International Journal of Respiratory and Pulmonary Medicine
Discharge Care Bundle for Patients with Acute Exacerbations of COPD: Benefit more likely to be seen beyond 30 Days
Shorofsky M, Lebel M, Sedeno M, Zhi Li P and Bourbeau J*
Respiratory Epidemiology and Clinical Research Unit, Montreal Chest Institute, McGill University, Canada
*Corresponding author: Jean Bourbeau, M.D, Respiratory Epidemiology and Clinical Research Unit, Center for Innovative Medicine (CIM), McGill University Health Centre (MUHC)1001 Decarie Blvd. Room C047371.5, Montreal (QC), Canada, Tel: 514 9341934 ext 32185 Fax: 514 8432083, E-mail: jean.bourbeau@mcgill.ca
Int J Respir Pulm Med, IJRPM-2-024, (Volume 2, Issue 3), Original Article; ISSN: 2378-3516
Received: June 29, 2015 | Accepted: July 29, 2015 | Published: August 03, 2015
Citation: Shorofsky M, Lebel M, Sedeno M, Zhi Li P, Bourbeau J (2015) Discharge Care Bundle for Patients with Acute Exacerbations of COPD: Benefit more likely to be seen beyond 30 Days. Int J Respir Pulm Med 2:024. 10.23937/2378-3516/1410024
Copyright: © 2015 Shorofsky M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: COPD is associated with significant morbidity, mortality, and hospital costs. The implementation of COPD "discharge care bundles" has been proposed as having an impact on readmissions. We developed and implemented a discharge care bundle and the aim of this study was to evaluate its effects on utilization of hospital services in a real life setting.
Methods: We conducted a retrospective chart review study from 2007-2013 to evaluate utilization of hospital services over three time periods (30, 90 days, and one year) post discharge care bundle implementation in two patient cohorts. The first cohort included patients who had utilized any hospital service in the previous year for respiratory complaints and the second included only those who had been admitted. These cohorts were analyzed to evaluate differences in readmissions pre and post discharge care bundle implementation.
Results: In the first cohort (210 patients), the 90-day hospital service utilisation rate after implementation was 23.3% versus 35.7% for one hospital service (p=0.049) and at one year it was 22.4% versus 50.0% (p<0.001). In the second cohort (118 patients), the 90 days readmission rate after implementation was 18.6% versus 32.2% for one readmission (p=0.017) and at one year it was 30.5% versus 61.9% (p=0.038). At one year the readmission rate for two readmissions was 14.4% versus 24.6% (p=0.049).
Conclusion: The implementation of a COPD discharge care bundle successfully decreases hospital health service utilization and hospital readmissions, with the benefit more likely to be seen on a longer period of follow up beyond 30 days.
Introduction
In Canada, COPD accounts for the greatest number of hospital admissions among all major chronic illnesses [1] and it is the only chronic disease in which mortality is still increasing [2,3]. The average hospitalization for an acute exacerbation of COPD lasts 10 days with an average cost of $10,000 per stay [4] and there are high readmissions rates after hospital discharge with 18% of patients readmitted once within one year and 16% readmitted twice [1]. Similarly, in the United States, 30-day readmission rates were 7.1% for the principal diagnosis of COPD and 17.3% for any diagnosis of COPD [5]. It is imperative that COPD exacerbations are not only managed as an acute episode, but prior to hospital discharge steps are taken to fulfill care gaps that would assist in improving quality outcomes.
The development and implementation of COPD "discharge care bundles" has been suggested as a practice that could bridge these care gaps and potentially have a positive impact on hospital readmissions and related morbidity and mortality [6-8]. To date however, there have been only a few studies on discharge care bundles for COPD. The typical components common to these discharge care bundles include a medicine reconciliation, review of inhaler technique prior to discharge, referral to health care services after discharge, and smoking cessation counselling. These preliminary studies have shown that the implementation of a discharge care bundle may have the potential to decrease 30-day hospital readmissions [6,7]. However, readmission rates after 30 days, individual components of the care bundle, and whether the discharge care bundle benefits all COPD patients are not known [6,7].
