International Journal of Surgery Research and Practice
Prospective Analysis and Technical Recommendations for Repair of Small Ventral/Umbilical Hernias Using the Ventralex Hernia Patch
Kejia Wang1 and Christophe R. Berney2*
1University of NSW, Australia
2Department of Surgery, University of NSW, Bankstown-Lidcombe Hospital, Australia
*Corresponding author: Christophe R Berney, Department of Surgery, University of NSW, Bankstown-Lidcombe Hospital, Eldridge Road, Bankstown-2200, Australia, Tel: +61403492428, E-mail: berneycr@hotmail.com
Int J Surg Res Pract, IJSRP-2-020, (Volume 2, Issue 1), Research Article; ISSN: 2378-3397
Received: February 10, 2015 | Accepted: March 10, 2015 | Published: March 12, 2015
Citation: Wang K, Berney CR (2015) Prospective Analysis and Technical Recommendations for Repair of Small Ventral/Umbilical Hernias Using the Ventralex Hernia Patch. Int J Surg Res Pract 2:020. 10.23937/2378-3397/1410020
Copyright: © 2015 Wang K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Mesh reinforcement of small ventral/umbilical hernias has become increasingly popular over the last decade. The Ventralex™ hernia patch has been evaluated for this purpose in a small number of studies with equivocal results, particularly in relation to post-operative hernia recurrence and mesh-related complications. The aim of this study was to examine the short- and long-term clinical outcomes of the technique, and to address the possible limiting factors.
Methods: Open mesh repair following strict surgical methodology was performed on 100 consecutive patients with small ventral/umbilical hernia defects of 1-3cm in diameter between April 2007 and December 2012. Short-term clinical outcome was obtained at 2- and 6-week post-operative visits, and long-term results were assessed by telephone interview with subsequent clinical review if judged necessary. Immediate post-operative complications, hernia recurrence, pain and Quality-of-Life (QoL) were also evaluated.
Results: There were no major short-term complications; minor complications including superficial wound infection and haemoserous wound discharge occurred in 9 patients (9%). The mean long-term follow-up was 37.9 months (range 6-75 months), with no hernia recurrences. No pain or mild pain was reported in 93.6% of patients, and 96.1% reported being satisfied or very satisfied with their repair.
Conclusion: This study demonstrates that open repair of small ventral/umbilical hernias using the Ventralex™ patch can be extremely safe and effective, with excellent long-term clinical outcome, when following a meticulous but easily reproducible surgical technique. Those main clinical steps include avoidance of large-sized patches, placing the mesh extraperitoneally (sublay) wherever possible, fixing the positioning straps with minimum tension, and always closing the abdominal fascia defect in front of the hernia patch.
Keywords
Mesh repair, Ventralex, Ventral hernia, Umbilical hernia, Composite patch
Introduction
Ventral hernias can occur anywhere in the anterior and lateral abdominal wall, most commonly at the umbilicus [1]. Although largely asymptomatic, the standard of care is surgical repair in order to avoid incarceration or bowel obstruction from strangulation. Recurrence rates of up to 50% with traditional suture-repair techniques [2,3] have led to the more frequent use of prosthetic meshes, especially in defects >3cm [4]. Over the last decade there has also been convincing evidence to recommend mesh reinforcement of smaller ventral hernias < 3cm in order to maintain low recurrence rates [4-6]. As such, the open underlay technique has been rapidly embraced by many surgeons as it is relatively non-invasive, can be easily and efficiently executed with minimal patient discomfort.
The Ventralex™ hernia patch (Bard�, Davol, Warwick, RI), introduced specifically for the surgical treatment of small ventral/umbilical hernias is a composite self-expanding and non-absorbable patch. It has a polypropylene (PP) side that remains in contact with the abdominal wall, encouraging tissue ingrowth and integration. The other side is made of expanded polytetrafluoroethylene (ePTFE) facing the intraperitoneal space, and providing a permanent barrier against adhesion formation. The main benefit of this technique is that fixation of the mesh is achieved principally by the intra-abdominal pressure that holds the prosthesis against the deep surface of the muscle, potentially improving tissue integration into the PP side of the mesh. Although short-term clinical outcome has been promising [7-9], the longer-term recurrence and complication rates have been equivocal in a small number of studies [9-12].
