Journal of Clinical Gastroenterology and Treatment
A Case of Acute Liver Failure Involving a Big Liver and a Small Cell
SAL Hall1*, T Thomas2, R Pathi3, KR Muller1 and AJ Wigg1
1Hepatology and Liver Transplantation Medicine Unit, Flinders Medical Centre, Adelaide, Australia
2Anatomical Pathology, Flinders Medical Centre, Adelaide, Australia
3Medical Imaging, Flinders Medical Centre, Adelaide, Australia
*Corresponding author: SAL Hall, Hepatology and Liver Transplantation Medicine Unit, Flinders Medical Centre, Adelaide, Australia, E-mail: samuel.hall@sa.gov.au
J Clin Gastroenterol Treat, JCGT-03-043, (Volume 3, Issue 1), Case Report; ISSN: 2469-584X
Received: October 19, 2016 | Accepted: February 27, 2017 | Published: March 02, 2017
Citation: Hall SAL, Thomas T, Pathi R, Muller KR, Wigg AJ (2017) A Case of Acute Liver Failure Involving a Big Liver and a Small Cell. J Clin Gastroenterol Treat 3:043. 10.23937/2469-584X/1510043
Copyright: © 2017 Hall SAL, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Liver transplantation (LT) is an effective treatment for eligible patients with Acute Liver Failure (ALF). Prompt evaluation and decision making are required as there is often a small window of opportunity for LT before deterioration of patient health makes LT futile. The consequences of failure to recognize malignancy induced ALF may be catastrophic resulting in inappropriate LT and a common problem in this setting is the relatively normal parenchymal appearance of the liver with contrast imaging. Transjugular liver biopsy must be considered in all cases of ALF that are idiopathic, and mandatory if associated with clinical features suggestive of malignancy including hepatomegaly, hypercalcaemia and elevated LDH. Our case describes such a scenario and demonstrates the value of liver biopsy in such a setting.
Keywords
Acute liver failure, Liver transplantation, Malignancy induced ALF
Abbreviations
ALF: Acute Liver Failure; LT: Liver Transplantation; LFTs: Liver Function Test; LDH: Lactate Dehydrogenase; AASLD: American Association for the Study of Liver Diseases; INR: International Normalized Ratio
Introduction
Acute Liver Failure (ALF) is a rare condition with high mortality. Clinicians can be confronted with the difficult task of being unable to confidently identify the cause of ALF during a small window of opportunity for Liver Transplantation (LT). If the aetiology of ALF remains unclear during this scenario, livery biopsy must be performed.
Case Report
A 65-year-old male presented with a 2-week history of jaundice, right upper quadrant pain and diffuse derangement of Liver Function Tests (LFTs). Past history included type 2 diabetes mellitus, hypertension, moderate alcohol consumption (20 g/day) for many years and a 40-pack year smoking history. His long-term medications included metformin, perindopril and amlodipine and there was no history of recent non-prescription drug use.
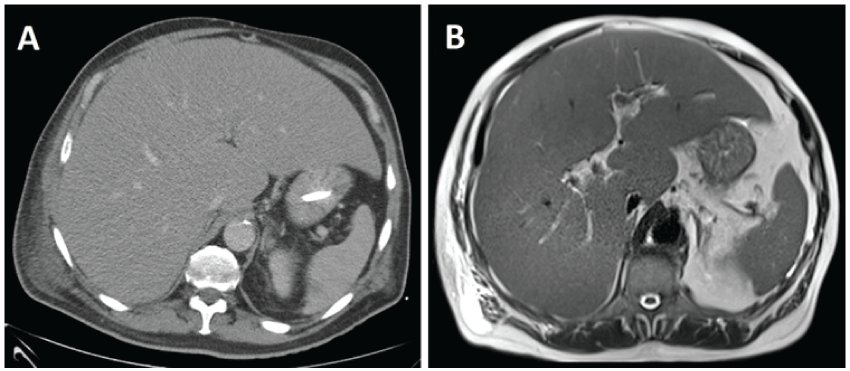
On presentation LFTs were as follows; bilirubin 5.4 mg/dL, ALP 225 U/L, GGT 515 U/L, ALT 234 U/L, AST 175 U/L, albumin 3.2 g/dL, INR 1.3, lactate dehydrogenase (LDH) 476 U/L and Uric Acid 10 mg/dL. The initial ALT to LDH ratio was less than 1.5, which meant acute viral hepatitis was a less likely cause of the clinical picture [1]. All serum & urinary screens for causes of acute liver function derangement were negative. The elevated LDH suggested malignancy was a potential cause for this scenario [2,3]. However, abdominal ultrasound, contrast CT (Figure 1A) and MRI (Figure 1B) showed hepatomegaly but with no discrete liver lesions and no biliary abnormalities. On day 10 of admission, the patient developed features of acute liver failure, in accordance with the American Association for the Study of Liver Diseases (AASLD) criteria [4], with worsening bilirubin (19.5 mg/dL), coagulopathy (INR 3.3) and encephalopathy (grade 3) and soon required admission to the intensive care unit.
