International Journal of Respiratory and Pulmonary Medicine
Relationship between Documented Confirmation of Endotracheal Tube Position and Mortality in the Emergency Department
Michael P Phelan1*, Jonathan M Glauser2, Fredric M Hustey1, Motunrayo Mobolaji-Lawal3 and Stephen W Meldon1
1Emergency Services Institute, Cleveland Clinic Health Systems, USA
2Metro Health Medical Center, Case Western Reserve University, USA
3Cleveland Clinic Lerner College of Medicine, USA
*Corresponding author: Michael P Phelan, MD, Emergency Services Institute, Cleveland Clinic Health Systems, 9500 Euclid Avenue, Cleveland OH 44195, USA, E-mail: PHELANM@ccf.org
Int J Respir Pulm Med, IJRPM-3-062, (Volume 3, Issue 4), Original Research Article; ISSN: 2378-3516
Received: March 09, 2016 | Accepted: November 19, 2016 | Published: November 21, 2016
Citation: Phelan MP, Glauser JM, Hustey FM, Mobolaji-Lawal M, Meldon SW (2016) Relationship between Documented Confrmation of Endotracheal Tube Position and Mortality in the Emergency Department. Int J Respir Pulm Med 3:062. 10.23937/2378-3516/1410062
Copyright: © 2016 Phelan MP, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective: To assess whether a multi-faceted intervention targeted toward improvement in emergency physician documentation rates of confirmation of endotracheal tube (ETT) position is associated with lower mortality rates in patients undergoing emergent endotracheal intubation.
Methods: We analyzed an emergency department (ED) performance improvement (PI) database from an airway registry that was developed to monitor the care of patients undergoing endotracheal intubation in prehospital settings or in the study site ED. PI initiatives included implementation of electronic health record (EHR) documentation templates for ETT placement/confirmation, an online educational module, and performance feedback. After a usual-care phase, quality improvement interventions were initiated. Mortality data from before and after the intervention were obtained from the EHR by trained reviewers using standardized data collection forms.
Results: Between 2006 and 2010, data for 961 patients were entered into the registry. Rates of documentation of appropriate methods of ETT position confirmation were higher after the intervention (557/758 [73.5%] vs. 122/198 [61.6%], RR 1.19; 95% CI, 1.06-1.34). Mortality rates improved throughout the intervention, with a trend toward a decrease in mortality after the intervention for the successive 3 years and an overall decline from 21.4% before to 18.1% in the 3 years following the intervention (P = 0.36).
Conclusion: Improvement in emergency physician documentation rates of ETT position confirmation was associated with a trend toward lower mortality rates, consistent with a trend identified in a previous analysis of survival in a national registry.
Keywords
Endotracheal intubation, Airway, Confirmation, Documentation, Mortality, Airway registry, Emergency department
Introduction
Management of the airway is the single most important intervention in the stabilization of critically ill patients in the emergency department (ED). It has been estimated that an average of 272 intubations are performed each year in an ED, based on a survey of 189 facilities. This number did not include patients arriving already intubated [1]. Airway management generally entails securing and maintaining an airway by use of an endotracheal tube (ETT). Failure to correctly place an ETT in the trachea and thus secure an airway can increase the risk of mortality and severe morbidity. The tube can become dislodged or placed in the esophagus or into a main stem bronchus. Misplacement of an ETT can result in inadequate ventilation, poor oxygenation, catastrophic clinical deterioration, and death [2]. Confirmation of correct ETT placement in the ED is an essential part of the care of patients undergoing intubation. Prompt recognition and repositioning of an incorrectly placed ETT can prevent potentially disastrous outcomes. Even when proper positioning of an initial airway has been documented in an outside facility, the tube can become dislodged bronchus during transport. Therefore, airway management and documentation become an ongoing process during a resuscitation [2]. The only way to reliably ensure accurate ETT placement is by using a specific verification method, followed by documentation in the medical record, i.e., secondary confirmation.
