Journal of Musculoskeletal Disorders and Treatment
Management of Occupational Shoulder Injuries in Primary Care
Glenn Brown1*, Kayne Park1 and Ryan T Bicknell2
1Department of Family Medicine, Queen's University, Canada
2Department of Surgery and Mechanical and Materials Engineering, Queen's University, Canada
*Corresponding author:
Glenn Brown, Associate professor and Head, Department of Family Medicine, Queen's University, 220 Bagot Street, Kingston, ON K7L 5E9, Tel: 613-533-9300 ext. 73959, Email: glenn.brown@dfm.queensu.ca
J Musculoskelet Disord Treat,
JMDT-1-002, (Volume 1, Issue 1),
Review Article
Received: August 31, 2015: Accepted: September 26, 2015: Published: September 28, 2015
Citation: Brown G, Park K, Bicknell RT (2015) Management of Occupational Shoulder Injuries in Primary Care. J Musculoskelet Disord Treat 1:002
Copyright: © 2015 Brown G. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The shoulder is the most mobile joint in the body and is comprised of an intricate complex of muscles, tendons, and ligaments. Due to thismobility and heavy reliance on arms, shoulder injuries are one of the most debilitating and common disorders afflicted in the workplace. They have been categorized as a high impact injury by the workplace safety and insurance board (WSIB) of Ontario due to the long recovery and return to work (RTW) times. Difficulty diagnosing shoulder injuries due to similar clinical presentations and variability withrange of motion (ROM) testing has led to uncertainty when administering proper treatment and an over reliance on diagnostic imaging. Current standards emphasize taking a thorough patient history, using basic physical examination tests to examine ROM, stability, and strength, and using specialized tests to help determineearly prognostic indicators. Physiotherapy is the first-line treatment for most non-traumatic shoulder injuries as it addresses most repetitive overload disorders commonly found in occupational settings. Analgesics and injections have a role for pain relief but should only be used as a temporary measure. A surgical approach can be considered if there is a specific pathology without red flag indicators but an initial trial of physiotherapy should be recommended. In conjunction with treatment, a patient tailored RTW plan should be developed with information about the injury and preventative measures with an emphasis on early RTW as there is evidence that regular work life promotes positive health benefits.
Keywords
Occupational shoulder injuries, Physical examination, Rotator cuff, Shoulder impingement, Adhesive capsulitis, Traumatic injury, Return to work, Modified work
Introduction
The shoulder joint is the most mobile joint in the human body but sacrifices stability as a result. The rotator cuff muscles, glenoid labrum, and glenohumeral (GH) ligaments provide the majority of stabilization but are prone to natural degeneration and fatigue with age, sports, or work [1,2]. This article will examine common shoulder disorder presentations, diagnosis, treatments, and RTW considerations.
Shoulder injuries are one of the most debilitating disorders commonly found in the workplace. They have been categorized as "high impact" claims, along with lower back injuries and fractures, by the WSIB based on long recovery and RTW times. These three high impact claims account for an average of 40% of all lost time benefit payments and 35% of all lost time claims from 2009 to 2014 with a higher number of average days lost than all other lost time claims from 2010 to 2013. Although the incidence of lost time claims from 2010 to 2014 of low back pain has steadily declined (20.6% to 17.7%), lost time claims from shoulder injuries have remained unchanged (6.4%) [3].
The source of workplace shoulder injuries is multifactorial and involves both physical and psychological factors. Physical factors - manual materials handling, vibration, static postures, work involving hands above shoulders, repetitive motions - are common, well known risks associated with occupational shoulder pain [4,5]. These factors can lead to shoulder pain due to the stress on the muscles and tendons from increased ischemia and inadequate time for rest [6]. These risks along with a patient's age (> 37) and possible psychological factors have shown strong correlations with the onset of shoulder disorders [1,7].
Common shoulder diagnoses covered in this article include rotator cuff disorders (subacromial impingement, partial and full thickness rotator cuff tears), adhesive capsulitis, and trauma-related injuries (GH instabilities and acromioclavicular (AC) disorders). With rotator cuff disorders being most common [8], shoulder disorders are prevalent in primary care and determining the correct diagnosis and treatment method is difficult because of their similar presentations [9]. Correctly identifying a shoulder injury can be done by taking an accurate patient history andappropriate physical examination. Further investigations such as ultrasound, magnetic resonance imaging (MRI), and X-ray are recommended for traumatic injuries, injuries signifying red flags, or uncertain diagnoses [8].
There are a variety of different options to treat shoulder injuries but they are heavily dependent on an accurate diagnosis. The main goal for treating shoulder injuries is to return the patient to regular activities with manageable pain and a functional ROM. Common treatment for shoulder injuriesinclude analgesics, injections, physiotherapy, and surgery. Physiotherapy, with possible analgesics or injections, is the most commonly prescribed treatment for minor shoulder disorders as it is a non-operative means shown to produce good results in patients [10,11]. Surgery is usually only recommended if the patient has reoccurring shoulder dislocations or red flags [8]. Treatment along with a RTW plan can be effective at restoring normal activity for patients.
