International Journal of Respiratory and Pulmonary Medicine
A Pain in the Neck: A Pott's Disease Case Study
Caitlin Naureckas1*, Jonathan Movson1,2 and E Jane Carter1,2
1Warren Alpert Medical School of Brown University, Providence, Rhode Island, USA
2The Miriam Hospital, Providence, Rhode Island, USA
*Corresponding author: Caitlin Naureckas, Warren Alpert Medical School of Brown University, 222 Richmond St. Box G-9999, Providence, Rhode Island-02912, USA, Tel: (401) 793-2500, Fax: (401) 793-4064, E-mail: Caitlin_naureckas@brown.edu
Int J Respir Pulm Med, IJRPM-2-030, (Volume 2, Issue 4), Case Report; ISSN: 2378-3516
Received: September 15, 2015 | Accepted: October 16, 2015 | Published: October 20, 2015
Citation: Naureckas C, Movson J, Carter EJ (2015) A Pain in the Neck: A Pott's Disease Case Study. Int J Respir Pulm Med 2:030. 10.23937/2378-3516/1410030
Copyright: © 2015 Naureckas C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
A 21-year-old Guatemalan male presented with six months of headaches and neck pain. MRI of the cervical spine demonstrated multiple inflammatory processes, both within the paraspinal soft tissue as well as within the bone itself, including the appearance of total destruction of C1. Microbiologic confirmation of Mycobacterium tuberculosis was made by fine needle aspiration. The patient was treated medically with appropriate anti-tuberculosis therapy coupled with aggressive pain control and careful neurological follow-up. Follow-up MRI at the end of treatment showed complete radiographic resolution. The patient had no neurologic sequelae. Indications for surgical intervention for management of Pott's disease (TB of the spine) are based on the presence of neurologic symptoms and/or the inability to manage pain, not on imaging alone. Aggressive pain management coupled with close neurologic follow-up and institution of appropriate TB treatment can often avoid surgical intervention, which generally involves the placement of hardware with resultant downstream management issues.
Keywords
Tuberculosis, Pott's disease, Medical management
Introduction
Tuberculosis (TB) of the spine, also known as Pott's disease, is the most common form of skeletal TB [1]. While the general consensus in the literature is that surgical stabilization should be reserved for patients with neurological sequelae or spinal instability [1,2] we have found that, in clinical practice, patients are often surgically treated. This is frequently due to either the initial (at times frightening) radiographic findings or severe pain, which is often not adequately managed in the context of rifampin drug interactions. We describe a case of advanced cervical spine tuberculosis in a young patient who was treated medically with appropriate anti-tuberculosis therapy and subsequently showed complete resolution of his skeletal findings on MRI.
Case Report
A 21-year-old male presented to the emergency room with severe neck pain and headache without any history of trauma. Symptoms had been present for six months and treated on an outpatient basis as migraine headaches. He denied fever, chills, cough, difficulty swallowing, leg or arm weakness, bowel or bladder incontinence, change in appetite, or other sites of pain. He did note night sweats and weight loss of over 20 pounds. He worked as a dishwasher with no occupational exposures. Born in Guatemala, he had been in the U.S. for two years. He denied exposure to tuberculosis in the past and had no history of any previous TB screening; he had received BCG vaccination during early childhood.
On physical exam, vital signs were normal with the exception of slight tachycardia. Neurological exam had no significant findings. Tenderness to palpation was noted in the posterior base of the neck. There was limited range of motion secondary to pain but no palpable swelling or mass. One BCG vaccination scar was noted on the upper arm.
Chest radiograph showed significant mediastinal lymphadenopathy, especially in the azygoesophageal recess. Lungs were clear except for mild post-obstructive pneumonitis associated with azygoesophageal recess adenopathy. Contrast enhanced MRI of the neck demonstrated a rim enhancing mass, consistent with an abscess in the pre-vertebral space centered at the C2/3 level. In addition, there was an inflammatory process extending from the C6 level to the skull base with extension through neural foramina into the spinal canal, with involvement of the clivus and the C1 and C2 vertebral bodies (Figure 1A). A separate similar appearing inflammatory process was present on the left side extending from the C4-C7 levels (Figure 1B). Right-sided cervical adenopathy was present. Within the posterior mediastinum there was a small abscess and surrounding inflammatory process adjacent to the T3 vertebral body (Figure 1C).
.
