Chi2test for categorical variables. Multiple logistic regression models were applied to analyze associations between lifestyle factors and T2D, as well as the components of the metabolic syndrome and T2D. The analyses were performed in a stepwise manner. The results are presented as odds ratios (OR) with 95% confidence intervals (95% CI).
Results
National registers (death register, hospital inpatient register and hospital outpatient register) include 260 individuals, out of a total of 2,350 individuals with a diabetes diagnosis on file, which corresponds to 11% of the studied population.
The study population was surveyed twice, in 1990-91 and 2002-03. Among those surveyed, 21 individuals reported that they had diabetes and/or were on treatment for diabetes; although they were not found in the registers. This discrepancy is related to the fact that primary care diagnoses are not included in the national registers.
In the surveyed population, 212 individuals with a verified diabetes diagnosis were identified (Table 4). Among these, 41 men reported diabetes already in 1990-91. These 41 men were all asked about diabetes treatment and 19 of them reported taking insulin. These 19 individuals were regarded as having type 1 diabetes and were excluded from the following analyses. These analyses were hence based on a population of 1,944 individuals who took part in at least one of the surveys.
![]()
Table 4: Diabetes frequencies according to national register and interviews.
View Table 4
As expected, the studied baseline characteristics; i.e., BMI, waist/hip ratio, blood pressure and blood lipids (components of the metabolic syndrome), showed a significant and systematic relationship with T2D (Table 5).
![]()
Table 5: How T2D during follow up relates to lifestyle factors and observations at baseline.
View Table 5
Physical activity estimated in different ways, as well as meal quality and occupation had a significant relationship with T2D. Smoking, alcohol consumption, stress (assessed as experienced demands), and educational level showed no such relationship in crude analyses (Table 5).
Further analyses using multiple regression models showed that physical activity assessed in various ways was significantly associated with a lower risk of T2D (high physical activity: OR=0.55 [95% CI 0.31-0.97], high physical work capacity: OR=0.65 [95% CI 0.47-0.89]). A high meal quality index was also significantly related to a low risk of T2D (OR=0.58 [95% CI 0.35-0.99]) (Table 6). Smoking, alcohol consumption, stress (estimated as experienced demands), occupation and educational level were not related to T2D in these adjusted analyses.
![]()
Table 6: Diabetes (T2D) and lifestyle factors with significant impact on the diabetes risk. Backward stepwise regression analyses with all the lifestyle factors included.
View Table 6
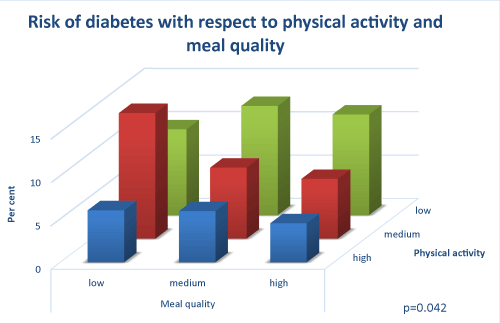
The interaction between physical activity and meal quality was analyzed using three-dimensional diagrams. The effect of physical activity was present among individuals with medium and high meal quality and an effect of meal quality was seen among those with high and medium physical activity (p=0.042). Among those with low physical activity, meal quality seemed to make no difference (Figure 1). When the physical activity index was replaced with physical work capacity in three categories (high, medium and low), a similar picture emerged (p=0.020). No effect of physical capacity was present if the meal quality was low and no effect of meal quality was seen if the physical capacity was low (Figure 2).
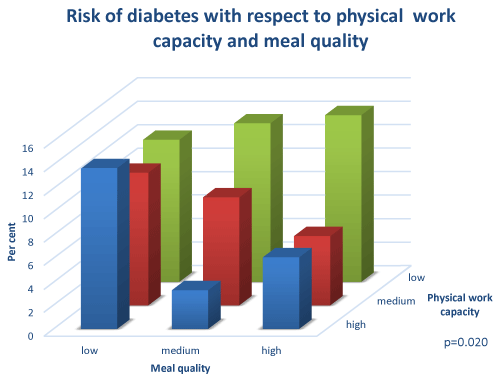
Figure 2: Risk of diabetes with respect to physical work capacity and meal quality.
