International Journal of Respiratory and Pulmonary Medicine
Does the Body Mass Index Affect the Success of Noninvasive Mechanical Ventilation in Patients with Acute Hypercapnic Respiratory Failure?
Esmehan Akpinar1, Serdar Akpinar2* and Nazire Ucar1
1Department of Chest Diseases, Ataturk Chest Diseases and Chest Surgery Education Research Hospital, Turkey
2Department of Chest Diseases, Intensive Care Unit, Diskapi Yildirim Beyazit Training and Research Hospital, Turkey
*Corresponding author: Serdar Akpinar MD, Department of Chest Diseases, Intensive Care Unit, Diskapi Yildirim Beyazit Training and Research Hospital, Turkey, Tel: +905335580592, E-mail: drserdarakpinar@yahoo.com
Int J Respir Pulm Med, IJRPM-2-014, (Volume 2, Issue 1), Research Article; ISSN: 2378-3516
Received: January 21, 2015 | Accepted: February 11, 2015 | Published: February 15, 2015
Citation: Akpinar E, Akpinar S, Ucar N (2015) Does the Body Mass Index Affect the Success of Noninvasive Mechanical Ventilation in Patients with Acute Hypercapnic Respiratory Failure? Int J Respir Pulm Med 2:014. 10.23937/2378-3516/1410014
Copyright: © 2015 Akpinar E, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective: Obesity has many negative effects on lung functions. It is not yet clear whether body mass index (BMI) affects the success of noninvasive mechanical ventilation (NIMV). The aim of this study was to investigate the differences in NIMV strategies, on the basis of BMI, in patients with acute hypercapnic respiratory failure and the effect of BMI on the success of NIMV.
Methods: A total of 86 patients who had acute hypercapnic respiratory failure were enrolled consecutively. They were grouped according to BMI as follows: BMI 18.5 - 24.9kg/m2 (normal); group 1, BMI 25 - 30kg/m2 (overweight); group 2, BMI>30kg/m2 (obese); group 3. Age, gender, duration of ICU stay, pressures of NIMV and Arterial Blood Gas (ABG) before, during and after the NIMV were recorded.
Results: In total, 52 patients (60%) were male. The mean age of the patients was 70 � 12 years. The success rates of NIMV in groups 1, 2 and 3 were 50%, 28% and 21%, respectively. The success rates were not significantly different between groups (p=0.79). In group 3, the respiratory rate was higher and pH was lower during the first hour compared to the other groups (p< 0.05, p< 0.05). PaCO2 levels were higher in group 3 on the first day and at the end of NIMV treatment (p=0.04, p< 0.05).
Conclusion: NIMV strategies should be different in acute hypercapnic respiratory failure patients with a high BMI, and in these patients, clinical improvement requires a long duration.
Keywords
Hypercapnic respiratory failure, NIMV, BMI
Introduction
Noninvasive Mechanical Ventilation (NIMV) application strategies and the factors affecting its success are still highly disputed issues. In acute and chronic respiratory failure cases, which may develop in association with different etiologies, there have been many studies concerning the applied NIMV methods and their results [1,2]. Among the factors concerning the patient, age and comorbid diseases (cardiovascular diseases, immunosuppression, pneumonia etc.) have been the most commonly emphasized [1]. However, few studies have investigated the influence of body weight or that of body mass index (BMI) in acute respiratory failure on NIMV.
In patients with chronic respiratory failure, it has been observed that lower BMI can lead to the impairment of pulmonary functions and the reduction of NIMV efficiency [3]. However, the effects of higher BMI in NIMV application are still not clearly known. Obesity (BMI>30kg/m2) has become an important health problem, affecting 312 million people in developed and developing countries, and its prevalence in intensive care units has been substantially increasing [4,5]. There is obesity in 18% of the patients with chronic obstructive pulmonary disease (COPD) and in 16% to 24% of the patients with other respiratory failures [3].