Since 2007, the McGill University Health Centre (MUHC), an academic institution, has undertaken an organizational knowledge transfer initiative, the RECAP project (Rehabilitation, Education for COPD, and Added-value to the medical Practice), to document and overcome care gaps. To help fix these care gaps, a discharge care bundle tool was developed, implemented and data were collected as part of regular practice. We performed a chart review study to evaluate the implementation of this Discharge Care Bundle over a six-year time period to determine if there was a decrease in hospital readmission and emergency department visit rates over a short period, e.g., 30 days, a long period, e.g., 90 days, and one year post hospital discharge. We also evaluated whether the benefits of the discharge care bundle were indistinguishable to all COPD patients and if its benefits were related to specific components rather than the entirety of care.
Methods
Designing the COPD Discharge Care Bundle
Mapping the patient pathway: Before designing the discharge care bundle, we undertook a process that included mapping the patient pathway from admission to discharge. This was done based on a retrospective chart review over 3 years, which allowed us to identify care gaps and to develop a discharge care bundle according to the needs.
Meeting and engaging the medical staff: In November 2006, we carried out a number of teaching sessions where the results of the care gaps were presented. As well, we organized focus groups to discuss barriers and find out some possible solutions. Barriers mentioned included high turnover of residents and nursing staff, and lack of standardization in the medical practice for the patient discharge from the hospital. The solution included the development and use of standardized tools to plan the discharge of COPD patients and ensure quality improvement.
Discharge care bundle development:
The COPD care bundle (See in the Supplement) includes the following steps to be taken during the admission and before patient discharge:
1. Establishing COPD diagnosis with spirometry.
2. Evaluating smoking status and intervention as needed.
3. Evaluating patient's integration of education self-management strategies.
4. Referring to the community services for COPD and medical follow-up.
5. Referring to pulmonary rehabilitation.
6. Prescribing maintenance respiratory medication as per the National guidelines although there was no protocol requirement.
Implementation of the discharge care bundle: The discharge care bundle was implemented on the medical ward of the Montreal Chest Institute (MCI) at the MUHC. It was completed for patients with the admitting diagnosis of COPD, COPD/pneumonia, or COPD/Congestive Heart Failure.
Inclusion criteria: In this article we are presenting an analysis from 6 years of data (May 2007 until March 2013) following the implementation of the discharge care bundle.
We only included patients that had at least one hospital visit for a respiratory complaint to any of the MUHC hospital sites in the previous year, as documented in the electronic database OACIS.
To properly evaluate the impact on reference to community services post-admission, we only included patients who were discharged to home (e.g. we excluded patients who were transferred to another hospital or a Long Term Care facility).
Data collection post implementation
All patients admitted to the MCI from 2007 to 2013 with the appropriate diagnosis were included for final analysis. This project was approved by the Research Ethic Board of McGill University Health Centre (12-418-BMA). Information on patient and disease characteristics collected from the discharge care bundle was extracted from a dedicated RECAP database with supplementary information extracted from OACIS, an electronic database that tracks admissions, clinic visits, diagnoses, laboratory and imaging results, and baseline patient characteristics.
Patients were broken down into two cohorts. The first and largest cohort (Hospital Utilization Cohort) included COPD patients who had at least one: 1) unscheduled Emergency Room (ER) visit, 2) day hospital admission or 3) medical ward admission the previous year for respiratory complaints. The second cohort (Ward Cohort), a subset of the largest cohort, included only those who were actually admitted to the medical ward or Day Hospital in the previous year. In the Hospital Utilization Cohort, the readmission rates to the ward, ER, or Day Hospital at 30 days, 90 days, and one-year post discharge care bundle implementation were analyzed to determine total usage of hospital services. In the Ward Cohort, the readmission rates to the ward and day hospital at 30 days, 90 days, and one-year post discharge care bundle implementation were analyzed to determine rates of readmission to medical wards only. For final analysis a Day Hospitalization was considered a ward admission because these patients would not have been sent home and likely have been admitted to the medical ward if the Day Hospital was not available. No results for zero readmissions at any timeframe were included in the final analysis, as the pre/post study design required at least one readmission in the previous year. Therefore by one year follow up there would have been no patients with zero admissions in the previous year.