As the factors affecting the patient at work are multifactorial, a proper RTW plan should take daily activities into account and check for physical and psychological risks. An early RTW plan with activity modificationcan assist with the patient's rehabilitation through social support, financial security, and physical activityto increase the chances for a successful work reintegration [12]. With proper RTW interventions from clinicians and communication between those involved, there is a much greater chance for successful recovery and return to normal activity [12,13].
Shoulder biomechanics
The shoulder being the most mobile joint in the body comprises many different muscles, bones, and ligaments. With most injuries occurring with the rotator cuff muscles (supraspinatus, infraspinatus, subscapularis, and teres minor), understanding their regular function and interaction with the surrounding tissue (ligaments, glenoid labrum, etc...) is key to diagnosing and administering proper treatment.
The scapula comprises the origin of the rotator cuff muscles and glenoid labrum and is used as a base for stabilizing the humeral head [14]. Scapular position is important for maximal force in daily activities. Improper positioning of the scapula (scapular protraction) can affect the internal and external rotation strength of the rotator cuff muscles along with decreasing subacromial space [15].
The rotator cuff muscles main roleis to keep the humeral headcentred andcompressed into the glenoid during dynamic and staticarm movements [2]. Along with this function, they assist the larger muscles (deltoid, pectoralis major, etc...) with abduction (supraspinatus), internal rotation (subscapularis), and external rotation (infraspinatus, teres minor) [14]. Weakness in these muscles from fatigue (repetitive or overhead work) has been shown to shift the humeral head superiorly, increasing the risk for impingement from tendon compression [16].
Another biomechanical factor to consider is the arm position. Arm position and movement greatly effects humeral head movement as shown by Massimini et al. This study demonstrated large anterior/posterior shifts and ligament elongation during 90° shoulder abduction with and without external rotation [17].
Knowledge of the biomechanics involved in shoulder movements can help practitioners determine a correct diagnosis and understand the underlying issues that may cause pain or weakness in shoulder disorders.
Pathophysiology
There are various pathophysiological reasons for the onset of a shoulder disorder. Workplace factorsthat can increase the prevalence are age, type of work, and repetitive/awkward positions [5,6,18]. These factors create opportunity for fatigue and micro trauma from overexertion and overuse of the shoulderand without adequate rest time can increase the risk of ischemia and tendinopathy [6,14,19,20]. Ischemia and rotator cuff tendinopathy, consisting of tendonitis or tendinosis, can affect the repair of collagento increase the risk for further mechanical failure [20,21]. This resulting failure can lead to subacromial impingement and resulting rotator cuff muscle atrophy [2,22].
Muscular imbalance from muscle fatigueas well as awkward positions have been shown to shift the humeral head and cause substantial lengthening of the GH ligaments [16,17]. There are also correlations of acromion shape with rotator cuff damage. Studies have shown associations between acromion shape (particularly type III (hooked) acromion) and rotator cuff tears due to decreased subacromial space and supraspinatus impingement [23,24].
Clinical presentations
The majority of patients presenting with a shoulder injury will have symptoms ranging from pain with specific movements to limited ROM but differentiating these symptoms and determining a diagnosis is a difficult task [8,22]. Taking a thorough patient history, identifying the cause of injury, and conducting ROM tests are the best methods to determine an accurate diagnosis [25].
Patient history
A comprehensive history is the most valuable method for diagnosing patients, as thephysical examination, including specialized tests, can have varying results and should be used as a measure to rule in or rule out a diagnosis [9,25,26]. Patient history should include information about: age, hand dominance, recreational activities, location of pain, onset of pain, and pain at night, duration of pain, when the pain occurs, and severity of pain, past medical history, and family history [8,11]. Practitioners need to remain alert to "red flags" which should be managed by an appropriate specialist. Common red flags include history of cancer with unexplained deformity or sensory deficit, massive/multiple rotator cuff tear, failed shoulder reduction, significant weakness without pain, fever, or epileptic seizure or neurologic sensation after trauma [8,25].
Physical examination
The physical exam begins with a visual inspection to check for any abnormalities of the shoulder region. Abnormalities can be found by palpation and general inspection with the contralateral shoulder for symmetry, deformity, tenderness, redness, crepitus, bruising, atrophy, or swelling [8,11]. Checking the patient's ROM by testing both their active and passive ROM with shoulder abduction/adduction, flexion/extension, and internal/external rotation can show weakness, pain, or stiffness in the shoulder [8,11,25]. Specialized testing can then be used as supplementary information to attempt to isolate the area of pain.
Specialized physical tests
Commonly used tests for detecting injury to specific rotator cuff muscles in rotator cuff tears or impingement are internal/external rotation lag tests, internal/external rotation resistance tests, the empty can test, the drop arm test, the Hawkins-Kennedy test, and the painful arc test. These tests have been created to isolate specific rotator cuff muscles or cause controlled pain.
The internal rotation resistance (Figure 1) and lag (Figure 2) tests examine the subscapularis.
.
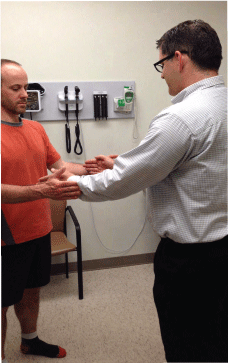
Figure 1: Internal Rotation Resistance Test
The patient flexes the elbow of both arms to 90° with both arms full adducted. The patient attempts to rotate both hands internally, into the stomach, while the clinician resists the internal rotation.
