International Journal of Diabetes and Clinical Research
The Burden of Co-morbid Depression in Ambulatory Patients with Type 2 Diabetes Mellitus at Kenyatta National Hospital, Kenya
Kanu Joseph E1*, Otieno CF Frederick1, Karari Emma M1, Okech-Helu Violet2 and Mutai Kenn2
1Department of Clinical Medicine and Therapeutics, University of Nairobi, Nairobi, Kenya
2Kenyatta National Hospital, Nairobi, Kenya
*Corresponding author:
Kanu Joseph E, MB, ChB, MMed, Senior Resident in Medicine, Department of Clinical Medicine and Therapeutics, University of Nairobi, Nairobi, Kenya, E-mail: josephkanu17@yahoo.com
Int J Diabetes Clin Res, IJDCR-3-055, (Volume 3, Issue 1), Research Article; ISSN: 2377-3634
Received: January 05, 2016 | Accepted: March 23, 2016 | Published: March 26, 2016
Citation: Kanu JE, Otieno CFF, Karari EM, Okech-Helu V, Kenn M (2016) The Burden of Comorbid Depression in Ambulatory Patients with Type 2 Diabetes Mellitus at Kenyatta National Hospital, Kenya. Int J Diabetes Clin Res 3:055. 10.23937/2377-3634/1410055
Copyright: © 2016 Kanu JE, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Co-morbid depression is a serious condition in patients with diabetes that negatively affects their self-management, including drug adherence, consequently, the treatment outcomes and quality of life are also affected.
Objective: To determine the burden of co-morbid depression in ambulatory patients with type 2 diabetes at the Kenyatta National Hospital (KNH) and to document their socio-demographic and clinical characteristics and any associated risk factors.
Methods: This was a cross-sectional study done on patients living with type-2 diabetes on follow-up at the diabetes out-patient clinic (DOPC) at the KNH. Systematic sampling method was used to recruit 220 study subjects. The PHQ-9 questionnaire was used to assess for co-morbid depression. Socio-demographic and clinical details were obtained both from the subjects and their medical records. Physical examination was done, including blood pressure and BMI determined. Blood samples were collected from the cubital fossa to measure HbA1C in COBAS INTEGRA system with its reagent in the pre-dilution cuvette for automated analysis of glycated hemoglobin (HbA1c). Statistical associations of patients’ characteristics and co-morbid depression were determined using Chi-square test and Odds Ratios.
Results: The prevalence of co-morbid depression in patients with type 2 diabetes at the DOPC of KNH using the PHQ-9 was 32.3% (95% CI 26.4-38.6%). Of these, depression was mild in 42.3%, moderate in 40.8% and severe in 16%. Subjects with co-morbid depression were: aged 65years and above (p = 0.006), over-weight/obese (p = 0.035), and had longer duration of diabetes of 5years and above. The presence of co-morbid depression was significantly associated with poor glycaemic control, (OR = 3.3, 95% CI, 1.6 - 6.8, p = 0.001).
Conclusions: About one-third (32.3%) of the study subjects with type 2 diabetes had co-morbid depression. Patients with type 2 diabetes who are at higher risk (older age of 65 years and above, long duration of diabetes, poor glycaemic control and presence of diabetes-related complications,) should be screened for co-morbid depression.
Background
Diabetes is a metabolic disorder characterized by hyperglycemia resulting from defects in insulin secretion, insulin utilization, or both [1]. The vast majority of diabetes is type 2 diabetes comprising about 90% of cases [1].
Diabetes is a chronic disease which affects virtually every organ in the human system. The global prevalence of diabetes is continuously rising and the World Health Organization (WHO) projected that 300 million people will suffer from diabetes by 2025 [2].
The prevalence of diabetes in sub-Saharan Africa is expected to triple by 2030, making it a cause for concern not only for health professionals but also policy makers as they initiate strategies to tackle it [3].
Kenya, like other developing countries, is experiencing this emerging diabetes epidemic. It is estimated that the prevalence of diabetes in the country is about 3.3%. This figure is projected to rise to 4.5% by 2025 if this trend continues, according to Kenya National Diabetes Strategy [4]. Diabetes-related co-morbidities and complications are expected to rise in parallel with the rising numbers of diabetes.