Perhaps the most relevant publication regarding the pathogenesis of mesh-related complication and recurrence is that by Berrevoet et al. [12]. In this unique study the authors controlled the final positioning of the patch using a laparoscope and found that in half of the cases the self-expanding ring of the mesh was inadequately deployed, thus allowing the PP material to come in contact with the viscera. They also observed a surprisingly higher than usual recurrent rate (14.8%) and their conclusion was that this could be related to a combination of material characteristics and technical errors [12]. In response, an author of our current study (C.R. Berney) wrote a �Letter to the Editor� [13] suggesting reasons for the limiting factors related to this new technique and making three recommendations: a) avoid using large-sized (8cm) patches intraperitoneally, b) do not fix the positioning straps with too much tension as it will increase the �cupping� effect of the mesh, thus creating more risk of adhesion formation onto the PP side of the patch, and c) aim for placement of the mesh in the retromuscular (or extraperitoneal) space rather than intraperitoneally [13]. Those comments were made at the time on the basis of non-peer-reviewed data. Consequently, the aim of our current cohort study was to evaluate the short and long-term clinical outcomes of the Ventralex™ patch using these recommendations. Long-term parameters included Quality-of-Life (QoL), chronic pain and hernia recurrence.
Materials and Methods
Data collection
Data was gathered prospectively from 100 consecutive elective patients with small ventral/umbilical hernias, with a defect size 1-3cm in diameter and repaired using an open underlay (or sublay) technique with the Ventralex™ patch from April 2007 to December 2012.
Surgical technique
All repairs were performed under the care of a single surgeon. Patients were given 1g of intravenous cephalothin preoperatively. Under general anaesthesia using mechanical ventilation by laryngeal mask airway and preferentially without myorelaxation, a small infraumbilical curvilinear skin incision was made. The hernia sac was dissected out, opened and excised if necessary after reduction of its contents. The prosthesis was pre-soaked in gentamicin, folded in half with the ePTFE side facing out (Figure 1), inserted through the defect and positioned either intraperitoneally (underlay) or preferably in the extraperitoneal space (sublay). A medium-sized (6.4cm) Ventralex™ mesh was preferentially deployed and the straps were secured onto the edges of the defect with 2-4 interrupted 2/0 ProleneTM (�Ethicon, Cincinnati, OH) or 2/0 Polydioxanone (PDS II, �Ethicon) sutures, ensuring they were not too tight to avoid a cupping effect of the mesh. The fascia defect was then approximated anteriorly using interrupted sutures of 1-PDS (Figure 2) and the umbilicus reattached to the fascia. The wound was closed in layers with absorbable subcuticular 3/0 CaprosynTM (Covidien, Mansfield, MA) to skin (Figure 2), Steri-stripsTM and a waterproof dressing to keep intact for 5 days. Patients were discharged home the same day on prophylactic oral cephalexin for 5 days and simple analgesia as required.
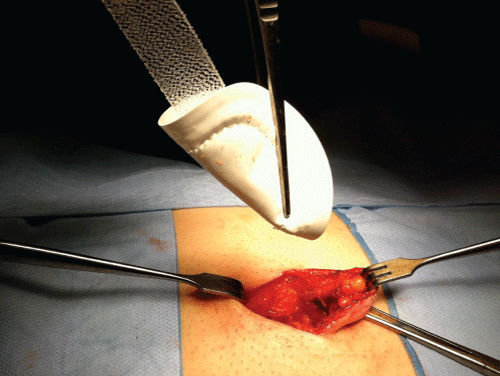
Figure 1: Ventralex™ mesh showing its ePTFE side
View Figure 1
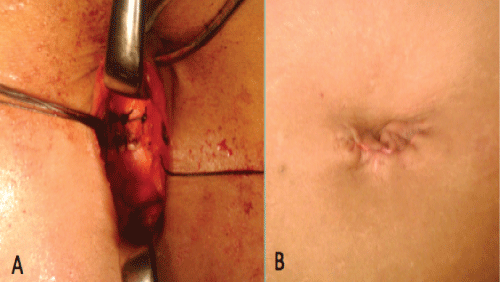
Figure 2: Closure of abdominal fascia with 1-PDS (A) and skin with subcuticular 3/0 Caprosyn (B) sutures
View Figure 2
Patient follow-up and evaluation of patient satisfaction
Following routine post-operative visits at weeks 2 and 6, patients had subsequent follow-up organized if deemed necessary. Finally, an attempt to contact all patients via telephone interview was made between June and July in 2013. Inquiries comprised any adverse event related to the procedure, including hernia recurrence and return of symptoms such as pain, discomfort or swelling. Chronic pain was assessed using the visual analogue score (VAS) and QoL using a comprehensive scoring system (Carolinas comfort scale [CCS]) (Table 1) specially designed for hernia repairs [14]. Patients dissatisfied with their long-term clinical outcome or concerned with potential hernia recurrence were offered a follow-up consultation with the operating surgeon. The data were analyzed using statistical tests for univariate categorical data (chi-square) where appropriate. Our local ethics committee approved the study.