A positive test will show the patient experiencing pain or weakness.
View Figure 1
.
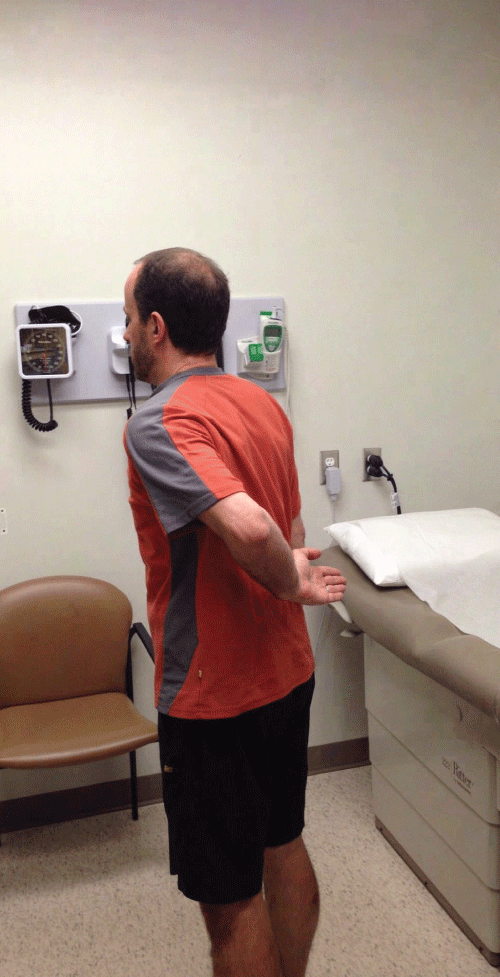
Figures 2: Internal Rotation Lag Test
The patient flexes their elbow 90° and places the back of their hand on their lower back. They then lift the hand off their back and attempt to hold this position.
A positive test is found if they have difficulty holding this position.
View Figures 2
The external rotation resistance (Figure 3) and lag (Figure 4) test the infraspinatus.
.
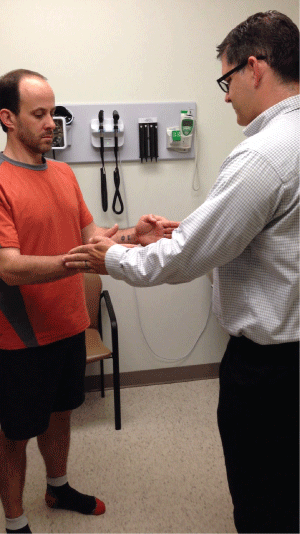
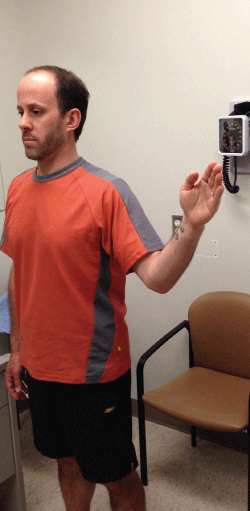
Figure 3: External Rotation Resistance Test
The patient flexes the elbow of both arms to 90° with both arms full adducted. The patient attempts to rotate both hands externally, away from each other, while the clinician resists the external rotation.
A positive test will show the patient experiencing pain or weakness in one arm more than the other.
View Figure 3
.
Figure 4: External Rotation Lag Test
The patient flexes the elbow 90° and abducts their arm 20°. The clinician then externally rotates the arm 90° and the patient attempts to hold this position.
The test is positive if the patient has difficulty holding the externally rotated arm.
View Figure 4
The empty can test (Figure 5) and the drop arm test (Figure 6) check for the supraspinatus.
.
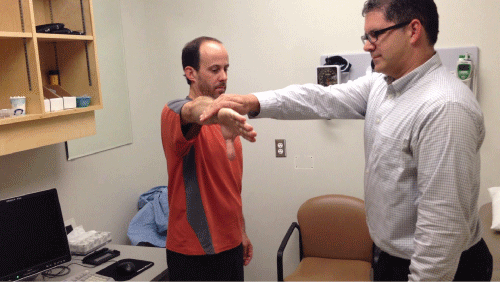
Figure 5: The Empty Can Test
Patient abducts arm 90° then brings the arm forward 30° horizontally. They fully internally rotate and then resist downward force from the clinician.
A positive test is shown with pain or weakness in holding the arm in this position.
View Figure 5
.
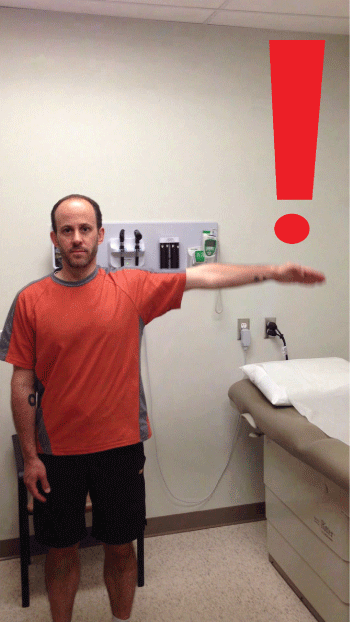
Figure 6: The Drop Arm Test
The arm of the affected shoulder is raised to maximum abduction. The patient then slowly lowers the arm.