Depression is a chronic psychopathological state that involves a triad of symptoms with low or depressed mood, anhedonia, and low energy or fatigue. Other symptoms, such as sleep and psychomotor disturbances, feeling of guilt, low self- esteem, suicidal tendencies, as well as autonomic and gastrointestinal disturbances, are also present [5].
The lifetime prevalence of depression is as high as 20% in the general population worldwide with a female to male ratio of about 5:2 [5]. According to WHO, depression is ranked as the fourth global burden of disease, responsible for the greatest proportion of burden associated with non-fatal health outcomes and account for approximately 12% of total years lived with disability [6]. It is predicted to become second only to ischemic heart disease as a cause of morbidity worldwide [7].
Patients with type-2 diabetes have a rate of major depression 1.6-2 times higher than those in the general population affecting one in every 10 diabetic patients [8].
Diabetes distress (concerns and worries of diabetes and its management) is associated with depressive symptoms [9]. Co-morbid depression is associated with poor self-care [10], poor adherence to medication [11], chronic complications [12-14] and higher mortality rates [15].
Significance of the Study
Depression is a serious co-morbid condition in diabetes patients that negatively affects self-management, drug adherence, treatment outcomes and quality of life. Knowing the burden of the clinical condition heralds the first step to managing it. There are scarce published data on depression in ambulatory type 2 diabetes in this region. Therefore the study was done to determine the prevalence and severity of co-morbid depression in ambulatory type 2 diabetes patients at KNH and to document their socio-demographic and clinical characteristics.
Methods
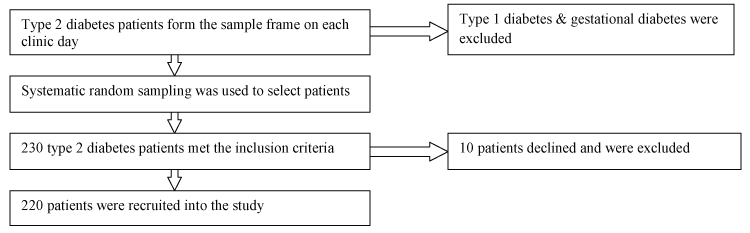
This was a descriptive cross-sectional study that we conducted at the diabetes out-patient clinics in KNH. The study population consisted of patients of age ≥ 30 yrs with a diagnosis of type 2 diabetes for ≥ 1 year and followed up at the diabetes clinic. We used a systematic sampling method to recruit the subjects wherein every 2nd patient on the minor clinic day and every 4th on the major clinic day that met the inclusion criteria was selected (Figure 1).
To collect socio-demographic and clinical data standard questionnaire was used. Patient Health Questionnaire 9 (PHQ-9), was used to assess symptoms of depression [16] (Table 1) (Appendix). PHQ-9 assesses the extent of bother by symptoms of Depressive illness in the previous two (2) weeks on a Likert scale (not-at-all to nearly-every-day). The symptoms range from interest or pleasure in doing tasks, feeling of hopelessness, trouble falling asleep, feeling tired, feeling bad about self, trouble with concentration, slow speaking or restlessness and a feeling of being better dead. The last, tenth, question on the PHQ-9 tool used performs Functional Health Assessment by seeking to know the psycho-social functioning of the study subjects is affected by the emotional difficulties. PHQ-9 has been validated locally and there is a Kiswahili translation available. The standard mercury sphygmomanometer was used to measure Blood Pressure (mmHg), weighing scale for weight (kilograms) and a stadiometer to measure height (meters).
![]()
Table 1: Socio - demographic characteristics of the study subjects.
View Table 1
Inclusion criteria
1. The patients of age ≥ 30 years with a documented diagnosis of type 2 diabetes of ≥ 1 year attending the diabetes clinic and gave informed consent.
2. Participants who were able to speak and understand Kiswahili and/or English.
Exclusion criteria
The patients with psychiatric illness other than depression and patients who did not consent to participate were excluded.
