International Journal of Oral and Dental Health
Hygienic and Dietetic Guidelines for Implant-Supported Full-Arch Immediate Loading Prostheses
Menini M1, Dellepiane E1*, Pesce P1, Zunino P1, Bevilacqua M1, Drago C2, Baldi D1 and Pera P1
1Division of Implant Prosthodontics, Department of Surgical Sciences, University of Genoa, Italy
2Marquette University School of Dentistry, Milwaukee, Wisconsin, USA
*Corresponding author: Dr. Elena Dellepiane, Department of Prosthodontics (Pad. 4), University of Genoa, Ospedale S. Martino, L. Rosanna Benzi 10, 16132 Genova, Italy, Tel : + 39 0103537421, Mobile: +39 3497318187, Fax: + 39 0103537402, E-mail: elena.dellepiane@unige.it, elena.dellepiane@virgilio.it
Int J Oral Dent Health, IJODH-1-018, (Volume 1, Issue 4), Review Article; ISSN: 2469-5734
Received: September 09, 2015 | Accepted: November 07, 2015 | Published: November 09, 2015
Citation: Menini M, Dellepiane E, Pesce P, Zunino P, Bevilacqua M, et al. (2015) Hygienic and Dietetic Guidelines for Implant-Supported Full-Arch Immediate Loading Prostheses. Int J Oral Dent Health 1:018. 10.23937/2469-5734/1510018
Copyright: © 2015 Menini M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Proper oral hygiene and diet are important considerations for success in implant prosthodontics. However, detailed hygienic and dietetic guidelines for patients rehabilitated with implant-supported, immediate loading prostheses are lacking in the literature.
Methods: The authors have developed a dietary and hygienic protocol for patients rehabilitated with implant-supported, full-arch, immediate loading prostheses in order to avoid occlusal overloads during osseointegration and optimize healing.
Results: The dietary and hygienic guidelines provided in this paper emphasize the importance of maintaining proper oral hygiene and diet to support osseointegration and soft tissue healing during post-surgery healing periods.
Conclusions: The protocol presented has been an effective instrument to obtain and maintain osseointegration in patients rehabilitated with full-arch, immediate loading prostheses.
Keywords
Diet, Oral hygiene, Dental implants
Introduction
Two factors have been identified as the main causes for implant failure: occlusal overload and plaque accumulation [1]. Occlusal forces may be influenced by several factors, including diet [2]. Consequently implants should not be loaded with tough foods until at least the 12th week. Bone healing in weeks 6 through 12 yields wooven bone which is not completely mineralized. Then, woven bone is replaced by lamellar bone which is more mineralized and better able to withstand the forces of mastication.
The literature is lacking detailed dietary protocols for patients rehabilitated with full-arch, immediate loading rehabilitations; publications generally do not give specific information or the indications consist of general advice [3,4]. Optimal oral hygiene should be required of patients before and after any surgical intervention associated with implant therapy [5]. Patients must be instructed to perform high levels of home care and educated about the correlation between their active participation in treatment and long-term success.
Crestal bone levels are particularly sensitive to oral hygiene levels within the first 3 to 4 months after implant placement [5]. However, some patients find fixed, full-arch, implant-supported prosthesis particularly challenging to clean.
The need for a specific dietary program came from the recognition that patients might be susceptible to problems associated with poor wound healing and implant complications. The dietary protocol was developed in collaboration with the department of dietetics of the University of Genoa, organized according to the time that elapsed from the surgical appointment. In parallel, a hygienic protocol was developed.
