Journal of Clinical Gastroenterology and Treatment
Coexistence of Acute Appendicitis and Perforated Meckel's Diverticulitis: A Rare Presentation in Older Adults
Rahman Senocak, Mehmet Ince, Sahin Kaymak, Zafer Kilbas and M Tahir Ozer*
Department of General Surgery, Gulhane Military Medical Academy, Turkey
*Corresponding author:
M. Tahir Ozer, Department of General Surgery, Gulhane Military Medical Academy, 06018, Turkey, Tel: + 90 312 304 5116, Fax: + 90 312 304 5007, E-mail: mtahirozer@gmail.com
J Clin Gastroenterol Treat, JCGT-2-017, (Volume 2, Issue 1), Case Report; ISSN: 2469-584X
Received: January 14, 2016 | Accepted: February 13, 2016 | Published: February 16, 2016
Citation: Senocak R, Ince M, Kaymak S, Kilbas Z, Ozer MT (2016) Coexistence of Acute Appendicitis and Perforated Meckel's Diverticulitis: A Rare Presentation in Older Adults. J Clin Gastroenterol Treat 2:017. 10.23937/2469-584X/1510017
Copyright: © 2016 Senocak R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
An appendectomy is one of the most commonly performed abdominal surgical procedures. During this operation, a Meckel's diverticulum (MD) can occasionally be found as an incidental finding, but the coexistence of both appendicitis and a perforated MD is fairly rare. Complications associated with an MD commonly occur in males, but the frequency of complications decreases with aging. Here, we present a rare case with a simultaneous coexistence of appendicitis and a perforated MD in an older patient. A 54-year-old man presented to the emergency department with a 24-hour history of gradually progressive abdominal pain. An abdominal ultrasound revealed free abdominal fluid in the lower abdomen, a non-compressible appendix that was 8.5 mm in diameter, and an increased wall thickness of the terminal ileum and caecum, suggesting perforated appendicitis. An exploratory laparotomy through a lower midline incision was performed. A typical appendectomy was performed and further abdominal exploration revealed an MD that was 3 cm in length with an inflamed and fibrinoid appearance located 60 cm proximal to the ileocecal valve and adhering to the pelvic peritoneum. A subsequent diverticulectomy was performed using a stapler. The patient had an uneventful recovery and was discharged on the sixth postoperative day. We recommend that searching for an MD should be done even when an acute appendicitis has been diagnosed. The reason for this is because these two conditions may exist simultaneously in patients of an advanced age and present with similar clinical features.
Keywords
Appendicitis, Meckel Diverticulum, Acute abdomen, Appendectomy
Abbreviation
MD: Meckel's Diverticulum
Introduction
A Meckel's diverticulum (MD) is the most prevalent congenital anomaly of the small intestine, occurring in 2-4% of the general population [1].In more than 90% of patients, it is located on the antimesenteric side of the ileum within 90 cm of the ileocecal valve [2]. Clinical presentations of MD are diverse and include abdominal pain, vomiting, jelly stool, and a palpable mass; however, the main clinical presentation is gastrointestinal bleeding in 25-50% of symptomatic MD patients. Other findings associated with MD are intestinal obstruction, intussusception, and diverticulitis [3]. On the other hand, an appendectomy is one of the most commonly performed abdominal surgeries. During this operation, MDs can occasionally be found as incidental findings, but the coexistence of appendicitis and a perforated MD is fairly rare. Here we present a rare case of a coexisting appendicitis and perforation of an MD in an older patient.
Case Report
A 54-year-old man presented to the emergency department with a 24-hour history of gradually progressive abdominal pain. He had no fever and no related gastrointestinal symptoms such as epigastralgia, nausea, and anorexia. He reported that his pain started in the middle of the abdomen and was then replaced by pain in the right lower quadrant, a classic presentation with acute appendicitis. The patient was hospitalized following a medical history, which was negative for previous operations and diseases. An abdominal examination showed some rigidity and moderate tenderness on palpation in the periumbilical area and bilateral lower quadrants. Laboratory findings included a white blood cell (WBC) count of 23.3 × 103/μl with 86.4% neutrophils and high-sensitivity C-reactive protein (CRP) levels of 161 mg/dl (0-3). An abdominal ultrasound demonstrated a moderate amount of free abdominal fluid (3 cm in thickness) in the lower abdomen, a non-compressible appendix that was 8.5 mm in diameter, and an increased wall thickness of the terminal ileum and caecum, suggesting perforated appendicitis. A computed tomography (CT) scan was not performed because it was thought that it would not change the management of the patient.