Obesity has important effects on pulmonary functions and the functioning of other systems. Direct and indirect relationships between obesity and Obesity Hypoventilation Syndrome (OHS), Obstructive Sleep Apnea Syndrome (OSAS), postoperative acute respiratory failure and other medical problems have been demonstrated [6]. These patients are usually admitted to an intensive care unit for various reasons, such as hypercapnic respiratory failure, cor pulmonale, COPD attack, asthma attack, and pulmonary embolism [6,7]. The optimal mechanic ventilation methods applied in the intensive care unit are usually not used. The aim of the study was to investigate the effect of the BMI on the success of NIMV in patients with acute hypercapnic respiratory failure.
Materials and Methods
The patients who admitted to the respiratory care unit of Atat�rk Chest Disease and Thoracic Surgery Training and Research Hospital between December, 2011 and March, 2013 and had acute hypercapnic respiratory failure were included. This study was planned as a retrospective cohort study. The required approval of the local ethics committee was obtained before beginning the study. The cases were divided into three groups as follows: Group 1 was composed of subjects with normal weight BMI between 18.5 - 24.9kg/m2, Group 2 was formed composed of overweight patients with BMI between 25 - 30kg/m2, and Group 3 was composed of obese patients with BMI greater than 30kg/m2.
Inclusion criteria
Patients who had acute hypercapnic respiratory failure (pH< 7.35 and PaCO2>45 mmHg in ABG analysis, respiratory rate>25 per minute) were included in the study.
Exclusion criteria
Patients with malignancy or terminal respiratory disease, loss of conscious or clouding of consciousness (except hypercapnic encephalopathy), respiratory and/or cardiac arrest, intense secretion, agitation and lack of cooperation, unstable clinical condition (hypotensive shock, cardiac ischemia), trauma, burns, anatomic disorders of the face that would prevent a mask from being secured, impaired cough and swallowing reflex, and pure hypoxemic failure (PaO2< 60mmHg and PaCO2< 45mmHg in ABG analysis) were excluded from the study.
Definition criteria
Acute hypercapnic respiratory failure was defined to be present if PaO2 was < 60mmHg when patients received oxygen therapy and PaCO2>45mmHg and pH< 7.35.
OSAS was defined according to American Academy of Sleep Medicine Task Force (Table 1) [8].
![]()
Table 1: Obstructive sleep apnea syndrome (OSAS) definition according to American Academy of Sleep Medicine Task Force.
View Table 1
Overlap syndrome was defined as the combination of COPD and sleep apnea- hypopnea syndrome [9]. COPD was defined according to the GOLD criteria [10].
Age, gender, APACHE II score, serum C-reactive protein (CRP) level, respiratory rate, intubation, mortality, lengths of stay in intensive care unit, lengths of stay in hospital, diagnoses, comorbid diseases, sessions of NIMV application, inspiratory positive airway pressure (IPAP), expiratory positive airway pressure (EPAP), initial, first hour-, fourth hour-, twenty fourth hour- ABG and the ABG values during discharge from the intensive care unit of all cases included into the study were recorded. The patients that had one major criterion (fever>38�C, cough, purulent sputum) or two minor criteria (dyspnea, chest pain, pulmonary consolidation evidence in physical examination, leukocyte counts >12000mm3 or < 4000 mm3) consistent with pneumonia, together with infiltration evidence in X-ray images, were considered as having pneumonia [11].
The failure of NIMV was determined in cases with 1 major or 2 minor criteria within the first hour of NIMV. The major criteria were considered to be respiratory arrest, loss of consciousness, psychomotor agitation necessitating sedation, impaired hemodynamics (systolic blood pressure < 70 mmHg or >180mmHg), and bradycardia (HR< 50 beats/min). The minor criteria were a RR of >35/min that was also higher compared to the rate recorded at the time of initial presentation, arterial pH < 7.30 that was also lower compared to the initial presentation, PaO2< 45mmHg despite oxygen support, and absence of a cough reflex that would clear secretions.
