Journal of Clinical Gastroenterology and Treatment
"Colonic Lipoma: Incidental and Urgent Management, Report of Two Cases and Review of the Literature"
Justo I*, Marcacuzco A, Caso O, Cambra F, García-Nebreda M, Nutu A, Rivas C and Jiménez C
12 de Octubre University Hospital. Avda de Cordova S/N Madrid, Spain
*Corresponding author:
Iago Justo Alonso, MD, PhD, 12 de Octubre University Hospital, Avda de Cordova S/N Madrid, Spain, Tel: +0034-635676562, E-mail: iagojusto@hotmail.com
J Clin Gastroenterol Treat, JCGT-2-028, (Volume 2, Issue 2), Case Series; ISSN: 2469-584X
Received: April 09, 2016 | Accepted: May 27, 2016 | Published: May 29, 2016
Citation: Justo I, Marcacuzco A, Caso O, Cambra F, García-Nebreda M, et al. (2016) "Colonic Lipoma: Incidental and Urgent Management, Report of Two Cases and Review of the Literature". J Clin Gastroenterol Treat 2:028. 10.23937/2469-584X/1510028
Copyright: © 2016 Justo I, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Introduction
Lipomas are benign tumors rarely found in the digestive tract, particularly rare in the colon [1], that were first described by Bauer in 1757 as an unusual cause of intussusception in the adult. Lipomas are most often small, asymptomatic and identified as incidental findings during colonoscopy [2]. Nonetheless, up to 25% are symptomatic in the form of abdominal pain, bleeding, diarrhea or intussusception [3]. Ninety percent of lipomas in the colon are located at the submucosal layer, with only few originating in the subserosa [4]. When lipomas present as bowel obstruction, they are often pedunculated and large [5].
Clinical Case 1
A previously healthy 33-year-old male recently diagnosed by colonoscopy of a colonic submucosal lesion vs extrinsic compression of the hepatic colonic flexure, presented with abdominal pain, diarrhea and rectorrhagia for a month. He complained of worsening symptoms in the previous hours, associated to vomiting. On examination, the patient was afebrile and presented with a distended abdomen that was painful upon deep palpation, but had no signs of rigidity or peritoneal inflammation. Lab work-up showed discrete leukocytosis.
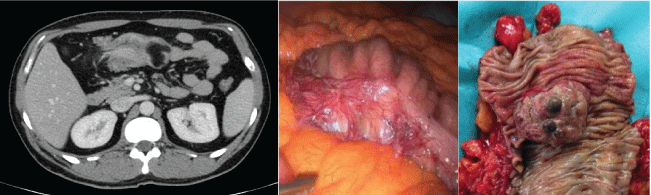
An urgent CT showed a colo-colonic intestinal invagination and a 3,7 cm mass compatible with a lipoma at the hepatic flexure, which served as the head of the intussusception. There was also post-stenotic dilation (Figure 1).
.
Figure 1: CT showing colo-colonic intussusception. Macrocospic image of the lesion. Right: during laparoscopy. Left: macroscopic view.
View Figure 1
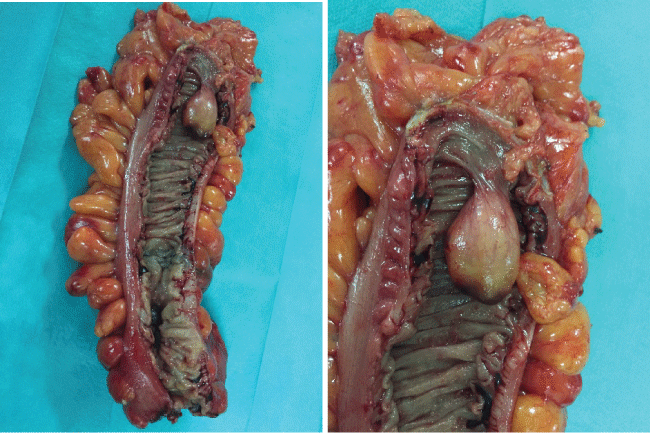
With these findings, the patient underwent an exploratory laparoscopy that identified a colo-colonic intussusception of the transverse colon (Figure 1) associated to a short right colon, for which he received a laparoscopic right hemicolectomy.
The patient's postoperative course was uneventful. The pathological report revealed intussusception caused by the lipoma, with no evidence of malignancy.
