Journal of Dermatology Research and Therapy
Fluoroscopy-Induced Chronic Radiodermatitis
Tugba Falay, Vefa Aslı Erdemir, Sevil Savaş, Mehmet Salih Gürel and Ezgi Ozkur*
Department of Dermatology, Istanbul Training and Research Hospital, Turkey
*Corresponding author:
Ezgi Ozkur, Department of Dermatology, Istanbul Training and Research Hospital, Kasap Ilyas Mahallesi, Org. Abdurrahman Nafiz Gürman Cd., 34098, Istanbul, Turkey, Tel: +905303886781, E-mail: ezgierdal@hotmail.com
J Dermatol Res Ther, JDRT-2-031, (Volume 2, Issue 4), Case Report; ISSN: 2469-5750
Received: June 24, 2016 | Accepted: August 27, 2016 | Published: August 29, 2016
Citation: Falay T, Erdemir VA, Savaş S, Gürel MS, Ozkur E (2016) Fluoroscopy-Induced Chronic Radiodermatitis. J Dermatol Res Ther 2:031. 10.23937/2469-5750/1510031
Copyright: © 2016 Falay T, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Fluoroscopy induced chronic radiation dermatitis (FICRD) is a rare complication which can be difficult to diagnose and treat. Recently fluoroscopy use has increased and the diagnostic and the theuropathic fluoroscopy procedures are becoming more complex; therefore incidence of FICRD is rising. Because of presentation often occurs after months or years patients are sometimes unaware of exposure to radiation. Early diagnosis is important for both therapy and radiation-induced malignancies. We report these cases to emphasize the importance of recognizing fluoroscopy as a cause of chronic radiation dermatitis which requires an early diagnosis and a good clinical follow-up.
Introduction
Radiation dermatitis is related to the traditional x-ray radiation. Soon after the discovery of x-ray, the skin symptoms were defined as acute dermatitis in 1895 and then chronic radio dermatitis in 1899 [1]. Fluoroscopy is a visualization method which based on X-ray and has a real time vision through a device called fluoroscope. Today, the developments in the interventional radiology that uses the fluoroscopy guided procedures have enhanced the prognosis of cardiac diseases therefore an increasing number of chronic radiation dermatitis cases caused by fluoroscopy have been reported in recent years [2].
Cases
Case 1
A 84-year-old male presented to our dermatology clinic with a 2-year history of a painful non healing ulcer on his back. Physical examination revealed a well demarcated, rectangular-shaped, indurated, reticulated erythematous atrophic plaque with telangiectasia (Figure 1A). There was sharply circumscribed ulcer with a yellow sticky fibrin and thick yellow-brown crust on the centre of the lesions. Clinical impression was a radiation dermatitis; however, the patient denied a history of radiation exposure. A punch biopsy was performed and on histopathological examination thickening on the blood vessel walls and swelling on the endothelium cells, pleomorphic, bizarre-looking fibroblastic cells with big hyperchromatic nucleus along with eosinophilic homogenized collagen fibers in dermis was observed (Figure 2A and Figure 2B). Further investigation of the patient’s history revealed a coronary artery bypass graft surgery 20 years ago and coronary artery stenting 2 years ago which lasted 8 hours. With the clinical and histopathologic findings, the diagnosis of FICRD was established.
.
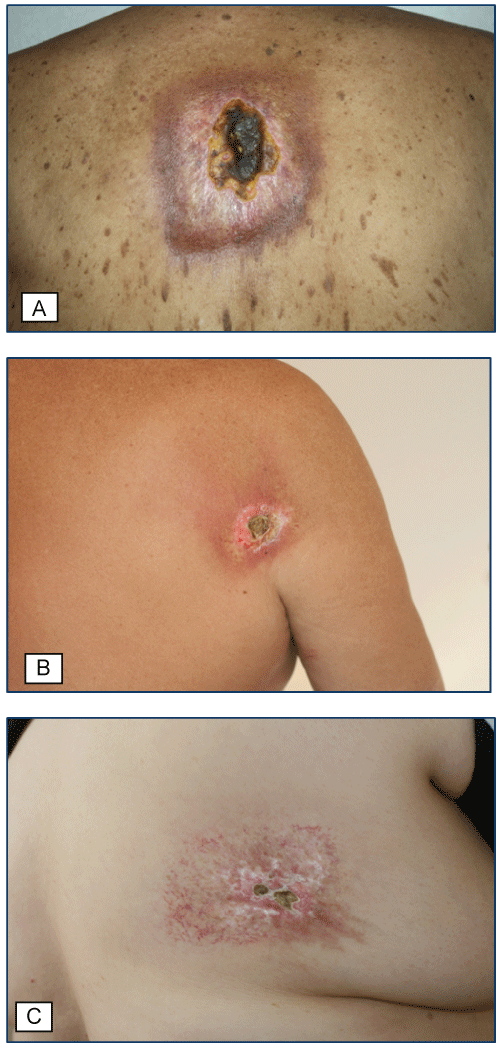
Figure 1: A) A well demarcated, rectangular-shaped, reticulated erythematous atrophic plaque with overlying telangiectasia on interscapular region and sharply circumscribed ulcer with thick yellow-brown crust on the centre of the lesions (Case 1); B) A well demarcated, angulated, erythematous atrophic plaque with overlying telangiectasia on the lateral side of right scapula and an ulcer with thick brown crust on the upper part of the lesion (Case 2); C) A well demarcated, rectangular-shaped, reticulated erythematous atrophic plaque with overlying telangiectasia on right dorsolateral back and an ulcer with hard thick crust on the right side of the lesion (Case 3).
