Journal of Clinical Gastroenterology and Treatment
Diarrhea as First Symptom in Systemic Erythematous Lupus in Child - A Case Report
Milena Rios Santos1,2*, Patrícia Cerqueira Lima1,3, Luciana Rodrigues Silva1,4, Marilia Menegassi Zotareli2, Cibele Dantas Ferreira Marques1,2,4 and Hemerson Dyego Novais Gomes5
1Hospital Universitário Professor Edgard Santos, Centro Pediátrico Prof. Hosannah de Oliveira, Rua Augusto Viana, Canela-Salvador BA, Brasil
2Hospital São Rafael, Avenida São Rafael, 2152 São Marcos - Salvador-BA, Brasil
3Hospital Geral Roberto Santos, Rua Direta do Saboeiro, s/n-Cabula, Salvador-BA, Brasil
4Hospital Aliança, Av. Juracy Magalhães Jr., 2096 - Rio Vermelho, Salvador-BA, Brasil
5Acadêmico de Medicina, Universidade do Estado da Bahia, Campus I, Salvador-BA, R. Silveira Martins, 2555-Cabula, Salvador-BA, Brasil
*Corresponding author:
Milena Rios Santos, Hospital Universitário Professor Edgard Santos, Centro Pediátrico Prof. Hosannah de Oliveira, Rua Augusto Viana, Canela-Salvador BA, Brasil, Fax: +55 (71) 3283-8319, E-mail: milenarioss@gmail.com
J Clin Gastroenterol Treat, JCGT-2-032, (Volume 2, Issue 3), Case Report; ISSN: 2469-584X
Received: February 25, 2016 | Accepted: August 27, 2016 | Published: August 30, 2016
Citation: Santos MR, Lima PC, Silva LR, Zotareli MM, Marques CDF, et al. (2016) Diarrhea as First Symptom in Systemic Erythematous Lupus in Child - A Case Report. J Clin Gastroenterol Treat 2:032. 10.23937/2469-584X/1510032
Copyright: © 2016 Santos MR, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Introduction
The systemic erythematous lupus (LES) is a chronic inflammatory disease of autoimmune aetiology, characterized by the involvement of multiple organs and systems. It can be related to the production of different antibodies and the formation of immune complexes. It is a universally distributed disease which most frequently affects young females in childbearing age. It is uncommon to occur before ten years of age and very rare before five years of age [1].
The early LES in children is responsible for around 10-20% of all patients [1]. Recent studies show an incidence of 0.36-0.9 in 100,000 children [2]. Its prevalence in females is less evidenced among children, especially in patients diagnosed before puberty.
The clinical manifestations of LES are polymorphic, with the involvement of various systems and organs, which often delays its diagnosis. The gastrointestinal symptoms are common in patients with LES, which could mimic any other condition in the digestive system, making the diagnosis more difficult.
The most frequent symptoms with involvement of the digestive and hepatic systems are: adverse reactions to medication, gastrointestinal infections, reporting of abdominal pain and the hepatic pathologies. Less commonly prevalent are the occurrence of lupus mesenteric vasculitis, enteropathy with protein loss, intestinal pseudo-obstruction and acute pancreatitis. All these findings represent complications which should be suspected, in view of the gastrointestinal involvement in this infirmity. Despite the prevalence of LES in the digestive tract, its initial manifestation through diarrhea is uncommon in all ages [3].
There are no specific antibodies related to the involvement of the digestive tract. However, the use of image tests, gastrointestinal endoscopy with biopsies can assist the differential diagnosis. It is highlighted that the most important factor is the clinical suspicion. Most complications improve after treatment with corticoids and immunosuppressant agents. Complications in other organs tend to be worse and can compromise the patients' prognosis.
Case Report
This is a 9-year-old female patient, admitted with reported aqueous diarrhea, with approximately six episodes a day, presence of mucus, no bleeding, associated to vomiting and anorexia, besides weigh loss of 10 kg approximately ten days before admission. She was on the 20th day post-surgery for appendectomy. Infectious, metabolic and inflammatory causes were dismissed after diagnostic investigation.
