International Journal of Respiratory and Pulmonary Medicine
Pulmonary Capillary Wedge Pressure Measurement: A Challenge for Diagnosis of Pulmonary Arterial Hypertension
F. Zoreka1,4,5, H. Bouvaist1,4*, E. Vautrin1,4, S. Marlière1,4, R. Guerbaai1,4 , J. Labarere2,5, G. Vanzetto1,4,5 and C. Pison3-5
1University Clinic of Cardiology, France
2Medical Evaluation Unit, France
3University Clinic of Pneumology France
4Pole Thorax and Vascular Centre Hospitalier Universitaire de Grenoble, France
5Universite Grenoble Alpes, France, ALBaath University, Syria
*Corresponding author: Dr Hélène Bouvaist, Clinique Universitaire de Cardiologie, Pole Thorax et Vaisseaux, Centre Hospitalier Universitaire de Grenoble, France, E-mail: hbouvaist@chu-grenoble.fr
Int J Respir Pulm Med, IJRPM-2-010, (Volume 2, Issue 1), Research Article; ISSN: 2378-3516
Received: November 29, 2014 | Accepted: January 08, 2015 | Published: January 11, 2015
Citation: Zoreka F, Bouvaist H, Vautrin E, Marlière S, Guerbaai R, et al., (2015) Pulmonary Capillary Wedge Pressure Measurement: A Challenge for Diagnosis of Pulmonary Arterial Hypertension. Int J Respir Pulm Med 2:010. 10.23937/2378-3516/1410010
Copyright: ©2015 Zoreka F, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: International registries report an aging population suffering from PAH (Pulmonary Artery Hypertension) engendering diagnosis difficulties linked with growing cases of group 2 related to left heart failure with preserved Ejection Fraction (PH-HFpE). Pulmonary Capillary Wedge Pressure (PCWP) measurement by right heart catheterization remains a technical challenge for patient classification; many centers still use digital PCWP given by cath lab software. Here, we have tried to demonstrate misclassification impact of this approximation.
Methods: We investigated the PCWP-Left Ventricular End Diastolic Pressure (LVEDP) relationship in a prospective series of 31 patients undergoing heart catherization for suspicion of PAH. Digital and end expiration PCWP were measured in right and left pulmonary arteries for comparison with end expiration LVEDP.
Results: We explored 31 patients, 65.4 � 11 years old, 67.7% were female, with LVEF 60.6 � 5.2%, Diagnosis of HFpEF was found in 62% of cases and PAH in 10% when using end expiration LVEDP. Right end expiration PCWP, left end expiration PCWP, right digital PCWP, left digital PCWP and end expiration LVEDP were respectively 16.2 � 6.7 mmHg, 16,6 � 6.4 mmHg, 12.2 � 6.1mmHg (p< 0.001), 12.7 � 6.1mmHg, and 15.8 +/- 4.8mmHg, with a significant difference (p< 0.001) between the right and left digital PCWP and end expiration LVEDP.
Conclusion: Using digital PCWP instead of end expiration PCWP measurement during RHC, results in a significant underestimation of the LVEDP, this translated to 22% of patients with Pulmonary Hypertension (PH) being misclassified as having group1 rather than group2 PH. Misclassified patients are at risk of receiving inadequate therapy and biased therapeutic studies. When in doubt left heart catheterization should be performed for PAH diagnosis.