Sample size determination
Using the Cochran formula [17], a sample size of 220 diabetic mellitus patients was calculated to estimate prevalence of co-morbid depression at 95% confidence interval within 6.2% precision error.
Definition of study variables
Depression: PHQ-9 score of ≥ 10 was described as presence of clinical depression, a level of score at which there was optimal discriminatory power to make diagnosis of Major Depressive illness [16].
Severity of depression: Clinical depression was categorized into Moderate (10-14), moderately severe (15-19) and Severe (20-27) based on the PHQ-9 scores in the brackets.
Body mass index (BMI): This was calculated and expressed in kg/m2 and classified as: Underweight (< 19 kg/m2), Normal (20-24.9 kg/m2), Pre-obese/overweight (25-29.9 kg/m2) and Obese (≥ 30 kg/m2) as per The International Obesity Task Force of WHO 2000 [18].
Blood pressure: A subject was considered to have arterial hypertension if he/she was a on blood pressure lowering drugs from the hospital records. For subjects with no prior history of hypertension, a blood pressure ≥ 140/90 mmHg was considered to have hypertension. (JNC 8 Guidelines 2014) [19].
Diabetes control: This was assessed by measuring HbA1C, using COBAS INTEGRA machine, in an automated platform. HbA1C ≤ 7% was categorized as good/optimal metabolic control and HbA1C > 7% as poor/sub-optimal control (ADA 2015 Recommendations) [20].
Data analysis
Statistical analysis was done using IBM SPSS statistics v21 (2012). Prevalence of co-morbid depression was calculated and presented as a percentage of the total study subjects, at 95% confidence interval. In addition, the proportion with co-morbid depression was presented as percentages. Factors associated with depression were analyzed using Chi square tests and odds ratios (OR). Statistically significant factors in the univariate associations were put in binary logistic regression model to determine factors independently associated with co-morbid depression while controlling for confounding effects. The statistical tests were performed at 5% level of significance (p value less or equal to 0.05 will be interpreted as significant) (Table 2 and Table 3).
![]()
Table 2: Factors associated with co - morbid depression in the study patients.
View Table 2
![]()
Table 3: Independent factors associated with Co - morbid Depression in the study subjects.
View Table 3
Ethical Considerations
Permission and approval was obtained from the Department of Clinical Medicine and Therapeutics of the University of Nairobi and the Institution’s Ethical Review Committee for research, before data collection.
We obtained consent from the study subjects after providing them with adequate information about the study. Blood pressure, BMI and HBA1C results were communicated to patients as well as their primary physicians for clinical decision-making. Those who were found to have depression were referred to the mental health department for further care. Blood samples were used only for the intended purpose and were discarded after the study.
Results
A total of 220 participants with type 2 diabetes mellitus were recruited into the study. Below is a summary of their characteristics.
Discussion
The study was set to determine the burden of co-morbid depression in ambulatory patients living with type 2 diabetes at the diabetes out-patient clinic of KNH using the PHQ-9 questionnaire.
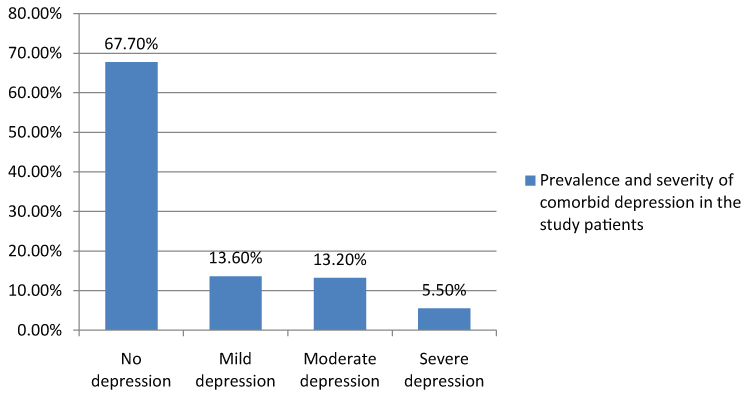
The prevalence of co-morbid depression in the study subjects in the out-patient clinic of this hospital was found to be 32.3%, 95% CI 26.4-38.6%, and more than half (18.7%) of them had moderate to severe depression. This is a significant proportion of people already afflicted by a chronic disease (Figure 2).