To use the APACHE II score system, the admittance of the patients to the intensive care unit (ICU), ABG analysis, biochemistry, hemogram, arterial blood pressure, body temperature, Glasgow Coma Scale (GCS), respiratory rate (RR) and heart rate (HR) were recorded.
NIMV application was performed through BiPAP Vision (BiPap® Vision, Respironics, USA) by using an oronasal mask of standard dimensions such that it covered the nose and the mouth. At the beginning, expiratory positive airway pressure (EPAP) was adjusted as 5cm H2O and Inspiratory Positive Airway Pressure (IPAP) was adjusted to 10cm H2O in pressure-support mode. As the cases improved according to the alterations in blood gas, the pressures were increased to 1 to 2cm H2O. Back-up rate was adjusted in the beginning of the NIMV, it was not manipulated during treatment. Additionally, medical treatment appropriate to their diagnoses was administered.
Statistical Analysis
Data analysis was performed with the SPSS for Windows 15 software package. Descriptive statistics were summarized in a table by determining the means and standard deviations.
The Kruskal Wallis test was used for the comparison of ventilator parameters and ABG values. The Chi-Square test was used in the comparison of mortality, intubation, length of stay in the hospital, and length of stay in the Intensive Care Unit between groups. In the patients with successful NIMV, the Chi-Square test and Mann-Whitney U test were used in the comparison of differences in terms of pneumonia, diagnosis of OSAS, APACHE II score, and CRP level. The t-test was used in the comparison of diagnosis ratios between groups. The results were considered to be statistically significant when p< 0.05.
Results
A total of 310 patients were accepted to the ICU of Atat�rk Chest Disease and Thoracic Surgery Training and Research Hospital between December, 2011 and March, 2013. A hundred and ten patients had acute hypercapnic respiratory failure. Of these, 86 patients who had acute hypercapnic respiratory failure were included in the study. Twenty-four patients were excluded (5 patients had agitation and lack of cooperation, 7 had malignancy, 2 had anatomic disorders of face, 6 had intense secretion and 4 of them had respiratory arrest). The number of patients in study groups (Group 1-3) respectively as follows; 45, 26, 15. Fifty two of patients were male (60.5%) and thirty four (39.5%) of them were female and the mean age of patients was 70 � 12 years. The mean BMI values of the three groups are summarized in Figure 1. When studied in terms of primary disease, sixty three (73%) of the cases had a diagnosis of COPD, eighteen (20%) had a diagnosis of OSAS, two (2.3%) had a diagnosis of Overlap syndrome, two (2.3%) had a diagnosis of restrictive disorder associated with kyphoscoliosis and one (1.2%) had a diagnosis of other diseases (Figure 2). Eighty percent [12] of the obese patients were female, and 20% (3) of them were male. There were more female patients in the obese group (p=0.01). The intubation ratio was found to be 31.2% in the first group, 30.3% in the second group and 40% in the third group. Although there was no statistically significant difference between the groups, the intubation ratio was higher in the third group (p=0.79).
