International Journal of Respiratory and Pulmonary Medicine
Unusual Case of Necrotizing Pneumonia
Rajapriya Manickam*, Kabir Oladipo Olaniran and Raghu Loganathan
Division of Pulmonary and Critical care Medicine, Lincoln Medical and Mental Health Center, USA
*Corresponding author: Rajapriya Manickam, Division of Pulmonary and Critical care Medicine, Lincoln Medical and Mental Health Center, Bronx, New York, USA, Tel: 917-375-5626; E-mail: rajee07@gmail.com
Int J Respir Pulm Med, IJRPM-2-019, (Volume 2, Issue 2), Case Report; ISSN: 2378-3516
Received: March 12, 2015 | Accepted: April 02, 2015 | Published: April 06, 2015
Citation: Manickam R, Olaniran KO, Loganathan R (2015) Unusual Case of Necrotizing Pneumonia. Int J Respir Pulm Med 2:019. 10.23937/2378-3516/1410019
Copyright: © 2015 Manickam R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Coccidioidomycosis is caused by inhalation of Coccidoides spores which is endemic in south western parts of USA and an uncommon cause of pneumonia in non-endemic areas. We report a young Hispanic man who lives in New York presenting with diabetic ketoacidosis and severe pulmonary Coccidioidomycosis. Through this case report and review we want to familiarize clinicians from non-endemic area to this unusual cause for necrotizing pneumonia, its association with diabetes mellitus, other risk factors for dissemination and the management strategy.
Introduction
Pulmonary Coccidioidomycosis is an uncommon cause of necrotizing pneumonia in non-endemic areas. We report a case of severe pulmonary Coccidioidomycosis in a young immigrant who lives in New York and discuss the association with diabetes mellitus.
Hospital Course
A young 32 year old Hispanic man presented with 4-weeks history of polyuria, polyphagia and weight loss and 2-weeks history of hemoptysis and shortness of breath. He denied fever, chills, night sweats, sick contacts, skin rash, glandular swelling or recent travel. He was a farmer who had emigrated from Mexico to New York City over a year ago and was currently working at a local grocery store. He denied any prior history of pulmonary symptoms. On examination the patient was cachectic, febrile, tachycardic and tachypneic and in respiratory distress. There were bronchial breath sounds in the right infraclavicular area. Laboratory investigations revealed mild leukocytosis and diabetic ketoacidosis (DKA). The chest X-ray (Figure 1) showed a dense right upper lobe infiltrate with bronchiectasis. A chest computed tomography (CT) (Figure 2) showed cavitary consolidation of the right upper lobe with patchy infiltrates in the right and left lower lobes.
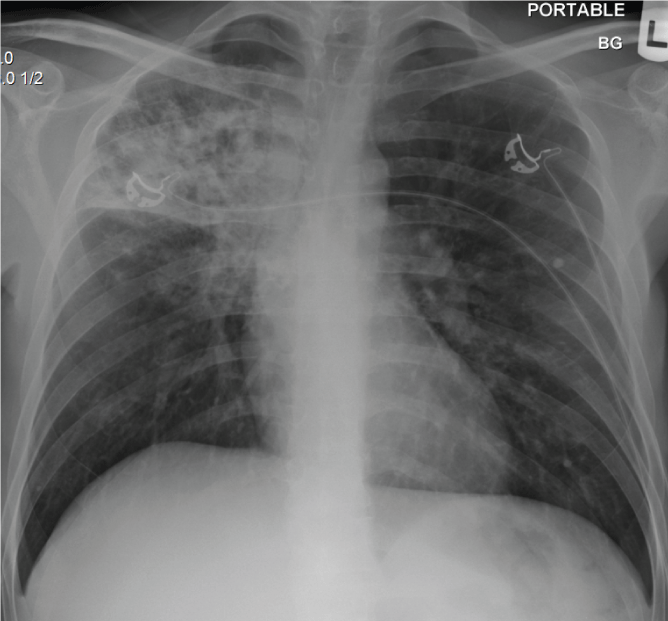
Figure 1: Chest radiograph showing right upper lobe consolidation and
retraction of horizntal fissure.
