Journal of Clinical Gastroenterology and Treatment
Portal Hypertension Does Not Preclude the Efficacy of Direct-acting Anti-Hepatitis C Viral Therapy
Kazuhiko Morii1*, Takeharu Yamamoto1, Shinichiro Nakamura2, Mitsuki Fukumoto1, Reiko Iwamoto1, Mai Yoshioka1 and Hiroaki Okushin1
1Department of Hepatology, Japanese Red Cross Society Himeji Hospital, Japan
2Department of Gastroenterology and Hepatology, Okayama University Hospital, Japan
*Corresponding author:
Kazuhiko Morii, MD, PhD, Department of Hepatology, Japanese Red Cross Society Himeji Hospital, 1-12-1 Shimoteno, Himeji, Hyogo 670-8540, Japan, Tel: +8179-294-2251, Fax: +81-79-296-4050, E-mail: moriikazuhiko@gmail.com
J Clin Gastroenterol Treat, JCGT-2-036, (Volume 2, Issue 4), Research Article; ISSN: 2469-584X
Received: August 08, 2016 | Accepted: October 20, 2016 | Published: October 24, 2016
Citation: Morii K, Yamamoto T, Nakamura S, Fukumoto M, Iwamoto R, et al. (2016) Portal Hypertension Does Not Preclude the Efficacy of Direct-acting Anti-Hepatitis C Viral Therapy. J Clin Gastroenterol Treat 2:036. 10.23937/2469-584X/1510036
Copyright: © 2016 Morii K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: This study aimed to investigate whether patients with hepatitis C virus (HCV)-related cirrhosis and clinically significant portal hypertension (CSPH) could show satisfactory virological and safety outcomes on direct-acting antiviral (DAA) therapy.
Methods: Patients with HCV-related cirrhosis treated with DAA therapy were collected in the period between December 2014 and December 2015. Patient characteristics, therapeutic details, and safety outcomes were evaluated. CSPH was defined as presence of gastroesophageal varices via esophagogastroduodenoscopy.
Results: Totally, 113 patients were included in this study; 26 with CSPH and 87 without CSPH. HCV genotype 1b-infected patients were treated with either daclatasvir plus asunaprevir or sofosbuvir plus ledipasvir. HCV genotype 2-infected patients were treated with sofosbuvir plus ribavirin. Sustained virological response (SVR) rates were equally good in patients with CSPH (96%) and in those without CSPH (93%). In patients who achieved SVR, prompt improvements in the hepatic function were observed. Recovery was more pronounced in patients with CSPH. There was no early treatment discontinuation and no hepatic decompensation.
Conclusions: DAA therapy in patients with HCV-related cirrhosis and CSPH could achieve a high SVR rate and early improvements in the hepatic function. This treatment strategy showed relatively fair safety outcomes.
Keywords
Direct-acting antiviral, Hepatitis C virus, Liver cirrhosis, Clinically significant portal hypertension, Gastroesophageal varices
Introduction
Patients with hepatitis C virus (HCV)-related cirrhosis have been considered difficult-to-treat cohorts with limited treatment options and an unfavorable prognosis in the era of interferon-based antiviral therapy. Advanced fibrosis and clinically significant portal hypertension (CSPH), defined as hepatic venous pressure gradient (HVPG) over 10 mmHg, is an ominous predictor of poor treatment efficacy [1,2]. Reiberger, et al. showed that the sustained virological response (SVR) rate was 51% in Child-Pugh class A cirrhotic patients without CSPH compared with 14% in those with CSPH after treatment with pegylated interferon and ribavirin [3,4]. Multivariate analysis revealed that an elevated HVPG is an independent risk factor for treatment failure. Patients with cirrhosis and CSPH have a low chance to achieve SVR and an increased incidence of serious adverse effects. Some explanations have been suggested why portal hypertension reduces antiviral treatment response; disturbed pharmacokinetics such as altered hepatic drug uptake and altered distribution owing to the irregular splanchnic and intrahepatic blood flow, congested intestinal mucosa due to portal hypertension, and impaired T cell chemoattraction and interaction with the HCV-infected hepatocytes owing to the increased hepatic sinusoidal shear stress [3,5].