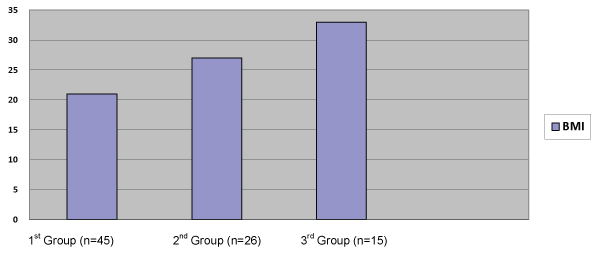
Figure 1: Mean Body Mass Index (BMI) values
View Figure 1
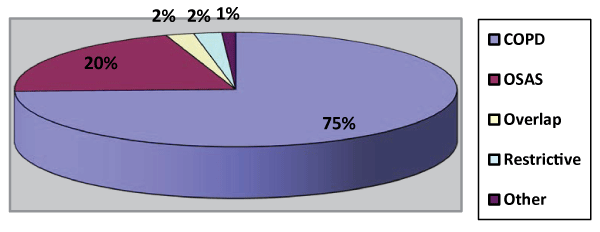
Figure 2: The distribution of the patients according to their primary diagnoses (COPD: Chronic Obstructive Pulmonary Disease; OSAS: Obstructive
Sleep Apnea Sendrome)
View Figure 2
Mortality was observed in ten patients (22.5%) in the first group, three patients (11.5%) in the second group and three patients (20%) in the third group. No statistically significant difference was found between the groups (p=0.53). The length of stay in the ICU was 10 � 3 days in the first group, 9 � 6 days in the second group and 10 � 12 days in the third group. No statistically significant difference was found between the groups (p=0.93).
The length of stay in the hospital was 17 � 13 days in the first group, 19 � 7 days in the second group and 22 � 11 days in the third group. No statistically significant difference was found between the groups (p=0.34).
When the success of NIMV was studied in terms of groups, it was found to be 50.2% in the first group, 28.3% in the second group and 21% in the third group. No statistically significant difference was found between the groups (p=0.79). However, the success rate of NIMV was lower in obese patients. There was pneumonia as an additional disease in 25.9% of the fifty eight patients with successful NIMV and in 44% of the twenty eight patients with unsuccessful NIMV. Although it was not statistically significant, there rate of patients with pneumonia was higher in the group with unsuccessful NIMV.
When the groups were studied, no significant difference was found in the respiratory rate before NIMV application between the groups (p=0.47). The mean respiratory rate of the first hour after NIMV application was 21 � 4 in the first group, 20 � 4 in the second group and 26 � 6 in the third group. In obese patients, the respiratory rate of the first hour was higher, and this difference was statistically significant (p=0.05) (Figure 3). A total of 15.5% of the patients with successful NIMV and 21.4% of those with unsuccessful NIMV had OSAS. No statistically significant difference was found (p=0.55).
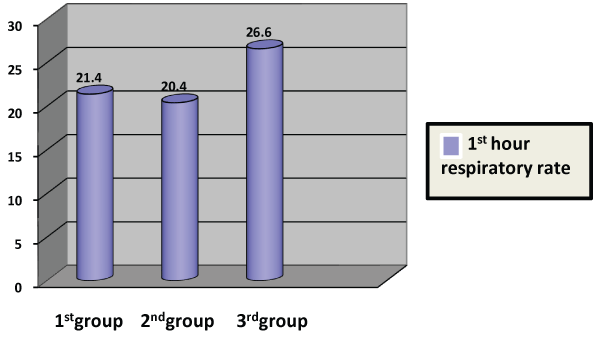
Figure 3: First-hour respiratory rates of the groups after the application of Noninvasive Mechanical Ventilation (NIMV)
View Figure 3
The mean serum CRP level was 7 � 6mg/L in the first group, 9 � 6mg/L in the second group and 6 � 5 mg/L in the third group. There was no statistically significant difference between the groups. (p=0.64). However, while the mean CRP level was 6 � 6mg/L in the group with successful NIMV, it was 10.1 � 6mg/L in the group with unsuccessful NIMV. Accordingly, the CRP level was statistically higher in the group with unsuccessful NIMV (p=0.01).
The mean APACHE II score was 23.2 � 3.9 in patients with unsuccessful NIMV, and this was significantly higher compared to patients with successful NIMV (p=0.001). When the cases in which either mortality was observed or not were investigated, the mean APACHE II score values were 23 � 2 and 17.9 � 4, respectively. The APACHE II values in the group in which mortality was seen was higher, and this difference was statistically significant (p=0.01).
