Journal of Clinical Gastroenterology and Treatment
Abdominal Upper Gi Injury in 416 Polytraumatized Patients
Matthias Heuer1*, Björn Hussmann2, Rolf Lefering3, Gernot M Kaiser4, Sven Lendemans2 and TraumaRegister DGU5
1Department of General, Visceral and Vascular Surgery, Catholic Hospital of Essen, Germany
2Department of Trauma and Orthopedic Surgery, Alfried-Krupp Krankenhaus, Essen, Germany
3Institute for Research in Operative Medicine, University of Witten/Herdecke, Campus Cologne-Merheim, Cologne, Germany
4Department of General and Visceral Surgery, St. Bernhard Hospital, Kamp-Lintfort, Germany
5Committee on Emergency Medicine, Intensive Care and Trauma Management of the German Trauma Society, Sektion NIS, Germany
*Corresponding author:
Matthias Heuer, MD, PhD, Department of General, Visceral and Vascular Surgery Catholic Hospital of Essen, Hospitalstraße 24, 45329 Essen, Germany, Tel: +49 (201) 6400 2768, Fax: +49 (201) 6400 1752, E-mail: matthias.heuer@uk-essen.de
J Clin Gastroenterol Treat, JCGT-2-027, (Volume 2, Issue 2), Original Research; ISSN: 2469-584X
Received: February 15, 2016 | Accepted: May 27, 2016 | Published: May 29, 2016
Citation: Heuer M, Hussmann B, Lefering R, Kaiser GM, Lendemans S, et al. (2016) Abdominal Upper Gi Injury in 416 Polytraumatized Patients. J Clin Gastroenterol Treat 2:027. 10.23937/2469-584X/1510027
Copyright: © 2016 Heuer M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: The relevance of abdominal upper GI trauma in severely injured patients within a large collective has not been thoroughly analyzed yet. This study aims at assessing the prevalence of abdominal upper GI trauma in relation to the outcome and the currently established algorithm of treatment.
Methods: 148,498 patients from the TraumaRegister DGU® of the German Trauma Society (TR-DGU) (2002-2013) were analyzed retrospectively. All patients with an "Injury Severity Score" (ISS) ≥ 9, direct admission to a trauma center, age ≥ 16 and an abdominal injury (AISabdomen ≥ 2) were included. Patients with abdominal trauma (AISabdomen ≥ 2) were compared to patients with added abdominal upper GI trauma (AISabd. upper GI 2-4/5).
Results: 13,491 (19.7%) of 148,498 patients had documented abdominal injuries. 416 (3.1%) patients with abdominal injury additionally showed an abdominal upper GI injury (AISabdomen ≥ 2, AISabd. upper GI 2-4/5) and were analyzed in dependency of the classification of the American Association for the Surgery of Trauma (AAST) organ-severity score. AAST-abdominal upper GI (stomach and duodenum): II°: 1.1%, III°: 1.4%, IV°/V°: 0.6%. Patients with leading abdominal upper GI injury (grade IV and V) thereby showed a significant increase of mortality (IV°/V°: 16.2%).
Conclusions: The results presented here show the prevalence and the outcome of abdominal upper GI injury in a large collective within the TR DGU for the first time.
Keywords
Trauma, Abdominal upper GI injury, Mortality, Prognosis
Introduction
In multiple-injury patients, the stomach and duodenum are part of the injury pattern to varying degrees in around 0.5-2% of the documented cases [1]. In industrialized countries, abdominal injuries are mostly caused by a blunt accident mechanism [2]. And yet, the abdominal upper GI injury is frequently not directly life-threatening. In 30-40% of the cases, complications occur, which may lead to a significant reduction in quality of life, e.g. due to nutrition problems and/or in chronic post-traumatic/ -operative adhesions, particularly in young patients [3]. Due to the partly retroperitoneal position of the duodenum and its close proximity to large vessels, associated injuries are generally severe. Furthermore, with increasing severity of the abdominal upper GI injury, other organ systems are also involved so that more than 90% of the patients exhibit at least one other injured abdominal organ [4-6].
