International Journal of Respiratory and Pulmonary Medicine
An Enlarging Airway Foreign Body
Vijay Hadda*, Kavitha Venkatnarayan, Karan Madan, Anant Mohan and GC Khilnani
Department of Pulmonary Medicine, All India Institute of Medical Sciences, New Delhi, India
*Corresponding author: Vijay Hadda, Assistant Professor, Department of Pulmonary Medicine and Sleep Disorders, All India Institute of Medical Sciences, New Delhi, India, Tel: +91-9868883208, E-mail: vijayhadda@yahoo.com
Int J Respir Pulm Med, IJRPM-2-011, (Volume 2, Issue 1), Case Report; ISSN: 2378-3516
Received: December 31, 2014 | Accepted: January 23, 2015 | Published: January 26, 2015
Citation: Hadda V, Venkatnarayan K, Madan K, Mohan A, Khilnani GC (2015) An Enlarging Airway Foreign Body. Int J Respir Pulm Med 2:011. 10.23937/2378-3516/1410011
Copyright: © 2015 Hadda V, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
A 25-year-old female patient presented with dry coughs of 20 days duration and fever for four days.Examination of respiratory system revealed no significant abnormality. Chest radiograph was normal. CT scan of the thorax revealed endobronchial opacity in the right main bronchus suggestive of a foreign body. Patient retrospectively recollected history of betel nut aspiration just prior to onset of symptoms. Flexible bronchoscopyrevealed a large sized blackish-brownish large foreign body (betel nut) in the right main bronchus which was successfully removed using the flexible bronchoscope itself. Due to the hygroscopic character of betel nut, it had absorbed moisture and had considerably increased in size. Although rigid bronchoscope is the preferable modality for removal of large sized airway foreign bodies, flexible bronchoscope is especially useful and often preferable as it obviates the need for general anesthesia.
Background
Foreign body (FB) aspiration is a common occurrence among preschool children however it is uncommonly seen in adults. In adults, the diagnosis is usually delayed due to non-asphyxiating symptoms and many times confused with other lung diseases. [1] Foreign body aspiration if undiagnosed can often lead to distal airway complications such as partial or whole lung collapse, post-obstructive pneumonia, hemoptysis etc. Once diagnosed, the management involves use of rigid or flexible bronchoscopy (FOB) for prompt removal the FB [1]. Here in we present a young female who presented almost 3 weeks after aspiration of a betel nut and was successfully managed with use of FOB. Owing to the hygroscopic nature of the aspirated FB, the same had absorbed water and had assumed a larger than its original size leading to a possibly delayed presentation. Flexible bronchoscopic removal of this large organic foreign body is another highlight of this case.
Case Report
A 25-year lady presented with dry cough of 20 days duration. There was no history of breathlessness, chest pain, hemoptysis or fever at the time of onset of symptoms. Four days prior to presentation, patient developed fever associated with worsening cough associated with mucopurulent expectoration. Patient had been prescribed some medications at a local center with which fever and expectoration improved but cough persisted. Her appetite and weight were normal during this period.
On examination, blood pressure (100/78mmHg), pulse rate (94/min) and respiratory rate (22/min) were normal. Examination of chest revealed no significant abnormality. Other systemic examination was also unremarkable. Posteroanterior radiograph of chest was normal (Figure 1). In view of persistent symptoms, CT scan examination of the thorax was (Figure 2) done. It revealed endobronchial opacity in the right main bronchus suggestive of a foreign body which was almost completely occluding the lumen of the right main bronchus. Hyperlucency of the right lung fields was also observed suggestive of post obstructive hyperinflation. The opacity looked well defined and did not appear to arise from the wall of the bronchus. Patient�s history was reviewed again and she recollected that on the night prior to onset of symptom, she was chewing a betel nut and while laughing on a joke during conversation she had likely aspirated it.