View Figure 1
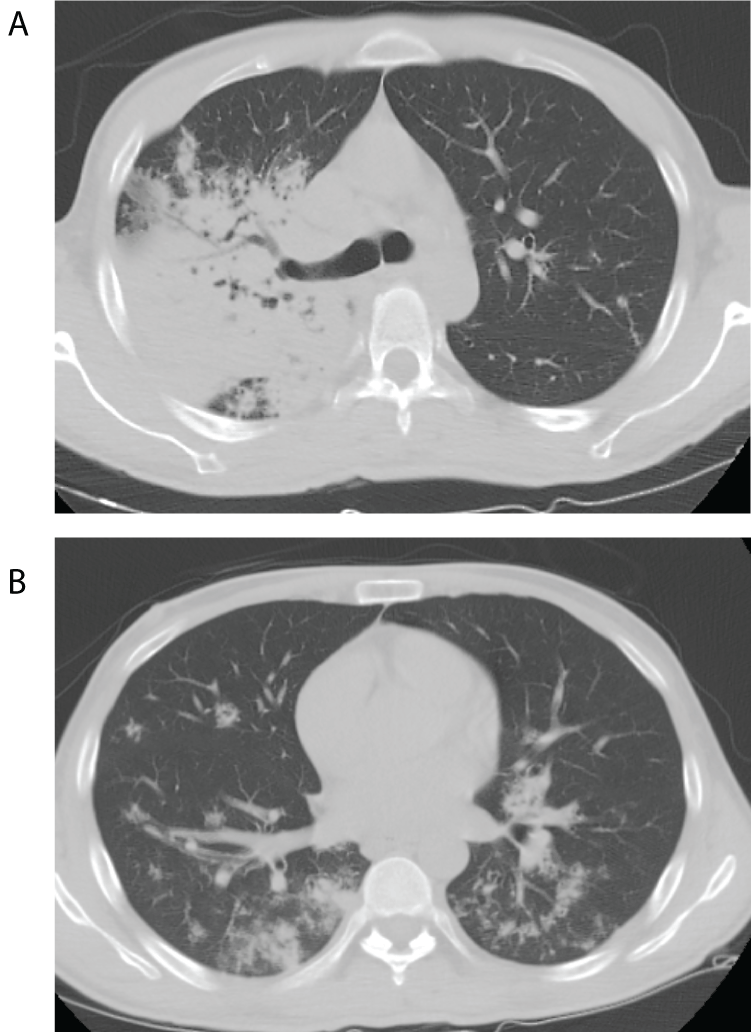
Figure 2: (A) Representative image of Chest CT showing dense consolidation
of the right upper lobe. (B) Represenattive image of Chest CT showing
bilateral patchy lower lobe infiltrates.
View Figure 2
The patient was treated for diabetic ketoacidosis and community-acquired pneumonia. Due to the location of the infiltrate, the patient was placed on airborne isolation while pulmonary tuberculosis was ruled out. All three sputum acid-fast bacillus (AFB) cultures and HIV serology were negative. The patient continued to have fever after nearly a week of IV antibiotics (ceftriazone and azithromycin) and developed drenching night sweats. Bronchoscopy with bronchoalveolar lavage (BAL) and transbronchial biopsy were done. No endobronchial lesions were appreciated; however there were copious mucoid secretions. BAL cultures, AFB and cytology were negative. Histopathologic examination with H&E stain showed ill-defined granulomas with encapsulated spherules (Figure 3) measuring 20-40�m in diameter diagnostic of pulmonary Coccidioidomycosis. Subsequently serum antibodies to Coccidioidomycosis were found to be positive. An elevated hemoglobin A1c of 16.4% was reported The patient was started on oral fluconazole and discharged home after clinical improvement. On outpatient follow up, a repeat chest CT showed resolution of pulmonary lesions.