Since in-hospital mortality results from the cumulative impact of all injured organs, these impacts the increase in the total injury severity scores (ISS). The mortality rate after abdominal upper GI trauma documented in the literature accordingly has a wide range and varies between around 10 and 25%. A distinction is made here between early- stage mortality, mostly due to blood loss, and late-stage mortality [7]. Late-stage mortality is not infrequently based on secondary complications of the intensive care treatment, which may lead to sepsis as well as multiple organ failure in connection with the functional failure after trauma [8]. The actual specific significance of abdominal upper GI injury for the onset of such complications, however, is not yet fully understood in this context.
It must be noted, however, that a clear paradigm shift concerning the surgical treatment of abdominal injuries has occurred in the past few decades [9,10]. The conservative treatment of abdominal injuries has increasingly become the method of choice in hemodynamically stable patients after blunt trauma as a result of both the increasing multidisciplinarity and the corresponding interventional, mostly radiological but also more advanced conservative treatment options. Angioembolization may have success rates of up to 70-80% in various traumatic and on traumatic intra-abdominal hemorrhages; but this is not yet a standardized procedure in this context in Germany. In hollow organ injuries this interventional or conservative approaches play a subordinated role. However, there is also consensus that despite all non-surgical treatment options, hemodynamically unstable patients with relevant hemorrhages, more severe injuries or hollow organ injuries in general due to contamination should have surgery [11]. Here, the time of operation is determined by the acuteness of the events.
This study investigates the distribution and the significance of abdominal upper GI injuries in polytrauma patients.
Furthermore, it analyzes whether this injury constitutes an additional risk factor after trauma. A treatment algorithm based on this was derived accordingly.
Material and Methods
Between 2002 and 2013, a total of 148,498 patients were prospectively documented in the TR-DGU. The TraumaRegister DGU® of the German Trauma Society (Deutsche Gesellschaft für Unfallchirurgie, DGU) was founded in 1993. The aim of this multi-center database is an anonymous and standardized documentation of severely injured patients. Data are collected prospectively in four consecutive time phases from the site of the accident until discharge from hospital: A) Pre-hospital phase, B) Emergency room and initial surgery, C) Intensive care unit and D) Discharge. The documentation includes detailed information on demographics, injury pattern, comorbidities, preand in-hospital management, course on intensive care unit, relevant laboratory findings including data on transfusion and outcome of each individual. The inclusion criterion is admission to hospital via emergency room with subsequent ICU/ICM care or reaches the hospital with vital signs and dies before admission to ICU.
The infrastructure for documentation, data management, and data analysis is provided by AUC - Academy for Trauma Surgery (AUC - Akademie der Unfallchirurgie GmbH), a company affiliated to the German Trauma Society. The scientific leadership is provided by the Committee on Emergency Medicine, Intensive Care and Trauma Management (Sektion NIS) of the German Trauma Society. The participating hospitals submit their data anonymously into a central database via a web-based application. Scientific data analysis is approved according to a peer review procedure established by Sektion NIS. The participating hospitals are primarily located in Germany (90%), but a rising number of hospitals of other countries contribute data as well (at the moment from Austria, Belgium, China, Finland, Luxembourg, Slovenia, Switzerland, The Netherlands, and the United Arab Emirates). Currently, approx. 25,000 cases from more than 600 hospitals are entered into the database per year. Participation in Trauma Register DGU® is voluntary. For hospitals associated with TraumaNetzwerk DGU®, however, the entry of at least a basic data set is obligatory for reasons of quality assurance [12]. The present study is in line with the publication guidelines of the TraumaRegister DGU® and registered as TR-DGU project ID 2015-035.
In this analysis the following eligibility criteria were used:
1. "Injury Severity Score" (ISS) ≥ 9,
2. direct admission from scene to a trauma center and subsequent treatment for at least 3 days,
3. age ≥ 16,
4. abdominal injury (AISabdomen ≥ 2),
5. European data record.
ISS and the severity of individual injuries were determined with the 2005 edition of the "Abbreviated Injury Scale" (AIS). The existence of sepsis was defined based on the criteria of the ACCP/SCCM consensus conference committee [13]. The definition of organ failure (OF) followed the SOFA score (Sequential Organ Failure Assessment) [14]. An individual OF was defined by at least 3 SOFA score points; a multi-organ failure (MOF) was defined as simultaneous failure of at least two organs.