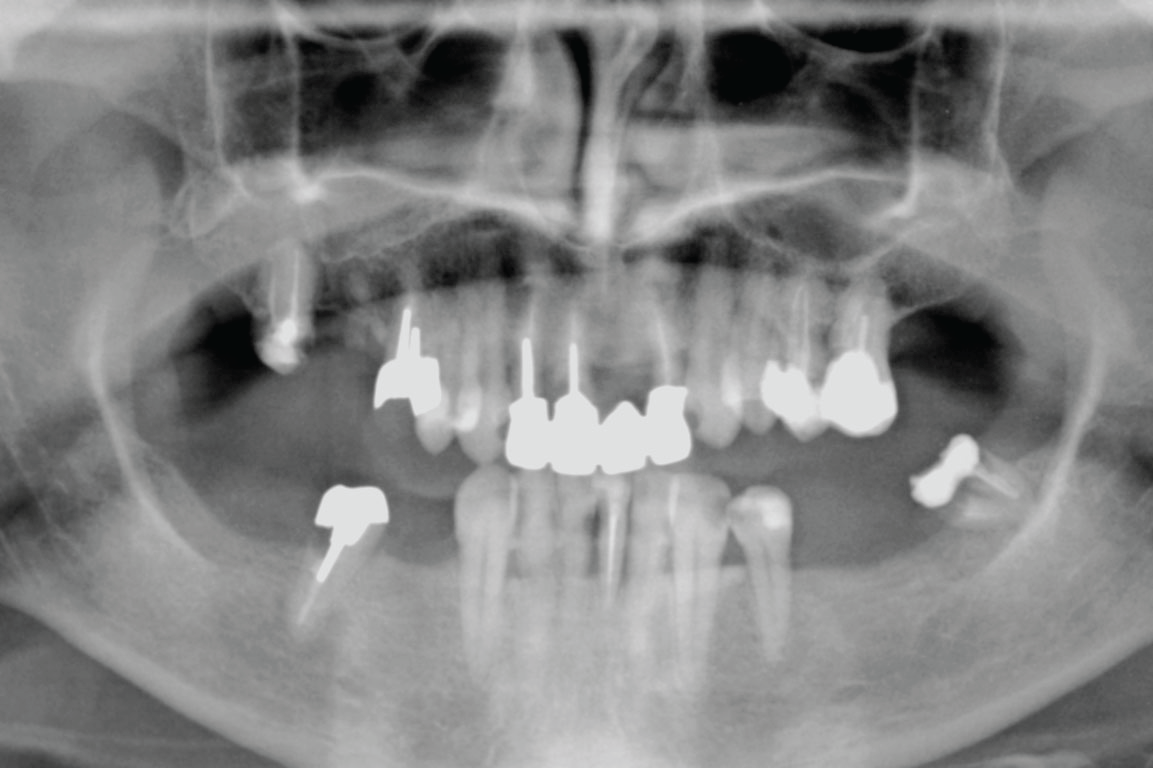
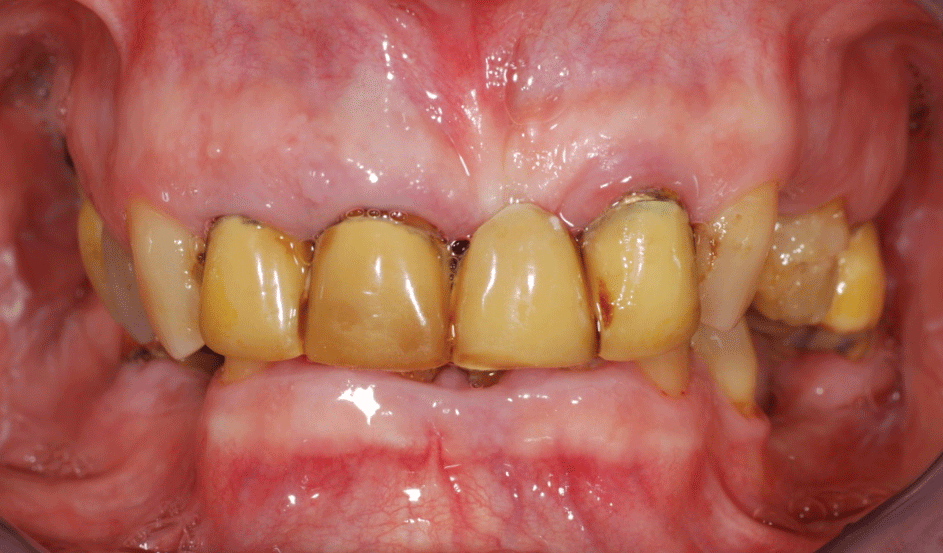
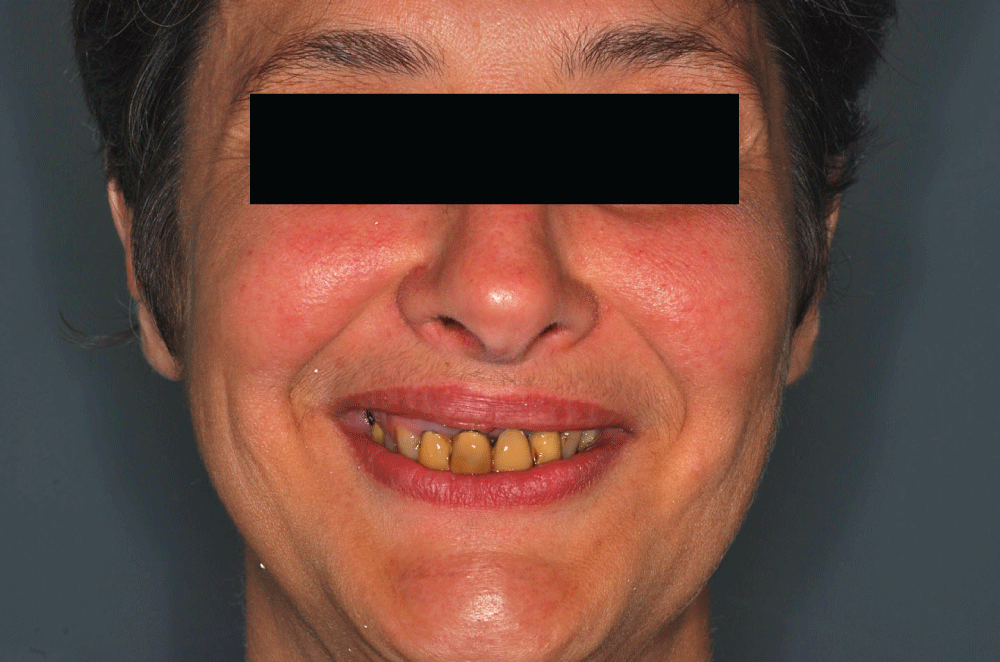
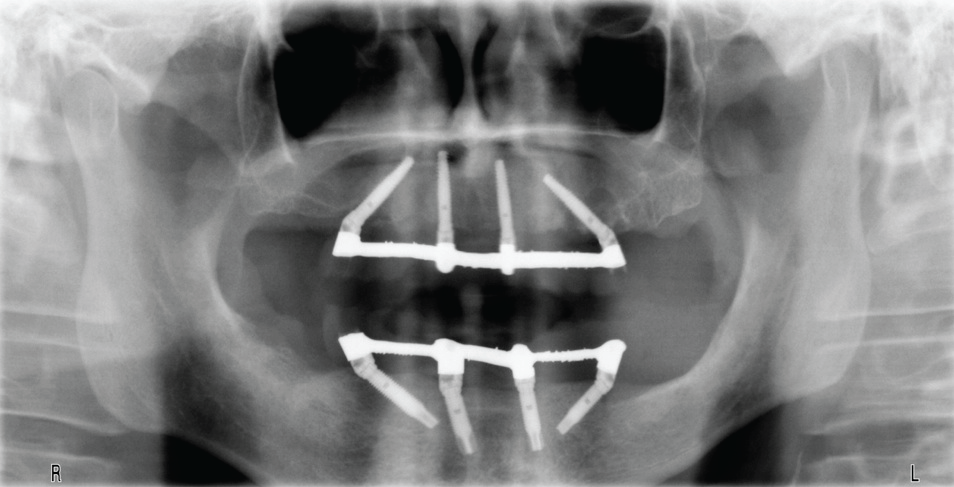
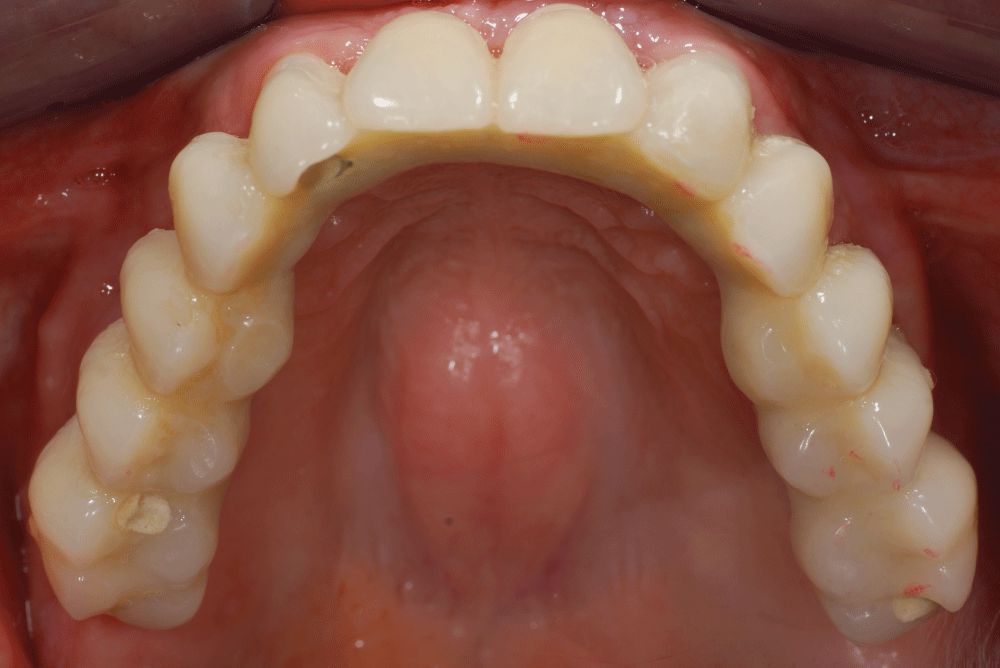
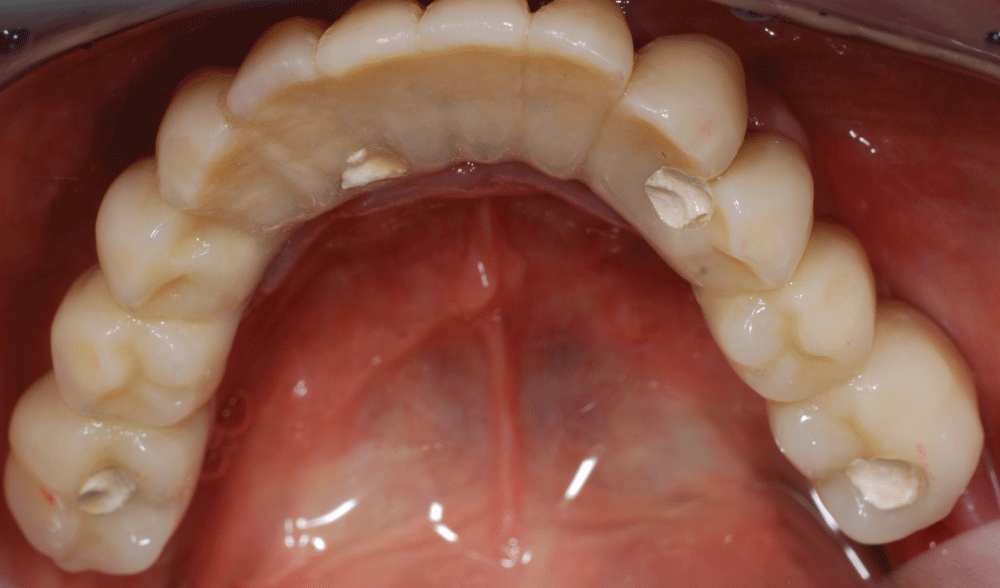
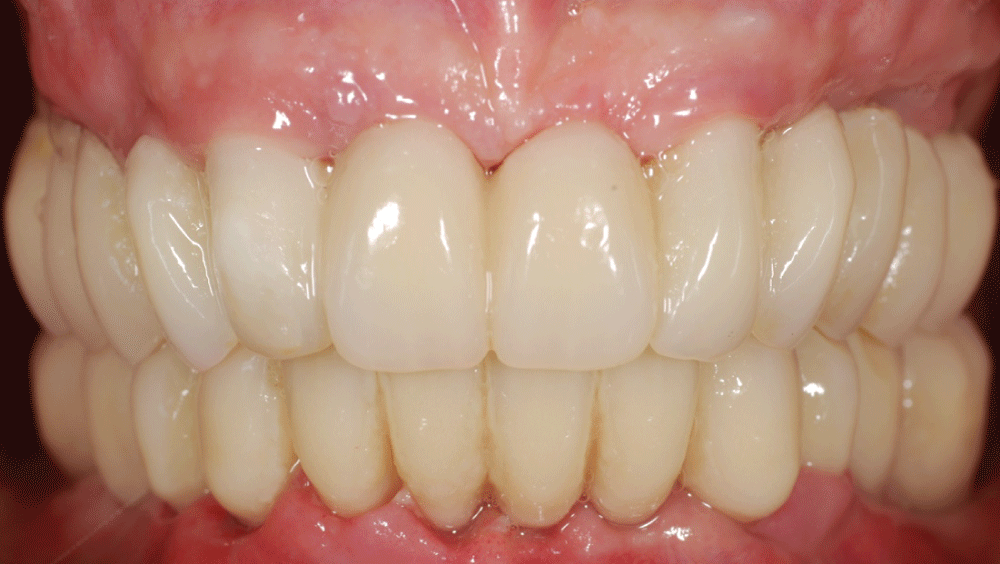
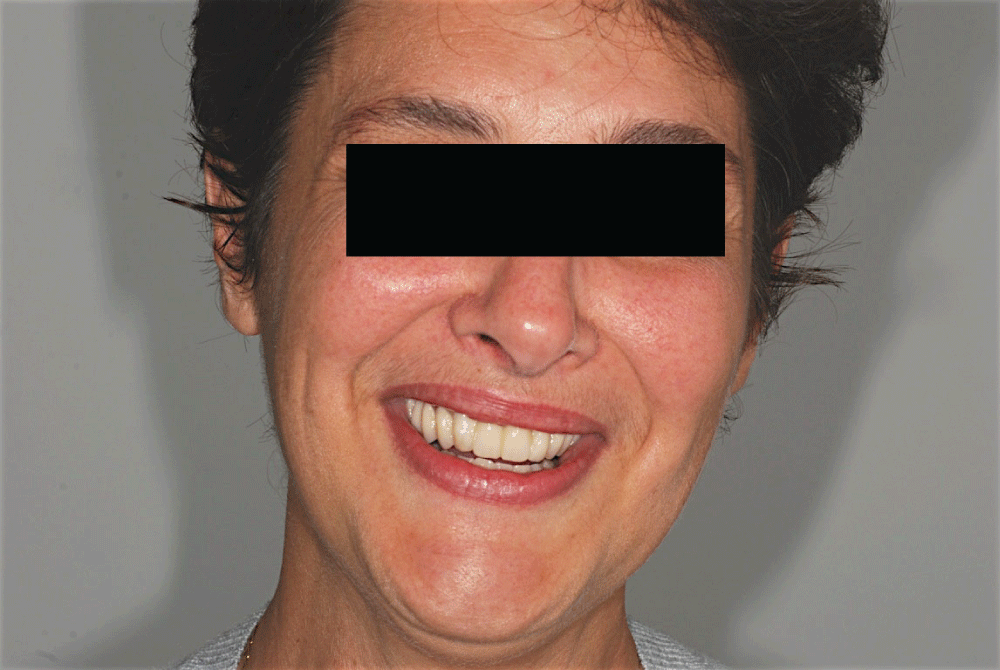
The instructions were developed for patients treated according to the Columbus Bridge Protocol [6,7] (CBP), a surgical and prosthodontic protocol for rehabilitation of atrophic, edentulous jaws using distal tilted implants (Figure 1, Figure 2, Figure 3, Figure 4, Figure 5, Figure 6, Figure 7 and Figure 8), but they may also be useful in similar rehabilitations.
Methods
Oral hygiene instructions - general requirements