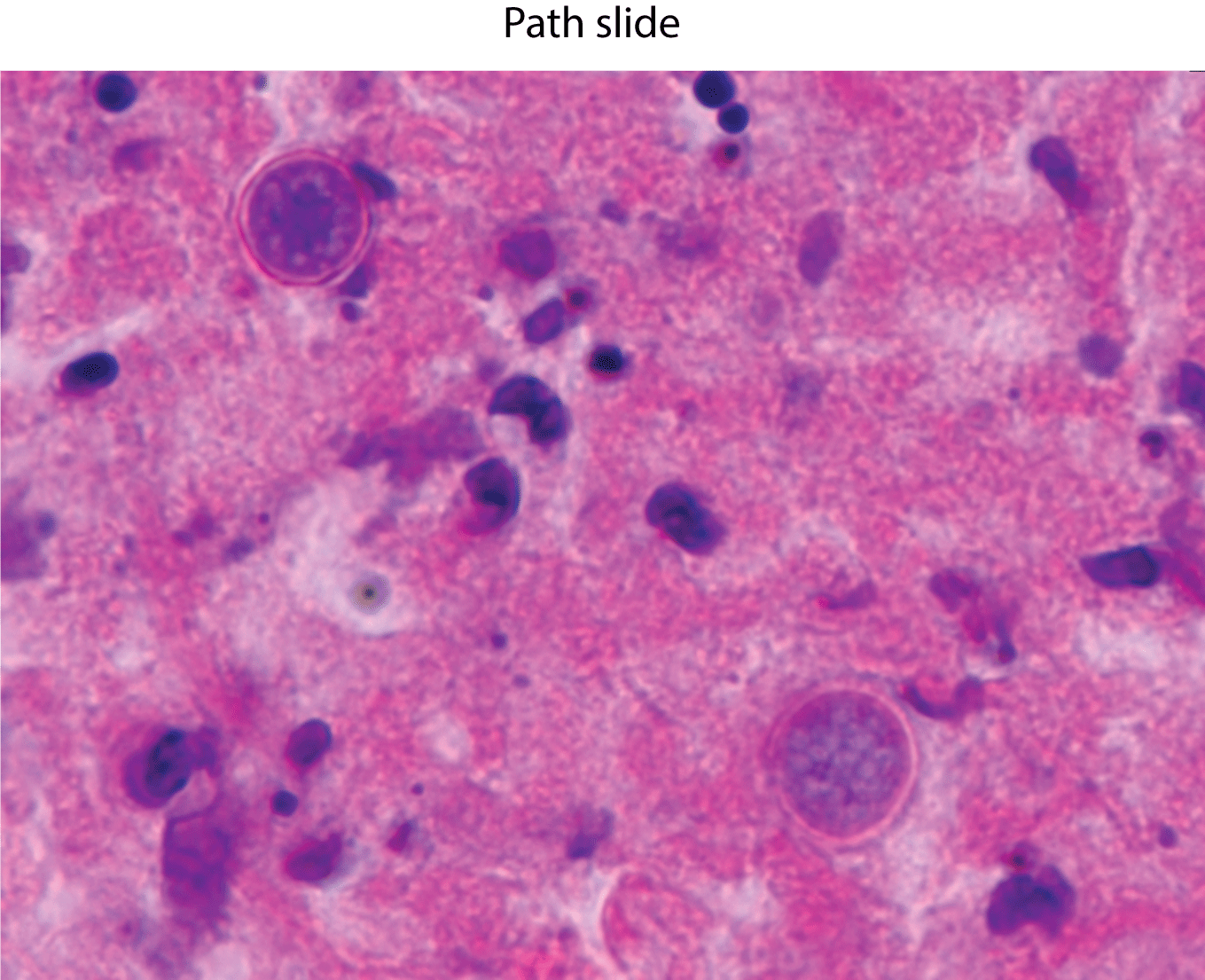
Figure 3: Histopathological examination of right lower lobe transbronchial
lung biopsy showing coccidioides immitis, presents as large thick walled
spherules containing numerous endospores.
View Figure 3
Discussion
Coccidioidomycosis (Valley fever) is caused by inhalation of Coccidioides spores - Coccidioides immitis typically in San Joaquin Valley of California and Coccidoides posadasii, typically outside of California [1]. It is a dimorphic soil dwelling fungus. Coccidoides immitis was first identified in 1892 in Argentina but its pulmonary manifestations and understanding of its mode of transmission was not clear until the 1940s [2]. We now know that Coccidioides found predominantly in the soil of warm, arid desert regions of the Western hemisphere located between the north and south 40� latitudes. This area encompasses California, Nevada, Utah, Arizona, parts of Texas, New Mexico and Mexico, where our patient emigrated from. Transmission is via inhalation of soil particles containing Coccidioides spores. Given his prior occupation as a farmer, it is reasonable to suggest that he has been carrying the fungus for a period of time prior to his presentation. However, coccidioidomycosis is typically a primary lung infection, not reactivation. After inhalation of Coccidioides spores, 60% of infected persons remain asymptomatic while the rest develop mild-to-severe pulmonary disease with only 1% developing disseminated disease [3].Risk factors for severe disease include African or Filipino descent, advanced age, T-cell immunosuppression from any cause including AIDS, pregnancy and diabetes mellitus.