Although the first-hour and fourth-hour values of PaCO2 were higher in the obese group after NIMV application and the fourth-hour pH values were lower in this group, there was no significant difference between the three groups. However, the first-hour pH value was found to be lower in obese patients and first day and discharge PaCO2 values were found to be statistically higher in these patients. (p< 0.05, p=0.04, p< 0.05, respectively) (Table 2).
![]()
Table 2: Arterial Blood Gas (ABG) values during the treatment progress.
View Table 2
Although the initial respiratory rates of the patients of the three groups were closer to each other, the first-hour respiratory rate after NIMV application was found to be higher in the obese group (mean= 27 � 6 per minute, p=0.04). In terms of ventilator parameters, the mean IPAP values were 16 � 2cm H2O in the first group, 16 � 3cm H2O in the second group and 20 � 3 cm H2O in the third group. The NIMV pressure values were in significantly higher in the obese group (p=0.001). When the mean EPAP values were compared, they were 6 � 1 cm H2O in the first group, 7 � 2cm H2O in the second group and 9 � 2 cm H2O in the third group. A statistically significant correlation was found between an increase of BMI and EPAP values (p=0.001) (Table 3).
![]()
Table 3: The differences between mean Inspiratory Positive Airway Pressure (IPAP) and Expiratory Positive Airway Pressure (EPAP) values in terms of body
mass index (BMI)
View Table 3
Discussion
In this study, NIMV application and its results resulted in differences in obese patients compared to the other groups. In the group of obese patients, the response in the ABG analysis to NIMV application was slower compared to other groups and the carbon dioxide ratios progressed higher in the progress of treatment. When obese patients were compensated with higher IPAP values, the IPAP and EPAP levels increased with BMI.
Obesity is occurring at an increasing rate, not only in developed countries but also in developing countries. Previous publications have indicated that OHS is one of the important causes of the respiratory failure and occurs in higher ratios in females. Among them, the obesity ratio was found to be higher in females in a study which included 219 patients and in which the influences of obesity in the ICU were studied [12]. Similarly, in a study including 2148 patients in the intensive care unit that investigated the influences of BMI, the authors found that 65% of obese patients were female [13].
In a study comprising seventy-three patients with hypercapnic respiratory failure, the authors found that the ratio of females among obese patients was 72% [14]. In a study conducted in Turkey, the obesity incidence was found to be 15% to 16% and the obesity ratio was found to be 20% in males and 40% in females [15]. In this study, 17% of the patients were obese, of which 80% were female. Obesity is seen more commonly in young adults, and the lower incidence of obesity in elderly people may be due to cardiovascular events [13]. However, in this study, the mean age was around the geriatric age group and there was no difference in age between the groups.
Goulenok and EI-Solh investigated the influence of obesity on the patients in the ICU, and their results from two distinct studies demonstrated that the mortality ratio was statistically higher in obese patients [16,17]. In a study that comprised fifty morbid obese patients, the authors found a higher mortality in the group having greater BMI [18]. In two distinct studies, the authors found no significant relationship between mortality and obesity [12,19].
In a meta-analysis comprising 88051 patients, no significant relationship was found between obesity and mortality [20]. However, because the patients were of heterogeneous groups, this study does not provide additional information concerning obese patients.
In our study, although the mortality ratios in obese patients were found to be higher, this result was not statistically significant. Previous studies investigating the effect of BMI on mortality rates in ICU patients concluded that mortality was higher in obese patients [12,17,18]. However, in these studies, the ratio of morbidly obese patients was higher than in our study.
In recent studies, the utility of the serum CRP level as an important indicator of inflammation and respiratory failure has been investigated. Additionally, various studies have showed that the level of CRP is increased in obesity. It was found that the elevation of CRP was associated with the failure of mechanical ventilation and with the length of intubation duration in a study of thirty patients in the ICU [21]. In a study of ninety-five patients, the authors found that higher APACHE II and CRP levels were related to the failure of NIMV in patients with acute hypercapnic respiratory failure [22]. In another study, the authors found that in their cohort of sixty patients with acute hypercapnic respiratory failure, APACHE II and CRP levels were independent risk factors for determining the success of treatment with NIMV [23]. In a study, it was found that higher CRP values were associated with poor prognosis in patients with OHS in which NIMV was applied. In this study, a statistically higher CRP level was found in the unsuccessful NIMV group [24].