Before surgery, a full-mouth scaling must be performed. It has been proven that microbial populations found on and around dental implants have been impacted by microbial populations in the mouth prior to implant surgery [5]. The hygiene techniques taught to patients vary according to their clinical situations, depending on the presence of teeth with periodontal disease and the presence of fixed or removable prostheses. Bacteria can be transferred from tooth surfaces to adjacent implant sites during extraction procedures so it is important for patients to understand that they must follow the requisite oral hygiene procedures even on teeth scheduled for extraction during implant placement to reduce the potential for intra-oral bacterial cross-contamination, increased inflammation and risk of infection during surgery.
After delivery of the prostheses (24 to 48 hours after surgery), patients are instructed on oral hygiene procedures, designed to be effective but not traumatic to the recently operated on tissues. At recall appointments, dental hygienists evaluate the condition of tissues, assess whether plaque control has been correctly performed, reinforces patients' motivation and makes dietary recommendations. The procedures are performed with teflon or plastic curettes, ultrasonic scalers with composite points, rubber cups and air polishing (e.g. bicarbonate or glycine powder). The use of metal instruments should be avoided because they can scratch the superficial titanium surfaces, making implants more vulnerable to increased plaque adhesion [8].
Dietary instructions - general requirements
Patients need to follow a balanced diet that includes all essential food groups, as illustrated in the Mediterranean diet pyramid [9]. Post-surgical diets must supply all elements that could affect tissue healing and osseointegration, such as proteins and vitamins (especially A, C, B2 and D) [10]. This diet also include mineral salts, calcium, phosphorus, and magnesium. The authors have found that the mean age for patients rehabilitated with full-arch immediate loading procedures is usually between 50 and 65 years old. However a wide range of age has been reported for patients rehabilitated with similar protocols [11,12].