This prevalence of co-morbid depression is lower than that reported in a cross-sectional study by Ndetei DM et al. [21], also done in Kenya which included 2,770 general medical out-patients across 10 different health facilities. They reported that 42.3% of their study patients had clinical depression using BDI [21]. The cohort of patients in the study of Ndetei et al. had various diagnostic labels that included, but not limited to, cancers, respiratory diseases, cardiovascular diseases, diabetes, and HIV disease. More than half of the patients suffering from cancer (59.6%) and HIV/AIDS (52.2%) had co-morbid depression. The heterogeneous diagnostic labels and data collection tool would probably explain the observed differences in prevalence of depression compared to our study.
The overall prevalence of co-morbid depression in our study was comparable to other studies done in sub-Saharan Africa on patients with type 2 diabetes in the out-patient setting. Teklay et al. in Ethiopia found a prevalence of 33% using PHQ-9, in their cross-sectional, hospital-based study of 267 diabetic out-patients, 2011 [22], Camara A. et al. in Guinea found a prevalence of 34.4%, using HADS tool in a cross-sectional, hospital-based study, 2014 [23], and Akena D. et al. in Uganda, in their cross-sectional survey used PHQ-9 on patients with type 2 diabetes and found a prevalence of co-morbid depression of 34.8% [24]. This similarity in the prevalence of co-morbid depression in patients with type 2 diabetes may be due to shared psycho-social stressors among sub-Saharan Africans. The countries in sub-Saharan Africa share health system challenges and comparable poverty indices of their populations that may help explain part of this similarity in prevalence. However the prevalence of depression in our study was lower than that reported by Amit R et al. in India [25], of 41%, using PHQ-9 in a cross-sectional hospital-based study, 2009. It was relatively higher than the prevalence reported by studies in the developed world on patients with type2 diabetes. Ali S. et al. in the UK [26] reported a prevalence of 9.3%, using CESD tool in their cross-sectional study, 2009 and Chaoyang Li et al. in the USA [27] found a prevalence of 8.3%, using PHQ-9 in their population-based survey, 2008.
The prevalence reported in these studies differ, probably due to variation in characteristics of study participants coming from populations of multiple social and cross-cultural backgrounds, level of income of countries [28] use of different psychometric tools in studies with varying definitions of depression [29], and the diversity in psycho-social stressors from one community to another in the many countries where the studies were conducted.
In our study, the mean age of subjects with co-morbid depression was 59.1 ± 8.5 years, similar to that of the overall study population of 57.1 ± 8.6 years. Forty five (45.5%) percent of the study patients aged above 65years had co-morbid depression compared to 15.8% of the younger age group of 35-44 years. Old age above 65yrs was significantly associated with presence of co-morbid depression. (p = 0.006) in univariate analysis. This age is associated with diabetes-related complications, co-morbidities and therefore added hurdle in coping with diabetes care. Other investigators like Nitin J et al. in India in a cross-sectional study, 2010 [30] and Camara A. et al. in Guinea [22], had similar finding, but Akena D et al. [23]. In their cross-sectional study in Uganda, reported that their study subjects with co-morbid depression were younger, and they were also poorer and suicidal.
We found no significant association between gender and co-morbid depression (p = 0.130), apparently fewer females (28.5%) had depressive symptoms than the males (38.2%) in this study. We did not specifically interrogate the obtaining psycho-social support systems of our study subjects beyond knowing their marital and employment status. Even then, the marital status, employment and the level of formal education were not significantly associated with presence of co-morbid depression (p = 0.783, p = 0.110 and p = 0.261 respectively) in this study.
The study of Nitin J et al. in India [18] and a multicenter cross-sectional study of Ali Khan et al. in Pakistan, 2010 [19], both found female gender, among other risk factors, to be associated with co-morbid depression. Katon WJ et al. [11], in a longitudinal study, Tellez-Zenteno JF et al. [31], in a cross-sectional study of 189 subjects in Mexico, found female gender, young age, poor psycho-social support, low formal education and socio-economic status, amongst other risk factors, were associated with presence of co-morbid Depression in their patients with type 2 diabetes.