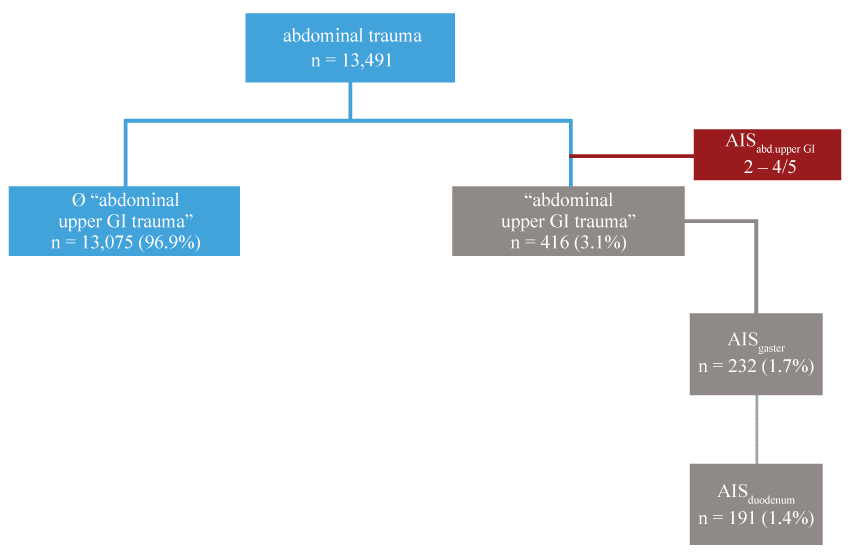
To represent abdominal upper GI injuries in their entirety, supposedly minor traumas, i.e. starting with AISabd. upper GI 2, were also taken into account in the data analysis, table 1. All those patients who had an abdominal injury (AISabdomen ≥ 2), but non abdominal upper GI injury (AISabd. upper GI = 0) were assigned to the "abdominal trauma" group. Patients with a documented abdominal upper GI injury (AISabd. upper GI 2-5) were placed in the "abdominal upper GI trauma" group and were analyzed according to the severity of injury, figure 1.
.
Figure 1: Organigram of the population; broken down into the respective grades of severity (AIS) in abdominal upper GI trauma; percentage calculation of abdominal trauma/abdominal upper GI trauma.
View Figure 1
![]()
Table 1: AAST-scale for classification of abdominal upper GI injuries [36].
View Table 1
In order to assess the risk of death based on the initial severity of injury, a prognosis was made using the Revised Injury Severity Classification, version 2 (RISC-2) [15]. The RISC-2 score has been developed and validated using data from more than 30,000 patients from the TR-DGU. Thirteen different factors which are present on hospital admission are used to estimate hospital outcome in primary admitted cases. Among the prediction variables are: orst and second worst injury, head injury, age, gender, type of injury, pupil size and reactivity, Glasgow Coma Scale, coagulopathy, blood pressure, base deficit, and hemoglobin level [16-18].
The actual observed hospital mortality is then compared with the estimated prognosis based on RISC-2. The relation of actual mortality and prognosis is expressed by the standardized mortality ratio (SMR) where the observed outcome is divided by the expected outcome (prognosis). Thus if SMR < 1 then outcome is better than expected. The statistical uncertainty involved in the SMR is demonstrated by using a 95% confidence interval (95%-CI).
Statistics
Since 2002, data collection was done with internet-based data entry software with integrated plausibility checks. The anonymized data were analyzed with the statistical program SPSS (Version 22, IMB Inc. Armonk NY, USA). Incidences are presented with counts and percentages, continuous values with mean and standard deviation (SD). Analysis was mainly restricted to descriptive statistics. Statistical tests were avoided due to the multiple number of comparisons (several groups and outcome parameters), as well as the high sample size which could lead to formal statistical significances in case of even minor differences. In selected situations only, data from the group with abdominal upper GI trauma were compared statistically against the remaining groups (χ2 test for incidence rates and U-test for continuous values).
Results
An abdominal trauma occurred in 13,491 (19.7%) of the patients. The further classification of the patients is shown in table 2 and figure 1. The incidence of an abdominal upper GI injury according to the stated criteria was a rare injury at 3.1% among the abdominal injuries.
![]()
Table 2: Demographic and clinical data after primary admission to a trauma center; as a function of the grade of severity of the abdominal upper GI injury.