Statistical analysis
Descriptive data are reported as mean (SD) or n (%) or median (Q1-Q3), as appropriate. For each cohort, McNemar's test (or binomial exact test if any discordant cell frequency is less than 4) was used to test the difference of readmission proportion categorized to patients with 1 and/or 2, and more than 3 readmissions, between the two periods 30-days post and 30-days pre-RECAP; the analysis was repeated for the corresponding 90-day and 1-year periods. The readmission frequency was summarized as a per-person per-year, and Poisson regression model was used to test the frequency difference. Statistical significance was determined with two-sided tests and p<0 .05. In the secondary analysis, a univariate and multivariate Poisson regression model with a robust error variance was fitted to the data to estimate the effect on readmissions of the individual components of the COPD discharge care bundle. Using the total number of admissions before and after discharge during 30-days, 90-days, and 1-year as the outcome measures, some selected individual components on discharge care bundle were put in the model as the predictors to estimate risk of readmissions, and crude and mutual adjusted Relative Risks were calculated for each component. All statistical analyses were performed using SAS version 9.3 (SAS Institute Inc., Cary, NC).
Results
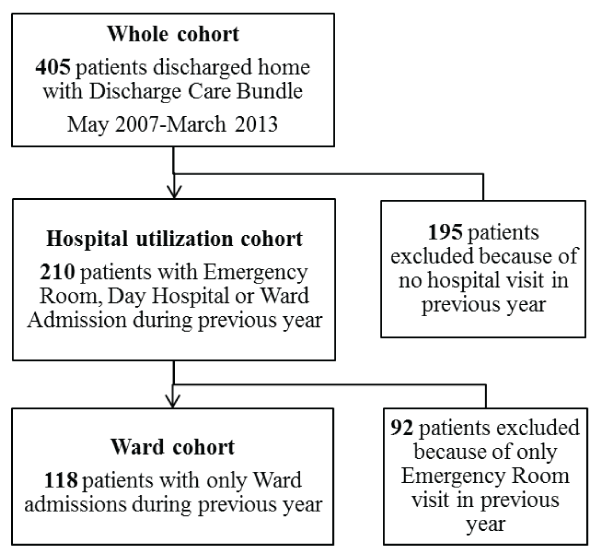
During the study period 405 patients were admitted with COPD, COPD/Pneumonia, or COPD/CHF using the COPD discharge care bundle. Of these 405 patients, 210 had at least one unplanned visit to the ER or had been admitted to the Day Hospital or to the Medical Ward and were included for final analysis (Hospital Utilization Cohort). From this cohort there were 118 patients that were admitted to the Medical Ward (Ward Cohort) (Figure 1).
The median age of the entire population was 71.4 years with equally distributed males and females. The median length of hospital admission was 6.0 days. COPD was listed as the only admission diagnosis for 68.6%, COPD/Pneumonia for 28.1.7% and COPD/CHF for 3.1%. The patient characteristics for the 2 cohorts were similar to the entire population data. Complete baseline characteristics are presented in table 1. The overall 30-day ward readmission rate for the entire study population was 14.6%.
![]()
Table 1: Baseline characteristics of the Whole Cohort, the Hospital Utilization Cohort, and the Ward Cohort.