View Figure 2
Discussion
Our results are well in line with what is known aboutT2D epidemiology [10,25]. The components of the metabolic syndrome had a strong relationship with T2D, as expected. The studied lifestyle factors were related to T2D as expected, but only physical activity and meal quality had a significant impact in the adjusted analyses. Graphic analyses indicate an interaction between physical activity and meal quality, in those individuals with low physical activity seemed not to be �helped by� a high meal quality. Men with high physical activity generally had a low risk of T2D, regard less of meal quality.
The preventive effect of different kinds of diet has been discussed over the years and there is still controversy regarding the optimum design of preventive diets [26-28]. Other studies indicate that a combination of lifestyle factors is associated with a substantial risk reduction [25]. Intervention studies have focused on changes to the diet and physical activity [29]. However, we have not found any study elucidating how the different factors integrate with each other. A Japanese study showed that low physical activity but not recessive calorie intake was associated with T2D [30], and another Japanese study report showed that eating speed was associated with the incidence of diabetes [31]. Finally, an American study supports our findings and reported that breakfast omission and the organization of the meals were related to the T2D risk [32].
A significant relationship between physical activity and prevention of T2D is supported by many studies [9,33,34]. Physical activity is related to other factors with an impact on the risk of T2D, such as adiposity, blood pressure, dyslipidemia and inflammation. It is not clear whether the positive effect of physical activity is due to the exercise per se or results from favorable changes to the body composition [35]. The effect of physical activity may be modified by a number of diabetes genes; however, this modification is supposed to be of moderate magnitude [36,37].
The main strength of this study is a well-defined and controlled population-based cohort documented over a long time, using registers, interviews, questionnaires and tests. The cohort constitutes a representative sample of the Swedish countryside population, as the surveys were performed in nine different districts around the country. The districts were chosen to meet known geographical health gradients [16]. The quality of the data has been evaluated in a number of studies. The internal loss of data is generally low and previously proven methods and validated questionnaires have been used for most aspects [17].
To estimate the meal quality we developed a standardized interview to assess differences between individuals. No validated instrument that would be useful in this context was found in the literature at the time of the first survey. Internal validation of the meal quality index has not shown any disqualifications, as the distribution, standard deviation, skewness and kurtosis all indicate that the variable has a normal distribution.
A weakness of our study may be the relatively small number of individuals with T2D. On the other hand, the cases are well identified both in registers and through interviews. The identification of persons with T2D was carried out using national registers and information from two surveys with an interval of more than ten years. The registers failed to capture all cases, which indicate that our method of retrieving the cases improved the incidence rating. This register short coming is probably related to the fact that doctors in primary care do not report to the national registers. Only doctors affiliated with hospitals have to report consecutively to the registers. Some cases, especially from recent years, have probably been missed, as they could not be assessed in interviews after the second survey.
We estimated physical activity in different ways; physical workload assessed through interviews, self-reported physical leisure activity, and measurement of physical work capacity, as previously described. These estimates of physical activity/capacity are relevant in this context.
Smoking, alcohol consumption and stress had no significant relationship with T2D in this study. We are well aware that experienced job demands, according to Karasek/Theorell, are just one perspective of the broad stress concept. Other methods may of course be used [38].
Conclusion
Physical activity and meal quality were significantly related to T2D and we found an interaction between these two lifestyle factors. The preventive effect of meal quality was seen among physically active individuals. Men with low physical activity had a high risk, regardless of meal quality. High meal quality does not seem to compensate for physical inactivity. The results emphasize the importance of focusing on lifestyle in a comprehensive manner when addressing diabetes prevention. More research addressing the interaction between lifestyle variables is needed.
Acknowledgments
This study was supported by grants from the LRF Research Foundation. Previous surveys were supported by grants from AFA insurance, the LRF Research Foundation and the Swedish Council for Working Life. We especially acknowledge Professor emeritus Lennart Levi for initiating the project idea.