Patient safety in the ED begins with the airway. Thus, it is not surprising that numerous quality assessment studies have been conducted surrounding this critical clinical intervention. Much of the research on airway interventions in the ED has focused on specific medications and techniques best utilized to achieve expeditious endotracheal intubation. A decent proportion of the literature addresses intubation success after a given number of attempts, the need for a surgical airway, and variation of intubation success rates by specialty [3-5]. One report indicated that the need for multiple intubation attempts to secure an airway was independently associated with an increased incidence of adverse events, including cardiac arrest, dysrhythmia, hypotension, unrecognized esophageal intubation, hypoxemia, and main stem bronchus intubation [6]. More recently, investigators have considered the amount of practice needed for airway skill maintenance in pediatric emergency physicians [7] and rates of successful emergency intubation in children [8]. Clearly, this topic is of broad concern to those involved in emergency care in a variety of settings and for anyone concerned with quality assessment of a critical clinical intervention [9].
In addition to enhancing patient care and safety, appropriate documentation of ETT placement and confirmation of correct positioning is paramount for patient safety. Our understanding of verification of airway placement as a quality indicator and as a measure of patient safety is a relatively recent phenomenon, beginning within the past 15 years. In 2008, the National Quality Forum included documentation of ETT placement as an emergency medicine metric [10]. With regard to documentation of airways specifically, the field of emergency medicine has lagged behind the American Society of Anesthesiologists in applying basic standards for airway placement and monitoring [11]. ED airway registries have been created only recently. The National Emergency Airway Registry (NEAR) appeared in 1998 and 2000 and now holds records from more than 6000 cases [12,13].
We demonstrated previously that the quality of documentation of airway placement in the ED is inadequate, especially for patients who arrive to the ED already intubated [14]. Whether the process of airway documentation occurs reflects in part the increasing complexity of medical records. It is vital to verify that the patient actually has a secure airway; therefore, verification is an essential component of patient safety in the emergency setting.
We also previously demonstrated the success of a multifaceted quality improvement initiative in improving confirmation documentation rates [15]. Our quality improvement initiative included an implementation of ED EHR documentation templates for ETT placement/confirmation, an online educational module for emergency physicians (COMET), and continuous performance feedback.
The purpose of the current study was to evaluate whether the use of a multi-faceted intervention designed to improve emergency physicians' documentation rates of the confirmation of ETT position is associated with lower mortality rates in patients undergoing emergent endotracheal intubation. This analysis is a study of airway documentation as it relates to patient safety issues and whether education can influence this critical metric. In addition, this study will play a role in ensuring the field of emergency medicine advances to match the standards set by anesthesiologists in the critical area of airway documentation.
Methods
Setting and population
The setting for this observational cohort study was the ED of an urban tertiary care center with an annual census of approximately 60,000 patients and an affiliated emergency medicine residency program. All patients who arrived intubated (having been intubated in the prehospital setting or at the referring ED) or who underwent endotracheal intubation in the study site ED were included in our analysis. Cases in which alternative airway devices (e.g., King airway, LMA) were used were included only if the first device was changed to a standard ETT in the study site ED. Surgical airways (chronic tracheostomy patients) were excluded a priori from inclusion in the registry and therefore from this analysis.
Data collection
The initial airway registry, launched in 2006, was developed as part of a performance improvement project designed to monitor the care of ED patients following emergent ETT placement. The construction of this registry has been described previously [14,16]. Briefly, a standardized airway registry form (the Intubation Audit Form [Appendix]) was completed by the ED staff physician immediately after an intubation (or immediately after verification of proper ETT placement in the event that the tube was placed before the patient arrived in the ED). These forms were used to identify study patients and then medical records were reviewed using a standardized audit tool for documentation of confirmation of tube placement. Appropriate documentation of confirmation was defined according to recommendations from the American College of Emergency Physicians (ACEP), which cite three options for confirmation: end-tidal CO2 detection, re-evaluation with direct laryngoscopy, or use of an esophageal detection device [17].
Over a 12-month period in 2007, a series of quality improvement initiatives were implemented in an attempt to improve documentation of appropriate methods of ETT position confirmation. The construction and implementation of these initiatives have also been described previously [16]. Briefly, they included an ED electronic health record (EHR) airway documentation charting template, an online educational module for emergency physicians, and continuous performance feedback. The airway registry was queried for all patients in the usual-care (2006-2007) and intervention (2008-2010) phases. This patient information was then used to obtain mortality data via review of the EHR by trained reviewers using standardized data collection forms (Table 1). The 12-month implementation phase was not included in the mortality analysis.