![]()
Table 1: Carolinas Comfort Scale questionnaire (maximum: 115 points)
View Table 1
Results
There were 101 consecutive elective mesh repairs conducted in 100 patients with small ventral hernias, all of which were performed electively. All patient demographics, hernia and mesh characteristics as well as associated pathologies are summarized in Table 2. Out of the 101 Ventralex™ meshes implanted, the majority (80%) were 6.4cm in diameter. Following the publication from Berrevoet and colleagues in 2011 [12], only three large-sized meshes were used, of which 2 were inserted in the extra-peritoneal space. This also corresponded with a radical change of practice as from then on all the prostheses were preferentially inserted in the extraperitoneal space. As a result, during the last 20 months of the study a total of 23 of 37 patches were placed that way (23/37; 62.2%).
![]()
Table 2: Demographics, Clinical and Mesh Characteristics
View Table 2
Post-operative complications
Overall, minor 30-days post-operative complications were recorded in 9 patients (9%) (Table 3). There were 4 superficial wound infections that occurred despite 5 days of post-surgical prophylactic antibiotics, all successfully treated with supplemental oral antibiotic therapy. Three patients developed a transitory minor haemoserous discharge from the umbilical wound that spontaneously subsided with simple wound care and regular changing of dressings. Finally, one small superficial haematoma and one symptomatic seroma were both treated conservatively. There were no major early or late intraperitoneal, or mesh-related complications.
![]()
Table 3: Summary of the 10 post-operative complications observed over the
course of the study
View Table 3
Patient assessment of pain and satisfaction levels
Telephone contact was possible for 83 of the 100 surgical patients, but 5 of them were excluded from further analysis as they were unable to answer questions of the CCS survey we asked, mainly due to language barrier or time constraint issues. One patient seemed unhappy but was unwilling to discuss it further or return for a follow-up visit. The mean postoperative follow-up of the 78 remaining patients was 37.9 months (range 6-75 months). The results are summarized in Table 4. In total, 87.2% and 6.4% of the interviewed patients experienced either no pain or mild pain from their hernia repair, respectively. When looking at those complaining of moderate or severe pain, the mesh had been placed intraperitoneally (underlay) in 4 out of the 5 cases. Similar results were observed with regards to the satisfaction level assessment as 96.1% of the patients reported being satisfied or very satisfied with their hernia repair. Furthermore, the three patients who were either neutral or unsatisfied with their surgical treatment had an intraperitoneal prosthesis put in place.
![]()
Table 4: Analysis of postoperative pain score (VAS) and satisfaction levels
(CCS) in 78 patients post open underlay mesh repair of small ventral hernias
View Table 4
There was no statistical significance when correlating pain or satisfaction levels to the gender, hernia localisation, mesh size, or to those patients who underwent synchronous repair of associated pathologies. We did not encounter any cases of hernia recurrence. Out of five patients who reported residual swelling at the previous hernia repair site, one tested negative for hernia recurrence on abdominal ultrasonography following subsequent review in the surgeon�s rooms, while the remaining four patients did not come to the clinic for review.
Discussion
To date, eight relevant studies evaluating the Ventralex™ prosthesis have been published [7-12,15,16] and summarized in Table 5. Overall, mesh-related complications including deep infection requiring mesh removal or division of symptomatic intraperitoneal adhesions occurred in 13 of the total 606 repairs (2.1%). Comparatively, we encountered only 9 minor early complications unrelated to mesh implantation (Table 3). Furthermore, our rate of hernia recurrence was nil with a mean follow-up of 37.9 months. This compares well with previous studies with mean follow-up of over 24 months (range of 0-14.8%; Table 5).