View Table 2
The 416 patients with an abdominal upper GI injury had an average age of 41.4 ± 18.7 years; 72.4% were male, table 2. The average ISS was 30.5 ± 14.3 points. With regard to demographic parameters, moreover, it was shown that in contrast to patients with other abdominal injuries, e.g. liver and kidney, patients with abdominal upper GI trauma were on average older (kidney = 37.5 ± 17.4; liver = 34.9 ± 15.6) and averaged over both groups male (72.4 vs. 66.0%). At 93.3%, the number of blunt traumata was as expected in the "abdominal upper GI trauma" group.
Mortality
The overall mortality of AISabd. upper GI 4/5 injuries within the "abdominal upper GI trauma" group, at 22.1%, was increased in comparison to patients with AISabd. upper GI 3 injuries (17.5%) and the overall mortality in this group (17.4%), table 3. Patients with a score 2 abdominal upper GI injury showed a mortality of 14.5% (ISS: 28.4), in patients with a score 4/5 injury, the mortality increased to 22.1% (ISS: 37.0), table 2 and table 3. An investigation of early stage mortality (within the first 24 hours following primary care) at 16.2 showed that in AISabd. upper GI 4/5 injuries significantly more patients died within 24 hours than in the second and third group (6.9 and 8.1%, AISabd. upper GI 2 and 3). Restricted to primary admitted patients the expected mortality in the abdominal upper GI subgroup is 17.3% (RISC-2). Since the observed mortality is 17.4%.
![]()
Table 3: Representation of early-stage and overall hospital mortality related to the level of severity of the abdominal upper GI injury as and comparison of observed mortality and expected outcome according to the RISC-2 score. This table only contains primary admitted cases (no transfers).
View Table 3
Transfusion requirement
In the "abdominal upper GI trauma" group, in patients of various grades of injury severity, a transfusion requirement comparable to the normal population was established for all groups under consideration (0, 1-9 and ≥10 units of Erythrocyte Concentrate), table 2. In essence, the groups under consideration here appear unequally distributed. Only significantly higher use of transfusions was reported in patients with AISabd. upper GI 4/5 injuries (32.4 vs. 25.3%), blood packs 1-9, and AISabd. upper GI 4/5 injuries (20.6 vs. 12.9%), blood packs ≥ 10, in comparison to the average. The partly concomitant higher blood loss can also be seen in the blood pressure trend both preclinically and in the emergency room phase above all in the more severe injuries. In all groups, the overall blood pressure could only be raised slightly during initial clinical care (emergency room phase).
Surgical management
In table 4, the tendency to operate on patients with relevant abdominal upper GI injuries (AISabd. upper GI ≥ 2) is shown. In parallel with this, a declining trend in surgical care of abdominal upper GI injury patients is again noted over the stated periods, the mortality rate for these patients likewise declined steadily. As expected, mostly patients with severe abdominal upper GI injuries (AISabd. upper GI ≥ 3) had surgical treatment, table 4. When considering the surviving patients, a balanced length of stay in hospital or time spent on the respirator for both groups (moderate, AISabd. upper GI 2 and 3, and severe, AISabd. upper GI 4 and 5, abdominal upper GI injuries) was seen without dependency.
![]()
Table 4: Patients with abdominal upper GI injuries who had surgery. Furthermore, the hospital-specific length of stay or time spent on the respirator as a function of AISabd. upper GI is also shown for all patients.
View Table 4
Sepsis and organ failure
Patients with abdominal upper GI injury show an increased rate of sepsis in comparison to the control population, table 5. However, patients with a more severe abdominal upper GI injury also display an increased overall severity of the injury, table 2. Apart from patients with a moderate/severe abdominal upper GI injury (AIS 3 and 4/5, 16.6 and 19.7%), no relevant differences in the rate of sepsis were shown in dependence of the severity of the injury. Concerning the rate of multiple organ failures, patients with score 4/5 injuries show a difference compared to the control population and to patients with a less severe grade of abdominal upper GI injury (43.3 vs. 34.6%).
![]()
Table 5: Details of the incidence of MOF according to the above-mentioned classification as well as of sepsis as a function of AISabd. upper GI.