A positive test is found if the arm drops after adducting to 90°.
View Figure 6
The Hawkins-Kennedy test (Figure 7) and painful arc test (Figure 8) are used to diagnose for shoulder impingement [27,8].
.
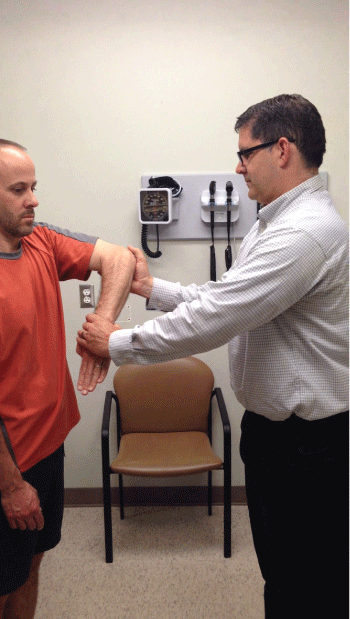
Figure 7: The Hawkins-Kennedy Test
The patient flexes the elbow 90° and then flexes the shoulder 90°. The patient then internally rotates and holds this position. The clinician attempts to further internally rotate the arm.
The test is positive if there is pain experienced during further rotation.
View Figure 7
.
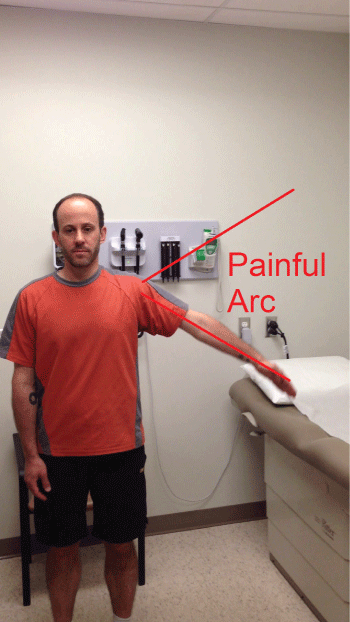
Figure 8: The Painful Arc Test
The patient abducts their arm to 180° from full adduction or vice versa.
The test is positive if the patient experiences pain during 60° to 120° of abduction or adduction.
View Figure 8
Initial measurements of weakness and pain can be conducted with the disabilities of the arm, shoulder, and hand (DASH) or Quick DASH questionnaires to check for improvement in treatments [29].
Diagnosis
Differentiating shoulder disorders is challenging due to the similarity of the symptoms. Factors attributed to differentiating between rotator cuff disorders, adhesive capsulitis, and traumatic injuries are patient history, mechanism of injury, and examinations.
Rotator cuff disorders
Rotator cuff disorders are the most common shoulder disorder and commonly affect people greater than 35 years of age with a higher risk as age increases [8]. Common rotator cuff disorders are shoulder impingement and partial and full thickness rotator cuff tears. They commonly present withatrophy, pain and/or weakness with active movements, and night pain [8,11,25]. Differentiating between impingement and rotator cuff tear is very difficult and highly dependent on the patient's history. This is because rotator cuff tears may be asymptomatic or they could have impingement from an underlying rotator cuff tear [30]. Some indicators for a differential diagnosis can be repetitive motions from overuse in tendinopathy (associated with impingement) or minor trauma for partial/full thickness tears [25,30].
Shoulder impingement is characterized by a decreased subacromial space which causes pinching of the soft tissue (supraspinatus, subacromial bursa, bicep tendon, etc...) between the acromion and humeral head [11]. This can be caused by muscular imbalances of the surrounding tissue resulting in compressive forces on the rotator cuff muscles [2,22]. The main symptom is pain and treatments are designed to reduce subacromial pressure with rotator cuff strengthening [10].
Rotator cuff tears can vary in size from partialtofull thickness tears. Rotator cuff tears are more likely to occur in traumatic events but persistent micro ruptures through sustained positions or repetitive movements can cause enough damage for the rotator cuff tendons to gradually tear, usually the supraspinatus [2,6,8,25]. These partial and full tears can be asymptomatic and differentiating partial or small full thickness tears from tendinopathy can be difficult [8].
Identifying the damaged rotator cuff muscle or differentiating between impingement and tears can be assisted with specialized ROM tests. Studies with strong results have been done to test different combinations of special tests. The Journal of the American Medical Association (JAMA) recommends using one pain provocative test (the painful arc test), three strength tests (internal/external rotation lag tests and the drop arm test), and one composite test (external rotation resistance test or the empty can test) as a general guide for checking which rotator cuff muscle may be damaged [27]. Another study developed a combination of tests to determine shoulder impingement or rotator cuff tear. Testing for impingement used the Hawkins-Kennedy test, painful arc test, and an infraspinatus test, while testing for a full thickness tear used the drop arm test, painful arc test, and an infraspinatus test [28]. There have been good results from these tests but special tests should still be used as an assistive measure for diagnosing a disorder [26].