How the presence of the accompanying pneumonia in patients with acute hypercapnic respiratory failure affects the success of NIMV is another important issue. Although the majority of the studies conducted for this purpose did not contain hypercapnic patients, some studies have demonstrated that the success rates of NIMV is lower in pneumonia patients with hypercapnic respiratory failure. In a postmortem study of forty-three patients who were hospitalized due to COPD attack and in which early period mortality was seen, the authors identified that the most important cause of death was pneumonia [25]. In various clinical studies, it has been stated that the ratio of intubation and mortality are higher in cases experiencing pneumonia due to attacks of COPD [26]. In our study, there was pneumonia in 44% of patients in the unsuccessful NIMV group, and a higher ratio of pneumonia was noticeable in the unsuccessful group.
Concerning the obese patients, the lengths of stay in the ICU is another issue to be emphasized. Among them, in a meta-analysis comprising 62045 patients, it has been emphasized that the lengths of stay in the ICU of the patients with BMI >30 kg/m2 is higher than that of the patients with BMI< 30kg/m2 [27]. In a study in which the influence of BMI on the length of stay in the ICU was investigated, it was reported that BMI does not affect the length of stay in the ICU, length of stay in hospital, mortality and intubation ratio [13]. In another study reporting that obesity does not affect the length of stay in the ICU, it was also found that there was no difference between obese and non-obese patients in terms of mortality and intubation [14]. In this study, there was no difference between the groups in terms of the length of stay in the ICU and the length of stay in hospital. Again, no difference was observed between the groups in terms of intubation ratios and mortality.
Alterations in ABG, particularly in pH, are an important criterion in evaluating the success of NIMV [28]. In several studies, it has been reported that patients with unsuccessful NIMV have lower pH values compared to those with successful NIMV [29]. On the other hand, no relationship has been shown between basal ABG values and between the responses to NIMV [30]. In a study involving seventy-six morbid obese patients having acute respiratory failure the authors emphasized that there was a delayed response to NIMV in more than the half of the patients and that the response in pH and PaCO2 levels was not sufficient at the end of the first hour [31]. In a study, it was emphasized that more time is required for PaCO2 to be reduced to below the 50mmHg level in obese patients. In a study which included forty-one obese hypercapnic patients, the authors reported that there was no difference between obese and non-obese patients in terms of carbon dioxide elimination rate [32].
Similarly, in this study, in obese patients, the first-hour pH was lower and first day- and discharge-PaCO2 values were higher after NIMV application compared to the control group. Thus, we suggest that pH and PaCO2 may be insufficient for the evaluation of the success of NIMV at an early period in obese patients. Furthermore, the application of failure criteria of NIMV in obese patients in the early period may lead to the earlier cessation of NIMV, which may be unnecessary and may lead to unnecessary intubations. Similarly, it is known whether the improvement in respiratory rate within the first hour is important in the evaluation of the objective response to NIMV [33-35]. In this study, the respiratory rate at the end of the first hour after NIMV application was found to be higher in obese group, compared to other groups.
The limitations of the study are as follows: this was a retrospective study and the number of the patients who were included to the study, especially morbidly obese ones, was limited. Further larger prospective studies are necessary to clarify the effects of BMI on NIMV application.
Conclusion
In conclusion, there are differences in the evaluation of the early response in obese patients with acute hypercapnic respiratory failure in whom NIMV has been applied compared to patients with normal BMI. In NIMV application, the first-hour respiratory rates of obese patients, and their first-hour- carbon dioxide values and their carbon dioxide values during the transfer from the intensive care unit progress at higher levels. It should be taken into account that the early response can be later than the normal response in obese patients in whom NIMV is applied due to acute hypercapnic respiratory failure.