View Table 5
Discussion
If the abdominal upper GI organ (stomach and duodenum) is injured during a trauma, other associated organ injuries occur in the majority of cases. Besides the direct damage, organ-specific (e.g. infection, tumors and positional anomalies) and systematic pre-existing conditions (e.g. diabetes, hypertension und ischemic) also affect the prognosis of the abdominal upper GI tract and in the end the overall prognosis. The main focus here is primarily on stabilization of the entire organism. Maintenance of the abdominal upper GI function is hereby also critically affected by more severe injury. In addition, the incidences for organ and multiple organ failure and sepsis as well as in-hospital mortality rates are shown.
Currently, there is, even with sub-optimal availability of data - due to a lack of studies with high evidence -a homogeneous standard of care in the treatment of traumatically affected hollow organs. This is mainly reflected in the currently applied clinical routine. Thus, with free air and/or liquid proven in morphological imaging, the indication for exploration and primary care is provided generously [19,20]. The timing of surgery is initially guided by the overall condition of the patient and the local severity, however, should be immediately sought to avoid an increase in the rate of complications [21-23]. For larger lesions a resection debridement with subsequent continuity recovery must take place. In restricted blood flow a sparing resection is recommended, followed by a planned "second look" [24,25]. This approach, subject to the "Damage Control Surgery" implies that defects are simply closed by stapler without restoring continuity primarily. Time-consuming intestinal sutures and anastomoses, especially with high injury severity, are deliberately avoided in favor of a short duration of surgery.
In the results shown here, an increase in organ-specific severity of abdominal upper GI injuries correlates with an increase in mortality. This can be explained by the likewise increasing overall severity of patient injuries since the ISS with increasing AISabd. upper GI has consecutively increased [26]. An expected, increasing number of massive transfusion patients was also seen in the groups with severe abdominal upper GI trauma. To what extent these poor prognosis cases specifically correlate with the abdominal upper GI injuries remains speculative since the transfusion of erythrocyte concentrates already leads to an increase in post-traumatic organ failure and to a deterioration in outcome in general [27,28]. Here, the preclinical data support the connection between the grades of abdominal upper GI injuries, the overall ISS and the rate of preclinical hypo-perfusion (RR blood pressure < 90 mmHg). However, as opposed to liver injury, abdominal upper GI injuries do not appear to constitute an additional risk factor here.
The operation rate initially increased, as expected, with increasing severity of injury. Interestingly, 89.9% of degree IV/V injuries are operated. However, this can be explained by the high mortality rate after 24 hours (22.1%), as the data suggest that many patients do not reach the time of surgery. Likewise risky for the further clinical outcome is the development of sepsis and/or septic abdomen. In the analogy of the trauma in this case the risk increases disproportionately [29]. In general it can be said that the mortality related to local peritonitis alone ranges at about 14% and may increase to up to 42% in the formation of a 4-quadrant peritonitis [30,31]. Nevertheless, large center studies have shown that the post-traumatic abdominal infection with only 9% takes 5th place of the infection complications [32]. This trend is also confirmed by our results, which showed largely independent high sepsis rates of about 17-19%, compared with the severity of the injury.
The question of clear criteria leading to the temporal procedure after abdominal and hollow organ trauma is not clearly answered by the current literature. However, it seems clear that hollow organ injuries must be treated surgically not necessarily for hemodynamic reasons, e.g. following bleeding, but rather for the sake of following contamination. However, criteria referring to the term "unstable" often used in current literature are not consistent.
Obligatory, also in this case, it should be responded to bleedings that have arisen in connection with hollow organ injuries. Not only in this context Clarke et al. could show that the mortality after trauma in the context of a bleeding shock increases every 3 minutes by 1%, so that the time from arrival in the emergency room to laparotomy is crucial for the prognosis [33,34]. Here, the cause of abdominal bleeding is of minor importance. More important is the type of care that is based on the criteria of "Damage Control Surgery" which are e.g. part of the class "Definitive Surgical Trauma Care" (DSTC) sponsored by the DGU. In our opinion, unstable patients should be identified by the following criteria: 1. Free fluid in the abdomen in the initial emergency room ultrasound, if applicable with an increase in the process, 2. loss of volume, i.e., necessity of substitution for stabilization of the circulation with a drop in systolic blood pressure ≤ 90 mmHg and 3. Signs of systemic perfusion deficiency with negative base excess and pH and possibly with an initial hemoglobin < 8 mg/dl with signs of consumption coagulopathy. The knowledge of the additional risks documented here, as they may arise from hollow organ injuries, may be influenced positively by a specific coagulation therapy and early substitution of EK.