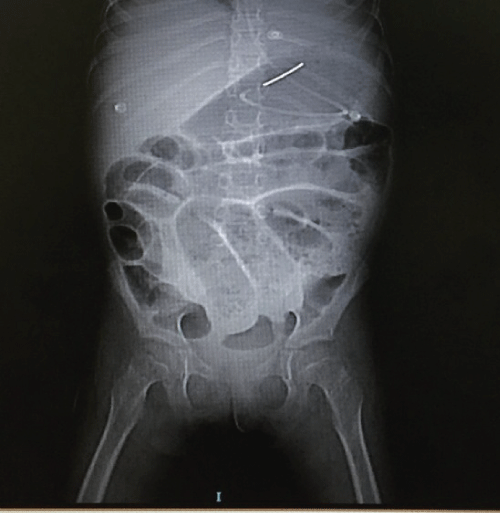
Diet was modified to no lactose intake; however the patient maintained the same pattern of dejection. A digestive endoscopy was performed, finding a discrete chronic esophagitis and discrete chronic gastritis, with normal duodenal mucosa. She was submitted to colonoscopy, which found a discrete reactional hyperplasia in the ileal mucosa, and normal colon and rectum mucosa. After 17 days of admission the patient continued with daily fever, abdominal distension, knee arthralgia, oliguria, proteinuria, anorexia and low mood, as well as a posterior episode of seizure. She was submitted to abdominal X-ray, which showed a significant dilation on the intestinal loops and diffuse thickening of the walls (Figure 1).
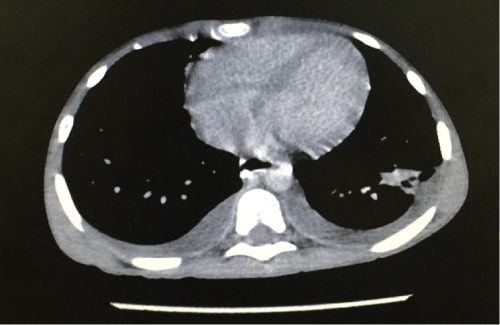
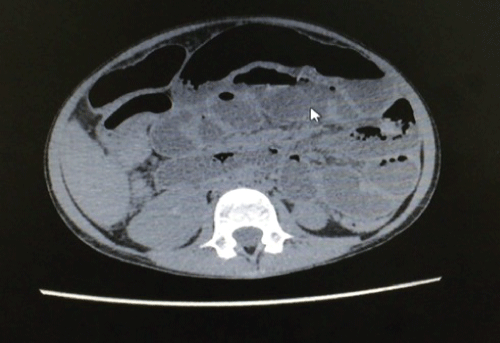
Due to worsening of the clinical symptoms the patient was transferred to Intensive Care Unit. A thorax and abdomen tomography showed dilation of intestinal loops, pyelocalyceal and bilateral urethral dilation, larger on the right side, pulmonary consolidation on the left and signs of ascites (Figure 2 and Figure 3). She was submitted to paracentesis and 1000 ml of ascetic fluid was drained.
She progressed to polyserositis and respiratory failure and needed mechanical ventilation. Following investigation she presented positive ANA dose and anti-DNA, anemia and thrombocytosis, as well as heavy proteinuria, which led to the diagnosis of Systemic Erythematous Lupus. Treatment was initiated by pulse therapy with methylprednisolone (2 mg/kg).
The patient progressed to clinical stability and progressive improvement after seven days of treatment. Maintenance treatment with cyclophosphamide and hydroxychloroquine followed. Two years after diagnosis, the patient is in regular follow-up treatment with a paediatric rheumatologist and is asymptomatic, and the disease is under control.
Discussion
Systemic Erythematous Lupus (LES) is an autoimmune disease whose physiopathology is based on the presence of antibodies and formation of immune complexes. It affects more females than males, on a rate of 10:1 [4].
This disease is uncommon, but not rare, among children. Its initial phase occurs more frequently between 12 and 16-years of age, it is uncommon before ten years of age and very rare before five years of age. It is more severe and has a higher involvement of the renal and central nervous systems in children than among adults [1]. Its diagnosis should be considered in every child who has been unwell for over a week, and a clinical assessment shows involvement of multiple systems. The clinical presentation mostly occurs in outbreaks and remissions, and is characterized by involvement of multiple systems, possibly involving cardiorespiratory, renal, neurological, haematological, osteoarticular, cutaneous and other systems.
The gastrointestinal manifestations, firstly described in 1986 by William Osler, are followed by evidence of the active disease in other organs, and are usually confused with collateral effects of medication used to control the disease [5].
Digestive symptoms can be presented in different ways, with the most common being: abdominal pain, bleeding, motility disorders, oral and rectal ulcers, steatorrhea and diarrhea. This last symptom is related to protein-losing enteropathy [6].
The manifestations in the oral cavity can be present in up to 50% of the patients diagnosed with LES [3]. Oral or nasopharyngeal ulceration is generally painless and is one of the criteria for a LES diagnosis. They are mostly caused due to the disease's activity, or could be associated to Sjogren's syndrome, infections or complications in treatment. However, in the present case, there has not been any oral or nasopharyngeal manifestation, despite what is reported in the literature.