References
-
Robino C, Faisy C, Diehl JL, Rezqui N, Labrousse J, et al. (2003) Effectiveness of non-invaziv positive pressure ventilation differs between decompaseted chronic restrictive and obstructive pulmonary disease patients. Intensive Care Med 29: 603-610.
-
El-Solh AA, Aquilina A, Pineda L, Dhanvantri V, Grant B, et al. (2006) Noninvasive ventilation for prevention of post-extubation respiratory failure in obese patients. Eur Respir J 28: 588-595.
-
Ambrosino N, Foglio K, Rubini F, Clini E, Nava S, et al. (1995) Non-invasive mechanical ventilation in acute respiratory failure due to chronic obstructive pulmonary disease: correlates for success. Thorax 50: 755-757.
-
Goligher E, Ferguson ND (2009) Mechanical ventilation: epidemiological insights into current practices. Curr Opin Crit Care 15: 44-51.
-
Ogden CL, Carroll MD, Curtin LR, McDowell MA, Tabak CJ, et al. (2006) Prevalence of overweight and obesity in the United States, 1999-2004. JAMA 295: 1549-1555.
-
Nowbar S, Burkart KM, Gonzales R, Fedorowicz A, Gozansky WS, et al. (2004) Obesity-associated hypoventilation in hospitalized patients: prevalence, effects, and outcome. Am J Med 116: 1-7.
-
Cuvelier A, Muir JF (2005) Acute and chronic respiratory failure in patients with obesity-hypoventilation syndrome: a new challenge for noninvasive ventilation. Chest 128: 483-485.
-
American Academy of Sleep Medicine Task Force (1999) Sleep-related breathing disorders in adults: recommendations for sydrome definition and measurement techniques in clinical researches. Sleep 22: 667-689.
-
Flenley DC (1985) Sleep in chronic obstructive lung disease. Clin Chest Med 6: 51-61
-
Pauwels RA, Buist AS, Calverley PM, Jenkins CR, Hurd SS; GOLD Scientific Committee (2001) Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease. NHLBI/WHO Global Initiative for Chronic Obstructive Lung Disease (GOLD) Workshop summary. Am J Respir Crit Care Med 163: 1256-1276.
-
Turkish Thoracic Society (2009) Consensus report on diagnosis and treatment of community-acquired pneumonia in adults. Toraks 10: 1-24.
-
Moock M, Mataloun SE1, Pandolfi M1, Coelho J2, Novo N1, et al. (2010) Impact of obesity on critical care treatment in adult patients. Rev Bras Ter Intensiva 22: 133-137.
-
Ray DE, Matchett SC, Baker K, Wasser T, Young MJ (2005) The effect of body mass index on patient outcomes in a medical ICU. Chest 127: 2125-2131.
-
Gursel G, Aydogdu M, Gulbas G, Ozkaya S, Tasyurek S, et al. (2011) The influence of severe obesity on non-invasive ventilation (NIV) strategies and responses in patients with acute hypercapnic respiratory failure attacks in the ICU. Minerva Anestesiol 77: 17-25.
-
Gultekin T, Ozer BK, Akin G, Bektas Y, Sagir M, et al. (2009) Prevalence of overweight and obesity in Turkish adults. Anthropol Anz 67: 205-212
-
Goulenok C, Monchi M, Chiche JD, Mira JP, Dhainaut JF, et al. (2004) Influence of overweight on ICU mortality: a prospective study. Chest 125: 1441-1445.
-
El-Solh A, Sikka P, Bozkanat E, Jaafar W, Davies J (2001) Morbid obesity in the medical ICU. Chest 120: 1989-1997.