View Table 1
Table 2 shows hospital service utilization at 30, 90 days, and one year for both cohorts. In the Hospital Utilization Cohort there was no difference in hospital service utilization post discharge care bundle implementation for patients using one service at 30 days and there was a significant increase in hospital utilization for those using two services at 30 days. At 90 days and one year, there was a significant decrease in hospital service utilization for patients using one service but no significant difference for those using two or more services. In the Ward Cohort there was no significant difference in readmissions at 30 days after discharge. At 90 days there was a significant decrease in readmissions post discharge care bundle implementation for patients with one readmission and there was a significant increase in readmissions for patients with two readmissions. At one year there was a significant decrease in readmissions for patients with one or two readmissions and a trend towards an increase in readmissions for patients with 3 or more readmissions. The admission frequency per patient per year showed no significant difference before and after discharge care bundle implementation in either the Hospital Utilization or Ward cohorts.
![]()
Table 2: Admission characteristics before and post-discharge for the Hospital Utilization and the Ward cohort.
View Table 2
Table 3 shows the effect on readmission of the individual components of the care bundle. On univariate analysis no components of the discharge care bundle reached significance in either the Hospital Utilization or Ward cohorts. On multivariate analysis for the Hospital Utilization cohort no components were significant, however there was a trend towards decreased readmissions at 30 and 90 days for patients who were able to identify their baseline respiratory condition, identify signs of deterioration, and have good cough technique. There was also a trend towards decreased readmissions at 30 days, 90 days, and one year for patients referred to Pulmonary Rehabilitation in the Hospital Utilization Cohort. On multivariate analysis for the Ward Cohorts there was a significant decrease in readmissions at 30 days, 90 days, and one year for patients who were able to identify their baseline respiratory condition, identify signs of deterioration, and have good cough technique. There was a significant decrease in readmissions at one year for patients who knew the resources available in case of exacerbation along with a trend towards decreased readmissions at 30 days and 90 days. There was also a significant decrease in readmissions at 30 days in the ward cohorts for patients referred to Pulmonary Rehabilitation, with a trend towards a decrease at 90 days and one year.
![]()
Table 3: The effect on readmissions of the individual components of the COPD discharge care bundle*.
View Table 3
Discussion
Our study is of special interest because it evaluated the use of a COPD discharge care bundle over the course of an extended timeframe in a real life setting. The study encompasses hundreds of patients over the course of a six year implementation time period while previous studies only had data on more a limited number of patients as the discharge planning tool was implemented over a much shorter time frame. We showed that the implementation of a COPD discharge care bundle reduces total hospital utilization and more specifically medical ward readmissions up to one year post discharge care bundle implementation in the "light users", which are those only requiring one readmission. However, this benefit was seen after a longer timeframe (90-days and 1 year) and not during the short term (30-days). Furthermore, it was not possible to demonstrate a benefit from a discharge care bundle in the "heavy users" (those with 3 or more admissions).
The problem of readmissions in patients with COPD is a major one, and it is often related to the variations in provision of care on patient discharge, implying that there would be a role for a systematic quality improvement approach [9,10]. There is a need for a consistent response from hospital medical staff to develop a standardized culture of care in which COPD patients' needs are met as part of routine practice. A study by Hopkinson et al. [6] was piloted on designing and implementing a COPD discharge care bundle on a respiratory ward. The 30-day readmission rate was 10.8% for patients where the bundle was used compared with 16.4% where it was not (95% CI for difference 2.1% to 13.2%). After implementation of the bundle, there was a downward trend in readmissions but this not found to be statistically significant.
The results of our study differ considering that the discharge care bundle had no effect on 30-day readmission rates. In our study population, the 30-day readmission rate of 14.6% was already low before the implementation of the discharge care bundle. One other difference could have been that in Hopkinson, there was the addition of a brief phone call 48 to 72 hours post-discharge to check whether patients were improving. We didn't have this component as part of the discharge care bundle. This could be an important component, in particular to prevent short-term readmissions.
However more recently Jennings et al. published a single-center, randomized clinical trial, assessing a pre-discharge care bundle in admitted patients with acute exacerbations of COPD [11]. Out of 172 patients enrolled in the trial there was no difference in 30 and 90-day readmission rates and therefore the trial was stopped early after interim analysis. One significant difference was that the discharge bundle designed by Jennings et al. did not include referral to a pulmonary rehabilitation program, which our study demonstrated to be a likely important component in COPD care, which is now reflected in current COPD care guidelines.
