Journal of Clinical Gastroenterology and Treatment
Buried Balloon: A Novel Complication from Percutaneous Radiologic Gastrostomy Tube Placement
Meghana Vellanki1*, Steve B Clayton2 and Patrick Brady1
1Department of Internal Medicine, Division of Digestive Diseases and Nutrition, University of South Florida Morsani College of Medicine, USA
2Department of Medicine, Division of Gastroenterology, University of South Carolina Greenville, USA
*Corresponding author:
Meghana Vellanki, Department of Internal Medicine, Division of Digestive Diseases and Nutrition, University of South Florida Morsani College of Medicine, 17 Davis Blvd. Suite 308, Tampa, FL 33606, USA, Tel: 407-334-4344, E-mail: Mvellank@health.usf.edu
J Clin Gastroenterol Treat, JCGT-1-007, (Volume 1, Issue 1), Case Series; ISSN: 2469-584X
Received: September 21, 2015 | Accepted: November 13, 2015 | Published: November 16, 2015
Citation: Vellanki M, Clayton SB, Brady P (2015) Buried Balloon: A Novel Complication from Percutaneous Radiologic Gastrostomy Tube Placement. J Clin Gastroenterol Treat 1:007. 10.23937/2469-584X/1510007
Copyright: © 2015 Vellanki M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Gastrostomy tube (G-tube) placement, once a staple of surgeons and gastroenterologists, has propagated into other fields of medicine with interventional radiology (IR) performing percutaneous radiologic gastrostomy (PRG). With more G-tubes being placed by IR, there have been novel complications associated with this technique. In the following case series, we describe one complication as a result of PRG tube placement by IR, called the "Buried Balloon". An analogous complication is the buried bumper syndrome which has been extensively described in gastroenterology (GI) literature. Currently, there is a paucity of data describing this complication.
Keywords
Buried bumper syndrome, Pull and push technique, Percutaneous endoscopic gastrostomy (PEG), Percutaneous radiologic gastrostomy (PRG)
Introduction
Percutaneous radiologic gastrostomies (PRG) are being placed with increasing frequency by Interventional Radiology. In the following case series, we describe an unreported complication due to PRG by IR, the buried balloon syndrome (BBS), analogous to the buried bumper syndrome described in the gastroenterology (GI) literature which occurs when the internal bumper of the G-tube erodes into the gastric wall.
In the "Pull" technique employed by GI, an incision is made, a puncture needle is inserted into the abdominal cavity, a wire is introduced and attached to the g-tube which is pulled in to position through the mouth under endoscopic guidance. Gastroenterologists use direct vision and resistance as an indication to determine the final position of the retention bumper.
In contrast, in the "Push" technique employed by IR, a similar incision is made on the abdominal wall and the wall of the stomach is anchored to the abdominal wall with T-fasteners. A series of dilators are then passed, the PRG tube is introduced, and anchored in place by inflating the balloon at the distal end.
During initial placement of PRG or PEG, there is a small amount of laxity on the bumper/balloon typically about 1-2 cm to prevent bumper/balloon erosion into the gastric wall. Further, standard care of G-tube requires insertion of the G-tube with 360 degree rotation.
Case 1
A 65 year old male with a PMH significant for chronic kidney disease, alcohol abuse, and oropharyngeal cancer had a PRG feeding tube placed by IR. Following PRG placement, the patient had several episodes of hematemesis, fever and abdominal pain, along with discharge around the G-tube site and was admitted for further management seven months later. During the hospital course, he had melenic stools (x6) along with pain, developed cellulitis at the PRG site, and tube feeds stopped infusing. He was empirically treated with antibiotics and underwent endoscopy.
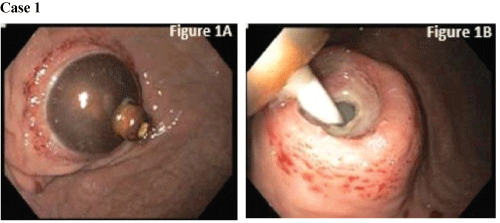
Endoscopy revealed a buried balloon within the gastric mucosa and he was further evaluated for possible removal. The G-tube balloon was buried into the abdominal wall with an underlying ulcer at the site of balloon impaction and purulent discharge underneath the balloon site (Figure 1A and Figure 1B). The balloon was deflated and manipulated free from the stomach wall. His G-tube was replaced and patient was able to resume feeds.