Clinical Case 2
A 51-year-old male with prior history of obesity and type II diabetes sought consultation for abdominal pain and rectorrhagia. Colonoscopy show a distal sigmoid tumor, approximately 18 cm from the anal margin and a pedunculated mass approximately 40 cm from the anal margin, compatible with lipoma. With these findings, the patient was taken to laparoscopic oncological sigmoidectomy with complete mobilization of the splenic flexure in order to fully resect the area containing the lipoma (Figure 2). The postoperative course was uneventful, except for Central venous catheter-related bacteremia that was propperly treated with antibiotics. The pathological report revealed a T3N1 (1/31) adenocarcinoma and a pedunculated lipoma without signs of dysplasia.
Discussion
Colonic lipomas are rare benign tumors of the digestive tract. Their incidence is estimated between 0.035 and 4.4%, peaking between ages fifty and sixty, with a female preponderance. They are usually solitary and most frequently occur in the ileocecal area [4].
Colonic intussusception is a rare form of presentation for this benign tumor; however, as 64% of neoplasias causing intussisception are malignant, we recommend surgery as the initial approach. The clinical picture of abdominal pain, obstructive symptoms and rectorraghia or melena is unspecific, thus a high index of suspicion is needed for the diagnosis [6], and abdominal CT is the imaging technique with greatest diagnostic yield in these cases. Colonoscopy is useful for locating the injury or evaluating the degree of obstruction, however, since lipomas are usually submucosal injuries, they are very difficult to characterize by this technique alone. Other tests such as abdominal ultrasound or X-ray are less sensitive. Laparoscopy can be therapeutic, but to date there are no defined diagnostic or treatment patterns [7].
Intraoperative frozen section biopsies may be useful for obtaining a faster diagnosis and thus allow more limited resections [8]. The laparoscopic removal of these lesions, guided or not by endoscopy, may be very complex in urgent situations [3].
Conservative management and radiological follow-up may be considered in case of an incidental finding of intussusception in the absence of clinical repercussion and with a clear cause; however, in most cases, surgical resection of the affected area allows for the prevention of recurrences of the clinical presentation in the case of benign injuries and a curative treatment in malignant lesions [9]. This is especially true in cases requiring urgent intervention. There are reports in the literature of elective endoscopic resections of lesions up to 5 cm, but is not recommended due to the high risk of perforation [10].
Conclusion
Resection of lipomas must be considered in the management of the patients with this pathology who require abdominal surgery. Colo-colonic invagination is a pathology requiring surgical treatment that must be considered in the differential diagnosis of acute intestinal obstruction.
References
-
Bardaji M, Roset F, Camps R, Sant F, Fernandez-Layos MJ (1998) Symptomatic colonic lipoma: differential diagnosis of large bowel tumors. Int J Colorectal Dis 13: 1-2.
-
Ryan J, Martin JE, Pollock DJ (1989) Fatty tumours of the large intestine: a clinicopathological review of 13 cases. Br J Surg 76: 793-796.
-
Ladurner R, Mussack T, Hohenbleicher F, Folwaczny C, Siebeck M, et al. (2003) Laparoscopic-assisted resection of giant sigmoid lipoma under colonoscopic guidance. Surg Endosc 17: 160.
-
Rogy MA, Mirza D, Berlakovich G, Winkelbauer F, Rauhs R (1991) Submucous large bowel lipomas. Presentation and management. An 18-year study. Eur J Surg 157: 51-55.
-
Zhou X, Hu K., Jiang Y (2014) A 4 cm lipoma of the transverse colon causing colonic intussusception: A case report and literatura review. Oncol Lett 8: 1090-1092.
-
Nallamothu G, Adler DG (2011) Large colonic lipomas. Gastroenterol Hepatol (N Y) 7: 490-492.
-
Boler DE, Baca B, Uras C (2013) Laparoscopic resection of colonic lipomas: When and why? Am J Case Rep 14: 270-275.
-
Gordon RS, O'Dell KB, Namon AJ, Becker LB (1991) Intussusception in the adult--a rare disease. J Emerg Med 9: 337-342.
-
Kwang S, Choi S, Jung E, Jung C, Jung S, et al. (2014) Surgical strategy for colonic intussusception caused by a giant colonic lipoma: a report of two cases and a review of the literatura. Ann Coloproctol Jun 30:147-150.
-
Popa B, Ilie M, Sandru V, Hortopan M, Beuran M, et al. (2015) Endoscopic resection of a giant colonic lipoma causing severe anemia. J Gastrointestin Liver Dis 24: 142.