Introduction
Since 2000, international registries show that the profile of patients with pulmonary arterial hypertension (PAH) has evolved [1-5]. PAH explored patients are older and present much comorbidity such as obesity, hypertension and coronary artery disease. Differential diagnosis with heart failure and preserved ejection fraction (HFpEF) is the current challenge in this population [6]. Indeed cardiac echocardiography can eliminate systolic left ventricular dysfunction and valvular heart disease, but is often faulted for identifying diastolic left ventricular dysfunction and for evaluating pulmonary vascular resistances. Therefore, there is a need for right heart catheterization (RHC) in the diagnosis of PAH along with the measurement of pulmonary capillary wedge pressure (PCWP), which is essential for Pulmonary Hypertension (PH) classification [7]. PAH is defined by a mean pulmonary arterial pressure (mPAP) equal or higher than 25 mmHg and PCWP lower or equal to 15 mmHg [5]. Nevertheless, a left ventricular end diastolic pressure (LVEDP) equal or below 15 mmHg remains the gold standard to differentiate pre- and post- capillary pulmonary hypertension. Strong correlations between PCWP and LVEDP have been reported in many studies [8,9] allowing the use of sole PCWP for PH diagnosis, avoiding left heart catheterization [7]. Thus, digital PCWP given by cath-lab software is frequently used. Nevertheless, inaccurate PCWP measurement can cause misclassification of PH and lead to inadequate treatment [10]. Only patients in category 1 PAH are eligible for specific treatment by endothelin antagonist, PDE5 inhibitors or prostacyclin [7]. At present, only these patients benefit from this treatment.
The aim of this study is to prospectively evaluate the impact of PCWP measurement techniques on PH misclassification in patients referred for RHC with echocardiographic suspicion of PAH.
Method
Study design
This is a cross sectional study approved by the board and ethic committee of the University Teaching Hospital of Grenoble, and every patient gave informed consent for heart catheterization.
Patients
This study consisted of 31 consecutive patients referred to our PH center from January to June 2013 for right and left heart catheterization with a presumed echocardiographic diagnosis of PAH. Inclusion criteria were NYHA > 2 dyspnea, with preserved left ventricular EF, absence of valvular disease, and Doppler Right ventricle-Right atrium gradient >50mmHg. Chronic Thromboembolic Pulmonary Hypertension (CTEPH) and significant pulmonary disease patients were excluded.
RHC technique
Pressure transducer was adjusted to the zero line using the midthorax, before beginning the procedure. Patients were positioned in strict dorsal decubitus. Premedication benzodiazepin was given 1h prior to catheterization. The procedures occurred in the cardiology cath lab under fluoroscopic guidance. A Swan-Ganz catheter (Edwards 7F) was used for measurement of pulmonary pressures via the right basilic or the right jugular vein. LVEDP was assessed with a pigtail catheter (4 or 5 French) introduced by retrograde route, most of the time via the right radial artery. Systolic, mean, and diastolic arterial pulmonary pressure, and digitally computed PCWP (given by the software) as well as end expiration PCWP figure 1 were measured in the right and left pulmonary artery successively as referred in figure 2a-2c.
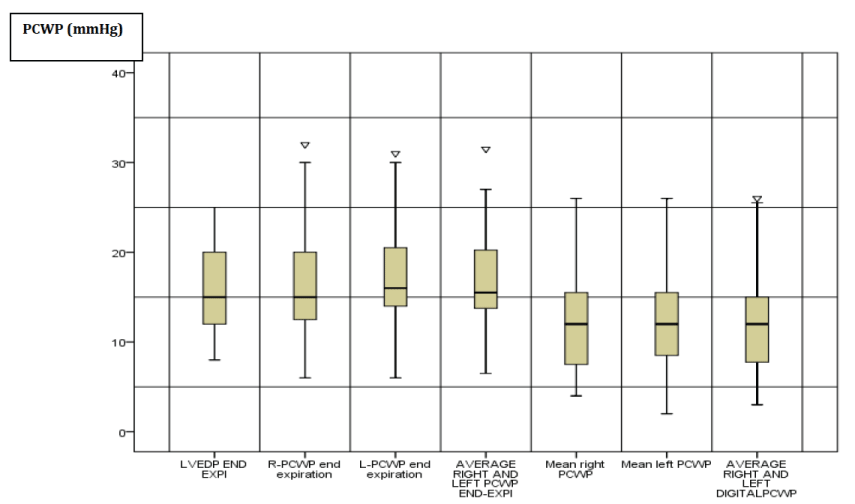
Figure 1: Boxplots distribution of different PCWP and LVEDP
measurement.
R: Right; L: Left; PCWP: Pulmonary Capillary Wedge Pressure; LVEDP
end-Exp: Left Ventricular End Diastolic Pressure End Expiration. The boxes
represent the interquartile range (Q3-Q1) between the limit inferior of the
box Q1 and the limit superior of the box Q3. The border inferior of the bars
represent the minimal value which was superior to the limit Q1-1.5 X(Q3-Q1).