Thirty nine, (39.3%) percent, of the study subjects who were either on combination (OGLAs + insulin) or insulin-only therapy, had co-morbid depression compared to 26.3% on OGLAs-only but there was no significant association between treatment groups and Co-morbid Depression. However, medication burden as well as daily insulin injections are potential stressors in the group of patients who are on injections.
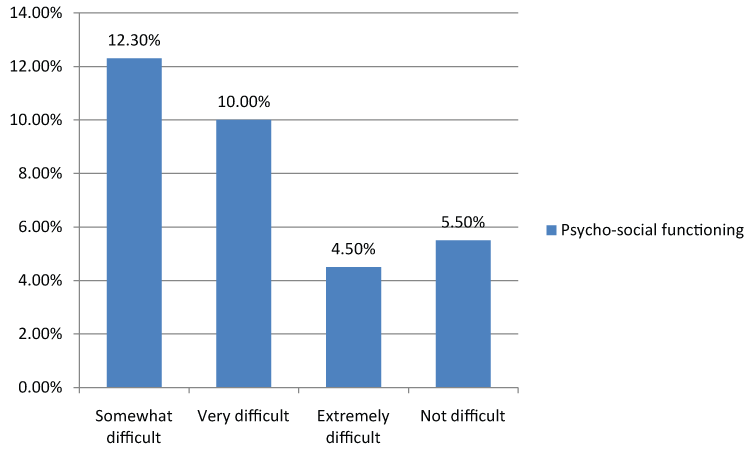
We observed that high BMI ≥ 25 kg/m2 (overweight and obese) was significantly associated with co-morbid depression (p = 0.035) in univariate, but collapsed in multivariate analysis. Obesity in some patients with diabetes: can be a consequence of reduced physical activities, an observation in those with co-morbid depression, as reported by Lin EH et al. [32], and unhealthy diets, as reported by Dipnal JF et al. [33]. The tenth item on PHQ-9 tool assesses physical and psycho-social function. In this study, over 80% of the subjects with Co-morbid Depression reported difficulty with physical and psycho-social function of varying proportions. We did not explore the dietary discretions and physical activity status of our study patients (Figure 3).
There was a significant association between longer duration of diabetes (5 yrs and above) and co-morbid depression. (p = 0.044). Other workers, Tapash et al. in a cross-sectional study, 2011, in Bangladesh [34], Nitin J et al. in India [29], Ali Khan et al. in Pakistan [35] also reported that longer duration of diabetes was significantly associated with co-morbid depression. The patients with longer duration of diabetes are more likely to have co-existing complications of diabetes and high disease burden with additional health care challenges. These factors are potential stressors sufficient to drive depression (or distress) in such patients with diabetes.
There was a significant association between presence of co-morbid depression and poor glycemic control (p = 0.006). Many studies, for example, Bot et al. in a multicenter cross-sectional study in Netherlands [36] and Marcello et al. in a cross-sectional study in Brazil [37], have reported the association of Depression with poor glycemic control in their study patients. This is an important observation that puts these patients at higher risk of complications associated with poor glycaemic control.
Conclusions
Co-morbid Depression occurred in 1 in 3 of the study subjects with type 2 diabetes, which is a fairly high prevalence. Poor glycaemic control was consistently associated with Co-morbid depression therefore, patients with type 2 diabetes should be screened for Co-morbid depression. However, other potential risk factors, (older age of 65 yrs and above, long duration of diabetes and presence of diabetes-related complications) should be screened for the same and treated.
Study Limitations
1. This study is a cross-sectional study, of a small sample size per formed at a single center, a tertiary hospital, therefore not representative of the general population in Kenya.
2. Cross-sectional design of this study limits one to infer causality between Depression and Diabetes.
3. We did not determine the medication adherence, diets, psycho-social support levels and systems nor actively searched diabetes-related complications in the patients.
Author contributions
Kanu Joseph E, josephkanu17@yahoo.com: Design of study, data collection, major financing, read the drafts and made in-put. Corresponding author.