Recently, significant advances in the treatment of HCV infection have been achieved with the introduction of interferon-free potent direct-acting antiviral (DAA) agents. The safety and efficacy of ledipasvir-sofosbuvir have been well established among patients with compensated cirrhosis and excellent rates of SVR over 90% have been reported [6,7]. Patients with cirrhosis and CSPH are the major difficult-to-treat patients in today's real-life cohorts. Therefore, we aimed to investigate whether patients with HCV-related cirrhosis and CSPH on DAA therapy could exhibit SVR rates and safety outcomes equivalent to those in patients without CSPH.
Patients and Methods
Methods
The present study is a retrospective cohort analysis. We collected the data of the patients with HCV-related cirrhosis treated with DAA therapy in the period between December 2014 and December 2015 at our institute, a community-based tertiary referral hospital with a specialized hepatology department. The electronic medical records were reviewed to evaluate patient characteristics, treatment responses, and safety outcomes. The biochemical data and viral load were recorded at week 0 (start of DAA therapy), week 4, week 8, end of treatment (EoT), and post-treatment week 12 (PT 12).
Patients
The eligible patients were: 1) treated with interferon-free DAA regimens against HCV-related chronic liver disease, 2) no co-infection with hepatitis B virus (HBV), 3) absence of residual hepatocellular carcinoma (HCC), and 4) presence of cirrhosis. Confirmation of the cirrhosis was determined either via a METAVIR score of F4 by liver biopsy specimens, if available, or the combination of an aspartate aminotransferase to platelet ratio index ≥ 2 plus a peripheral platelet count < 100 × 103/μL (Figure 1) [8,9]. The patient characteristics, laboratory test results, and viral load at the initial presentation were listed in table 1 and table 2. All patients were in 5a state of compensated cirrhosis at the initiation of the DAA therapy.
Assessment of CSPH
Patients with CSPH eventually exhibit ascites and/or gastroesophageal varices. Because Japanese medical insurance coverage for anti-HCV DAA therapy are confined to the patients with compensated cirrhosis, CSPH in this study was defined as presence of gastroesophageal varices via esophagogastroduodenoscopy (EGD). All included patients underwent EGD evaluate gastroesophageal varices. Patients were divided into a CSPH cohort and a non-CSPH cohort.
Antiviral therapy and follow-up
Patients infected with HCV genotype 1b were treated with daclatasvir (60 mg) once daily plus asunaprevir (100 mg) twice daily for 24 weeks or sofosbuvir (400 mg) plus ledipasvir (90 mg) once daily for 12 weeks. Patients with HCV genotype 2 were treated with sofosbuvir (400 mg) once daily plus body weight-based ribavirin (200-400 mg) twice daily for 12 weeks. These three combinations had been the only interferon-free DAA regimens approved for treatment of HCV infection at the time of the study in Japan. All patients were treated and followed up by board-certified hepatologists of the Japanese Society for Hepatology (KM and HO).
Statistical analysis
The primary statistical objective was to determine whether the patients with HCV-related cirrhosis and CSPH showed equivalent SVR rate and safety outcomes in DAA therapy compared to those without CSPH. Values are presented as the mean ± standard deviation. Standard statistical methods were used to analyze the results. Biochemical data were compared using the Mann-Whitney rank-sum and chi-square tests. P values less than 0.05 (two-tailed) were considered statistically significant. All analyses were performed using the EZR v1.26 software [10].
Ethics
The ethics committees of our institutional review board approved this study in accordance with the Declaration of Helsinki. Data collection and analyses were conducted on anonymized samples.
Results
Characteristics of the patients at the baseline
Between December 2014 and December 2015, 432 patients with HCV-related chronic liver diseases received DAA therapy in our institute. Three patients, co-infected with HBV and HCV, were excluded. No patients had concomitant infection with human immunodeficiency virus. A total of 113 patients that exhibited an initial peripheral platelet count below 100 × 103/μL were enrolled in the analysis. All patients were Japanese. Patients with gastroesophageal varices via EGD comprised the CSPH cohort (n = 26), and the remaining comprised the non-CSPH cohort (n = 87) (Figure 1). The patient characteristics are listed in table 1. HCV genotype 1b (90%) and 2 were represented. HCC had been treated by ablation or hepatic resection in 41 patients (36%) prior to the initiation of the DAA therapy. Absence of residual HCC was judged based on imaging study within a month before the DAA therapy. Mean Child-Turcotte-Pugh scores and model for end-stage liver disease (MELD) scores were 7.5 and 6.6 in the CSPH cohort, and 5.3 and 5.3 in the non-CSPH cohort, respectively. The CSPH cohort had significantly higher serum bilirubin levels, lower albumin levels, and higher prothrombin-time international normalized ratio (PT INR) than the non-CSPH cohort did. The CSPH cohort also had significantly lower hemoglobin content, platelet counts, and estimated glomerular filtration rate (eGFR). Eleven (42%) patients in the CSPH cohort had a history of ascites. Age, sex, body mass index, and baseline HCV viral load did not differ between the CSPH and non-CSPH cohorts.