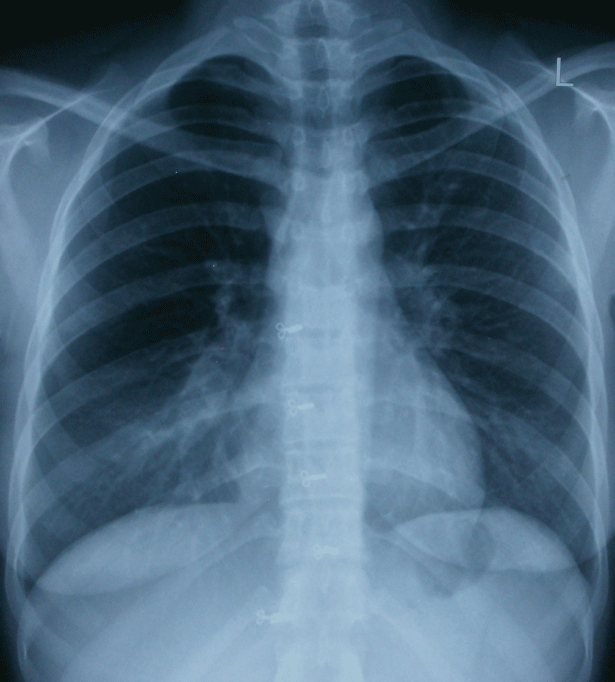
Figure 1: Postero-anterior chest radiograph showing no abnormality
View Figure 1
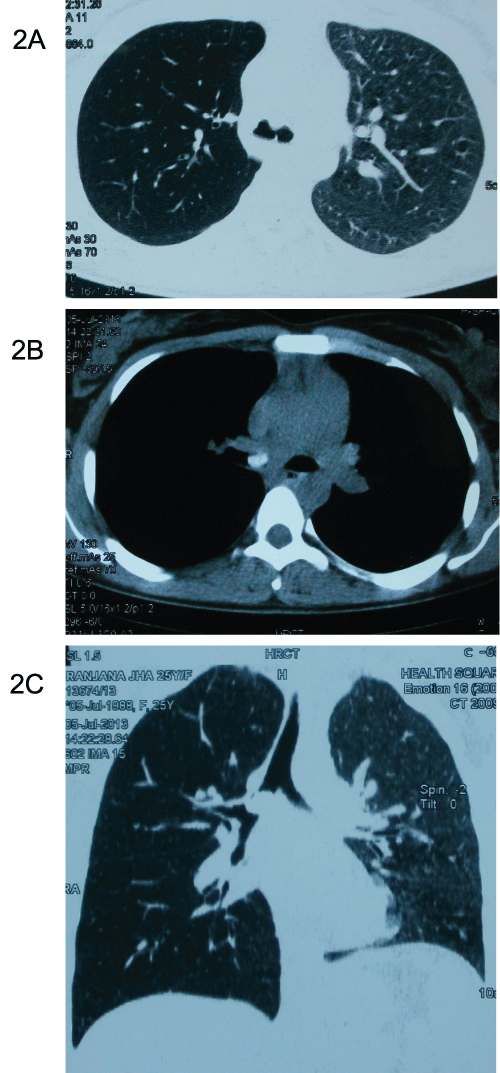
Figure 2: CT scan of the thorax showing a foreign body in the right main
bronchus completely occluding it (2a).Hyper lucent right lung field suggestive
of post obstructive hyperinflation due to ball valve effect is also seen (2b). The
coronal section of the same CT scan shows endobronchial opacity in the right
main bronchus which is almost completely occluding the lumen of the right
main bronchus (2c).
View Figure 2
With a diagnosis of FB aspiration in the right main bronchus, we performed FOB for further evaluation and to attempt removal of FB. FOB was performed under conscious sedation (using injection fentanyl and midazolam) and local anesthesia (using topical lignocaine). It revealed a blackish-brown large FB (betel nut) in the right main bronchus approximately 2.5 cm distal to the carina. The foreign body appeared to have enlarged in size after entry into the bronchial tree owing to its hygroscopic character as its size was considerably larger than that of a usual sized betel nut (Figure 3). FB was successfully removed using flexible bronchoscopic accessories (rat tooth forceps and dormia basket). Granulation tissue was also noticed at the FB impaction site.