Conclusion
For the first time, the results shown here indicate the prevalence and the outcome of abdominal upper GI injuries in a large population which was generated from the data of the TraumaRegister DGU®. The results prove that isolated abdominal upper GI injuries constitute a rare occurrence and thus can only be investigated through a multicenter study or through an evaluation of the register with the corresponding numbers of cases. The results show that abdominal upper GI injuries according to RISC score does not constitute an additional risk after trauma beyond that of the grade of severity.
When interpreting the present results, some limitations must be noted. Even if the documentation of the register is of prospective nature, this is a retrospective analysis. This is very valuable and important in many areas but on occasion must be examined critically with regard to the correlation and causality of the data. At the same time, possibly missing values in the data collection may constitute a certain potential for bias. The significance is also limited in the areas of certain subgroups, due to small numbers of cases [35].
Acknowledgements
Finally, we would like to thank the members of the Polytrauma Study Group of the German Society of Trauma Surgery (DGU) for the many years of intensive work on the trauma register. The Polytrauma Study Group has been integrated in the emergency, intensive care and severe injuries department of the DGU since the beginning of 2008.
Participating hospitals
A current list of the clinics which provided data for this analysis to the trauma register may be found at www.traumaregister-dgu.de. We wish to expressly thank them for their cooperation.
References
-
Bardenheuer M, Obertacke U, Waydhas C, Nast-Kolb D (2000) Epidemiology of the severely injured patient. A prospective assessment of preclinical and clinical management. AG Polytrauma of DGU. Unfallchirurg 103: 355-363.
-
Bouillon B, Kanz KG, Lackner CK, Mutschler W, Sturm J (2004) The importance of Advanced Trauma Life Support (ATLS) in the emergency room. Unfallchirurg 107: 844-850.
-
Ring A, Stein E, Stern J (2010) Isolated ileal perforation after blunt abdominal trauma. Zentralbl Chir 135: 342-344.
-
Heuer M, Taeger G, Kaiser GM, Nast-Kolb D, Kühne CA, et al. (2010) No further incidence of sepsis after splenectomy for severe trauma: a multi-institutional experience of the German trauma registry with 1,630 patients. Eur J Med Res 15: 258-265.
-
Heuer M, Kaiser GM, Lendemans S, Vernadakis S, Treckmann JW, et al. (2010) Transplantation after blunt trauma to the liver: a valuable option or just a "waste of organs"? Eur J Med Res 15: 169-173.
-
Franck A, Gerdes B, Karakas E, Rothmund M, Langer P (2010) [Mesh-wrapping of a traumatised liver with active bleeding: a subsequent complication--obstruction of the inferior vena cava]. Zentralbl Chir 135: 154-158.
-
Nast-Kolb D, Trupka A, Ruchholtz S, Schweiberer L (1998) [Abdominal trauma]. Unfallchirurg 101: 82-91.
-
Pfitzenmaier J, Buse S, Haferkamp A, Pahernik S, Djakovic N, et al. (2009) [Kidney injuries]. Unfallchirurg 112: 317-325.
-
Flohé S, Nast-Kolb D (2009) [Surgical management of life-threatening injuries]. Unfallchirurg 112: 854-859.
-
Woelfl CG, Gliwitzky B, Wentzensen A (2009) Standardised primary care of multiple trauma patients: Prehospital Trauma Life Support und Advanced Trauma Life Support. Unfallchirurg 112: 846-853.
-
Heuer M, Hussmann B, Kaiser G, Nast-Kolb D, Ruchholtz S, et al. (2014) Hollow organ injury and multiple trauma: treatment, course and outcome - an organ-specific evaluation of 1,127 patients from the trauma registry of the DGU. Zentralbl Chir 139: 445-451.
-
Ruchholtz S (2000) The trauma registry of the German society of trauma surgery as a basis for interclinical quality management. A multicenter study of the German society of trauma surgery. Unfallchirurg 103: 30-37.
-
Bone RC, Balk RA, Cerra FB, Dellinger RP, Fein AM, et al. (1992) Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. The ACCP/SCCM Consensus Conference Committee. American College of Chest Physicians/Society of Critical Care Medicine. Chest 101: 1644-1655.