.
Figure 1: Imaging of the Liver: A) CT abdomen; B) T2 weighted MRI image showing a moderately enlarged liver with mild diffuse steatosis. No focal lesions nor any diffuse infiltration are detected.
View Figure 1
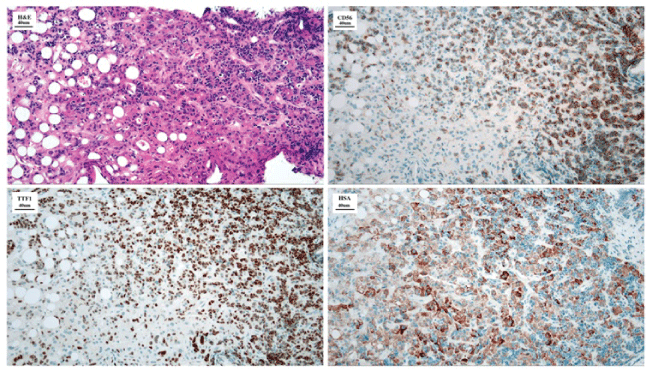
Transplantation for "sero-negative" ALF was considered but the development of hypercalcaemia and an elevated LDH together with significant hepatomegaly prompted an urgent transjugular liver biopsy (Figure 2). This revealed diffuse infiltration by a small cell neuroendocrine carcinoma with positive labelling for thyroid transcription factor-1 suggesting metastasis from a primary small cell lung cancer (SCLC). CT chest revealed centrilobular emphysema and a small irregular nodule at the apex of the left upper lobe suggestive of primary lung malignancy. There was no knowledge of any symptoms to suggest primary lung malignancy prior to this admission, although he did have a significant history of smoking. The patient continued to deteriorate rapidly and was deemed unsuitable for both Liver Transplantation (LT) and chemotherapy and died day 14 post admission.
.
Figure 2: Transjugular Liver Biopsy showing diffuse infiltration of hepatic parenchyma by a small cell carcinoma. The thyroid transcription factor 1 (TTF1) marker shows strong nuclear labelling of the small cell carcinoma.
View Figure 2
Discussion
AASLD defines acute liver failure as evidence of a coagulopathy, consisting of an International Normalized Ratio (INR) ≥ 1.5 and encephalopathy in a non-cirrhotic patient with a disease course of < 26 weeks' duration [4]. The most common causes of acute liver failure are viral and drug-induced hepatitis. In Australia, acetaminophen is the most common cause [5].
Hepatic metastases have been reported in up to 36% of individuals who die from cancer. The liver is the most common site for tumour deposits, but liver dysfunction may not be present. Jaundice may not even be present despite the liver having up to 90% tumour involvement [6].
Although SCLC and other malignancies with diffuse liver infiltration are a recognized cause of ALF, it remains an extremely rare but important cause of ALF. It has been reported in the literature to occur at a frequency as low as 4 in every 1000 cases of ALF [6]. Haematological malignancies are the leading cause of malignant hepatic infiltration and subsequent ALF. Less common malignant causes of ALF include primary lung, gastrointestinal, breast, urothelial, nasopharyngeal malignancy and melanomas [7].