Otieno Frederick CF, cfotieno@gmail.com: Design of the study, part financing, wrote all the drafts.
Karari Emma M, emkarari@essentialcardio.com: Design of study,read the drafts and made in-put.
Okech-Helu, Violet, Design of the study, read the drafts.
MutaiKenn, mutaikk@gmail.com: Participated in the design, sample size calculation and statistical analysis.
References
-
American Diabetes Association (2010) Position Statement on the diagnosis and classification of diabetes mellitus, Diabetes Care 33: S62-S69.
-
King H, Aubert RE, Herman WH (1998) Global burden of diabetes, 1995-2025: Prevalence, numerical estimates, and projections. Diabetes Care 21: 1414-1431.
-
Nyenwe EA, Odia OJ, Ihekwaba AE, Ojule A, Babatunde S (2003) Type 2 diabetes in adult Nigerians: a study of its prevalence and risk factors in Port Harcourt, Nigeria. Diabetes Res Clin Pract 62: 177-185.
-
Kenya National Diabetes Strategy 2010 -2015, Ministry of Public Health and Sanitation, pages 3-4.
-
Brigitta B (2002) Pathophysiology of depression and mechanisms of treatment. Dialogues Clin Neurosci 4: 7-20.
-
World Health Organization (2012) Revised global burden of disease (GBD) 2002 estimates, 2005.
-
Lester H, Howe A (2008) Depression in primary care: three key challenges. Postgrad Med J 84: 545-548.
-
Markowitz SM, Gonzalez JS, Wilkinson JL, Safren SA (2011) A review of treating depression in diabetes: emerging findings. Psychosomatics 52: 1-18.
-
van Bastelaar KM, Pouwer F, Geelhoed-Duijvestijn PH, Tack CJ, Bazelmans E, et al. (2010) Diabetes-specific emotional distress mediates the association between depressive symptoms and glycaemic control in Type 1 and Type 2 diabetes. Diabet Med 27: 798-803.
-
Gonzalez JS, Peyrot M, McCarl LA, Collins EM, Serpa L, et al. (2008) Depression and diabetes treatment nonadherence: a meta-analysis. Diabetes Care 31: 2398-2403.
-
Katon W, Russo J, Lin EH, Heckbert SR, Ciechanowski P, et al. (2009) Depression and diabetes: factors associated with major depression at five-year follow-up. Psychosomatics 50: 570-579.
-
Lin EH, Rutter CM, Katon W, Heckbert SR, Ciechanowski P, et al. (2010) Depression and advanced complications of diabetes: a prospective cohort study. Diabetes Care 33: 264-269.
-
Yu MK, Katon W, Young BA (2013) Diabetes self-care, major depression, and chronic kidney disease in an outpatient diabetic population. Nephron Clin Pract 124: 106-112.
-
Pouwer F, Beekman AT, Nijpels G, Dekker JM, Snoek FJ, et al. (2003) Rates and risks for co-morbid depression in patients with Type 2 diabetes mellitus: results from a community-based study. Diabetologia 46: 892-898.
-
Bruce DG, Davis WA, Starkstein SE, Davis TM (2005) A prospective study of depression and mortality in patients with type 2 diabetes: the Fremantle Diabetes Study. Diabetologia 48: 2532-2539.
-
Gilaye B, Williams MA, Lemma S, Deyessa N, Bahretibeb Y, Shibre T, et al. (2013) Validity of the Patient Health Questionnaire-9 for depression screening and diagnosis in East Africa. Psychiatry Res 210: 653-661.
-
Cochran WG (1977) Sampling Techniques. (3rd edn), John Wiley& Sons, New York.
-
The International Obesity Task Force of WHO 2000 (2004) Proposed classification of weight by body mass index(BMI). Int. J. Obes. 28:152-158.
-
James PA, Oparil S, Carter BL, Cushman WC, Dennison-Himmelfarb C, et al. (2014) 2014 evidence-based guideline for the management of high blood pressure in adults: report from the panel members appointed to the Eighth Joint National Committee (JNC 8). JAMA 311: 507-520.