Virological response
The overall SVR (SVR12) rate was 94%, by intention to treat analysis. No significant difference in the SVR rates was noticed between the patients with CSPH (96%) or those without (93%) (Table 1). Eighty-eight patients had received daclatasvir plus asunaprevir, 14 received sofosbuvir plus ledipasvir, and 11 received sofosbuvir plus ribavirin; the resultant SVR rates were 92%, 100%, and 100%, respectively (Table 2). The CSPH and non-CSPH cohorts similarly showed a rapid decline in the HCV viral load (Figure 2A). At week 4, HCV RNA became undetectable in two thirds of the patients and was below the quantitation limit (1.2 Log10 IU/mL) in the remaining patients. There were 7 cases (6%) of treatment failure in the daclatasvir plus asunaprevir group, all of them resulted from on-treatment breakthrough.
.
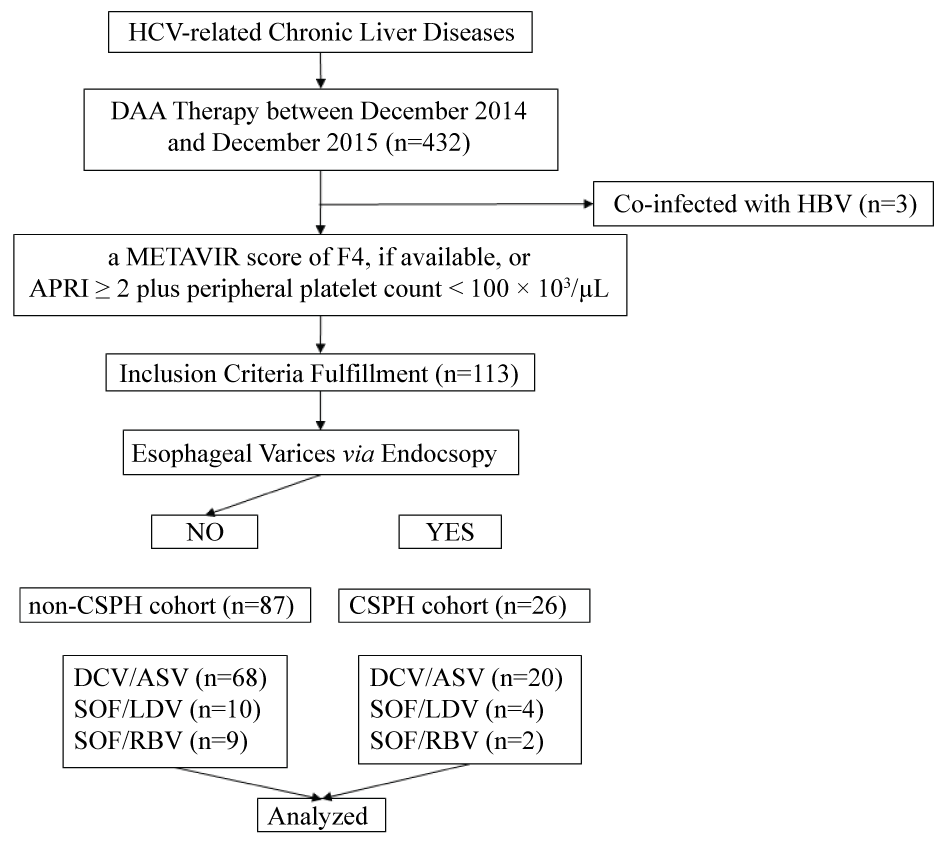
Figure 1: Patient inclusion flowchart.
APRI: Aspartate aminotransferase to Platelet Ratio Index; ASV: Asunaprevir, CSPH: Clinically Significant Portal Hypertension; DAA: Direct-Acting Antiviral; DCV: Daclatasvir; HBV: Hepatitis-B virus; HCV: Hepatitis-C virus; LDV: Ledipasvir; RBV: Ribavirin; SOF: Sofosbuvir
View Figure 1
![]()
Table 1: Baseline characteristics of the patients with and without CSPH.