The literature addressing the relationship of diabetes mellitus and coccidioidomycosis is sparse, but few reports suggest that diabetic patients are at increased risk of severe, progressive, and complicated coccidioidal infections and likely to have relapsing or cavitary disease than nondiabetics [4]. This is postulated to be related to decrease polymorphonuclear cell adherence, chemotaxis, phagocytosis and bactericidal activity. Westphal and Sarosi in 1994 [5] reviewed 3 cases of DKA associated with pulmonary coccidioidomycosis in an Arizona intensive care unit.
These were the only three associations over a 5 year period out of 66 DKA admissions. A more extensive retrospective study was performed by Santelli et al. in 2006 [6] where they looked at the effects of glycemic control on the course of Coccidioidomycosis. They found that despite treatment, cavitary pulmonary coccidioidomycosis was identified more often in diabetics than in nondiabetics. Additionally, coccidioidal infections in diabetics were more likely to relapse despite appropriate anti-fungal therapy. Disease severity (and therefore need to treat) appeared to correlate directly with hemoglobin A1c levels, as in our patient.
The non-specific presentation of coccidioidomycosis makes it difficult to diagnose and leads to an extensive workup for different conditions ranging from tuberculosis to malignancy and prolonged exposure to empiric antibiotic therapy, especially in non-endemic areas [7]. The diagnostic delay will allow for progression to more severe or disseminated disease [8]. Despite its varied presentation, the primary clinical manifestation of coccidioidomycosis is an acute respiratory infection virtually indistinguishable from community-acquired pneumonia [9]. Radiographic findings are typically lobar, segmental or subsegmental infiltrates with about 25% of cases involving hilar or paratracheal lymphadenopathy. However diffuse pneumonia, as diagnosed in our patient, which is characterized by involvement of all lung lobes, is uncommon except in immunocompromised patients. The criteria for establishing a diagnosis of coccidioidomycosis requires proven disease in a host with illness consistent with coccidioidomycosis and one of the following: (1) recovery in culture from a specimen obtained from the affected site or from blood; (2) histopathological or direct microscopic demonstration of the agent (Coccidioides spp. spherules ranging from 20-80�m on H&E staining or preferably on PAS or Gomori methanamine silver stains); (3) demonstration of coccidioidal antibody in CSF or a two dilution rise measured in two consecutive blood samples tested concurrently in the setting of an ongoing infectious process [10].
Most infected patients are asymptomatic or have self-limited respiratory illness and need only supportive care and periodic surveillance. Infectious Disease Society of America (IDSA) [11] recommends treatment with specific antifungals for symptomatic patients with risk factors for dissemination or extensive infection. The choice and duration of treatment with antifungals vary widely from patient to patient depending on their initial presentation and co-morbidities. Specific antifungals for treatment of coccidioidomycosis include amphotericin B, ketoconazole, fluconazole and itraconazole. In general, amphotericin B has been reserved only for severely ill, fulminant cases and pregnant women. Azoles have shown to be effective with good safety profile against Coccidioides and have become the first line of therapy in all other cases. Ketoconazole if the only FDA approved therapy for coccidioidomycosis, however newer less toxic fluconazole and itraconazole have replaced it. The efficacy of oral fluconazole and itraconazole for progressive, nonmeningeal coccidioidomycosis has been compared in a randomized double blind placebo controlled trial by mycoses study group [12]. Neither fluconazole nor itraconazole showed statistically superior efficacy in nonmeningeal coccidioidomycosis, however itraconazole has better response rate in skeletal infections. Fluconazole is the drug of choice for meningeal coccidioidomycosis. Newer antifungals posaconazole (a derivative of itraconazole) has been tried in refractory cases and been approved by European Commission as salvage therapy [13]. Combination therapy with amphotericin has been used in some refractory cases. Duration of therapy is controversial and again depending on the clinical course of the illness, but it should be at least 6 months in all patients and often a year or longer in others.