-
Duarte AG, Justino E, Bigler T, Grady J (2007) Outcomes of morbidly obese patients requiring mechanical ventilation for acute respiratory failure. Crit Care Med 35: 732-737.
-
Garrouste-Orgeas M, Troch� G, Azoulay E, Caubel A, de Lassence A, et al. (2004) Body mass index. An additional prognostic factor in ICU patients. Intensive Care Med 30: 437-443.
-
Hogue CW Jr, Stearns JD, Colantuoni E, Robinson KA, Stierer T, et al. (2009) The impact of obesity on outcomes after critical illness: a meta-analysis. Intensive Care Med 35: 1152-1170.
-
Bhattacharya B, Prashant A, Vishwanath P, Suma MN, Nataraj B (2011) Prediction of outcome and prognosis of patients on mechanical ventilation using body mass index, SOFA score, C-Reactive protein, and serum albumin. Indian J Crit Care Med 15: 82-87.
-
Kaya A, Ciledag A, Cayli I, Onen ZP, Sen E, et al. (2010) Associated factors with non-invasive mechanical ventilation failure in acute hypercapnic respiratory failure. Tuberk Toraks 58: 128-134.
-
Akpinar S, Rollas K, Akpinar EE, Alagoz A, Ucar N, et al. (2013) Effect of the presence of pneumonia on noninvasive ventilation success in chronic obstructive pulmonary disease cases with acute hypercapnic respiratory failure. Turk J Med Sci 43: 373-378.
-
Budweiser S, Riedl SG, J�rres RA, Heinemann F, Pfeifer M (2007) Mortality and prognostic factors in patients with obesity-hypoventilation syndrome undergoing noninvasive ventilation. J Intern Med 261: 375-383.
-
Zvezdin B, Milutinov S, Kojicic M, Hadnadjev M, Hromis S, et al. (2009) A postmortem analysis of major causes of early death in patients hospitalized with COPD exacerbation. Chest 136: 376-380.
-
Rello J, Rodriguez A, Torres A, Roig J, Sole-Violan J, et al. (2006) Implications of COPD in patients admitted to the intensive care unit by community-acquired pneumonia. Eur Respir J 27: 1210-1216.
-
Akinnusi ME1, Pineda LA, El Solh AA (2008) Effect of obesity on intensive care morbidity and mortality: a meta-analysis. Crit Care Med 36: 151-158.
-
Mehta S, Hill NS (2001) Noninvasive ventilation. Am J Respir Crit Care Med 163: 540-577.
-
Esteban A, Frutos-Vivar F, Ferguson ND, Arabi Y, Apeztegu�a C, et al. (2004) Noninvasive positive-pressure ventilation for respiratory failure after extubation. N Engl J Med 350: 2452-2460.
-
Garpestad E, Brennan J, Hill NS (2007) Noninvasive ventilation for critical care. Chest 132: 711-720.
-
Lemyze M, Taufour P, Duhamel A, Temime J, Nigeon O, et al. (2014) Determinants of noninvasive ventilation success or failure in morbidly obese patients in acute respiratory failure. PLoS One 9: 97563.
-
Rabec C, Merati M, Baudouin N, Foucher P, Ulukavac T, et al. (1998) [Management of obesity and respiratory insufficiency. The value of dual-level pressure nasal ventilation]. Rev Mal Respir 15: 269-278.
-
Plant PK, Owen JL, Elliot MW (2000) Early use of non-invasive ventilation for acute exacerbations of chronic obstructive pulmonary disease on general respiratory words: a multicentre randomised controlled trial. Lancet 355:1931-1935.
-
Brochard L, Mancebo J, Wysocki M, Lofaso F, Conti G, et al. (1995) Noninvasive ventilation for acute exacerbations of chronic obstructive pulmonary disease. N Engl J Med 333: 817-822.
-
Mas A, Masip J (2014) Noninvasive ventilation in acute respiratory failure. Int J Chron Obstruct Pulmon Dis 9: 837-852.