Malnutrition and poor nutritional intake are more common in older patients [13], so depending on patient age, emphasis may also be needed for zinc, iron, Vitamin D and the full range of B vitamins. Provision of adequate fluids and fiber must be recommended especially in elderly patients.
After surgery, the following dietary contraindications must be respected:
• Hot food and drinks need to be avoided as they may cause bleeding and increased swelling
• Salty and spicy foods (e.g. curry, paprika, pepper) may irritate oral mucosa
• Alcoholic drinks may dehydrate oral mucosa due to astringent effects
• Acidic substances (e.g. grapefruit, lemon, orange, carbonated drinks) may cause hypersalivation and wound irritations
• Raw vegetables or hard food (e.g. raw fennel or celery, toasted bread): may injure already inflamed mucosa and require intense masticatory activity
• Sticky foods (e.g. soft spreadable cheeses, caramels, nut butters) may prove difficult to remove from the oral cavity and prosthesis surfaces
• Food containing seeds may penetrate wounds and become foreign bodies
For dietary instructions to be effective, they must be practical, easy to follow and respect patients' pre-existing dietary habits. The purpose of dietary instructions is to give patients choices in the foods that they may eat and to provide suggestions for optimal meal planning.
Dietary recommendations must be customized for every patient according to the rate of healing, which varies from patient to patient. Patients with systemic pathologies (e.g. diabetes, high cholesterol, food intolerance, and hypertension) are advised to follow their usual diets but to modify: (1) food temperature (cold food on the first post-operative day, room temperature food on the second one) and (2) food consistency, which can be homogenized, liquidized, mashed or chopped into fine pieces. Recommendations for modifications for lactose-free, fat, sodium or sugar modified diets must be provided when needed.
Dietary and hygienic protocol
Before surgery, patients are instructed about the protocols to be followed. At each recare appointment, clinicians need to assess patient compliance with the dietary and hygienic guidelines and reinforce motivation.
First post-operative day
Patients must not to do rinsing of any kind to decrease the potential for bleeding. They are also taught to apply 0.5% chlorhexidine periodontal gel two or three times a day to the implant sites and to perform routine oral hygiene procedures on teeth in the opposing jaw. In the CBP, to fabricate metal frameworks, immediate prostheses are not inserted until the first post-operative day. The chlorhexidine gel is applied topically next to the healing caps and adjacent peri-implant tissues at least once in the morning and once prior to nighttime sleep, after other oral hygiene procedures. Patients also may substitute chlorhexidine gel for toothpaste since they are advised not to use toothpaste in or around the natural teeth in the opposing jaw to avoid generating foam and consequently the necessity to rinse.
Food must be cold and liquid or semi-liquid (Table 1). A liquid diet includes fluids that may consist of particles not macroscopically visible that do not require chewing before swallowing (fruit juices, milk, liquid yogurt, drinks prepared with syrups and meat or vegetable broth). A semi-liquid diet includes food with particles visible macroscopically such as ice cream, sherbet, creamed vegetables, liquidized fruit, homogenized fruit and yogurt. Semi-liquids may require some oral preparation by patients; active chewing is not involved.
![]()
Table 1: Suspensions and emulsions.
View Table 1
Second postoperative day
Patients may begin gentle rinsing for 1 minute with mouthwash that contains 0.2% chlorhexidine twice daily to reduce oral bacteria counts. Further rinses with hypotonic saline solution may be performed after meals (a spoonful of table salt in 125 ml water). Patients are advised to apply 0.5% chlorhexidine periodontal gel to the implant sites every evening. Routine oral hygiene procedures should be carried out in the opposing jaw. On the second postoperative day, the diet must still be liquid or semi-liquid, but it can be eaten at room temperature.
In order to fabricate the metal frameworks in the CBP, the immediate prostheses are generally delivered on the second post-operative day.
From delivery of the fixed provisional prosthesis to suture removal
From the delivery of the fixed prosthesis (day 2) until sutures are removed (day 7 to 10), patients must be cautioned not to traumatize the surgical wounds. Oral hygiene is maintained with two gentle rinses a day with mouthwash containing 0.2% chlorhexidine, oral rinses with hypotonic saline solution after every meal and application of 0.5% chlorhexidine periodontal gel once daily before sleep.