The superior border of bars represent the maximal value which was inferior
to the limit Q3+ 1.5 X(Q3-Q1). The line inside the box represents the median.
The triangle indicates number of outlier values situated above or below the
adjacent values.
View Figure 1
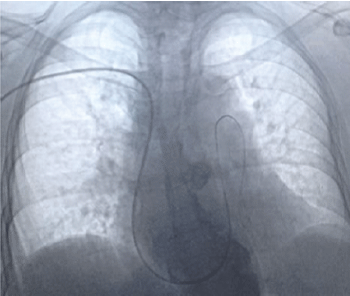
Figure 2A: Utilization of the 0.018 inch 180cm long wire inside the swann ganz
catheter to get the lower left pulmonary artery.
View Figure 2A
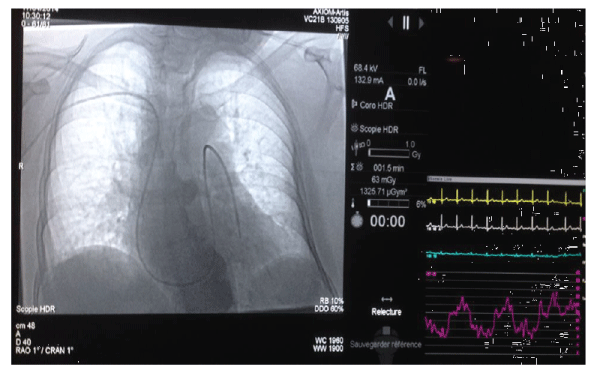
Figure 2B: Recording of spontaneous left end expiration PCWP measurement
guided by fluoroscopy monitoring.
View Figure 2B
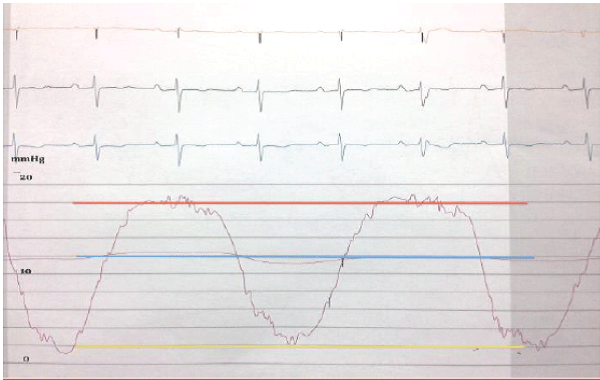
Figure 2C: PCWP wave form must specify end expiration PCWP (red line).
Instead of digital (blue line) or inspiration (yellow line)
View Figure 2C
The catheter tip was carefully pushed through the lower right and lower left pulmonary branch, when necessary using a 0.021 or 0,018-inch wire .To go through the left pulmonary artery we systematically used a 0,018- inch, 180cm long wire (TerumoR) from the right infundibulum to limit fluoroscopic time. The Swan Ganz balloon was always inflated in the right atrium and progression through the heart and vascular pulmonary bed was monitored by fluoroscopy, to limit the risk of pulmonary artery rupture and to access the lower branches. Cardiac output was measured by thermodilution technique with a 10ml bolus of frozen saline. LVEDP was both measured at end expiration and end of the diastole at the point corresponding to the upslope of the R wave on simultaneous electrocardiogram.
During RHC, patients� breathing was kept spontaneous to avoid abnormal amplitude of ventilation and especially forced expiration. Three experimented interventional cardiologists of the University Teaching Hospital of Grenoble performed catheterizations. Hemodynamic results were recorded and reviewed by two blinded interventional cardiologists. Reviewing of the PCWP was blinded from the LVEDP. No external funding was used to support this work. The authors are solely responsible for the design, conduct, analysis, drafting and editing of this study.