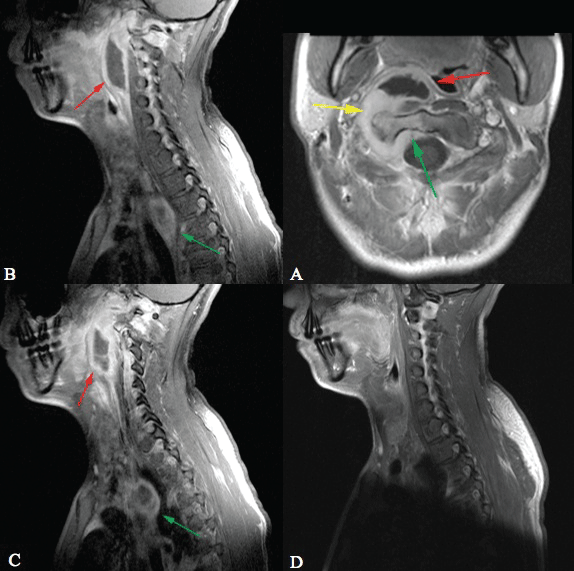
Figure A: Contrast enhanced axial TI weighted image demonstrates a pre-vertebral abscess (red arrow), enhancement and thickening of the peri-articular soft tissues surrounding the right C1/2 articulation (yellow arrow) and enhancement of the lateral mass of C2 (green arrow).
Figures B & C: Contrast enhanced, para-midline, sagittal T1 weighted images demonstrate an inflammatory processes in the right pre-vertebral space centered at the C2-3 disc space level (red arrow). There is a second similar appearing process centered at the T3 level in the posterior mediastinum (green arrow).
Figure D: Sagittal contrast enhanced T1 weighted image obtained post-therapy demonstrates complete resolution of the abscesses.
View Figure 1
Patient was admitted to the hospital where an ultrasound guided biopsy of the posterior neck mass was performed. Pathology demonstrated necrotizing granulomata, which were acid-fast bacilli (AFB) smear negative. Fiberoptic bronchoscopy was also performed with no demonstration of any endobronchial pathology; washings were also AFB smear-negative. Tuberculin skin testing was positive at 14 mm. Serum HIV testing was negative.
The patient was started on 4 daily anti-tuberculosis drugs (isonaizid [INH], rifampin, pyrazinamide, and ethambutol) under directly observed treatment (DOT) conditions, along with aggressive pain management. He was discharged to the local TB clinic.
Within two weeks Mycobacterium tuberculosis was cultured from his neck mass aspirate, sputa (expectorated), and bronchial washings. Drug susceptibility testing demonstrated that his organism was fully susceptible to all drugs.
Once his susceptibilities were known, his TB medications were adjusted accordingly with immediate discontinuation of ethambutol. After the first two months, his regimen was again switched, dropping pyrazinamide and retaining INH and rifampin three times per week for ten months. This regimen is consistent with CDC guidelines; in the U.S. individualized drug management is recommended. Images obtained at the end of treatment demonstrate complete resolution of the abscesses (Figure 1D).
Surgical decompression of the upper cervical abscess and stabilization with hardware had been considered early due to involvement of the skull base and the upper cervical vertebrae with the potential for bone destruction and spinal instability. Given his young age and lack of neurologic findings, it was elected to follow him carefully (at least twice per week with a careful neurologic examination) with the intent to operate if neurological compromise appeared.
Pain control was problematic during his first two months of treatment. This was likely exacerbated by the use of rifampin, which causes increased breakdown of narcotics via induction of cytochrome P450 in the liver [3]. Pain was eventually controlled with 100 micrograms of Duragesic patches every 72 hours coupled with 600 mg ibuprofen with each meal and PRN Percocet.
Discussion
Tuberculosis (TB) infection of the spine, also known as Pott's disease, represents approximately half of all cases of skeletal TB [4] but less than 1% of all TB cases [5]. Most common involved site is the mid thoracic vertebrae with involvement of the cervical spine much less common [6]. Due to its rarity in developed countries like the United States, this diagnosis can often be missed or delayed. Since a delay in diagnosis can lead to poorer outcomes, prompt recognition and treatment is essential [7,8].
Ideally, diagnosis of spinal TB is made by a combination of imaging, preferably MRI, and culture of Mycobacterium tuberculosis from biopsy samples [9,10]. A patient history of contact with an active TB patient or demonstration of TB infection via a positive purified protein derivative (PPD) skin test or Interferon-Gamma Release Assay (IGRA), are also supportive in arriving at the diagnosis [11]. Often the spinal lesions are accompanied by the presence of a large para-spinal abscess. The presence of such collections, often referred to as "cold abscesses," in the absence of fever, is very suggestive of TB [12-14].