One important contribution of our study was to demonstrate potential benefit beyond the short term, i.e., at 90 days and one-year post discharge care bundle implementation. We demonstrated that the discharge care bundle is beneficial in reducing readmissions; however the effects become more apparent over time. This could be explained by the fact that many components of the discharge bundle have a delayed effect, such as follow up with a respirologist, smoking cessation, and pulmonary rehabilitation, or the patient may also require time in acquiring adapted behaviour. By 90 days we had a significant decrease in hospital readmissions for the "lightest users" (those only requiring one readmission) and by one year we had a significant decrease in readmissions for those requiring two readmissions.
However, the discharge care bundle did not have an effect on the "heaviest users" which were those requiring three or more readmissions, and therefore we may not be able to claim generalizability. Our results suggest that the discharge care bundle is a good first step for COPD care, but patients with severe COPD and multiple readmissions may require a more in depth healthcare plan, more resources may be needed and services tailored to specific needs of the patients to generate a measurable effect on readmission rates.
Another important strength of our study is the analysis of the individual components of the discharge care bundle. Self-management components appear to be the most important, such as being able to identify baseline symptoms, signs of deterioration, and have implemented self-management skills including cough and breathing techniques. Other components in the hospital cohort such as referral to pulmonary rehabilitation and being aware of resources in case of an exacerbation reached significance at only one time period, but trended towards significance at all time frames. These interventions should not be underestimated as they may require more time to become effective within the continuum of care.
There were a number of limitations to our study. First, by design, our study was a single center, retrospective, chart review study with a pre/post design with patients acting as their own controls. COPD is a non-reversible progressive disease and overtime patients are likely to require more hospital services such as ER visits and ward admissions [12,13]. Also, we are unable to account for readmissions if patients present to hospitals outside of the MUHC system. However, as a retrospective study design, this discharge care bundle was implemented in a large scale, real life environment outside of a pre-determined study over the course of an extended timeframe. The pre-post design makes it difficult to correct from other changes in COPD care over the same time period and not related to the discharge care bundle. Most saliently, the beginning of the study period coincides with publication of the TORCH study, the timing of which has been shown in Quebec to coincide with a major change in COPD prescribing patterns (shift to increased ICS/LABA combination therapy). Despite the limitations of this type of study design, this study has allowed us to evaluate the effect of a discharge planning tool in a real life medical setting and therefore might be closer to the reality if implemented in other centers.
Patients included in the analysis had to have an admission in the previous year. Due to this requirement, we were unable to evaluate patients that had the discharge care bundle implemented on their first known presentation to our hospital. Therefore, all patients in our final study population were "sicker" than the COPD population as a whole. Since the discharge care bundle was successfully implemented in a speciality hospital with dedicated respiratory healthcare professionals, it is unclear how efficiently a discharge care bundle could be implemented and its effects on patients in a general medicine wards. On the other hand, patients from a general medicine ward may have been less sick and/or less likely to have previously been exposed to previous forms of self-management interventions and have had less communication with a specialized respiratory nurse. Therefore, our setting in a specialized respiratory hospital may have resulted in an underestimation of the effectiveness of a COPD discharge care bundle.
Reducing hospital readmissions has a significant impact in the current healthcare systems in both the United States and Canada, where both the public and private sectors are attempting to slow down the rapid rise in healthcare costs. A recent single center study in Canada showed that the addition of a COPD nurse navigator was able to significantly reduce total hospital admissions for COPD, decrease total hospital admission days for COPD, along with saving the hospital over $260,000 annually [12]. The implementation of COPD discharging planning tools, which utilizes specialized respiratory nurses, has the potential to have the same cost saving effects, even though this was not specifically analyzed in our study.