![]()
Table 1: Characteristics of intubated emergency department patients.
View Table 1
Outcome measure
Mortality was defined as the death of an intubated patient in the ED.
Statistical analysisStatistical analysis was performed using SAS software (version 9, Cary, NC). Proportions with 95% confidence intervals and p values are reported. To examine the difference in mortality rate before the intervention and after the intervention, we used the chi-squared test. A P value less than 0.05 was considered statistically significant.
Results
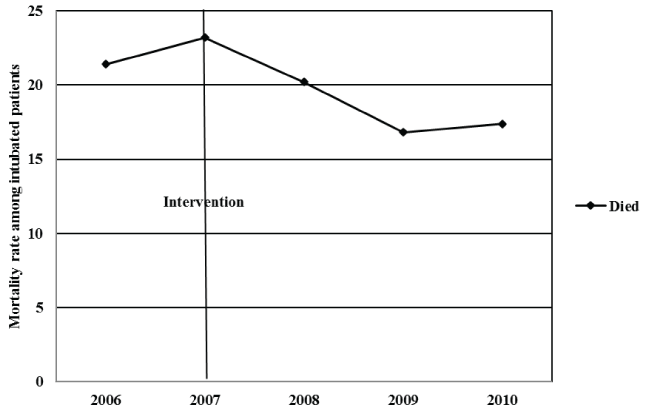
Between 2006 and 2010, data for 961 patients with ETT placement were entered into the registry: 201 patients prior to the quality improvement intervention, 207 patients during calendar year 2007 (the year of the quality improvement intervention), and 553 patients after the intervention. The rate of documentation of appropriate methods of ETT position confirmation was higher after the educational intervention (557/758 [73.5%] vs. 122/198 [61.6%], RR 1.19; 95% CI, 1.06-1.34) (P = 0.02). The mortality rate among intubated patients declined from 21.4% before the intervention to 18.1% (P = 0.36) after the intervention (Figure 1).
.
Figure 1: Mortality rate among intubated patients before and after introduction of quality improvement initiative.
View Figure 1
Discussion
The introduction of a multifaceted quality improvement program designed to improve appropriate documentation of ET tube location confirmation was associated with a decreased mortality rate among intubated ED patients. Unrecognized ETT misplacement can result in failure of oxygenation and ventilation, causing death or significant morbidity [18]. Miss rates for airway placement have been reported as 5.8% by Jones and associates [19], in the low single digits by Stewart and colleagues [20], and as high as 25% by Katz and Falk [21]. Further evidence that airway placement and confirmation constitute a patient safety concern comes from a secondary analysis of the Get with the Guidelines Resuscitation Database (GWTGR), which contains records from 75,777 patients in whom an ETT was placed [22]. That study demonstrated that patients whose ETT position was documented appropriately, as confirmed by capnography or an esophageal detection device, had a higher return of spontaneous circulation and survival to hospital discharge, with adjusted odds ratios of approximately 1.23 and 1.09, respectively, compared with those in whom this documentation was lacking [22]. To our knowledge, our current study is only the second one that supports the finding that improved documentation of confirmation is associated with a decrease in mortality rate. It is notable that most reports of airway placement in the emergency setting focus on complications of the procedure itself (e.g., hypoxia, bronchial intubation, arrhythmia) rather than documentation of tube position [23,24]. Al-Eissa and colleagues described a perception of success in core procedure performance, including endotracheal intubation, without mentioning verification of airway placement [25]. In this report, we address something more basic: whether documentary proof that tube position was confirmed is associated with decreased mortality rates among intubated ED patients.
Our study suggests a link between the quality of documentation of the ET tube confirmation process and the quality of the procedure itself. In terms of patient care, documentation of airway confirmation also provides a means of communication among providers across the spectrum of care and through patient handoffs. Incorrect ETT placement results in lack of oxygenation which, if not identified at every step, including handoffs, will lead to neurologic catastrophe and death. This is truly an issue of quality and safety. Emergency physicians are keenly aware of the critical nature of airway management. The ED should approach a zero-risk environment for airway management, including secondary confirmation of ETT placement as well as appropriate documentation of this confirmation.