-
Vincent JL, Moreno R, Takala J, Willatts S, De Mendonça A, et al. (1996) The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure. On behalf of the Working Group on Sepsis-Related Problems of the European Society of Intensive Care Medicine. Intensive Care Med 22: 707-710.
-
Huber-Wagner S, Lefering R, Qvick LM, Körner M, Kay MV, et al. (2009) Effect of whole-body CT during trauma resuscitation on survival: a retrospective, multicentre study. Lancet 373: 1455-1461.
-
Dutton RP, Lefering R, Lynn M (2006) Database predictors of transfusion and mortality. J Trauma 60: S70-77.
-
Ruchholtz S, Lefering R, Paffrath T, Oestern HJ, Neugebauer E, et al. (2008) Reduction in mortality of severely injured patients in Germany. Dtsch Arztebl Int 105: 225-231.
-
Lefering R (2009) Development and validation of the revised injury severity classification score for severely injured patients. Eur J Trauma Emerg Surg 35: 437-447.
-
Tan KK, Liu JZ, Go TS, Vijayan A, Chiu MT (2010) Computed tomography has an important role in hollow viscus and mesenteric injuries after blunt abdominal trauma. Injury 41: 475-478.
-
Nast-Kolb D, Bail HJ, Taeger G (2005) [Current diagnostics for intra-abdominal trauma]. Chirurg 76: 919-926.
-
Woltmann A, Thannheimer A, Hauck S (2003) Post-traumatic septic abdomen. Trauma Berufskrankh 5: 293-295.
-
Venkatesh KR, McQuay N Jr (2007) Outcomes of management in stable children with intra-abdominal free fluid without solid organ injury after blunt abdominal injury. J Trauma 62: 216-220.
-
Cigdem MK, Onen A, Siga M, Otcu S (2009) Selective nonoperative management of penetrating abdominal injuries in children. J Trauma 67: 1284-1286.
-
Becker HP, Willms A, Schwab R (2006) [Laparoscopy for abdominal trauma]. Chirurg 77: 1007-1013.
-
Espinoza R, Rodríguez A (1997) Traumatic and nontraumatic perforation of hollow viscera. Surg Clin North Am 77: 1291-1304.
-
Lendemans S, Heuer M, Nast-Kolb D, Kühne CA, Dammann M, et al. (2008) [Significance of liver trauma for the incidence of sepsis, multiple organ failure and lethality of severely injured patients. An organ-specific evaluation of 24,771 patients from the trauma register of the DGU]. Unfallchirurg 111: 232-239.
-
Malone D, Napolitano LM, Genuit T, Bochicchio GV, Kole K, et al. (2001) Total cytokine immunoassay: a more accurate method of cytokine measurement? J Trauma 50: 821-825.
-
Moore FA, Moore EE, Sauaia A (1997) Blood transfusion. An independent risk factor for postinjury multiple organ failure. Arch Surg 132: 620-624.
-
Nichols RL, Smith JW, Klein DB, Trunkey DD, Cooper RH, et al. (1984) Risk of infection after penetrating abdominal trauma. N Engl J Med 311: 1065-1070.
-
Woltmann A (1998) New development in treatment of peritonitis. Zentralbl Chir 123: 22-27.
-
Troja A, Hempen HG, Raab HR (2010) [Oesophageal perforation: a retrospective analysis of aetiology, diagnosis and therapy]. Zentralbl Chir 135: 59-64.
-
Stillwell M, Caplan ES (1988) The septic multiple-trauma patient. Crit Care Clin 4: 345-373.
-
Clarke JR, Trooskin SZ, Doshi PJ, Greenwald L, Mode CJ (2002) Time to laparotomy for intra-abdominal bleeding from trauma does affect survival for delays up to 90 minutes. J Trauma 52: 420-425.
-
Schroeppel TJ, Croce MA (2007) Diagnosis and management of blunt abdominal solid organ injury. Curr Opin Crit Care 13: 399-404.
-
Wutzler S, Westhoff J, Lefering R, Laurer HL, Wyen H, et al. (2010) [Time intervals during and after emergency room treatment. An analysis using the trauma register of the German Society for Trauma Surgery]. Unfallchirurg 113: 36-43.
-
The American Association for the Surgery of Trauma.





