Journal of Clinical Gastroenterology and Treatment
Giant Gastric Heterotopia in the Duodenum of an Adolescent Male and Review of the Literature
Laura El-Hage*, Vinay Sood and Cary Qualia
Albany Medical College, NY, USA
*Corresponding author:
Laura El-Hage, Albany Medical College, 47 New Scotland Avenue Albany, NY 12208, USA, Tel: (518)262-7500, Fax: (518)262-7505, E-mail: elhagel@mail.amc.edu
J Clin Gastroenterol Treat, JCGT-2-016, (Volume 2, Issue 1), Case Report; ISSN: 2469-584X
Received: November 08, 2015 | Accepted: February 09, 2016 | Published: February 12, 2016
Citation: El-Hage L, Sood V, Qualia C (2016) Giant Gastric Heterotopia in the Duodenum of an Adolescent Male and Review of the Literature. J Clin Gastroenterol Treat 2:016. 10.23937/2469-584X/1510016
Copyright: © 2016 El-Hage L, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Duodenal polyps are typically found during routine screening esophagogastroduodenoscopy for patients who have known hereditary polyposis syndromes. When polyps enlarge they may cause obstruction of the gastrointestinal tract, which is rare. We report an adolescent male without history of an underlying polyposis syndrome found to have multiple duodenal polyps comprised of gastric tissue during an upper endoscopy performed for vomiting. Differentiating between gastric heterotopia and gastric metaplasia is important, as heterotopia is typically benign, but metaplasia may be a sign of underlying Inflammatory Bowel Disease.
Case Presentation
A 12-year-old Caucasian male with a history of morbid obesity, hyperlipidemia, and episodic mood disorder presented with abdominal pain he had been experiencing for one year. He reported sharp pain predominantly in the epigastrium and occasionally in the right upper quadrant. The pain was exacerbated by eating spicy foods and large meals. Proton pump inhibitor therapy decreased the severity of his pain, but did not ameliorate this symptom. A few months prior to presentation, he developed non-bloody, non-bilious vomiting. The results of a complete blood count, basic metabolic panel, liver function tests, ESR, and CRP were within normal limits. The findings of an upper GI series and right upper quadrant ultrasound were normal as well.
.
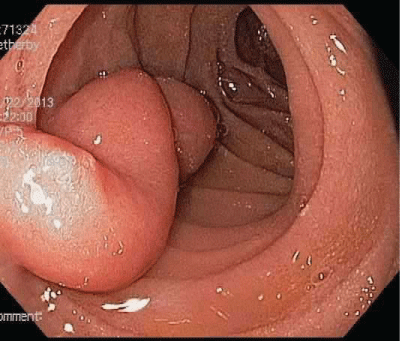
Figure 1: Endoscopic view of large polypoid lesion in the second portion of the duodenum, approximately 4 cm in length and 1 cm in width.
View Figure 1
An esophagogastroduodenoscopy revealed a large pedunculated polyp in the second portion of the duodenum, approximately 4 cm in length and 1 cm in width (Figure 1). This was removed in total. Two much smaller polyps (each approximately 2 mm in diameter) were also resected. One the smaller polyps can be seen in figure 2. Histologically, giant gastric heterotopia with reactive and hyperplastic changes (Figure 3), was seen in all biopsy specimens. A wireless capsule endoscopy study and colonoscopy were performed. No additional polyps or other mass lesions were identified. Since resection of the above lesions, the patient has been asymptomatic.
.
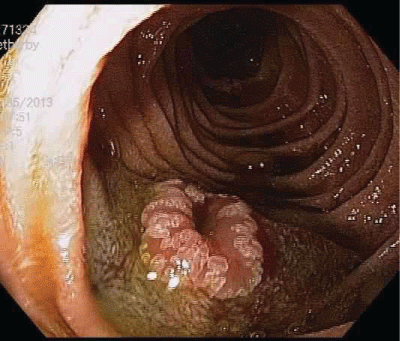
Figure 2: Endoscopic view of smaller polypoid lesion in the duodenum, following saline lift.
View Figure 2
.