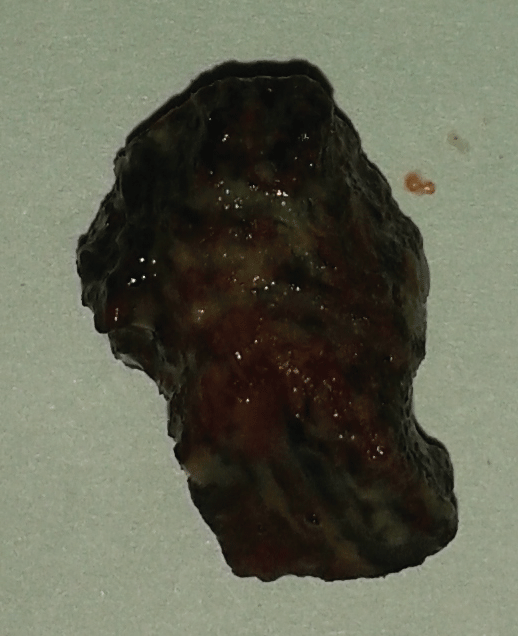
Figure 3: Blackish-brown large foreign body (betel nut) removed from the right main bronchus
View Figure 3
Patient had immediate improvement following the procedure and follow up chest radiograph was normal. There were no immediate or delayed complications and patient continues to be asymptomatic till date.
Discussion
Tracheobronchial FB aspiration is rare in adults. Risk factors in adults include altered sensorium, compromised airway reflexes, advanced age, trauma and dental procedures [1,2]. Adults constitute approximately 20% cases of tracheobronchial aspiration [2]. Peak incidence of foreign body aspiration occurs in preschool age children [3]. Among adults, the median age group reported is 60 years [2]. This is attributed to higher incidence of cerebrovascular and neurodegenerative disorders in elderly that compromise swallowing and airway protective reflexes. Most commonly aspirated materials include vegetable matter, dental appliances/prosthesis, medical appliances, bone fragments etc. [2]. A history suggestive of aspiration may not be forthcoming in most of the adults and some may recollect it retrospectively after the retrieval as occurred in our patient.
Vegetable matter � like foreign bodies constitute nearly 70% of cases in various series [4]. Betel nut is a commonly incriminated agent in foreign body aspirations from the South East Asian region. It is the most commonly reported foreign body in some studies. It can also cause reflex bronchospasm and erosion of the tracheobronchial tree [5]. Other commonly reported vegetable foreign bodies include peanuts, seeds and beans. Vegetable foreign bodies are more dangerous as being hygroscopic they absorb moisture, swell up and cause more bronchial obstruction. They may cause allergic or chemical bronchitis (vegetable bronchitis). They also cause problems during retrieval � may break into fragments or cause difficulty in negotiating the vocal cords due to hygroscopic nature as occurred in our patient [6]. In our patient, the removed foreign body was considerably larger in size than a usual betel nut and had caused excessive granulation tissue formation too at the site of impaction in the bronchial tree.
Most common symptom reported following aspiration of a foreign body is the �penetration syndrome� characterized by choking and intractable cough. This is followed by other symptoms like cough, fever, breathlessness and wheezing due to airway compromise or post obstructive complications like pneumonia [7]. Symptoms following aspiration may vary from life threatening airway obstruction to non specific symptoms. A history suggestive of aspiration may not be available always. In some the episode of aspiration may go unnoticed and they may present later with complications like post obstructive pneumonitis, hemoptysis, bronchiectasis, recurrent pneumonia, stricture or lung abscess [8]. A high index of suspicion is required in young adults and elderly who present with the above symptom complex for early diagnosis and management to avoid long term complications.
Chest radiograph is the most commonly performed investigation in the emergency department in suspected foreign body aspiration. It is diagnostic in < 30% of cases presenting with acute symptoms [9]. Even in chronic cases, nearly 30% of the patients have a normal chest radiograph. The yield of chest radiograph depends on the physical characteristics of the aspirated material. Chest radiographs are most useful if the aspirated material is radio opaque which can be readily identified. Organic materials are not radio opaque and are missed on chest radiographs as occurred in our patient. In such cases indirect radiological signs of aspiration include lung atelectasis/collapse if the foreign body completely occludes the bronchus (22.6%), post obstructive pneumonia (19.6%), hyperlucency secondary to air trapping if the foreign body has a ball valve effect (3.2%) and pneumomediastinum (3.2%) [9].