Adhesive capsulitis
Adhesive capsulitis (frozen shoulder) is an idiopathic onset of pain and ROM restriction due to a contracture of the shoulder capsule that affects people 40-60 of age with a higher prevalence in diabetics [31]. The disorder comes in three stages that, in total, can last approximately two years: the pain stage, the stiffness stage, and then a slow recovery stage [25,31]. The major difference on examination between frozen shoulder and other shoulder disorders is the limited globalactive and passive ROM, particularly in external rotation [25,31]. Specialized physical tests are generally not recommended as they can be difficult to examine appropriately due to the limited global passive ROM. Investigations such as X-ray show normal findings and can be used to exclude other possible disorders (osteoarthritis) that share similar symptoms [31]. In the case of osteoarthritis, frozen shoulder shares similar limited ROM but usually has a history of more gradual pain development [32].
Traumatic injuries
Trauma can be sustained at any age with various different onsets (falls on shoulder, falls with arm extended, dislocation) and can cause an assortment of different diagnoses (rotator cuff tear, GH disorder, AC disorder, fracture). Trauma related injuries are not predominately suffered in occupational settings but improper treatment and the subsequent return to work can affect daily activities and exacerbate symptoms. When examining the patient, appropriate cautions should be taken for the patient when checking ROM and using specialized tests as the area of injury may be susceptible to further damage. Further investigations (X-ray, ultrasound) depending on the history, severity, and physical examination results are usually required to check for serious pathologies [25].
GH disorders (general instability, dislocations) from trauma can include labrum issues (superior labrum anterior to posterior (SLAP) lesions), ligament damage, or fractures. Specialtests for labrum damage have highly varied results and have questionable reliability for assisting in diagnosis [33]. SLAP lesions are best examined with a history of trauma with symptomsconsisting of deep pain on movement, possible popping or locking, and general instability [34].
Labrum damage is also usually accompanied by other shoulder disorders such as rotator cuff tears and ligament damage [34,35]. Issues such as recurrent dislocations are best diagnosed with magnetic resonance arthrography (MRA) and a suspected fracture should be examined with X-ray [25,36].
AC disorders usually result from a fall on the shoulder and can cause subluxation of the AC joint. This disorder has six classifications (type I-VI) based on the amount of soft tissue damage. Types I and II are minor injuries of the AC ligament, while Types III-VI are severe subluxations of the AC joint and surrounding tissue [37]. Palpation of the AC joint by checking for tenderness, deformity, and compromised adduction can be indicative of AC disorders [11]. Further investigations (X-ray) may be required for suspected Type III or greater AC disorders [25].
Traumatic injuries are easily identified by patient history and the mechanism of injury but the resulting damage to the shoulder can be multi layered. Asymptomatic or minor trauma resulting in normal shoulder function should have an examination done with recommendation for X-ray to check for underlying bone damage. Highly debilitating traumatic injuries should be recommended to the correct specialist.
Investigations
Common investigations for shoulders include X-ray, MRI, MRA, and ultrasound [11]. Traumatic injuries should be investigated with X-ray to check for suspected bone damage or red flags while MRI and MRA should generally only be recommended if there are indications for surgery [22]. Although they are important for diagnosis and have high sensitivity and specificity, they are often overused in primary care when investigating patients that have injuries that can be treated conservatively [8,11,22,38] (Table 1).
![]()
Table 1: Major differential factors commonly present in rotator cuff disorder, adhesive capsulitis, and traumatic injury.
View Table 1
Treatment
The key to administering treatment to patients with shoulder injuries is determining a correct diagnosis. Once accurately diagnosed, the corresponding treatment can be recommended and the patient can begin healing. Common treatments for shoulder disorders include analgesics, injections, physiotherapy, and surgery.
Analgesics may be advised if the patient is experiencing severe pain but should only be recommended as a short term measure or used in conjunction with physiotherapy [8,22]. Possible recommendations include simple analgesics (paracetamol), non-steroidal anti-inflammatory drugs (NSAIDs), or corticosteroid injections but with strong attention to possible side effects for elderly or diabetic people [8,22,25].
Physiotherapy is usually the first treatment recommended to patients with non-traumatic shoulder disorders as it is a relatively inexpensive non-invasive method that can address key mechanical problems of the shoulder [11,39]. It can be administered in different forms such as exercise, stretching, and shockwave therapy. Exercise is usually advised as the main physiotherapy treatment as it can be done primarily at home, with correct guidance from a physiotherapist, it is readily available and can be done at any time.
A surgical approach should be considered only if the patient has evident red flags, traumatic events, or has failed conservative measures [8,11]. Orthopaedic surgeon referral may be recommended for young and active patients with traumatic injuries or severe rotator cuff damage but there is evidence that asymptomatic full thickness rotator cuff tears can be managed conservatively through physiotherapy [25,40].
Rotator cuff disorders
Treatment for rotator cuff disorders should look to reduce pain and return normal function by correcting the muscular imbalances causing impingement or tears [11]. Analgesics or injections and physiotherapy should be recommended to help correct mechanical issues [8,11].
Strengthening the rotator cuff muscles creates a stronger compression of the humeral head into the glenoid labrum and reduces the natural superior shift of the humeral head by the deltoid [11,16]. Unless there is severe rotator cuff damage or conservative measures have failed, surgery is usually not recommended [11].