An exploratory laparotomy through a lower midline incision was performed. After a large amount of pus was observed in the peritoneal cavity and among the small bowel loops, a markedly swollen and inflamed appendix was observed. Considering the amount of purulent fluid, a further assessment was required. After checking both the large and small bowels, an MD that was 3 cm in length with an inflamed and fibrinoid appearance was found 60 cm proximal to the ileocecal valve and adhering to the pelvic peritoneum (Figure 1). After relieving the adhesions, fibrinous tissue that accounted for a microperforation on the antimesenteric side of the ileum was seen. First, an appendectomy was performed, which was followed by a diverticulectomy using a TA 60 linear stapler and irrigation. An examination of the rest of the abdominal organs revealed no abnormalities. After the surgery, broad-spectrum intravenous antibiotics were commenced and the patient had an uncomplicated recovery. The patient was discharged on the sixth postoperative day without morbidity.
The histological assessment reported the presence of suppurative inflammation, segmental serositis, and a microperforation for the MD, and lymphoid hyperplasia and fecalith for the appendix.
.
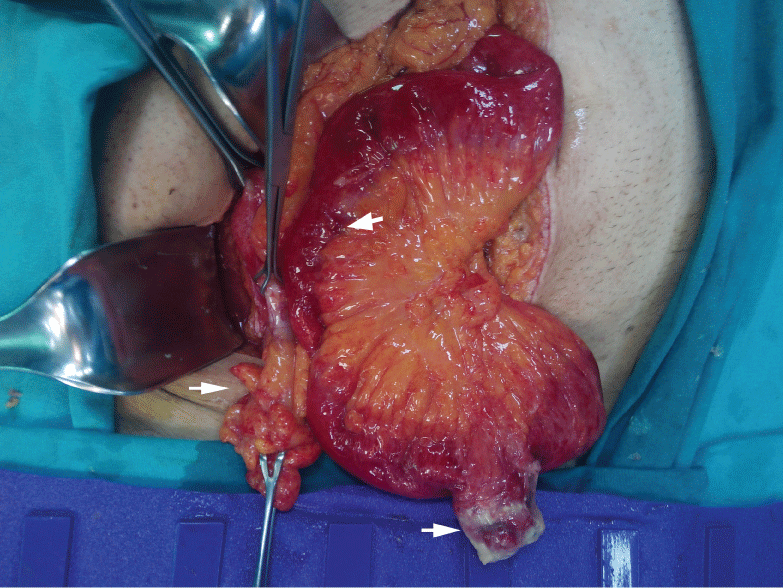
Figure 1: An intraoperative view of a swollen and inflamed appendix (left arrow), a perforated Meckel's diverticulum (approximately 3 cm in length) with distal inflammation and a fibrinoid appearance (right arrow), and an inflamed and edematous small bowel (upper white arrow).
View Figure 1
Discussion
When the omphalomesenteric duct has not completely obliterated during fetal life, MD occurs. It is the most prevalent congenital pathology of the gastrointestinal tract and is conventionally found in about 2% of the population. Although this condition is relatively common, complications can occur in 4-16% of cases, which include bowel obstruction, hemorrhage, diverticulitis, perforation, and intussusception [4]. The most common presenting symptom is obstruction, which occurs in nearly 40% of patients. Symptomatic MD commonly occurs in males, but the incidence of complications decreases with aging and the majority of complications occur in the pediatric ages. The second most common presentation is diverticulitis [5], and MD accounts for 10-20% of these complications but is seen more commonly in elderly patients [6].
Cullen et al. reported that the median age of patients with symptomatic diverticulum was 23 years (range: < 1 year to 82 years) [7]. Park et al. reported that the mean age of patients with a symptomatic MD was 27 years (31 ± 23.6 years) and that the frequency of symptomatic MD decreases with age in the adult population. The age of the oldest patient requiring an operation for symptomatic MD was 91 years [8]. McKay reported that the average age for symptomatic MD was 34.9 ± 23.2 years compared with 64.2 ± 16.5 years for asymptomatic patients [9]. The incidence of appendicitis peaked at 15 to 19 years for males, and subsequently, the incidence decreased gradually and reached a low point in the 55–59-year age group in both sexes [10]. Although the incidence of appendicitis and symptomatic MD decreased during the fifth decade, a coexistence of both diseases was found in the present case.
Meckel's diverticulitis and perforation of an MD usually present as acute appendicitis, except for the location of the pain [6]. Appendicitis is the most common preoperative diagnosis in cases of complicated MD. In the present case, the perforation of the MD produced limited peritonitis, but presumably it was thought that this was due to perforating appendicitis.
Radiologically, it can be difficult to diagnose an MD, especially if the diagnosis is initially not suspected. In the absence of bleeding, a preoperative diagnosis of symptomatic MD is difficult in the adult population. Fewer than 10% of symptomatic MD cases are diagnosed preoperatively [11].Ultrasound is performed mostly in non-specific abdominal pain; however, it has some limitations in diagnosing MD except for intussusception. Additionally, Groebli et al. reported that CT was able to diagnose MD in only one of 14 patients [12]. In this case, ultrasound was not diagnostically sufficient, probably because pelvic fluid was not specific to a perforation of the MD.