A chest CT scan may be helpful in patients presenting with non specific symptoms or in patients with a strong suspicion of foreign body aspiration but negative chest radiograph. The findings on CT scan depend on the physical characteristics of the foreign body and the time duration when performed after aspiration. The most definitive sign of the presence of an endobronchial foreign body may not be seen in all patients. Other nonspecific findings similar to chest radiograph include atelectasis, hyperlucency, bronchiectasis, lobar consolidation, tree-in-bud opacities, pleural effusion, and hilar adenopathy [10]. A normal chest radiograph or CT scan does not negate the need to directly inspect the airways in cases with strong suspicion.
Once diagnosed, prompt removal of foreign body is essential to avoid irreversible complications. Flexible bronchoscopy is successful in retrieval in 90% of cases [11]. Successful removal of large sized foreign bodies has also been reported using the flexible bronchoscope [12]. In certain situations, rigid bronchoscopy or surgery may be required. In patients presenting with critical airway obstruction or respiratory failure, rigid bronchoscopy is the preferred modality of retrieval [13,14]. Delay in diagnosis may lead to formation of granulation tissue and impaction of the foreign body leading to difficulty in retrieval. Various ancillary instruments are used for retrieval including rat toothed forceps, snare, fogarty balloon, dormia basket, cryoprobe etc. After retrieved, it is important to inspect the entire tracheobronchial tree to rule out other residual foreign bodies [15].
References
-
Boyd M, Chatterjee A, Chiles C, Chin R Jr (2009) Tracheobronchial foreign body aspiration in adults. South Med J 102: 171-174.
-
Limper AH, Prakash UB (1990) Tracheobronchial foreign bodies in adults. Ann Intern Med 112: 604-609.
-
McGuirt WF, Holmes KD, Feehs R, Browne JD (1988) Tracheobronchial foreign bodies. Laryngoscope 98: 615-618.
-
Anandkumar A, Ashokkumar C, Lathi A, Kishve S, (2013) Study of incidence and various types of foreign bodies in tracheobronchial tree in rural population. Indian Journal of Basic and Applied Medical Research 3: 27-32.
-
Samad L, Ali M, Ramzi H (1998) Tracheobronchial foreign bodies in children: reaching a diagnosis. J Pak Med Assoc 48: 332-334.
-
Sehgal A, Singh V, Chandra J, Mathur NN (2002) Foreign body aspiration. Indian Pediatr 39: 1006-1010.
-
Baharloo F, Veyckemans F, Francis C, Biettlot MP, Rodenstein DO (1999) Tracheobronchial foreign bodies: presentation and management in children and adults. Chest 115: 1357-1362.
-
Chen CH, Lai CL, Tsai TT, Lee YC, Perng RP (1997) Foreign body aspiration into the lower airway in Chinese adults. Chest 112: 129-133.
-
Pinto A, Scaglione M, Pinto F, Guidi G, Pepe M, et al. (2006) Tracheobronchial aspiration of foreign bodies: current indications for emergency plain chest radiography. Radiol Med 111: 497-506.
-
Zissin R, Shapiro-Feinberg M, Rozenman J, Apter S, Smorjik J, et al. (2001) CT findings of the chest in adults with aspirated foreign bodies. Eur Radiol 11: 606-611.
-
Lan RS (1994) Non-asphyxiating tracheobronchial foreign bodies in adults. Eur Respir J 7: 510-514.
-
Jamshed N, Madan K, Ekka M, Guleria R (2014) Successful flexible bronchoscopic management of a large-sized aspirated partial denture. BMJ Case Rep 2014.
-
Madan K, Aggarwal AN, Bhagat H, Singh N (2013) Acute respiratory failure following traumatic tooth aspiration. BMJ Case Rep 2013.
-
Madan K, Agarwal R, Aggarwal AN, Gupta D (2014) Therapeutic rigid bronchoscopy at a tertiary care center in North India: Initial experience and systematic review of Indian literature. Lung India 31: 9-15.
-
Swanson KL (2004) Airway foreign bodies: what's new? Semin Respir Crit Care Med 25: 405-411.