Case 2
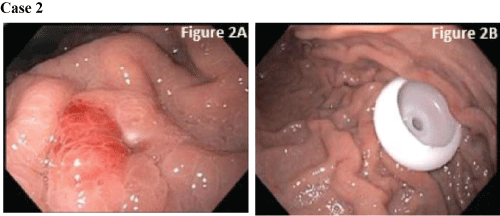
A 53 year old male with a PMH of Wernicke-Korsakoff syndrome, coronary artery disease, hypertension, and COPD was admitted for treatment of right toe gangrene, which led to a prolonged hospital stay. During his stay, the patient failed multiple swallow evaluations, and IR subsequently performed PRG. Placement was confirmed with contrast injection. One month later, there was concern for PRG infection and possible buried balloon as his nurse noticed discharge from PRG balloon insertion site. EGD was performed for further evaluation. The PRG balloon was not seen upon entry into stomach. There was an area of erythematous, edematous mucosa in the gastric body which appeared to be where previous PRG tube was placed (Figure 2A). A guide wire was passed through the existing PRG tube, was caught by a cold forceps, passed through the endoscope, and brought out through the mouth. The PRG tube balloon was deflated and the PRG was removed with external traction. Using the previously placed guide wire, a PEG tube was pulled through the abdominal wall. A satisfactory final position was confirmed endoscopically, and the PEG-tube was secured (Figure 2B).
Case 3
A 59 year old male with a PMH of ESLD from HCV, cirrhosis, mild renal insufficiency and primary laryngeal cancer underwent orthotopic liver transplant. His first PRG was placed post liver transplant day 11 as he required long term nutritional support. He was admitted three months later for elevated bilirubin of 12 mg/dL with a plan to do an ERCP for evaluation of intrahepatic ductal dilation. His PRG tube was in place at that time, but had not been used for tube feeds for 6 weeks. He complained of LUQ abdominal pain for the past two weeks along with two episodes of vomiting prior to admission. He continued to lose weight despite consuming "large amounts of food" and reported diarrhea since transplant. GI was consulted and EGD was performed.
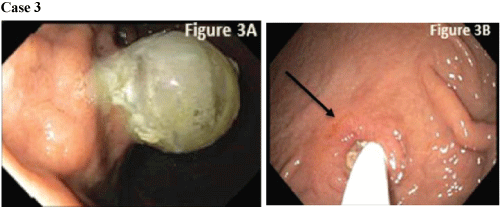
On this admission, EGD showed the balloon embedded in the gastric mucosa with underlying purulent discharge (Figure 3A). The mucosa was freed from the balloon using external pressure and internal pull that was provided endoscopically with a rat tooth forceps. The balloon was eventually freed and examination revealed an underlying ulcer in the G-tube tract (Figure 3B arrow). A balloon type G-tube replacement was successfully placed and patient was able to resume feeds.
.
Figure 3: (A) The balloon was embedded into the gastric mucosa. There was underlying purulent discharge in the stomach; (B) After the balloon was freed from the gastric wall, an ulcer was visible in the G-tube track.
View Figure 3
Discussion
The incidence of buried bumper is about 0.3-2.4% [1]. The incidence of BBS may be higher and the difference in placement technique could explain an increased rate of BBS. For example, the "pull" technique performed with endoscopy allows for direct visualization of the placement of the bumper, and how taut it is against the wall. PRG by IR uses a "push" technique, is performed with fluoroscopic guidance, and without direct visualization. The lack of direct visualization may contribute to a greater external tension being applied to the balloon and gastric wall ultimately resulting in erosion, ischemic necrosis and increased rates of BBS [2]. According to Cosentini et al. [3], both minor and major complications such as infection, bleeding, necrosis and peritonitis appear to be similar among the different techniques while Kohler et al. describe higher rate of complications, dislocations, and occlusions with the push-PEG technique [4].
The aim of this case series is to report a novel unreported complication associated with PRG. An explanation for the increased rate of "buried balloon" with PRG may be technique related. Further studies are needed to assess the complications associated with PRG and their causes.
References
-
Lynch CR, Fang JC (2004) Prevention and Management of Complications of Percutaneous Endoscopic Gastrostomy (PEG) Tubes. Pract Gastroenterol 22: 66-76.
-
Pop GH (2010) Buried Bumper Syndrome: can we prevent it? Pract Gastroenterol. 34: 8-13.
-
Cosentini EP, Sautner T, Gnant M, Winkelbauer F, Teleky B, et al. (1998) Outcomes of surgical, percutaneous endoscopic, and percutaneous radiologic gastrostomies. Arch Surg 133: 1076-1083.
-
Kohler G, Kalcher V, Koch OO, Luketina RR, Emmanuel K, et al. (2015) Comparison of 231 patients receiving either "pull-through" or "push" percutaneous endoscopic gastrostomy. Surg Endosc 29: 170-175.