Conclusions
Our study demonstrated that the implementation of a COPD discharge care bundle in a real life environment has the potential to decrease hospital health services utilization and hospital readmissions more likely to be seen over a longer period of follow up, i.e., at 90 days and 1 year. However, this may not be sufficient in the "heaviest users", e.g., patients with multiple hospital admissions. These findings suggest that, for a subset of patients, more resources and/or further adjustments in care would likely be required. This can only happen in an integrated system well adapted and centered on patients' biopsychosocial needs.
Acknowledgments
This study was funded by an unrestricted grant from GlaxoSmithKline, Boehringer Ingelheim and Bristol-Meyers Squibb.
The authors would like to thank the nurses and the physicians working on the medical ward of the Montreal Chest Institute of the McGill University Health Centre, the COPD nurses from the COPD clinic in developing the Discharge Care Bundle and Louise Auclair for the secretarial support.
Matthew Shorofsky assisted in the development of the proposal, made the chart review and data extraction, assisted in the analysis and wrote/reviewed the manuscript.
Michel Lebel and Maria Sedeno assisted in the development of the study proposal, the implementation of the study and reviewed the manuscript.
Pei Zhi Li developed the analysis plan, performed the analysis and reviewed the manuscript.
Jean Bourbeau developed the study proposal, supervised the implementation and the analysis of the results, and wrote/reviewed the manuscript.
Role of the sponsors
The sponsors were not involved in the development of the research proposal, the implementation, the analysis and the writing or reviewing of the manuscript.
References
-
(2008) Canadian Institute of Health Information. Health Indicators (Ottawa: CIHI, 2008).
-
Celli BR (2006) Predicting mortality in chronic obstructive pulmonary disease: chasing the "Holy Grail". Am J Respir Crit Care Med 173: 1298-1299.
-
Mannino DM (2005) Epidemiology and global impact of chronic obstructive pulmonary disease. Semin Respir Crit Care Med 26: 204-210.
-
Mittmann N, Kuramoto L, Seung SJ, Haddon JM, Bradley-Kennedy C, et al. (2008) The cost of moderate and severe COPD exacerbations to the Canadian healthcare system. Respir Med 102: 413-421.
-
Elixhauser A, Au DH, Podulka J (2011) Readmissions for Chronic Obstructive Pulmonary Disease, 2008: Statistical Brief #121.
-
Hopkinson NS, Englebretsen C, Cooley N, Kennie K, Lim M, et al. (2012) Designing and implementing a COPD discharge care bundle. Thorax 67: 90-92.
-
Matthews H, Tooley C, Nicholls C, Lindsey-Halls A (2013) Care bundles reduce readmissions for COPD. Nurs Times 109: 18-20.
-
Robb E, Jarman B, Suntharalingam G, Higgens C, Tennant R, et al. (2010) Using care bundles to reduce in-hospital mortality: quantitative survey. BMJ 340: c1234.
-
Buckingham RJL, Lowe W, Pursey NA, Roberts CM, Stone RA (2008) Report of the national chronic obstructive pulmonary disease audit 2008: resources and organisation of care in acute NHS units across the UK.
-
Scullion JE, Singh SJ, Morgan MDL (2010) BLF and BTS "Ready for home" Survey of the experiences of patients admitted to hospital with COPD. PT2: The discharge process 175.
-
Jennings JH, Thavarajah K, Mendez MP, Eichenhorn M, Kvale P, et al. (2015) Predischarge bundle for patients with acute exacerbations of COPD to reduce readmissions and ED visits: a randomized controlled trial. Chest 147: 1227-1234.
-
Dajczman E, Robitaille C, Ernst P, Hirsch AM, Wolkove N, et al. (2013) Integrated interdisciplinary care for patients with chronic obstructive pulmonary disease reduces emergency department visits, admissions and costs: a quality assurance study. Can Respir J 20: 351-356.
-
Bourbeau J, Saad N, Joubert A, Ouellet I, Drouin I, et al. (2013) Making collaborative self-management successful in COPD patients with high disease burden. Respir Med 107: 1061-1065.