Sources of support: LRF Research Foundation, AFA Insurance, and the Swedish Council for Working Life and Social Research.
References
-
King H, Aubert RE, Herman WH (1998) Global burden of diabetes, 1995-2025: prevalence, numerical estimates, and projections. Diabetes Care 21: 1414-1431.
-
Danaei G, Finucane MM, Lu Y, Singh GM, Cowan MJ, et al. (2011) National, regional, and global trends in fasting plasma glucose and diabetes prevalence since 1980: systematic analysis of health examination surveys and epidemiological studies with 370 country-years and 2�7 million participants. Lancet 378: 31-40.
-
Stringhini S, Tabak AG, Akbaraly TN, Sabia S, Shipley MJ, et al. (2012) Contribution of modifiable risk factors to social inequalities in type 2 diabetes: prospective Whitehall II cohort study. BMJ 345: e5452.
-
Mokdad AH, Ford ES, Bowman BA, Nelson DE, Engelgau MM, et al. (2000) Diabetes trends in the U.S.: 1990-1998. Diabetes Care 23: 1278-1283.
-
Wong ND (2006) Screening and risk stratification of patients with the metabolic syndrome and diabetes. Expert Rev Cardiovasc Ther 4: 181-190.
-
Katulanda P, Ranasinghe P, Jayawardana R, Sheriff R, Matthews DR (2012) Metabolic syndrome among Sri Lankan adults: prevalence, patterns and correlates. Diabetol Metab Syndr 4: 24.
-
Cuevas A1, Alvarez V, Carrasco F (2011) Epidemic of metabolic syndrome in Latin America. Curr Opin Endocrinol Diabetes Obes 18: 134-138.
-
Sanchez-Chaparro MA, Calvo-Bonacho E, Gonzalez-Quintela A, Fernandez-Labandera C, Cabrera M, et al. (2008) Occupation-related differences in the prevalence of metabolic syndrome. Diabetes Care 31: 1884-1885.
-
Hu FB, Manson JE, Stampfer MJ, Colditz G, Liu S, et al. (2001) Diet, lifestyle, and the risk of type 2 diabetes mellitus in women. N Engl J Med 345: 790-797.
-
Mozaffarian D, Kamineni A, Carnethon M, Djouss� L, Mukamal KJ, et al. (2009) Lifestyle risk factors and new-onset diabetes mellitus in older adults: the cardiovascular health study. Arch Intern Med 169: 798-807.
-
Marcinkiewicz A, Szosland D (2010) Selected risk factors of diabetes mellitus among road transport drivers. Int J Occup Med Environ Health 23: 175-180.
-
Nagaya T, Yoshida H, Takahashi H, Kawai M (2006) Policemen and firefighters have increased risk for type-2 diabetes mellitus probably due to their large body mass index: a follow-up study in Japanese men. Am J Ind Med 49: 30-35.
-
Hayashino Y, Yamazaki S, Nakayama T, Sokejima S, Fukuhara S (2010) The association between socioeconomic status and prevalence of diabetes mellitus in rural Japan. Arch Environ Occup Health 65: 224-229.
-
Thelin A, Holmberg S (2014) Type 2 diabetes among farmers and rural and urban referents: cumulative incidence over 20 years and risk factors in a prospective cohort study. Asia Pac J Clin Nutr 23: 301-308.
-
Nerbrand C, Svardsudd K, Horte LG, Tibblin G (1991) Are geographical differences in cardiovascular mortality due to morbidity differences or to methodological differences? The project "myocardial infarction in Mid-Sweden". Scand J Soc Med 19: 154-161.
-
Stiernstr�m EL, Holmberg S, Thelin A, Sv�rdsudd K (1998) Reported health status among farmers and nonfarmers in nine rural districts. J Occup Environ Med 40: 917-924.
-
Holmberg S, Stiernstr�m EL, Thelin A, Sv�rdsudd K (2002) Musculoskeletal symptoms among farmers and non-farmers: a population-based study. Int J Occup Environ Health 8: 339-345..
-
Stiernstr�m EL, Holmberg S, Thelin A, Sv�rdsudd K (2001) A prospective study of morbidity and mortality rates among farmers and rural and urban nonfarmers. J Clin Epidemiol 54: 121-126.