Statistical analysis
Continuous variables are expressed as mean � standard deviation (SD), categorical data is presented as percentages and frequencies. Correlations between digital PCWP and end expiration LVEDP and between end expiration PCWP and end expiration LVEDP were estimated using Pearson correlation coefficient. Agreement between measurements was assessed using intra class correlation coefficient [11]. Comparison of end expiration PCWP and digital PCWP in the right and left side, and then each one of them with the end expiration LVEDP, were performed using Student test for paired series. The diagnostic accuracy of right and left end expiration PCWP and digital PCWP was evaluated using end expiration LVEDP as reference standard with cut off >15mm Hg for the diagnosis of post capillary pulmonary hypertension [12]. P value 0.05 was considered statistically significant. SPSS version 22 was used for statistical analysis.
Results
Patient characteristics
We analyzed data from 31 patients. Mean age was 65.4 � 11.4 years, 67.7% were female. Brachial access was privileged to avoid complications: radial artery 80.6%, femoral artery 19.4%, basilic vein 45.2%, jugular vein 41.9% and femoral vein 12.9%. No complications were reported. The average mean PAP was 30.8 � 12.8 mm Hg, and the average PVR was 5.6 � 4.8 Wood Units Based on catheterization results, only 10% of referred patients were classified as having PAH when considering end expiration LVEDP values. The characteristics of patients and hemodynamic parameters are shown in table 1.
![]()
Table 1: Characteristics and hemodynamic parameters (N=31)
View Table 1
Hemodynamic parameters
Right and left end expiration PCWP are about same as end expiration LVEDP (< 1mmHg of difference) while digital right and left PCWP are significantly different from end expiration LVEDP (-3,4mmHg) (Table 2). We found a positive correlation between right end expiration PCWP, left end expiration PCWP, digital right PCWP, digital left PCWP and end expiration LVEDP with r value of 0.84, 0.92, 0.82, 0.85 respectively (P < 0.001). Only right and left end expiration PCWP had a good agreement with the end expiration LVEDP with intra class correlation 0.8 and 0.87 respectively (Table 3).
![]()
Table 2: Difference between different PCWP measurements and the LVEDP end
expiration. Positive values means that PCWP is higher, and the negative values
is lower than LVEDP.
View Table 2
![]()
Table 3: Correlation between PCWPS and LVEDP
View Table 3
Using end expiration LVEDP of =15 mmHg as the standard criteria to confirm the diagnosis of PAH, the operating characteristics of PCWP are demonstrated in Table 4. Better diagnostic accuracy is found for left end expiration PCWP with a sensitivity of 93.3%, a specificity of 87.5%, a positive predictive value of 87.5%, and a negative predictive value of 93.3%. AUR of digital PCWP was 0.76 in the right and left side. AUR of end expiration PCWP was 0.90 (95%CI 0.79; 1) in the right and 0, 80 (95%CI 0.66; �0.95) in the left without significant difference between these AUR, p= 0.36 for right end expiration PCWP, and 0.27 for right and left digital PCWP as compared with the best AUR of left end expiration PCWP.
![]()
Table 4: Diagnostic accuracy of different PCWP measurement for prediction of LVEDP >15mmHg.
View Table 4
Misclassification
Digital PCWP measured in the right or left pulmonary artery induced the same risk of 7/31 patient misclassification (22%). End expiration PCWP in the right pulmonary artery induced 3/ 31 patient misclassification (10%) and end expiration PCWP in the left pulmonary artery induced only 1 /31 misclassified patient (3%) compare with the LVEDP.
Discussion
Using digital PCWP instead of end expiration PCWP measurement during RHC results in a significant underestimation of the LVEDP, this translated to 22% of patients with PH being misclassified as having group1 rather than group2 PH. Using left end expiration PCWP seems to minimize the misclassification risk. This prospective study with blinding reviewing of the LVEDP and PCWP pressure waveforms confirm Ryan and all�s findings , demonstrating the correlation between end exp PCWP and LVEDP, along with the strong agreement between end expiration PWCP and LVEDP [10,13].
Patients
Our 65 years old cohort corresponds to the actual population screened for pulmonary hypertension (PH) in registries. Comorbidities are similar than those recently reported in the Reveal Registry [3] and the European registries [1,4]. Sixty-two percent of our patients presented with HFpEF, with or without associated PH at rest and only 10% of our population presented with PAH. Echocardiography screening overestimated the diagnosis of PH in 38% of our patient cohort emphasizing the need for heart catheterization in PAH diagnosis.