View Figure 1
.
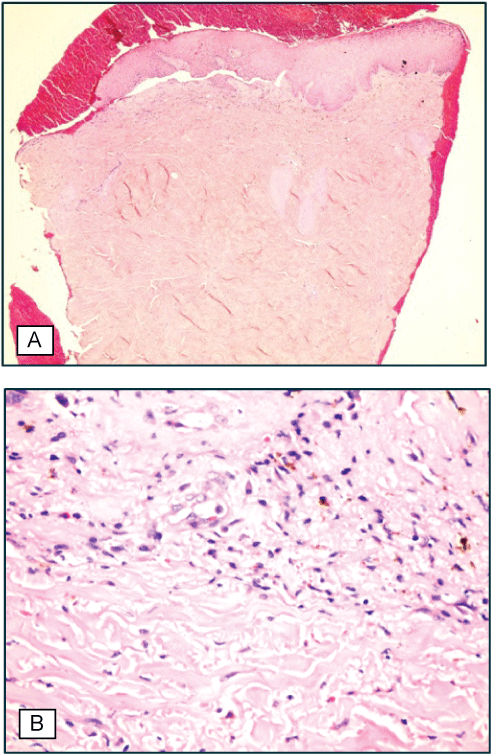
Figure 2: Case 1. A) Irregular acanthosis in epidermis, oedema and perivascular infiltrate consisting of inflammatory cells in dermis; B) Abnormal fibroblasts between homogenized collagen and sclerotic dermis.
View Figure 2
Case 2
A 73-year-old male applied with a 5 month history of itchy non healing wound on the back of right shoulder. In his dermatological examination; a well demarcated, angulated, erythematous atrophic plaque with telangiectasia was observed on the lateral side of right scapula (Figure 1B). On histopathological examination of the punch biopsy specimen, loss of epidermis, interstitial and perivascular mixed type inflammatory cell infiltration, eosinophilic appearance of collagen fibers and thickness and fibrin exudation in dermis were observed. Although this patient also denied history of radiation exposure, it was found out that he had been through 2 diagnostic cardiac catheterization four years ago, and in the same year, he had had 3 coronary artery stenting. In the light of these findings, the patient was diagnosed as FICRD.
Case 3
A 63-year-old female, who applied with a 13 years history of itchy non healing wound on the right low part of the back. Physical examination revealed a well demarcated, reticulated erythematous atrophic plaque with telangiectasia was observed on her right dorsolateral back (Figure 1C). Patient had a history of prolonged cardiac radiofrequency catheter ablation 13 years ago which lasted 5 hours. Several weeks after procedure, the patient was treated with acyclovir for a presumed diagnosis of herpes zoster of the corresponding area. Despite many different wound care efforts in many different hospitals, patient reported that the ulcer is never wholly healed, and got worse in time. A punch biopsy was performed and histopathological findings showed roughening, swelling, eosinophilic and partly hyalinized appearance of collagen bundles and an increase in the number of the elastic fibers in dermis. With the history, clinical and histopathological findings, diagnosis of FICRD was established.
Discussion
Interventional fluoroscopy provides real-time radiologic visualization during a variety of interventional and diagnostic procedures. In 1994, Food and Drug Administration (FDA) warn the radiologists and the cardiologists for skin damage caused by the radiation after prolonged exposure to fluoroscopic procedures [3].