-
(2015) Standards of Medical care in Diabetes-2015. Diabetes Care 38: S1-S2.
-
Ndetei DM, Khasakhala LI, Kuria MW, Mutiso VN, Kokonya DA, et al. (2009) The prevalence of mental disorders in adults in different level general medical facilities in Kenya: a cross-sectional study. Ann Gen Psychiatry 8: 1.
-
Teklay G, Hussien J, Tesfaye O (2013) Non-adherence and associated factors among type 2 diabetic patients in Jimmia University Specialized Hospital, Southwest Ethiopia. J Med Sci 13: 578-584.
-
Camara A, Baldé NM, Enoru S, Bangoura JS, Sobngwi E, et al. (2014) Prevalence of anxiety and depression among diabetic African patients in Guinea: Association with HbA1c levels. Diabetes Metab 41: 62-68.
-
Akena D, Kadama P, Ashaba S, Akello C, Kwesiga B, et al. (2015) The association between depression, quality of life and the healthcare expenditure of patients with diabetes mellitus in Uganda. J Affect Disord 174: 7-12.
-
Raval A, Dhanaraj E, Bhansali A, Grover S, Tiwari P (2010) Prevalence & determinants of depression in type 2 diabetes patients in a tertiary care centre. Indian J Med Res 132: 195-200.
-
Ali S, Davies MJ, Taub NA, Stone MA, Khunti K (2009) Prevalence of diagnosed depression in South Asian and white European people with type 1 and type 2 diabetes mellitus in a UK secondary care population. Postgrad Med J 85: 238-243.
-
Li C, Ford ES, Strine TW, Mokdad AH (2008) Prevalence of Depression among U.S. Adults with Diabetes: Findings from the 2006 Behavioral Risk Factor Surveillance System. Diabetes Care 31: 105-107.
-
Mendenhall E, Norris SA, Shidhaye R, Prabhakaran D (2014) Depression and type 2 diabetes in low- and middle-income countries: a systematic review. Diabetes Res Clin Pract 103: 276-285.
-
Holt RI, de Groot M, Lucki I, Hunter CM, Sartorius N, et al. (2014) NIDDK International conference report on diabetes and depression: current understanding and future directions. Diabetes Care 37: 2067-2077.
-
Joseph N, Unnikrishnan B, Raghavendra Babu YP, Kotian MS, Nelliyanil M (2013) Proportion of depression and its determinants among type 2 diabetes mellitus patients in various tertiary care hospitals in Mangalore city of South India. Indian J Endocrinol Metab 17: 681-688.
-
Téllez-Zenteno JF, Cardiel MH (2002) Risk factors associated with depression in patients with type 2 diabetes mellitus. Arch Med Res 33: 53-60.
-
Lin EH, Katon W, Von Korff M, Rutter C, Simon GE, et al. (2004) Relationship of depression and diabetes self-care, medication adherence, and preventive care. Diabetes Care 27: 2154-2160.
-
Dipnall JF, Pasco JA, Meyer D, Berk M, Williams LJ, et al. (2015) The association between dietary patterns, diabetes and depression. J Affect Disord 174: 215-224.
-
Roy T, Lloyd CE, Parvin M, Mohiuddin KG, Rahman M (2012) Prevalence of co-morbid depression in out-patients with type 2 diabetes mellitus in Bangladesh. BMC Psychiatry 12: 123.
-
Khuwaja AK, Lalani S, Dhanani R, Azam IS, Rafique G, et al. (2010) Anxiety and depression among outpatients with type 2 diabetes: A multi-centre study of prevalence and associated factors. Diabetol Metab Syndr 2: 72.
-
Bot M, Pouwer F, de Jonge P, Tack CJ, Geelhoed-Duijvestijn PH, et al. (2013) Differential associations between depressive symptoms and glycaemic control in out-patients with diabetes. Diabetic Medicine 30: e115-122.
-
Papelbaum M, Moreira RO, Coutinho W, Kupfer R, Zagury L, et al. (2011) Depression, glycaemic control and type 2 diabetes. Diabetol Metab Syndr 3: 26.