View Table 1
Biochemical responses during the DAA therapy
Serum levels of alanine aminotransferase (ALT) rapidly declined within the normal limit at week 4 in both cohorts (Figure 2B). A transient elevation of ALT occurred after week 8 in the non-CSPH cohort. Serum total bilirubin and albumin concentration showed more pronounced improvement in the CSPH cohort than in the non-CSPH cohort (Figure 2C and Figure 2D). The PT INR and serum creatinine concentration remained almost unchanged. The MELD score stabilized and incrementally decreased in both cohorts (Figure 2E). Serum alpha-fetoprotein (AFP) levels surprisingly showed a rapid decline in both cohorts (Figure 2F).
.
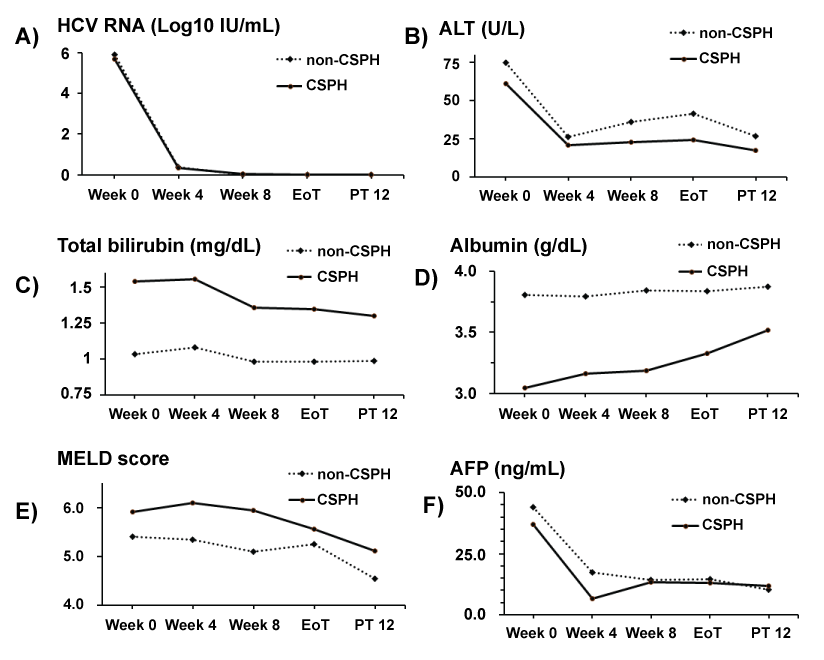
Figure 2: Virological and biochemical responses during DAA therapy in patients who achieved SVR (A to F).
(A) Mean change from the baseline in the HCV viral load. No differences in the viral load decline were found between the two cohorts. EoT, end of treatment; PT 12, post-treatment week 12; (B) Serum ALT levels rapidly declined to the normal limit at week 4 in both cohorts. Transient elevation was noticed from week 8 in the non-CSPH cohort; (C,D) Improvement of the serum total bilirubin and albumin was more evident in the CSPH cohort than in the non-CSPH cohort; (E) MELD score had decreased in in both cohorts; (F) Interestingly, serum AFP levels showed a rapid decline in both cohorts.
View Figure 2
![]()
Table 2: Baseline characteristics of the three treatment regimen groups.
View Table 2
Safety assessment
Mild adverse events, such as fatigue and decreased appetite were experienced by several patients. Slight elevations of ALT and/or total bilirubin levels were noticed in several patients treated with daclatasvir plus asunaprevir. Three patients required dose reduction of ribavirin, and then could continue the treatment regimen. Two patients in the CSPH cohort experienced serious adverse events on treatment; bacterial pneumonia and cryptogenic bacteremia, both in daclatasvir plus asunaprevir group. After transient DAA interruption and antibiotic treatment at hospital, both patients resumed the DAA therapy and finally achieved SVR. There were no grade 3 or 4 laboratory abnormalities leading to premature discontinuation of treatment. No patients experienced hepatic decompensation including ascites, hepatic encephalopathy, or variceal hemorrhage during the DAA therapy.
Discussion
This study demonstrated that DAA therapy achieved satisfactory SVR rates in patients with HCV-related cirrhosis and CSPH. SVR rates were high in patients with cirrhosis, irrespective of the concomitant CSPH. CSPH is not a "point of no return" where HCV eradication dose not result in improvement in liver function, in patients with compensated cirrhosis. This study proved the efficacy of the DAA therapy in these difficult-to-treat patients and thus, it might help to guide therapy decisions in the advanced stage of cirrhosis.