Getting health care personnel to improve their rates of documentation is no simple task, even for a procedure as fundamental and life-saving as securing an airway. One report documented a multi-pronged effort to improve records related to five basic aspects of the airway: drugs and doses used, grade of view, size of ETT, confirmation of placement, and adverse events encountered. Even with the introduction of a structured educational program, documentation of this information improved only slightly [26]. There are likely multiple barriers to improving procedure documentation in emergent airway management. The burden of documentation can become a threat to successful implementation of a process. Questions as to where a form is located, who is designated to fill it out, and where it goes after completion can be perceived as onerous to health care providers in a chaotic environment [27]. The work environment in any ED, including physical layout, crowding, design of tools, staffing levels, culture of safety, and goal conflicts, are not necessarily conducive to documentation [28]. Airway management almost always occurs in an intense, sometimes chaotic, environment. Practitioners are likely to be more concerned with life-saving therapeutic interventions than with their documentation. As with other interventions, the emergent nature of many intubations in the ED along with lack of time for documentation will always represent a barrier to consistent and timely reporting. We hope that our findings reinforce the importance of documentation in the provision of patient care.
Limitations
This study took place at a single institution, a tertiary referral center that receives a disproportionate number of critically ill patients in transfer. As such, it is not a typical inpatient facility. A disproportionate share of transferred intubated patients might have had their airway secured by physicians at other hospitals rather than by paramedics.
The relationship between increased rates of documentation of ETT confirmation and mortality in the ED is one of correlation, not causation. We did not collect data on and therefore were unable to control for some additional factors that could have influenced the mortality rate before and after the performance improvement intervention. These include indications for the need for intubation, age, gender, body mass index, and other clinical parameters such as severity of illness or CPR in progress on arrival,
Conclusion
The implementation of a series of performance improvement initiatives, i.e., continuous performance feedback, an online education module for emergency physicians, and implementation of electronic medical record documentation templates for the ED, improved documentation of airway placement. This increase was associated with an overall decline in patient mortality over the study period. Lack of verification of ETT placement, coupled with a failure to document confirmation, poses a significant risk to patient safety and quality of care.
Acknowledgement
The manuscript was copyedited by Linda J. Kesselring, MS, and ELS.
Ethical Statement
Human subjects research
This study, based on an airway registry, was approved by the institutional review board at the medical facility with which the authors are affiliated. The board determined that this research involved no more than minimal risk and that the criteria for waiver of consent were satisfied.
Conflicts of Interest
The authors report no conflicts of interest or sources of funding for this study.
References
-
Smith DC, Smithline HA (1997) Intubation practice in US EDs (abstract). Ann Emerg Med 30: 401.
-
Gausche M, Lewis RJ, Stratton SJ, Haynes BE, Gunter CS, et al. (2000) Effect of out-of-hospital pediatric endotracheal intubation on survival and neurological outcome: a controlled clinical trial. JAMA 283: 783-790.
-
Levitan RM, Rosenblatt B, Meiner EM, Reilly PM, Hollander JE (2004) Alternating day emergency medicine and anesthesia resident responsibility for management of the trauma airway: a study of laryngoscopy performance and intubation success. Ann Emerg Med 43: 48-53.
-
Jaberi M, Mitchell K, MacKenzie C (2001) Cricothyrotomy: good, bad, or ugly? (abstract). TraumaCare 11: 13.
-
Bair AE, Filbin MR, Kulkarni RG, Walls RM (2002) The failed intubation attempt in the emergency department: analysis of prevalence, rescue techniques, and personnel. J Emerg Med 23: 131-140.
-
Hasegawa K, Shigemitsu K, Hagiwara Y, Chiba T, Watase H, et al. (2012) Association between repeated intubation attempts and adverse events in emergency departments: an analysis of a multicenter prospective observational study. Ann Emerg Med 60: 749-754.
-
Losek JD, Olson LR, Dobson JV, Glaeser PW (2008) Tracheal intubation practice and maintaining skill competency: survey of pediatric emergency department medical directors. Pediatr Emerg Care 24: 294-299.