![]()
Table 5: Table 5: Summary of all studies evaluating the Ventralex™ underlay patch repair of small ventral hernias
View Table 5
The high recurrence rate (14.8%) reported by Berrovoet et al. [12] was accompanied with findings of inadequate patch deployment and mesh �cupping� on laparascopic examination. Interestingly, Tinelli et al. [16] were also able to assess mesh placement laparascopically but reported no similar issues and a 0% recurrence rate. A significant difference between the studies is that the majority of meshes used by Berrovoet et al. were large-sized, whereas Tinelli and colleagues only employed small or medium-sized hernia patches. Likewise in our study the majority of patches used were medium-sized. We believe the large-sized prosthesis is more likely to create the �cupping� effect and non-uniform deployment, thus reducing tissue ingrowth onto the PP side of the mesh and soft tissue interposing between the patch and the abdominal wall. Undoubtedly, hernia recurrence is likely to increase with such outcome. Finally, the �cupping� effect may also become accentuated if the straps have been secured too tightly to the fascia [17-19].
We also think that a mesh overlap of 3-5cm, generally recommended for most laparoscopic incisional and ventral hernia repairs [20-22], is unnecessary for much smaller defects repaired open. Firstly, as these defects are small the pressure needed to force a mesh through the abdominal wall opening has to be in comparison much greater than for a larger defect treated laparoscopically. Secondly, rather than overlap, it is the ratio (R) of the prosthetic dimensions (P) to that of the wall defect surface area (D) that is important. For instance, a defect of 1cm in diameter (D:0.8cm2) does not require a mesh overlap of 5cm in each direction (P:95cm2, R:P/D=118.8) and conversely an incisional hernia with a defect of 5cm in diameter (D:19.6cm2) will be more likely to recur if the mesh overlap is only 1cm wide (P: 38.5 cm2, R:P/D=1.96). The good outcomes achieved by Tinelli et al. occurred despite using only small and medium-sized patches, even with 13.7% of their repairs being defects >3cm (Table 5).
Finally, in closing the fascia above the prosthesis the entire surface area of the patch will be in contact with the abdominal wall, thus significantly maximizing the amount of tissue ingrowth into the PP side of the mesh. This offers good evidence that a large-sized Ventralex™ patch should preferably not be inserted intraperitoneally, as previously recommended by others [13]. Although initially not suggested by the Bard� company, in this series we have systematically closed the fascia defect since April 2008 and following our eleventh patient. This should be routinely performed.
Of real concern is that in several studies [9,11,16] meshes were used for abdominal wall defects < 1cm in diameter, including large-sized Ventralex™ patches in >50% of cases in one series [9]. Trying to insert a mesh through such a small opening is likely to rupture its memory recoil ring, thus compromising the success of the repair as the patch will no longer lie flat against the abdominal wall. It is also impossible to obtain direct tactile feedback through such a small defect during mesh placement so proper deployment of the patch cannot be ensured. In our study we did not consider using reinforcement prosthesis for the repair of abdominal wall defects < 1cm in diameter.
In 22.8% of our cases, the mesh was placed in the extraperitoneal space (sublay) between the posterior rectus sheath and the peritoneum, a higher frequency than any previous study. This method is the gold standard for the open repair of large midline incisional hernias due to its low recurrence rates [23,24]. By placing the mesh in front of the peritoneum, exposure to the bowel and subsequent development of complications such as adhesions can be avoided. Some would argue that creating an extraperitoneal space increases the risk of complications, such as seroma formation, hematoma or superficial wound infection [15]. Our findings do not corroborate this statement as early complications only occurred in 1/23 (4.3%) of extraperitoneal mesh placements compared to 9/78 (11.5%) of intraperitoneal cases. Additionally, Berrovoet et al. [9] reported a 3.6% recurrence rate when a mesh was positioned in the extraperitoneal space, compared to 8.3% with intraperitoneal insertion.