The diet should be semi-solid, consisting of food needing more oral manipulation than semi-liquid food but not actual chewing. These foods are distinguished from semi-liquid foods by their ability to maintain for a short time the shape of the container they were stored in. Semi-solid foods include polenta, creamed cereal, dense mashed and liquidized foods, homogenized fish or meat, soft-boiled eggs, soft and creamy cheeses, puddings and cremes.
From suture removal to soft tissue healing
From the day sutures are removed (about day 7 to 10) until the peri-implant soft tissues have healed (about week 3), patients continue with gentle oral rinses; the percentage of chlorhexidine could be decreased from 0.2% to 0.12%. Patients must brush the prosthesis on the operated jaw with delicate rotating movements using a soft-bristle toothbrush and they may modify their diets to include solid-soft foods that require more elaborate oral manipulation but not actual mastication. It is advisable to supply special instructions regarding food preparation:
• Noodles: small in size; well-cooked so they are soft, slippery and easy to swallow;
• Meats with the visible fat removed, prepared in ground or minced form;
• Vegetables: cooked and mashed;
• Fruits: ripened, peeled, without seeds (better if skinned and mashed);
• Foods containing small seeds (e.g. strawberries and kiwis): should still be avoided; seeds may get wedged or stuck between fixed prostheses and soft tissues; they tend to be difficult to remove during home oral hygiene procedures;
• Biscuits: soluble are preferred.
Mashing is not necessary for all foods; most can be chopped well with a knife and fork so they still appeal to patients. It is also useful to give patients examples of balanced diets as a guide to meal planning (Table 2).
![]()
Table 2: Standard dietary protocol of approximately 2,000 calories needed for a healthy male patient of normal weight.
View Table 2
From soft tissue healing to osseointegration
After soft tissue healing (around week 3), patients may start using extra-fine interdental cleaners with plastic-coated, inner metal cores to avoid traumatizing peri-implant soft tissues and scratching titanium abutments or implant surfaces. They must also use spongy dental floss with rigid ends to remove plaque from the interfaces between the prostheses and peri-implant mucosa. Brushing may be performed with soft or medium-bristle toothbrushes. Patients may continue to use mouthwash but without chlorhexidine since long-term use can cause discoloration of the prostheses.
Three weeks after surgery, an interdental brush of smaller size may be used that fits between the prostheses and soft tissues. Later on, due to the formation of wider gaps between prostheses and mucosa after soft tissue healing during the first post-operative month, interdental brushes and interdental spongy floss of greater size can be used [14].
Patients progressively start eating solid foods that require prolonged oral manipulation and chewing, avoiding all foods that require significant mastication such as nuts, hard bread, rolls, ribs, raw celery, dried fruit, nougat and hard pastries. Excessive occlusal loads must be avoided during the first 2 months after implant placement.
Patients who need to be careful about their caloric intake may substitute low-calorie foods where appropriate for any of the accepted food choices during the post-operative phases. Table 3 describes food quantities with similar caloric values that may be helpful for developing balanced diets that provide appropriate caloric intake.
![]()
Table 3: The foods listed in each box have the same caloric value.
View Table 3
Bone healing/maturation phase
Around week 8 patients may perform routine oral hygiene procedures using medium-bristle toothbrushes, spongy interdental floss, sized interdental cleaners, and mouthwash without chlorhexidine. Useful devices might also be oral irrigators and special angulated toothbrushes designed to clean lingual surfaces of fixed implant-supported prostheses. Patients may now be encouraged to eat a normal diet.
Definitive prostheses
Approximately 4 months after surgery, definitive prostheses are inserted onto the abutments and implants. The prostheses are designed with convex shapes on the intaglio surfaces with no sharp line angles or concavities in order to minimize plaque accumulation, facilitating home care procedures. The size of interdental brushes usually has to be reduced to compensate for decreased spaces between the intaglio surfaces of the new prostheses and the soft tissues.
During recare appointments, planned according to patients' ability to maintain proper oral hygiene, the fixed prostheses generally have to be removed (at least once a year) to evaluate potential abutment screw loosening and for complete hygiene procedures.
Peri-implant soft tissue probing depths, bleeding on probing and plaque accumulation are recommended at each appointment to evaluate the status of peri-implant mucosa [14]. Radiographs should also be performed every 4 months in the first year after surgery and then once a year thereafter.
Table 4 illustrates hygiene follow-up appointments. Table 5 summarizes the hygienic and dietary guidelines designed for patients treated according to the CBP.