Some exercise recommendations based on maximum voluntary isometric contraction (MVIC) for rotator cuff strengthening exercises include [41,42]:
• standing external rotation (infraspinatus, teres minor, supraspinatus)
• side lying external rotation (deltoid, infraspinatus, teres minor, supraspinatus)
• standing internal rotation (subscapularis, pectoralis major, latissimus dorsi)
• 90° shoulder abducted internal rotation (subscapularis, supraspinatus)
• standing abduction (supraspinatus, deltoid)
Along with exercise, high energy extracorporeal shock-wave therapy (ESWT) may be recommended as it has shown strong evidence with tissue regeneration and calcium deposit resorption forrotator cuff damage due to calcific tendinosis, while low energy ESWT has shown some evidence for short term pain relief in non-calcific tendinosis [43,44].
Adhesive capsulitis
Although the treatment goals of reduced pain and normal ROM are the same in each treatment method, treating adhesive capsulitis is a controversial issue [31,45]. Corticosteroid injections, with consideration of side effects, can be used to greatly reduce pain in the first stage and, in conjunction with light pendulum exercises and stretching, can be an effective non-operative treatment for increasing ROM [31]. If physiotherapy does not show significant improvement, manipulation under anaesthesia may be considered as it has been shown to have good efficacy for pain relief and restoration of motion but has been associated with complications, including humeral fracture and injury to the rotator cuff [31,45,46,47]. Arthroscopic release has also shown promising results with relief of pain and improvement in motion and is becoming more common for the treatment of frozen shoulder with potentially higher success and a lower complication rate compared with manipulation under anaesthesia [31,45,46].
Traumatic injuries
Treating traumatic injuries depends on the severity and area affected. Trauma involving minor injuries of the rotator cuff and AC joint can usually be treated non-operatively with physiotherapy and analgesia similar to rotator cuff disorders [8]. Major injuries resulting in significant weakness, suspected red flags, or minor injuries that fail conservative treatment will benefit from referral for possible surgery [25].
A key to successful treatment is regular follow-up. Patients should be seen in follow-up no later than four to six weeks after initial assessment to check their progress. Considerations based on the patient's progress should be to reduce analgesics depending on the pain, increase the intensity of the physiotherapy if ROM and pain improve, or refer to an orthopaedic surgeon if initial measures fail [11].
Return to work
There are numerous physical and psychological factors to consider when developing a successful RTW plan for patients. A comprehensive RTW plan should educate the patient on the basics of their shoulder injury, understand and suggest modificationsfor the patient's daily work activities, and establish proper communication with the patient, employer, and other possible health care professionals about the importance of returning to work. The RTW plan should also promote an early RTW as there is an association between increased time away from work and never returning to work [12]. Returning to work has been shown to have an overall positive health benefit and should be the main concern after a complete diagnosis and treatment routine has been developed [48].
Education
Informing the patient of their injury and potential preventative measures can be effective in keeping them healthy at work. Some topics of discussion can be about their injury, using good biomechanics for tasks (lifting, pushing, pulling), and practicing proper posture. Teaching the patient about their injury and why the injury occurred can help them learn how to avoid further injury and about the importance of keeping the rotator cuff muscles active and healthy. They can even adapt the knowledge learned in the clinic torecreational activities to further promote rotator cuff health.
Education about compromising positions (working above the shoulders, awkward external/internal rotation, etc...) during strenuous activity can be helpful as a preventative measure. These positions should be actively avoided and the workplace modified in order to eliminate these aggressors. Good form such as lifting objects closer to the body, using larger muscle groups (chest, legs), or emphasising the use of readily available workplace tools during occupational activities are some tips that can reduce risk of injury in the shoulder [49]. Posture is animportant factor to consider as well. The patient should focus on neutral scapular position during work as a protracted scapula has been shown to reduce rotator cuff rotation strength, which can lead to overexertion [15].
Work modification
To reduce risk and prevent further injury, workplace hazards should be identified and modifications should be made at work to return the patient to work early and facilitate physical healing and social support. Physical factors that have been associated with shoulder disorders include manual materials handling, vibration, static postures, work involving hands above shoulders, and repetitive motions while the psychological factors such as psychological job demands, job satisfaction, low work control, and lack of social support can also have debilitating effects on work [4,5,8,22]. Everyday work activities of the patient should be examined by the practitioner and recommendations should be made to reduce the activities mentioned earlier. Some adjustments for common aggressors can be to reduce weight when lifting by lifting several smaller loads, using step stools to keep overhead work to a minimum, and to vary tasks by using their non-dominant arm with neutral scapular posture [49]. If possible, direct workplace examinations should be taken to assist with the RTW process. These interventions show strong evidence of successful returns to work. A study conducted by Cheng and Hung [13], demonstrated significant improvement in RTW rates of individuals trained at their workplacewith assistance from a job coach compared to basic clinic-based work training and modifications. By determining the hazards within the workplace and in daily work activities, recommendations can be made for the patient to return to a modified work environment and to their regular familiar routine.
Communication
Communication between the healthcare provider, employer, patient, and the relevant worker's compensation board is essential for a successful RTW. Identifying the risk factors mentioned earlier and making sure that they are addressed with the people involved in keeping the patient healthy is important [49,50]. The patient's workplace should be appropriately modified to reduce shoulder aggressors. Communication should be ongoing to monitor progress and address any issues that further aggravate physical (increased pain, weakness) or psychological (low job satisfaction, low social support) symptoms [50].