In patients who achieved SVR, MELD scores had stabilized and incrementally improved in both cohorts [6]. These improvements were largely due to the decreases in bilirubin level and the increases in albumin level. The serum level of ALT had declined promptly to the normal range, just along with the rapid viral clearance. This therapeutic course indicated that continuing hepatic inflammation due to the replication of HCV might exert substantial stress on the liver. Hence, eradication of HCV infection could reverse the hepatic dysfunction, even in patients with advanced cirrhosis. Because our observation was for a rather short period, longer follow up studies after the DAA therapy are required.
The adverse events were generally mild and there was no premature treatment discontinuation or hepatic decompensation. Two patients in the CSPH cohort suffered from infectious events requiring hospitalization. These adverse events were indistinguishable from the infectious complications occurring during the clinical courses of advanced cirrhosis, and might be treatment-unrelated. Expertise as well as close monitoring is needed for treating patients with advanced liver disease by DAA therapy.
Interestingly, slight elevation of the serum ALT levels was observed in the non-CSPH cohort after week 8 (Figure 2B). Diverse adverse effects of the DAA therapy might cause this slight elevation of the ALT level. However, this explanation was inconsistent with the fact that there was no apparent elevation of the ALT levels in the CSPH cohort. Fatty liver did not seem to be the culprit because there was no difference in the BMI between the two cohorts (Table 1). Alcohol intake was strictly inhibited during the DAA therapy. We speculated that the eradication of HCV infection might reduce the inhibitory effects of HCV proteins on the adaptive immunity [6], and the consequent subtle change in the immunological and inflammatory environment might provoke some reactions, such as immune reconstitution inflammatory syndrome [11,12].
It was also surprising that the serum AFP levels showed rapid decline to the normal range in patients who achieved SVR (Figure 2F) [13]. An elevated AFP level is associated with an increased risk of HCC [14]. Post-interferon treatment, elevated ALT and AFP levels are associated with a risk of hepatocarcinogenesis in patients with chronic hepatitis C [15]. Today, it still remains elusive whether HCV eradication by interferon-free DAA therapy will ameliorate the further development of HCC. A recent study reported an unexpected high rate of HCC recurrence after HCV clearance with DAA therapy [16]. Our subjects were generally old-aged patients with cirrhosis and included a high proportion of patients with prior HCC. These patients are at high risk of recurrence or new development of HCC. It is important to follow up the patients after the therapeutic course carefully and to survey the development of HCC.
Direct measurement of HVPG was not performed in this study. It is an invasive procedure and not routinely performed during the daily clinical practice. Therefore, we employed the presence of gastroesophageal varices as a surrogate indicator of CSPH. As the cirrhosis progresses, the portal pressure increases beyond the threshold of CSPH resulting in the occurrence of gastroesophageal varices [17]. Seventy-two percent of the patients with CSPH had gastroesophageal varices. On the contrary, the presence of CSPH is established for patients with gastroesophageal varices via EGD [3]. Thus, we considered that the CSPH criterion adopted in this study is valid. In reality, the CSPH cohort had significantly worse hematological and biochemical data than the non-CSPH cohort did, indicating that the CSPH cohort suffered from more advanced cirrhosis. Of course, we must consider that CSPH does not always mean advanced cirrhosis. For example, unexpected large gastroesophageal varices may be observed in apparently compensated patients with portal vein thrombosis or primary biliary cholangitis.
Our study has several limitations. Numbers of the patients treated with sofosbuvir plus ledipasvir and sofosbuvir plus ribavirin were small. However, the purpose of this study was not to compare the treatment outcomes by each DAA regimen. The majority of the patients had HCV genotype 1b infection (90%), whereas 10% of the patients had genotype 2 infection, and no patients had genotype 1a or genotypes 3-6. The included patients were limited to Japanese. Moreover, only patients with compensated cirrhosis were enrolled in this study, thus the favorable efficacy and safety outcomes of this study could not be fully applied to the patients with decompensated cirrhosis. A recent clinical trial has reported that the newly approved DAA agents were able to treat HCV infection in patients with decompensated cirrhosis [7]. However, it is not completely known whether such new DAA agents can be safely adapted to the daily clinical practice.
In conclusion, interferon-free DAA therapy in HCV genotype 1b or 2-infected patients with compensated cirrhosis showed a high SVR rate, regardless of the concomitant CSPH. SVR was associated with gradual improvement in the hepatic function. This therapy revealed relatively fair safety outcomes. However, future questions arise about whether the DAA-induced SVR will produce persistent improvement in the liver function and decrease the risk of HCC in patients with advanced cirrhosis.