Even though all of our patients were routinely discharged from hospital on prophylactic oral antibiotics, four of them (4%) developed superficial wound infection that was successfully treated with oral antibiotics (Table 3). Abdominal wall and mesh infection are known risk factors for early hernia recurrence and sometimes require prosthesis removal, especially when containing ePTFE [18]. Ventral and in particular umbilical hernia repairs are associated with a higher rate of infection of up to 20% [19]. Beside older age and comorbidities, wound infection may relate to skin devascularisation when creating the umbilical skin flap or as a consequence of normal umbilical bacterial colonisation. Therefore, we think that soaking the mesh in Gentamicin prior to its insertion and closing the anterior fascia at the end of the procedure will minimize the risk of developing deep wound and mesh infection, as well as the aforementioned risk of recurrence. Studies utilising other type of mesh have also found that fascia closure was associated with lower infection [25] and hernia recurrence [26] rates. Since completion of this study we have now replaced the original Ventralex™ hernia patch by a newer and theoretically safer version of the prosthesis in terms of infection, as the ePTFE side of the dual-mesh has been replaced by an absorbable hydrogel barrier based on the same technology used in Seprafilm� (Ventralex™ ST hernia patch, Bard�, Davol, Warwick, RI).
Following their surgery, 87.2% of our interviewed patients did not experience any residual pain, defined as a VAS score of 0/10. Furthermore, 96.1% of them reported being satisfied or very satisfied with their hernia repair as assessed by the CCS (Table 4). In comparison, Tollens et al. [11] mentioned a significant number of patients who experienced a painful sensation when wearing tight clothing (12%) and/or complaint of a foreign-body type sensation (5%). Iversen and colleagues [10] only reported �chronic pain� in 1.3%, but the calculated VAS scores were above 0/10 in many of their patients. Moreover, 17.9% of their patients indicated deterioration in their self-estimated general health. Many clinicians define chronic pain as a pain lasting for more than 3 months despite the fact that the injury has healed. This definition is too broad, unclear and makes it therefore difficult to objectively compare results arising from different studies. Thus, assessing QoL rather than a VAS pain score after surgery is ultimately more accurate and should be preferentially employed when comparing results.
As our follow-up data was obtained from a patient phone questionnaire rather than face-to-face clinical assessment, we acknowledge that this drawback may have led to inaccurate recording of hernia recurrences. However, if a recurrence was suspected at interview then patients were offered follow-up clinical visits and ultrasonography. We also agree that as 17 of our total patient�s cohort were not contactable (83% follow-up rate), our results should be interpreted with caution. In comparison however, Iversen et al. [10] were able to obtain 81.6% questionnaires after a mean follow-up of 15.6 months (personal mean follow-up: 37.9 months). In the Hadi et al. series [7] only 30 out of 51 patients had a planned follow-up at 12 months, and finally Tollens and colleagues [11] were able to organise a long-term follow-up (mean 49 months) examination in less than 60% of their cases.
Conclusion
In summary, we believe that the merits of our short- and long-term results directly relate to a meticulous repetition of easily reproducible surgical steps for the placement of the Ventralex™ mesh. In order for surgeons unfamiliar with this technique to achieve similar outcomes, there are several key points that should always be abided by: we recommend using this approach for small defects 1-3cm in diameter, avoiding using a large-sized patch, fixing the positioning straps with minimum tension, always closing the fascia defect and placing the mesh in the extraperitoneal space (sublay) wherever possible.
References
-
Aguirre DA, Santosa AC, Casola G, Sirlin CB (2005) Abdominal wall hernias: imaging features, complications, and diagnostic pitfalls at multi-detector row CT. Radiographics 25: 1501-1520.
-
George CD, Ellis H (1986) The results of incisional hernia repair: a twelve year review. Ann R Coll Surg Engl 68: 185-187.
-
Paul A, Korenkov M, Peters S, K�hler L, Fischer S, et al. (1998) Unacceptable results of the Mayo procedure for repair of abdominal incisional hernias. Eur J Surg 164: 361-367.
-
Schumacher OP, Peiper C, L�rken M, Schumpelick V (2003) [Long-term results after Spitzy's umbilical hernia repair]. Chirurg 74: 50-54.
-
Christoffersen MW, Helgstrand F, Rosenberg J, Kehlet H, Bisgaard T (2013) Lower reoperation rate for recurrence after mesh versus sutured elective repair in small umbilical and epigastric hernias. A nationwide register study. World J Surg 37: 2548-2552.
-
Arroyo A, Garc�a P, P�rez F, Andreu J, Candela F, et al. (2001) Randomized clinical trial comparing suture and mesh repair of umbilical hernia in adults. Br J Surg 88: 1321-1323.
-
Hadi HI, Maw A, Sarmah S, Kumar P (2006) Intraperitoneal tension-free repair of small midline ventral abdominal wall hernias with a Ventralex hernia patch: initial experience in 51 patients. Hernia 10: 409-413.