Conclusion
The shoulder complex is a very mobile joint but can be prone to mechanical failure and an approach to treatment can be a difficult process. Shoulder disorders can be detrimental to a patient's work life and can greatly affect basic daily activity. An accurate patient history, conducting a thorough physical examination, and identifying workplace hazards are essential for creating a patient specific treatment and RTW plan. Returning to work early with knowledge of their injury and open communication with the people involved can facilitate continued healing and a return to regular activity.
References
-
Cassou B, Derriennic F, Monfort C, Noton J, Touranchet A (2002) Chronic neck and shoulder pain, age, and working conditions: longitudinal results from a large random sample in France. Occup Environ Med 59: 537-544.
-
Page P (2011) Shoulder Muscle Imbalance and Subacromial Impingement Syndrome in Overhead Athletes. Int J Sports Phys Ther 6: 51-58.
-
WSIB (2015) By The Numbers: 2014 WSIB Statistical Report - Schedule 1.
-
Mayer J, Kraus T, Ochsmann E (2012) Longitudinal evidence for the association between work-related physical exposures and neck and/or shoulder complaints: a systematic review. Int Arch Occup Environ Health 85: 587-603.
-
van der Windt DA, Thomas E, Pope DP, de Winter AF, Macfarlane GJ, et al. (2000) Occupational risk factors for shoulder pain: a systematic review. Occup Environ Med 57: 433-442.
-
Hagberg M (1984) Occupational musculoskeletal stress and disorders of the neck and shoulder: a review of possible pathophysiology. Int Arch Occup Environ Health 53: 269-278.
-
Bugajska J, Zolnierczyk-Zreda D, Jedryka-Goral A, Robert Gasik, Katarzyna Hildt-Ciupinska, et al. (2013) Psychological factors at work and musculoskeletal disorders: a one year prospective study. Rheumatol Int 33: 2975-2983.
-
Mitchell C, Adebajo A, Hay E, Carr A (2005) Shoulder pain: diagnosis and management in primary care. BMJ 331: 1124-1128.
-
van der Windt DA, Koes BW, Boeke AJ, Deville W, De Jong BA, et al. (1996) Shoulder disorders in general practice: prognostic indicators of outcome. Br J Gen Pract 46: 519-523.
-
Hanratty CE, McVeigh JG, Kerr DP, Basford JR, Finch MB, et al. (2012) The effectiveness of physiotherapy exercises in subacromial impingement syndrome: a systematic review and meta-analysis. Semin Arthritis Rheum 42: 297-316.
-
Greenberg DL (2014) Evaluation and treatment of shoulder pain. Med Clin North Am 98: 487-504.
-
(2011) Realising the health benefits of work. A position statement. The Australasian Faculty of Occupational & Environmental Medicine.
-
Cheng AS, Hung LK (2007) Randomized controlled trial of workplace-based rehabilitation for work-related rotator cuff disorder. J Occup Rehabil 17: 487-503.
-
Reid D (1992) Sports Injury Assessment and Rehabilitation. Churchill Livingstone, New York, USA.
-
Smith J, Dietrich CT, Kotajarvi BR, Kaufman KR (2006) The effect of scapular protraction on isometric shoulder rotation strength in normal subjects. J Shoulder Elbow Surg 15: 339-343.
-
Chopp JN, O'Neill JM, Hurley K, Dickerson CR (2010) Superior humeral head migration occurs after a protocol designed to fatigue the rotator cuff: a radiographic analysis. J Shoulder Elbow Surg 19: 1137-1144.
-
Massimini DF, Boyer PJ, Papannagari R, Gill TJ, Warner JP, et al. (2012) In vivo glenohumeral translation and ligament elongation during abduction and abduction with internal and external rotation. J Orthop Surg Res 7: 29.
-
Brewer BJ (1979) Aging of the rotator cuff. Am J Sports Med 7: 102-110.
-
Sommerich CM, McGlothlin JD, Marras WS (1993) Occupational risk factors associated with soft tissue disorders of the shoulder: a review of recent investigations in the literature. Ergonomics 36: 697-717.
-
Bass E (2012) Tendinopathy: Why the Difference Between Tendinitis and Tendinosis Matters. Int J Ther Massage Bodywork 5: 14-17.
-
Riley G, Harrall R, Constant C, Chard M, Cawston T, et al. (1994) Tendon degeneration and chronic shoulder pain: changes in the collagen composition of the human rotator cuff tendons in rotator cuff tendinitis. Ann Rheum Dis 53: 359-366.
-
Shanahan EM, Sladek R (2011) Shoulder pain at the workplace. Best Pract Res Clin Rheumatol 25: 59-68.
-
Mohamed RE, Abo-Sheisha DM (2014) Assessment of acromial morphology in association with rotator cuff tear using magnetic resonance imaging. The Egyptian Journal of Radiology and Nuclear Medicine 45: 169-180.
-
Toivonen DA, Tuite MJ, Orwin JF (1995) Acromial structure and tears of the rotator cuff. J Shoulder Elbow Surg 4: 376-383.
-
(2004) The Diagnosis and Management of Soft Tissue Shoulder Injuries and Related Disorders: Best Practice Evidence-Based Guideline. The New Zealand Guidelines Group.