-
Socialstyrelsen (1986) Klassifikation av sjukdomar 1987. Systematisk f�rteckning. Stockholm: Liber/Allm�nna f�rlaget.
-
Socialstyrelsen (1997) International Statistical Classification of Diseases and Related Health Problems, Thenth Revision. (Swedish version), (3rd edn) Uppsala: Almqvist & Wiksell.
-
Ilmarinen J, Knauth P, Klimmer F, Rutenfranz J (1979) The applicability of the Edholm Scale for activity studies in industry. Ergonomics 22: 369-376.
-
Tornvall G (1963) Assessment of physical capabilities. Acta Physiol Scand 58: 17-55.
-
Brunner EJ, Mosd�l A, Witte DR, Martikainen P, Stafford M, et al. (2008) Dietary patterns and 15-y risks of major coronary events, diabetes, and mortality. Am J Clin Nutr 87: 1414-1421.
-
Karasek RA, Theorell T (1990) Healthy Work: Stress, Productivity and the Reconstruction of Working Life. New York: Basic Books.
-
Reis JP, Loria CM, Sorlie PD, Park Y, Hollenbeck A, et al. (2011) Lifestyle factors and risk for new-onset diabetes: a population-based cohort study. Ann Intern Med 155: 292-299.
-
Morimoto A, Ohno Y, Tatsumi Y, Mizuno S, Watanabe S (2012) Effects of healthy dietary pattern and other lifestyle factors on incidence of diabetes in a rural Japanese population. Asia Pac J Clin Nutr 21: 601-608.
-
Salas-Salvad� J, Martinez-Gonz�lez M�, Bull� M, Ros E (2011) The role of diet in the prevention of type 2 diabetes. Nutr Metab Cardiovasc Dis 21: B32-48.
-
(SBU) Sbfmu: Mat vid diabetes. En systematisk litteratur�versikt. In: SBU Rapport. Stockholm: 210.
-
van Dam RM (2003) The epidemiology of lifestyle and risk for type 2 diabetes. Eur J Epidemiol 18: 1115-1125
-
Iijima K, Iimuro S, Ohashi Y, Sakurai T, Umegaki H, et al. (2012) Lower physical activity, but not excessive calorie intake, is associated with metabolic syndrome in elderly with type 2 diabetes mellitus: the Japanese Elderly Diabetes Intervention Trial. Geriatr Gerontol Int 12: 68-76.
-
Sakurai M, Nakamura K, Miura K, Takamura T, Yoshita K, et al. (2012) Self-reported speed of eating and 7-year risk of type 2 diabetes mellitus in middle-aged Japanese men. Metabolism 61: 1566-1571.
-
Mekary RA, Giovannucci E, Willett WC, van Dam RM, Hu FB (2012) Eating patterns and type 2 diabetes risk in men: breakfast omission, eating frequency, and snacking. Am J Clin Nutr 95: 1182-1189.
-
Bassuk SS, Manson JE (2003) Physical activity and the prevention of cardiovascular disease. Curr Atheroscler Rep 5: 299-307.
-
Jefferis BJ, Whincup PH, Lennon L, Wannamethee SG (2012) Longitudinal associations between changes in physical activity and onset of type 2 diabetes in older British men: the influence of adiposity. Diabetes Care 35: 1876-1883.
-
W�rnberg J, Cunningham K, Romeo J, Marcos A (2010) Physical activity, exercise and low-grade systemic inflammation. Proc Nutr Soc 69: 400-406.
-
Qi L, Hu FB, Hu G (2008) Genes, environment, and interactions in prevention of type 2 diabetes: a focus on physical activity and lifestyle changes. Curr Mol Med 8: 519-532.
-
Belkina AC, Denis GV (2010) Obesity genes and insulin resistance. Curr Opin Endocrinol Diabetes Obes 17: 472-477.
-
Egede LE, Dismuke CE (2012) Serious psychological distress and diabetes: a review of the literature. Curr Psychiatry Rep 14: 15-22.