Acknowledgments
The authors would like to acknowledge the work of staff in Department of Hepatology: Asuka Tabata, Ayumi Fujioka, and Ryota Oshima.
Funding
None.
Conflict of Interest
The authors declare no conflict of interest.
References
-
Bruno S, Stroffolini T, Colombo M, Bollani S, Benvegnù L, et al. (2007) Sustained virological response to interferon-alpha is associated with improved outcome in HCV-related cirrhosis: a retrospective study. Hepatology 45: 579-587.
-
Ghany MG, Strader DB, Thomas DL, Seeff LB; American Association for the Study of Liver Diseases (2009) Diagnosis, management, and treatment of hepatitis C: an update. Hepatology 49: 1335-1374
-
Reiberger T, Rutter K, Ferlitsch A, Payer BA, Hofer H, et al. (2011) Portal pressure predicts outcome and safety of antiviral therapy in cirrhotic patients with hepatitis C virus infection. Clin Gastroenterol Hepatol 9: 602-608.
-
Grace ND (2011) Patients with clinically significant portal hypertension caused by hepatitis C virus cirrhosis respond poorly to antiviral therapy. Clin Gastroenterol Hepatol 9: 536-538.
-
Liu C, Zhu H, Tu Z, Xu YL, Nelson DR (2003) CD8+ T-cell interaction with HCV replicon cells: evidence for both cytokine- and cell-mediated antiviral activity. Hepatology 37: 1335-1342.
-
Curry MP, O'Leary JG, Bzowej N, Muir AJ, Korenblat KM, et al. (2015) Sofosbuvir and Velpatasvir for HCV in Patients with Decompensated Cirrhosis. N Engl J Med 373: 2618-2628.
-
Charlton M, Everson GT, Flamm SL, Kumar P, Landis C, et al. (2015) Ledipasvir and Sofosbuvir Plus Ribavirin for Treatment of HCV Infection in Patients With Advanced Liver Disease. Gastroenterology 149: 649-659.
-
Bashour FN, Teran JC, Mullen KD (2000) Prevalence of peripheral blood cytopenias (hypersplenism) in patients with nonalcoholic chronic liver disease. Am J Gastroenterol 95: 2936-2939.
-
Lin ZH, Xin YN, Dong QJ, Wang Q, Jiang XJ, et al. (2011) Performance of the aspartate aminotransferase-to-platelet ratio index for the staging of hepatitis C-related fibrosis: an updated meta-analysis. Hepatology 53: 726-736.
-
Kanda Y (2013) Investigation of the freely available easy-to-use software 'EZR' for medical statistics. Bone Marrow Transplant 48: 452-458.
-
Balagopal A, Thio CL (2015) Editorial Commentary: Another Call to Cure Hepatitis B. Clin Infect Dis 61: 1307-1309.
-
French MA (2009) HIV/AIDS: immune reconstitution inflammatory syndrome: a reappraisal. Clin Infect Dis 48: 101-107.
-
Miyaki E, Imamura M, Hiraga N, Murakami E, Kawaoka T, et al. (2015) Daclatasvir and asunaprevir treatment improves liver function parameters and reduces liver fibrosis markers in chronic hepatitis C patients. Hepatol Res 46: 758-764.
-
Oka H, Tamori A, Kuroki T, Kobayashi K, Yamamoto S. (1994) Prospective study of alpha-fetoprotein in cirrhotic patients monitored for development of hepatocellular carcinoma. Hepatology 19: 61-66.
-
Asahina Y, Tsuchiya K, Nishimura T, Muraoka M, Suzuki Y, et al. (2013) α-fetoprotein levels after interferon therapy and risk of hepatocarcinogenesis in chronic hepatitis C. Hepatology 58: 1253-1262.
-
Reig M, Mariño Z, Perelló C, Iñarrairaegui M, Ribeiro A, et al. (2016) Unexpected early tumor recurrence in patients with hepatitis C virus –related hepatocellular carcinoma undergoing interferon-free therapy: a note of caution. J Hepatol 65: 719-726.
-
D'Amico G, Garcia-Tsao G, Pagliaro L (2006) Natural history and prognostic indicators of survival in cirrhosis: a systematic review of 118 studies. J Hepatol 44: 217-231.