Coccidial infections pose a great challenge for transplant patients in endemic area. Patients with a history of recent coccidioidomycosis or positive serologic results at transplantation are recommended to receive fluconazole at 400 mg/day for life. Some programs propose universal prophylaxis with fluconazole of 6-12 months for primary prevention [14].
In our case, based on the clinical picture after the resolution of DKA, it was decided to start the patient on fluconazole 400 mg daily. Follow up clinical presentation in clinic and repeat chest CT confirmed overall resolution of pathology. Per recommendations, treatment will be continued for 6 months to one year.
Conclusion
In conclusion, we have presented an unusual case of bilateral necrotizing pneumonia due to coccidioidomycosis in a newly diagnosed uncontrolled diabetic patient occurring in a non-endemic area. From the literature, it is clear that concurrent uncontrolled diabetes is a risk factor for severe coccidioidomycosis. Clinicians should be aware of such delayed presentations of coccidioidomycosis in non-endemic areas; especially in immigrants from Mexico. High suspicion is key for prompt diagnosis. Antifungal treatment and tighter glucose control play an important role in preventing complications and reducing chance for relapse.
References
-
Fisher MC, Koenig GL, White TJ, Taylor JW (2002) Molecular and phenotypic description of Coccidioides posadasii sp. nov., previously recognized as the non-California population of Coccidioides immitis. Mycologia 94: 73-84.
-
Hirschmann JV (2007) The early history of coccidioidomycosis: 1892-1945. Clin Infect Dis 44: 1202-1207.
-
Brown J, Benedict K, Park BJ, Thompson GR 3rd (2013) Coccidioidomycosis: epidemiology. Clin Epidemiol 5: 185-197.
-
Joshi N, Caputo GM, Weitekamp MR, Karchmer AW (1999) Infections in patients with diabetes mellitus. N Engl J Med 341: 1906-1912.
-
Westphal SA, Sarosi GA (1994) Diabetic ketoacidosis associated with pulmonary coccidioidomycosis. Clin Infect Dis 18: 974-978.
-
Santelli AC, Blair JE, Roust LR (2006) Coccidioidomycosis in patients with diabetes mellitus. Am J Med 119: 964-969.
-
Galgiani JN (1999) Coccidioidomycosis: a regional disease of national importance. Rethinking approaches for control. Ann Intern Med 130: 293-300.
-
Chuang A, Thomas R, Hoffman RS (2005) Disseminated coccidioidomycosis in an immunocompetent person living in New York City. J Urban Health 82: 339-345.
-
Parish JM, Blair JE (2008) Coccidioidomycosis. Mayo Clin Proc 83: 343-348.
-
De Pauw B, Walsh TJ, Donnelly JP, Stevens DA, Edwards JE, et al. (2008) Revised definitions of invasive fungal disease from the European Organization for Research and Treatment of Cancer/Invasive Fungal Infections Cooperative Group and the National Institute of Allergy and Infectious Diseases Mycoses Study Group (EORTC/MSG) Consensus Group.Clin Infect Dis 46: 1813-1821.
-
Galgiani JN, Ampel NM, Blair JE, Catanzaro A, Johnson RH, et al. (2005) Coccidioidomycosis. Clin Infect Dis 41: 1217-1223.
-
Galgiani JN, Catanzaro A, Cloud GA, Johnson RH, Williams PL, et al. (2000) Comparison of oral fluconazole and itraconazole for progressive, nonmeningeal coccidioidomycosis. A randomized, double-blind trial. Mycoses Study Group. Ann Intern Med 133: 676-686.
-
Nagappan V, Deresinski S (2007) Reviews of anti-infective agents: posaconazole: a broad-spectrum triazole antifungal agent. Clin Infect Dis 45: 1610-1617.
-
Vucicevic D, Carey EJ, Blair JE (2011) Coccidioidomycosis in liver transplant recipients in an endemic area. Am J Transplant 11: 111-119.