The radiopaque contrast agent flow injected into the body is visualized on fluoroscopy method. Even though the fluoroscopic X-ray rapidly diminishes in the tissue, the entry point of the beam is exposed to the maximum level of radiation [4]. The ionized radiation causes keratinocyte damage on the basal layer; inflammation starts and the cell proliferation is interrupted [5].
The symptoms may start days, months or years after procedure. The threshold dose of radiation that causes skin damage is specified as 2 Gy. The necessary exposure for chronic radiodermatitis induced by fluoroscopy is 10-12 Gy. Moreover, the period between the radiation episodes, the size and the location of the exposed area, smoking, obesity, diabetes mellitus, thyroid diseases, collagen tissue diseases and some drugs may increase skin damage [6]. Actually, the radiation dose given during the fluoroscopy is low and does not exceed the threshold dose for the skin damage. However when the duration of exposure is prolonged or multiple procedures performed within a short time whom always be aware of risk of FICRD. Therefore, follow up is important especially for the patients that had > 10 Gy radiation dose [7].
The diagnosis of FICRD depends on the clinical findings and the former radiation exposure of the affected area. Radiation dermatitis following coroner procedures is mostly seen on the midline of back, scapular area, right anterolateral chest and below the right axilla [8]. Generally, even not necessary, there is acute radiation dermatitis history before chronic radiation dermatitis. While erythema, epilation, dermal atrophy are observed in acute dermatitis, telengiectasia, ulceration, and necrosis are apparent in chronic radiation dermatitis [7]. Its shape is generally geometric and angular. Clinically, it may simulate morphea, erythema ab igne and fixed drug eruption [9,10]. Histopathologically, chronic radiodermatitis is characterized by epidermal atrophy, ulceration, telangiectasic vessels, thickened and sclerotic dermal collagen bundles that include atypical stellate fibroblasts and the loss of adnexal structures [11].
Treatment of radiation dermatitis can include topical, intralesional steroids or surgical excision grafting but there are no guidelines on definitive treatment [12,13]. mProvider education is essential for the prevention of FICRD. Physicians involved in this type of interventions should be aware of FICRD and be precautious of radiation dosage and minimization of the area exposed to radiation.
References
-
Food and Drug Administration Mandatory Device Reporting.
-
Reichman EF (2014) Fluoroscopy-induced radiation dermatitis. J Emerg Med 47: e117-119.
-
(1994) Public health advisory: avoidance of serious X-ray-induced skin injuries to patients during fluoroscopically-guided procedures. Food and Drug Administration, Center for Devices and Radiological Health, Rockville.
-
Wagner LK, Eifel PJ, Geise RA (1994) Potential biological effects following high X-ray dose interventional procedures. J Vasc Interv Radiol 5: 71-84.
-
Ryan JL (2012) Ionizing radiation: the good, the bad, and the ugly. J Invest Dermatol 132: 985-993.
-
Miller DL, Balter S, Noonan PT, Georgia JD (2002) Minimizing radiation-induced skin injury in interventional radiology procedures. Radiology 225: 329-336.
-
Balter S, Hopewell JW, Miller DL, Wagner LK, Zelefsky MJ (2010) Fluoroscopically guided interventional procedures: a review of radiation effects on patients' skin and hair. Radiology 254: 326-341.
-
Spiker A, Zinn Z, Carter WH, Powers R, Kovach R (2012) Fluoroscopy-induced chronic radiation dermatitis. Am J Cardiol 110: 1861-1863.
-
Schecter AK, Lewis MD, Robinson-Bostom L, Pan TD (2003) Cardiac catheterization-induced acute radiation dermatitis presenting as a fixed drug eruption. J Drugs Dermatol 2: 425-427.
-
Henry MF, Maender JL, Shen Y, Tschen JA, Subrt P, et al. (2009) Fluoroscopy-induced chronic radiation dermatitis: a report of three cases. Dermatol Online J 15: 3.
-
Anderson EB, Draft KS, Lee RA, Elenitsas R (2006) Update in dermatopathology. Am J Clin Pathol 125: S50-70.
-
Koenig TR, Wolff D, Mettler FA, Wagner LK (2001) Skin injuries from fluoroscopically guided procedures: part 1, characteristics of radiation injury. AJR Am J Roentgenol 177: 3-11.
-
Koenig TR, Mettler FA, Wagner LK (2001) Skin injuries from fluoroscopically guided procedures: part 2, review of 73 cases and recommendations for minimizing dose delivered to patient. AJR Am J Roentgenol 177: 13-20.