Presenting symptoms of a perforated MD are classically akin to symptoms of the perforation of other hollow viscera, including either localized or generalized peritonitis. Initial resuscitation and antibiotics after diverticulectomy or segmental resection with peritoneal drainage is the main treatment of choice for a perforated MD. For a long time, open laparotomic surgery has been employed as an efficient method to handle the complications of MD. A simple diverticulectomy is appropriate for MD with a narrow base. A segmental resection and anastomosis should also be considered in patients with inflammation in the nearby ileum [13]. In the present case, a simple diverticulectomy with a stapler was performed because of the associated peritonitis.
Cullen et al. reported that early postoperative morbidity was 12% and the mortality rate was 2% compared with a 1% mortality rate in patients after incidental diverticulectomies [7]. Park et al. reported that the postoperative complication rate was 13% and no deaths occurred [8]. Grobli et al. found two postoperative complications in the asymptomatic group (n = 52) and one in the symptomatic group (n = 67), but no deaths in either group [12]. Postoperative complications mainly include wound infections, a prolonged ileus, and anastomotic leaks. Early studies noted operative mortality rates in the range of 11-20% from MD complications; however, more recent reports suggest mortality rates of near 0%. In the current case, the coexistence of both diseases did not cause morbidity or mortality.
No specific physical signs or symptoms occur that make it possible to differentiate Meckel's diverticulitis from acute appendicitis. It is surprising that a perforation of an MD was diagnosed for this case, but it is not surprising that the clinical diagnosis of acute appendicitis was made. The literature suggests that an MD should be sought if the appendix is normal; however, if the appendix is overtly inflamed, the search for an MD is controversial. Some authors have suggested [14] that a search for an MD should be routine, while others [15] have emphasized that surrounding organs should be carefully explored, even though appendicitis has been diagnosed. We recommend that a search for an MD should be done even if acute appendicitis has been diagnosed since these two conditions may exist simultaneously in advanced ages and present with similar clinical findings.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest.
Consent
Informed consent was obtained from all patients for being included in the study.
Funding
The authors received no financial support for the research and/ or authorship of this article.
Contributors
MÍ and ZK was involved in the primary care of the patient; MIand SK were involved in the surgical management of the patient and provided the photographs; RS and MTO drafted the manuscript and critically reviewed and corrected the manuscript and will act as guarantor.
References
-
Sagar J, Kumar V, Shah DK (2006) Meckel's diverticulum: a systematic review. J R Soc Med 99: 501-505.
-
DiGiacomo JC, Cottone FJ (1993) Surgical treatment of Meckel's diverticulum. South Med J 86: 671-675.
-
Pantongrag-Brown L, Levine MS, Buetow PC, Buck JL, Elsayed AM (1996) Meckel's enteroliths: clinical, radiologic, and pathologic findings. AJR Am J Roentgenol 167: 1447-1450.
-
Vernon AH, Georgeson KE, Harmon CM (2004) Pediatric laparoscopic appendectomy for acute appendicitis. Surg Endosc 18: 75-79.
-
Yahchouchy EK, Marano AF, Etienne JC, Fingerhut AL (2001) Meckel's diverticulum. J Am Coll Surg 192: 658-662.
-
Matsagas MI, Fatouros M, Koulouras B, Giannoukas AD (1995) Incidence, complications, and management of Meckel's diverticulum. Arch Surg 130: 143-146.
-
Cullen JJ, Kelly KA, Moir CR, Hodge DO, Zinsmeister AR, et al. (1994) Surgical management of Meckel's diverticulum. An epidemiologic, population-based study. Ann Surg 220: 564-568.
-
Park JJ, Wolff BG, Tollefson MK, Walsh EE, Larson DR (2005) Meckel diverticulum: the Mayo Clinic experience with 1476 patients (1950-2002). Ann Surg 241: 529-533.
-
McKay R (2007) High incidence of symptomatic Meckel's diverticulum in patients less than fifty years of age: an indication for resection. Am Surg 73: 271-275.
-
Lin KB, Lai KR, Yang NP, Chan CL, Liu YH, et al. (2015) Epidemiology and socioeconomic features of appendicitis in Taiwan: a 12-year population-based study. World J Emerg Surg 10: 42.
-
Ymaguchi M, Takeuchi S, Awazu S (1978) Meckel's diverticulum. Investigation of 600 patients in Japanese literature. Am J Surg 136: 247-249.
-
Groebli Y, Bertin D, Morel P (2001) Meckel's diverticulum in adults: retrospective analysis of 119 cases and historical review. Eur J Surg 167: 518-524.
-
Varcoe RL, Wong SW, Taylor CF, Newstead GL (2004) Diverticulectomy is inadequate treatment for short Meckel's diverticulum with heterotopic mucosa. ANZ J Surg 74: 869-872.
-
Mischinger HJ, Berger A, Colombo T, Kronberger L (1989) Is the search for Meckel's diverticulum in appendectomy still a current problem in common surgical practice? Chirurg 60: 549-552.
-
Nordback I, Matikainen M (1985) Secondary appendicitis-a sign of some other intra-abdominal inflammation. Ann Chir Gynaecol 74: 134-136.