-
Martin DF, Williams RF, Mulrooney T, Voeller GR (2008) Ventralex mesh in umbilical/epigastric hernia repairs: clinical outcomes and complications. Hernia 12: 379-383.
-
Berrevoet F, D'Hont F, Rogiers X, Troisi R, de Hemptinne B (2011) Open intraperitoneal versus retromuscular mesh repair for umbilical hernias less than 3 cm diameter. Am J Surg 201: 85-90.
-
Iversen E, Lykke A, Hensler M, Jorgensen LN (2010) Abdominal wall hernia repair with a composite ePTFE/polypropylene mesh: clinical outcome and quality of life in 152 patients. Hernia 14: 555-560.
-
Tollens T, Den Hondt M, Devroe K, Terry C, Speybroeck S, et al. (2011) Retrospective analysis of umbilical, epigastric, and small incisional hernia repair using the VentralexTM hernia patch. Hernia 15: 531-540.
-
Berrevoet F, Van den Bossche B, de Baerdemaeker L, de Hemptinne B (2010) Laparoscopic evaluation shows deficiencies in memory ring deployment during small ventral hernia repair. World J Surg 34: 1710-1715.
-
Berney CR (2012) Re: Laparoscopic evaluation shows deficiencies in memory ring deployment during small ventral hernia repair. World J Surg 36: 1206.
-
Heniford BT, Walters AL, Lincourt AE, Novitsky YW, Hope WW, et al. (2008) Comparison of generic versus specific quality-of-life scales for mesh hernia repairs. J Am Coll Surg 206: 638-644.
-
Vychnevskaia K, Mucci-Hennekinne S, Casa C, Brachet D, Meunier K, et al. (2010) Intraperitoneal mesh repair of small ventral abdominal wall hernias with a Ventralex hernia patch. Dig Surg 27: 433-435.
-
Tinelli A, Malvasi A, Manca C, Alemanno G, Bettocchi S, et al. (2011) Post-laparoscopic mesh in post-menopausal umbilical hernia repair: a case series. Minim Invasive Ther Allied Technol 20: 290-295.
-
Burger JW, Luijendijk RW, Hop WC, Halm JA, Verdaasdonk EG, et al. (2004) Long-term follow-up of a randomized controlled trial of suture versus mesh repair of incisional hernia. Ann Surg 240: 578-583.
-
Stremitzer S, Bachleitner-Hofmann T, Gradl B, Gruenbeck M, Bachleitner-Hofmann B, et al. (2010) Mesh graft infection following abdominal hernia repair: risk factor evaluation and strategies of mesh graft preservation. A retrospective analysis of 476 operations. World J Surg 34:1702-1709.
-
Farrow B, Awad S, Berger DH, Albo D, Lee L, et al. (2008) More than 150 consecutive open umbilical hernia repairs in a major Veterans Administration Medical Center. Am J Surg 196: 647-651.
-
Bedi AP, Bhatti T, Amin A, Zuberi J (2007) Laparoscopic incisional and ventral hernia repair. J Minim Access Surg 3: 83-90.
-
Rives J, Lardennois B, Pire JC, Hibon J (1973) [Large incisional hernias. The importance of flail abdomen and of subsequent respiratory disorders]. Chirurgie 99: 547-563.
-
Stoppa RE (1989) The treatment of complicated groin and incisional hernias. World J Surg 13: 545-554.
-
Schumpelick V, Klinge U, Junge K, Stumpf M (2004) Incisional abdominal hernia: the open mesh repair. Langenbecks Arch Surg 389: 1-5.
-
Iqbal CW, Pham TH, Joseph A, Mai J, Thompson GB, et al. (2007) Long-term outcome of 254 complex incisional hernia repairs using the modified Rives-Stoppa technique. World J Surg 31: 2398-2404.
-
Petersen S, Henke G, Zimmermann L, Aumann G, Hellmich G, et al. (2004) Ventral rectus fascia closure on top of mesh hernia repair in the sublay technique. Plast Reconstr Surg 114: 1754-1760.
-
Booth JH, Garvey PB, Baumann DP, Selber JC, Nguyen AT, et al. (2013) Primary fascial closure with mesh reinforcement is superior to bridged mesh repair for abdominal wall reconstruction. J Am Coll Surg 217: 999-1009.