Current literature supports medical treatment with four-drug therapy as first-line treatment for tuberculosis of the spine [1,15-17]. Given the risks of surgical intervention, it should be pursued only when necessary; indications include neurological sequelae, spinal instability, significant kyphosis, refractory pain, or failure of medical treatment [2,15,18,19]. In our experience, frightening radiographs have occasionally pushed early surgical intervention given the belief that stabilization is needed to avoid neurologic complications. We have also seen patients sent for surgical stabilization after minimal attempts at pain management. As our patient was young and without neurological symptoms, the hope was to avoid surgical stabilization with hardware, which, along with the risk of infection, would have reduced his range of motion and potentially decreased quality of life. Close neurological follow-up with appropriate TB medications and aggressive pain control allowed for successful medical management. Indications for surgery should not be solely based on imaging; one must instead look at the complete clinical picture. Rapid initiation of treatment coupled with aggressive pain management and close medical follow-up served to solve the problem of this pain in the neck without turning an acute problem into a chronic one.
References
-
Moon MS, Sung-Soo K, Hanlim M (2013) Tuberculosis of the spine: current views in diagnosis, management, and setting a global standard. Orthop Trauma 27: 185-194.
-
Jutte PC, Van Loenhout-Rooyackers JH (2006) Routine surgery in addition to chemotherapy for treating spinal tuberculosis. Cochrane Database Syst Rev 2006: CD004532.
-
Guengerich FP (1999) Cytochrome P-450 3A4: regulation and role in drug metabolism. Annu Rev Pharmacol Toxicol 39: 1-17.
-
Moon MS (1997) Tuberculosis of the spine. Controversies and a new challenge. Spine (Phila Pa 1976) 22: 1791-1797.
-
Turgut M (2001) Spinal tuberculosis (Pott's disease): its clinical presentation, surgical management, and outcome. A survey study on 694 patients. Neurosurg Rev 24: 8-13.
-
Rom W, Garay S (1996) Tuberculosis Boston: Little, Brown and Company.
-
Kamara E, Mehta S, Brust JC, Jain AK (2012) Effect of delayed diagnosis on severity of Pott's disease. Int Orthop 36: 245-254.
-
Nussbaum ES, Rockswold GL, Bergman TA, Erickson DL, Seljeskog EL (1995) Spinal tuberculosis: a diagnostic and management challenge. J Neurosurg 83: 243-247.
-
Cormican L, Hammal R, Messenger J, Milburn HJ (2006) Current difficulties in the diagnosis and management of spinal tuberculosis. Postgrad Med J 82: 46-51.
-
Desai SS (1994) Early diagnosis of spinal tuberculosis by MRI. J Bone Joint Surg Br 76: 863-869.
-
Ilgazli A, Boyaci H, Basyigit I, Yildiz F (2004) Extrapulmonary tuberculosis: clinical and epidemiologic spectrum of 636 cases. Arch Med Res 35: 435-441.
-
Jung NY, Jee WH, Ha KY, Park CK, Byun JY (2004) Discrimination of tuberculous spondylitis from pyogenic spondylitis on MRI. AJR Am J Roentgenol 182: 1405-1410.
-
Rivas-Garcia A, Sarria-Estrada S, Torrents-Odin C, Casas-Gomila L, Franquet E (2013) Imaging findings of Pott's disease. Eur Spine J 4: 567-578.
-
Pigrau-Serrallach C, Rodriguez-Pardo D (2013) Bone and joint tuberculosis. Eur Spine J 4:556-566.
-
Garg RK, Somvanshi DS (2011) Spinal tuberculosis: a review. J Spinal Cord Med 34: 440-454.
-
Kotil K, Alan MS, Bilge T (2007) Medical management of Pott disease in the thoracic and lumbar spine: a prospective clinical study. J Neurosurg Spine 6: 222-228.
-
Nene A, Bhojraj S (2005) Results of nonsurgical treatment of thoracic spinal tuberculosis in adults. Spine J 5: 79-84.
-
Dunn R, van der Horst A, Lippross S (2015) Tuberculosis of the spine--Prospective neurological and patient reported outcome study. Clin Neurol Neurosurg 133: 96-101.
-
Varatharajah S, Charles YP, Buy X, Walter A, Steib JP (2014) Update on the surgical management of Pott's disease. J Orthop Traumatol 100: 233-239.