-
Hegedus EJ, Goode A, Campbell S, Morin A, Tamaddoni M, et al. (2008) Physical examination tests of the shoulder: a systematic review with meta-analysis of individual tests. Br J Sports Med 42: 80-92.
-
Hermans J, Luime JJ, Meuffels DE, Reijman M, Simel DL, et al. (2013) Does this patient with shoulder pain have rotator cuff disease?: The Rational Clinical Examination systematic review. JAMA 310: 837-847.
-
Park HB, Yokota A, Gill HS, El Rassi G, McFarland EG (2005) Diagnostic accuracy of clinical tests for the different degrees of subacromial impingement syndrome. J Bone Joint Surg Am 87: 1446-1455.
-
Gummesson C, Ward MM, Atroshi I (2006) The shortened disabilities of the arm, shoulder and hand questionnaire (QuickDASH): validity and reliability based on responses within the full-length DASH. BMC Musculoskelet Disord 7: 44.
-
Ostor AJ, Richards CA, Prevost AT, Speed CA, Hazleman BL (2005) Diagnosis and relation to general health of shoulder disorders presenting to primary care. Rheumatology (Oxford) 44: 800-805.
-
Lewis J (2015) Frozen shoulder contracture syndrome - Aetiology, diagnosis and management. Man Ther 20: 2-9.
-
Seth A (2014) Thawing the frozen shoulder. InnovAiT 7: 421-427.
-
Cook C, Beaty S, Kissenberth MJ, Siffri P, Pill SG, et al. (2012) Diagnostic accuracy of five orthopedic clinical tests for diagnosis of superior labrum anterior posterior (SLAP) lesions. J Shoulder Elbow Surg 21: 13-22.
-
Nam EK, Snyder SJ (2003) The diagnosis and treatment of superior labrum, anterior and posterior (SLAP) lesions. Am J Sports Med 31: 798-810.
-
Habermeyer P, Gleyze P, Rickert M (1999) Evolution of lesions of the labrum-ligament complex in posttraumatic anterior shoulder instability: a prospective study. J Shoulder Elbow Surg 8: 66-74.
-
Bencardino JT, Beltran J, Rosenberg ZS, Rokito A, Schmahmann S, et al. (2000) Superior labrum anterior-posterior lesions: diagnosis with MR arthrography of the shoulder. Radiology 214: 267-271.
-
Mazzocca AD, Arciero RA, Bicos J (2007) Evaluation and treatment of acromioclavicular joint injuries. Am J Sports Med 35: 316-329.
-
Buchbinder R, Staples MP, Shanahan EM, Roos JF (2013) General practitioner management of shoulder pain in comparison with rheumatologist expectation of care and best evidence: an Australian national survey. PLoS One 8: e61243.
-
Marinko LN, Chacko JM, Dalton D, Chacko CC (2011) The effectiveness of therapeutic exercise for painful shoulder conditions: a meta-analysis. J Shoulder Elbow Surg 20: 1351-1359.
-
Kuhn JE, Dunn WR, Sanders R, An Q, Baumgarten KM, et al. (2013) Effectiveness of physical therapy in treating atraumatic full-thickness rotator cuff tears: a multicenter prospective cohort study. J Shoulder Elbow Surg 22: 1371-1379.
-
Reinold M, Wilk K, Fleisig G, Zheng N, Barrentine S, et al. (2004) Electromyographic Analysis of the Rotator Cuff and Deltoid Musculature During Common Shoulder External Rotation Exercises. J Orthop Sports PhysTher 34: 385-394.
-
Decker MJ, Tokish JM, Ellis HB, Torry MR, Hawkins RJ (2003) Subscapularis muscle activity during selected rehabilitation exercises. Am J Sports Med 31: 126-134.
-
Bunker T, Smith C (2014) Frozen Shoulder. European Surgical Orthopaedics and Traumatology 1185-1199.
-
Huisstede BM, Gebremariam L, van der Sande R, Hay EM, Koes BW (2011) Evidence for effectiveness of Extracorporal Shock-Wave Therapy (ESWT) to treat calcific and non-calcific rotator cuff tendinosis--a systematic review. Man Ther 16: 419-433.
-
Galasso O, Amelio E, Riccelli DA, Gasparini G (2012) Short-term outcomes of extracorporeal shock wave therapy for the treatment of chronic non-calcific tendinopathy of the supraspinatus: a double-blind, randomized, placebo-controlled trial. BMC Musculoskelet Disord 13: 86.
-
Uppal HS, Evans JP, Smith C (2015) Frozen shoulder: A systematic review of therapeutic options. World J Orthop 6: 263-268.
-
Loew M, Heichel TO, Lehner B (2005) Intraarticular lesions in primary frozen shoulder after manipulation under general anesthesia. J Shoulder Elbow Surg 14: 16-21.
-
Waddell G, Burton AK (2006) Is Work Good for Your Health and Well-being? The Stationary Office, London.
-
(2007) Occupational Health and Safety Council of Ontario (OHSCO). Part 3A: MSD Prevention Toolbox - Getting Started. Musculoskeletal Disorders (MSDs) Prevention Series.
-
(2012) Shoulder Program of Care: Reference Guide. WSIB.