A transversal cohort study found 15% of patients with oral cavity lesions in Brazil, compared to 46% of the population studied in England [7]. These lesions can be treated with corticoids or topic tacrolimus, and the majority starts to regress days or weeks after beginning of treatment. Cases of dyspepsia and presence of peptic ulcerous disease have also been reported in patients with LES, and studies suggest a relationship with long term treatment with non-steroid anti-inflammatories and corticosteroids.
Episodes of abdominal pain can be present in 8 to 40% of patients with LES [5]. Reports include cholecystitis, pancreatitis, peptic ulcers and mesenteric vasculitis. One of the most severe gastrointestinal complications is the vasculitis of blood vessels of intestine, which could progress to ischemia, haemorrhages, perforations or peritonitis [8]. Clinical presentation is variable and a definitive diagnosis is difficult in the early days. The prevalence of intestinal vasculitis has been reported as varying between 0.2-53% in patients with LES [3].
Diarrhea is frequently chronic and associated to protein-losing enteropathy, which affects the small intestine, resulting in villus atrophy and oedema of submucosa. It is characterized by hypoalbuminemia and diarrhea. Treatment is based on the use of corticoids in low dosages. Some patients benefit from concomitant treatment with antibiotics and there are reports of an exceptional adoption of a gluten free diet, however there is no consensus [3].
Persistent diarrhea resulting from the intestinal inflammatory disease is also described in the literature. There are reported cases of association between systemic erythematous lupus with ulcerative rectocolitis (URC), where the symptoms of LES started after treatment for URC with sulfasalazine. The association with Crohn Disease is rare, however is also described [9]. Patients with LES and intestinal inflammatory disease show less photosensitivity, serositis and neurological involvement when compared to patients with isolated LES. The anti-dsDNA is found in most patients with this association and there is a risk of leukopenia and thrombocytopenia.
Conclusion
Systemic Erythematous Lupus can affect any organ or system in the body. Secondary gastrointestinal manifestations are common after diagnosis and are frequently associated to the disease's activity and not an initial manifestation. Whenever present, atypical symptoms or adverse reactions to treatment should always be investigated.
Since the oral mucosa is the most common symptom, a complete and detailed evaluation of the oral cavity should always be performed. Diarrhea could have multiple causes on a patient carrying LES. Although infrequent, it should always be investigated since it can actually be a first symptom of the disease, especially in cases of systemic involvement.
References
-
Malattia C, Martini A (2013) Paediatric-onset systemic lupus erythematosus. Best Pract Res Clin Rheumatol 27: 351-362.
-
Petty RE, Cassidy JT (2001) Systemic lupus erythematosus. In: Cassidy JT, Petty RE, (eds). Textbook of paediatric rheumatology. (5th edn), WB Saunders: 396-449.
-
Xin-Ping T, Xuan Z (2010) Gastrointestinal involvement in systemic lupus erythematosus: Insight into pathogenesis, diagnosis and treatment. World J Gastroenterol 16: 2971-2977.
-
Hiraki LT, Feldman CH, Liu J, Alarcón GS, Fischer MA, et al. (2012) Prevalence, incidence, and demographics of systemic lupus erythematosus and lupus nephritis from 2000 to 2004 among children in the US Medicaid beneficiary population. Arthritis Rheum 8: 2669-2676
-
Sultan SM, Ioannou Y, Isenberg DA (1999) A review of gastrointestinal manifestations of systemic lupus erythematosus. Rheumatology 38: 917-932.
-
Richer O, Ulinski T, Lemelle I, Ranchin B, Loirat C, et al. (2007) French Pediatric-Onset SLE Study Group. Abdominal manifestations in childhood-onset systemic lupus erythematosus. Ann Rheum Dis 66: 174-178.
-
Johnson AE, Cavalcanti FS, Gordon C, Nived O, Palmer RG, et al. (1994) Cross-sectional analysis of the differences between patients with systemic lupus erythematosus in England, Brazil, and Sweden. Lupus 3: 501-506.
-
Kishimoto M, Nasir A, Mor A, Belmont HM (2007) Acute gastrointestinal distress syndrome in patients with systemic lupus erythematosus Lupus 16: 137-141.
-
Koutroubakis IE, Kritikos H, Mouzas IA, Spanoudakis SM, Kapsoritakis AN, et al. (1998) Association between ulcerative colitis and systemic lupus erythematosus: report of two cases. Eur J Gastroenterol Hepatol 10: 437-439.