SCLC commonly deposits tumour in the liver, because it is highly invasive. However, a rapid progression to acute liver failure is extremely rare [8]. Death ensues within days to weeks once SCLC has metastasised to the liver resulting in ALF [9].
Clinicians must be vigilant with idiopathic ALF to exclude malignancy. The consequences of failure to recognize malignancy induced ALF may be catastrophic resulting in inappropriate and futile LT. The mechanism of ALF in this setting is unknown but may relate to rapid microvascular invasion of vast areas of hepatic parenchyma [10].
A common problem in this setting is the relatively normal parenchymal appearance of the liver with contrast imaging, as in this case, where both CT and MRI did not demonstrate discrete tumour deposits [8]. Both CT and MRI have very low sensitivities for detecting hepatic tumour deposits less than 2 cm with sensitivities of 20% and 33% respectively [11].
Relevant clues in this case included; gross hepatomegaly, hypercalcaemia (likely paraneoplastic), and elevated LDH and lung nodule on repeat review of CT scan. Elevated LDH has been described in a number of prior case reports involving metastatic tumour deposits to the liver and its elevation on admission was also an important clinical clue in this case [2,3]. LDH is also a prognostic marker for an increased risk of developing ALF once SCLC has metastasised to the liver [7]. In our view transjugular liver biopsy must be considered in all cases of ALF that are idiopathic, and mandatory if associated with clinical features suggestive of malignancy including hepatomegaly, hypercalcaemia and elevated LDH.
References
-
Cassidy WM, Reynolds TB (1994) Serum lactic dehydrogenase in the differential diagnosis of acute hepatocellular injury. J Clin Gastroenterol 19: 118-121.
-
McGuire BM, Cherwitz DL, Rabe KM, Ho SB (1997) Small-cell carcinoma of the lung manifesting as acute hepatic failure. Mayo Clin Proc 72: 133-139.
-
Ke E, Gomez JD, Tang K, Sriram KB (2013) Metastatic small-cell lung cancer presenting as fulminant hepatic failure. BMJ Case Rep 2013: bcr2012007865.
-
Lee WM, Larson AM, Stravitz RT (2011) AASLD Position Paper: The Management of Acute Liver Failure: Update 2011. Alexandria: American Association for the Study of Liver Diseases.
-
Lee WM (2008) Etiologies of acute liver failure. Semin Liver Dis 28: 142-152.
-
Rowbotham D, Wendon J, Williams R (1998) Acute liver failure secondary to hepatic infiltration: a single centre experience of 18 cases. Gut 42: 576-580.
-
Athanasakis E, Mouloudi E, Prinianakis G, Kostaki M, Tzardi M, et al. (2003) Metastatic liver disease and fulminant hepatic failure: presentation of a case and review of the literature. Eur J Gastroenterol Hepatol 15: 1235-1240.
-
Miyaaki H, Ichikawa T, Taura N, Yamashima M, Arai H, et al. (2010) Diffuse liver metastasis of small cell lung cancer causing marked hepatomegaly and fulminant hepatic failure. Intern Med 49: 1383-1386.
-
Kaira K, Takise A, Watanabe R, Mori M (2006) Fulminant hepatic failure resulting from small-cell lung cancer and dramatic response of chemotherapy. World J Gastroenterol 12: 2466-2468.
-
Alexopoulou A, Koskinas J, Deutsch M, Delladetsima J, Kountouras D, et al. (2006) Acute liver failure as the initial manifestation of hepatic infiltration by a solid tumor: report of 5 cases and review of the literature. Tumori 92: 354-357.
-
Heiken JP, Weyman PJ, Lee JK, Balfe DM, Picus D, et al. (1989) Detection of focal hepatic masses: prospective evaluation with CT, delayed CT, CT during arterial portography, and MR imaging. Radiology 171: 47-51.