-
Kerrey BT, Rinderknecht AS, Geis GL, Nigrovic LE, Mittiga MR (2012) Rapid sequence intubation for pediatric emergency patients: higher frequency of failed attempts and adverse effects found by video review. Ann Emerg Med 60: 251-259.
-
Green SM (2012) A is for airway: a pediatric emergency department challenge. Ann Emerg Med 60: 261-263.
-
National Quality Forum. National Voluntary Consensus Standards for Emergency Care.
-
American Society of Anesthesiologists. Standards for basic anesthetic monitoring.
-
Walls RM, Vissers RJ, Sagarin MJ (1998) 2392 emergency department intubations: first report of the ongoing national airway registry (NEAR 97) study. Acad Emerg Med 5: 393.
-
Walls RM, Gurr DE, Kulkarni RG (2000) 6294 emergency department intubations: second report of the ongoing National Emergency Airway Registry (NEAR) II Study. Ann Emerg Med 36: S51.
-
Phelan MP, Glauser J, Wickline D, Schrump S, Gaber-Patel K, et al. (2011) How well do emergency physicians document confirmation of endotracheal tube placement? Am J Med Qual 26: 300-307.
-
Phelan MP, Hustey FM, Glauser JM, Bena J (2015) A multifaceted quality improvement program improves endotracheal tube confirmation documentation in the emergency department. Am J Med Qual 30: 66-71.
-
Phelan MP, Glauser J, Yuen HW, Sturges-Smith E, Schrump SE (2010) Airway registry: a performance improvement surveillance project of emergency department airway management. Am J Med Qual 25: 346-350.
-
American College of Emergency Physicians. Practice resource: verification of endotracheal tube placement.
-
Henderson J (2010) Airway management in the adult. In: Miller RD, Eriksson LI, Fleisher LA, Wiener-Kronish JP, Young WL, Miller's Anesthesia. (7th edn), Philadelphia, Churchill Livingston: Elsevier; 1573.
-
Jones JH, Murphy MP, Dickson RL, Somerville GG, Brizendine EJ (2004) Emergency physician-verified out-of-hospital intubation: miss rates by paramedics. Acad Emerg Med 11: 707-709.
-
Stewart RD, Paris PM, Winter PM, Pelton GH, Cannon GM (1984) Field endotracheal intubation by paramedical personnel. Success rates and complications. Chest 85: 341-345.
-
Katz SH, Falk JL (2001) Misplaced endotracheal tubes by paramedics in an urban emergency medical services system. Ann Emerg Med 37: 32-37.
-
Phelan MP, Ornato JP, Peberdy MA, Hustey FM; American Heart Association's Get With The Guidelines-Resuscitation Investigators (2013) Appropriate documentation of confirmation of endotracheal tube position and relationship to patient outcome from in-hospital cardiac arrest. Resuscitation 84: 31-36.
-
Sakles JC, Laurin EG, Rantapaa AA, Panacek EA (1998) Airway management in the emergency department: a one-year study of 610 tracheal intubations. Ann Emerg Med 31: 325-332.
-
Tayal VS, Riggs RW, Marx JA, Tomaszewski CA, Schneider RE (1999) Rapid-sequence intubation at an emergency medicine residency: success rate and adverse events during a two-year period. Acad Emerg Med 6: 31-37.
-
Al-Eissa M, Chu S, Lynch T, Warren D, Seabrook JA, et al. (2008) Self-reported experience and competence in core procedures among Canadian pediatric emergency medicine fellowship trainees. CJEM 10: 533-538.
-
Winton J, Celenza A, Jackson T (2008) Improving documentation of endotracheal intubation in an adult emergency department. Emerg Med Australas 20: 488-493.
-
Schenkel SM (2012) Doing and documenting. Jt Comm J Qual Patient Saf 38: 513-514.
-
Pines JM, Kelly JJ, Meisl H, Augustine JJ, Broida RI, et al. (2012) Procedural safety in emergency care: a conceptual model and recommendations. Jt Comm J Qual Patient Saf 38: 516-526.