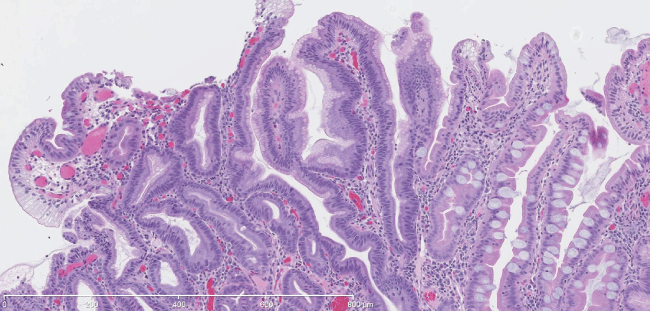
Figure 3: Duodenal biopsy. H&E stained section at 200x shows hyperplastic foveolar type gastric mucosa arising adjacent to villous type small intestinal mucosa.
View Figure 3
Discussion
Heterotopic tissue can be seen throughout the gastrointestinal tract. It is most commonly documented in the adult population. The true prevalence is likely higher than documented, since many individuals with heterotopic tissue are asymptomatic and thus undiagnosed. The tissue may be found incidentally during upper or lower endoscopy. Gastric heterotopia is a rare congenital lesion and is frequently associated with other congenital anomalies of the gastrointestinal tract, such as tracheoesophageal fistula, Meckel diverticulum, and digestive duplication [1]. The most common location of gastric heterotopia in children is within a Meckel diverticulum of the small intestine.
The distinction between gastric heterotopia and gastric metaplasia is based on both macroscopic and microscopic appearance of the intestinal mucosa. The initial differentiation begins on gross inspection. In a polypoid lesion, such as in our patient, the absence of endoscopic features of duodenitis including mucosal erythema, erosion, ulceration or loss of mucosal folds in the proximal duodenum favors heterotopia. Microscopically, the histologic findings favoring heterotopia include oxyntic mucosa and normal duodenal mucosa as opposed to gastric mucous cells in a background of chronic duodenitis. Dysplasia is strictly a histologic diagnosis which was absent on microscopic evaluation. It is a crucial distinction, since gastric metaplasia or dysplasia is acquired and can occur in patients who have Inflammatory Bowel Disease.
In contrast to our patient and as confirmed by Attard et al. most children who have duodenal polyps are asymptomatic [2]. Most have previously been diagnosed with polyposis syndromes and are found to have duodenal polyps while undergoing a screening or surveillance esophagogastroduodenoscopy. In polyposis syndromes, the most prevalent histologic subtypes of duodenal polyps are Brunner's gland hyperplastic polyps (33%), hamartomatous (17%), and heterotopic gastric gland polyps (8%) [2].
Our patient was distinct because he developed vomiting due to the transient obstruction caused by his large duodenal polyp. The blockage of the second portion of the duodenum caused him to have intermittent small bowel obstruction. Prior to vomiting he had abdominal pain, likely caused by mucosal irritation secondary to release of hydrochloric acid from the parietal cells located within the polyp. As the ectopic tissue grew in size, the symptoms of the patient reported herein evolved.
Clinical signs and symptoms of heterotopic gastric mucosa vary drastically and therefore complicate and delay diagnosis. As they did in our patient, symptoms may improve with the administration of proton pump inhibitors, presumably since this will decrease the secretion of erosive hydrochloric acid from the ectopic tissue. Although our patient had a large, obstructing polyp easily identifiable on endoscopy, some ectopic tissue is not grossly visible. Due to the difficulty of endoscopic diagnosis of non-polypoid lesions, a Technetium-99 m-pertechnetate scintigraphy study should be considered in any patient suspected of having undiagnosed ectopic gastric mucosa. Early diagnosis and appropriate treatment may alleviate long term risks, such as ulceration, perforation, and progression to metaplasia.
References
-
Ben Brahim E, Jouini R, Aboulkacem S, Jaouadi F, Labbene N, et al.(2011) Gastric heterotopia: clinical and histological study of 12 cases. Tunis Med 89: 935-939.
-
Attard TM, Abraham SC, Cuffari C (2003) The clinical spectrum of duodenal polyps in pediatrics. J Pediatr Gastroenterol Nutr 36: 116-119.