Hemodynamic measurement
The use of digital PCWP instead of end expiration PCWP can cause between 1/4 and 1/3 of patient misclassification, as reported here. In early 1990, in a retrospective study, Eduardo and al published a difference >5mmHg between mean PCWP and LVEDP in 30% of their right and left heart catheterized population [14].
Cath lab software does not differentiate end expiration PCWP and give digital PCWP despite new diagnostic guidelines recommending end-expiration PCWP measurement [5] during RHC in the initial diagnostic evaluation of PH. Practitioners who perform RHC should obtain and print PCWP waveforms documenting the end expiration PCWP measurement for PAH diagnosis. Thus, cath lab software should be modified to avoid confusion for practitioners and patient misclassification.
Left pulmonary artery measurement
To our knowledge, this study is the first to report the interest and the method for measuring PCWP in the left pulmonary artery. Practitioners usually measure PCWP in the right pulmonary artery because it is easier to access with a Swan Ganz inflated balloon catheter. Systematic use of a 0,021 or 0,018-inch wire inside the Swan Ganz catheter from the right ventricular infundibulum to the left pulmonary artery enabled an easy access to the left pulmonary artery.
In our series, left end expiration PCWP did not statistically differ from right end expiration PCWP but proved important to prevent misclassification of PAH. This could be explained by left pulmonary anatomy, the lower branch of the left artery being more vertical than the right one. Therefore, in our experience, the Swan Ganz catheter always remains in the pulmonary artery axis, lessening the risk of pressure wave damping. In addition, the absence of left middle lobe artery possibly allows a better reproducibility of the catheter position.
Misclassification
Although our patients were quite different from those of Ryan and all, with a majority of HFpEF diagnosis, we confirm that the use of digital PCWP instead of the end expiration PCWP or the LVEDP induce a misclassification in 22% of patients with PH as having PAH rather than group 2 PH. Referral PAH centers report an evolution in the type of PH patients, who are older and presenting more comorbidities, than 10 years ago (Reveal and French registry). Our population reflects this: mean age of 65 years old, 45.2% of HTA and 22.6% of AF. Using digital PCWP underestimates the PCWP, and thus increases diagnosis of PAH and indications for specific PH therapy. The inaccuracy of treatment carries a risk of acute heart failure in HFpEF patients and decreased possibilities to benefit from appropriate specific explorations and treatments for diastolic heart disease. Also, misclassified PAH patients could be wrongly included in therapeutic studies who test new PAH medication. This could mask potential benefits of new drugs for PAH patients because given to group 2 PH patients instead. We therefore suggest that patients who are included in PH therapeutic studies should be explored in the early diagnosis stage by left heart catheterization if end expiration PCWP wave form cannot be accurately obtained in both right and left pulmonary arteries. Left end expiration PCWP seems to minimize the risk of misclassification in our series (1/31 patient). PCWP measurement by RHC has to include a rigorous measurement of end expiration PCWP in the left pulmonary artery, as this seems to be more reliable than in the right pulmonary artery. End expiration PCWP measurement should be detailed in RHC reports and left heart catheterization should be performed when PCWP waveform is not accessible, before specific PAH treatment initiation.
Limitations
Our study represents a selected population from a single center, referred for evaluation and treatment of PH. In our study PCWP measurements are confirmed by the presence of appropriate waveform and appropriate fluoroscopic positioning appreciated by the practitioner, however fluoroscopy position at each measurement time point was not recorded.
Conclusion
At present, the suspected PAH population in developed countries is older with more comorbidities, and therefore requires a rigorous initial hemodynamic exploration to avoid misclassification of PAH patients. Using digital PCWP measurements instead of end expiration PCWP measurements during RHC results in a significant underestimation of LVEDP, and translated to 22% of patients with pulmonary hypertension being misclassified as having PAH rather than PH-HFpEF. Those misclassified patients are exposed to inadequate therapy and could falsify therapeutic studies. Our study suggests that using left end expiration PCWP in the inferior left pulmonary artery minimizes this misclassification risk when compared with using the right pulmonary artery. When end expiration PCWP waveform cannot be obtained accurately, a left heart catheterization should be performed to get LVEDP, which is the gold standard to determine post capillary pulmonary hypertension. Despite cath lab software, physicians need to ensure that the PCWP at end-expiration has been reported.