![]()
Table 4: Hygienic Follow-up.
View Table 4
![]()
Table 5: Summary of the hygienic and dietetic recommendations for the Columbus Bridge Protocol. Chlorhexidine (clx).
View Table 5
A prospective study [6] demonstrated that patients treated with the CBP, including the hygienic and dietetic protocols described above, at 6-year follow-up visits have showed optimal implant survival rate (93.9%), prosthodontic survival rate (100%) and interproximal crestal bone resorption (mean: 1.62 ± 1.23 mm). The results compare favorably with those of patients treated with traditional delayed loading protocols.
Conclusions
This protocol needs to be validated with prospective clinical trials but in the authors' experience it was beneficial for patients rehabilitated with full-arch immediate loading prostheses. Scheduled follow-up visits must be provided to ensure optimal cooperation among dentists, hygienists and assistants, supported by dieticians, whose skills can improve the prognosis for clinical success.
References
-
Menini M, Signori A, Tealdo T, Bevilacqua M, Pera F, et al. (2012) Tilted implants in the immediate loading rehabilitation of the maxilla: a systematic review. J Dent Res 91: 821-827.
-
Del Fabbro M, Testori T, Francetti L, Taschieri S, Weinstein R (2006) Systematic review of survival rates for immediately loaded dental implants. Int J Periodontics Restorative Dent 26: 249-263.
-
Pesce P, Menini M, Tealdo T, Bevilacqua M, Pera F, et al. (2014) Peri-implantitis: a systematic review of recently published papers. Int J Prosthodont 27: 15-25.
-
Misch CE, Wang HL, Misch CM, Sharawy M, Lemons J, et al. (2004) Rationale for the application of immediate load in implant dentistry. Implant Dent 13: 207-217.
-
Balshi SF, Wolfinger GJ, Balshi TJ (2005) A prospective study of immediate functional loading, following the Teeth in a Day protocol: a case series of 55 consecutive edentulous maxillas. Clin Implant Dent Relat Res 7: 24-31.
-
Malo P, Nobre Mde A, Petersson U, Wigren S (2006) A pilot study of complete edentulous rehabilitation with immediate function using a new implant design: case series. Clin Implant Dent Relat Res 8: 223-232.
-
Mombelli A, Marxer M, Gaberthuel T, Grunder U, Lang NP (1995) The microbiota of osseointegrated implants in patients with a history of periodontal disease. J Clin Periodontol 22: 124-130.
-
Tealdo T, Menini M, Bevilacqua M, Pera F, Pesce P, et al. (2014) Immediate versus delayed loading of dental implants in edentulous patients' maxillae: a 6-year prospective study. Int J Prosthodont 27: 207-214.
-
Tealdo T, Bevilacqua M, Pera P (2012) Columbus Bridge Protocol. Immediate loading bridge. Second Edition. Rho (MI): Quintessenza.
-
Traini T, Assenza B, San Roman F, Thams U, Caputi S, et al. (2006) Bone microvascular pattern around loaded dental implants in a canine model. Clin Oral Investig 10: 151-156.
-
Corbella S, Del Fabbro M, Taschieri S, De Siena F, Francetti L (2011) Clinical evaluation of an implant maintenance protocol for the prevention of peri-implant diseases in patients treated with immediately loaded full-arch rehabilitations. Int J Dent Hyg 9: 216-222.
-
Bach-Faig A, Berry EM, Lairon D, Reguant J, Trichopoulou A, et al. (2011) Mediterranean diet pyramid today. Science and cultural updates. Public Health Nutr 14: 2274-2284.
-
Nix S (2013) Surgery and Nutrition support. In: Williams' Basic Nutrition & Diet Therapy. 14th (edn). St Louis: Elsevier, 447-466.
-
Mudge AM, Ross LJ, Young AM, Isenring EA, Banks MD (2011) Helping understand nutritional gaps in the elderly (HUNGER): A prospective study of patient factors associated with inadequate nutritional intake in older medical inpatients. Clin Nutr 30: 320-325.
-
Bourne M (2002) Texture, viscosity and food. In: Elsevier (ed) Food texture and viscosity: concept and measurement. (2nd edn). Academic Press, London, 1-32.
-
Swanson RB, McKemie RJ, Sabrin MD, Milly P J (2012) Soy Milks as a Dairy Milk Substitute in Prepared Food Products: Effects on Quality and Acceptability. Fam Consum Sci Res J 40: 255-266.