References
-
Hoeper MM, Huscher D, Ghofrani HA, Delcroix M, Distler O, et al. (2013) Elderly patients diagnosed with idiopathic pulmonary arterial hypertension: Results from the COMPERA registry. Int J Cardiology 168: 871-880.
-
Ling Y, Johnson MK, Kiely DG, Condliffe R, Elliot CA, et al. (2012) Changing Demographics, Epidemiology and Survival of Incident Pulmonary Arterial Hypertension. Am J Respir Crit Care Med 186: 790-796.
-
Badesch DB, Raskob GE, Elliott CG, Krichman AM, Farber HW, et al. (2010) Pulmonary arterial hypertension: baseline characteristics from the REVEAL Registry. Chest 1372: 376-387.
-
Humbert M, Sitbon O, Chaouat A, Bertocchi M, Habib G, et al. (2006) Pulmonary arterial hypertension in France: results from a national registry. Am J Respir Crit Care Med 173: 1023-1030.
-
Hoeper MM, Bogaard HJ, Condliffe R, Frantz R, Khanna D, et al. (2013) Definitions and Diagnosis of Pulmonary Hypertension. J Am Coll Cardiol 62: 42�50.
-
Thenappan T, Shah SJ, Gomberg-Maitland M, Collander B, Vallakati A, et al. (2011) Clinical Characteristics of Pulmonary Hypertension in Patients With Heart Failure and Preserved Ejection Fraction. Circ Heart Fail 2011; 4:257-265.
-
Galie N, Hoeper MM, Humbert M , Torbicki A, Vachiery JL, et al. (2009) Guidelines on diagnosis and treatment of pulmonary arterial hypertension: The Task Force on Diagnosis and Treatment of Pulmonary Arterial Hypertension of the European Society of Cardiology and the European Respiratory Society. Eur Heart J 30: 2493-2537
-
Sharma GV, Woods PA, Lambrew CT, Berg CM, Pietro DA, et al. (2002) Evaluation of a noninvasive system for determining left ventricular filling pressure. Arch Intern Med 162: 2084-2088.
-
Rudolf K.F. Oliveira, Roberta P. Ramos, Eloara V.M. Ferreira, Fl�vio F. Arbex, Carlos E.B. Kapins, et al. (2012) Pulmonary Capillary Wedge Pressure 15 mmHg Is A Good Indicator Of Normal Left Ventricular Filling Pressure In Pulmonary Arterial Hypertension Patients. Ajrccm �conference 2012.185.1_MeetingAbstracts. A6225.
-
Ryan JJ, Rich JD, Thiruvoipati T, Swamy R, Kim GH, et al. (2012) Current practice for determining pulmonary capillary wedge pressure predisposes to serious errors in the classification of patients with pulmonary hypertension. Am Heart J 163: 589-594.
-
Field AP (2005) "Intraclass Correlation," in Encyclopedia of Statistics in Behavioral Science, Chichester: John Wiley & Sons: 948-954.
-
Bossuyt PM, Reitsma JB, Bruns DE, Gatsonis CA, Glasziou PP, et al. (2003) The STARD Statement for Reporting Studies of Diagnostic Accuracy: Explanation and Elaboration. Clinical Chemistry 49: 17-18.
-
Halpern SD, Taichman DB. FCCP (2009) Misclassification of Pulmonary Hypertension Due to Reliance on Pulmonary Capillary Wedge Pressure Rather Than Left Ventricular End-Diastolic Pressure. Chest 136: 37-43
-
Flores ED, Lange RA, Hillis LD (1990) Relation of mean pulmonary arterial wedge pressure and left ventricular end-diastolic pressure. Am J Cardiol 66: 1532-1533.





