Journal of Musculoskeletal Disorders and Treatment
Use of CD-ROMS for Digital Image Viewing During New Pediatric Orthopaedic Consults - Do We Need a Standardized Viewer for Digital Imaging?
Czoch Wojciech1, William Hennrikus2, Alexander Kish2* and Douglas Armstrong2
1Department of Orthopaedic Surgery, University of Virginia School of Medicine, USA
2Department of Orthopaedics, Penn State College of Medicine, USA
*Corresponding author: Alexander J Kish, Department of Orthopaedics, Penn State College of Medicine, 30 Hope Drive, Hershey, PA 17033 USA, Fax: 717-531-0216, Tel: 717-531-7006, E-mail: alexanderjkish@gmail.com
J Musculoskelet Disord Treat, JMDT-2-006, (Volume 2, Issue 1), Research Article
Received: November 26, 2015: Accepted: January 29, 2016: Published: February 01, 2016
Citation: Wojciech C, Hennrikus W, Kish A, Armstrong D (2016) Use of CD-ROMS for Digital Image Viewing During New Pediatric Orthopaedic Consults - Do We Need a Standardized Viewer for Digital Imaging?. J Musculoskelet Disord Treat 2:006
Copyright: © 2016 Wojciech C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The purpose of this study is to perform a practice management evaluation of CD-ROM imaging. Thirty-three patients who presented with images on a CD-ROM before and 33 patients after the addition of DICOM software were compared. Data collected included; site of origin of the CD-ROM, time in minutes spent to access the images, number of computers tried until images were viewed, cases of failure to view the images, quality of the images on a Likert 1-5 scale, and the need to repeat images. Prior to the application of DICOM software, average time to access the images was 16 minutes; average number of computers needed was 2 (range 1-4). Image quality averaged 2.8. Repeat images were needed in seven cases. After introduction of the DICOM software the average time to view the images was 3.5 minutes; average number of computers needed was 1 (range 1-2). The image quality averaged 3.8. Repeat images were indicated in 5 cases. Advances in computer software including the DICOM viewer can improve workflow, physician productivity and potentially patient satisfaction. Despite our use of advanced computer software, 3 CD-ROMS (9%) were unreadable. Standardization of software for digital imaging is needed.
Introduction
Patients routinely present for a new consultation to the pediatric orthopaedic clinic with digitalized images on multimedia CD-ROMs obtained from outside institutions [1]. This digital imaging technique can potentially be more time consuming for the physician in clinic trying to view the images on a computer than conventional radiology film. Software incompatibility that exists between medical centers creates an obstacle in medical record keeping [2]. The CD-ROMs from outside systems contain DICOM reader programs, which vary from vendor-to-vendor. It is the variation in these reader programs that cause difficulty for the receiving clinic. One study has shown greater than 25% of outside images brought in by patients on CD-ROM are not compatible with the host institution, leading to unnecessary re-imaging to confirm a diagnosis [3]. In an effort to streamline sharing of medical imaging, the Digital Imaging and Communications in Medicine (DICOM) standard was created by the National Electric Manufacturers Association. This uses a single, standard file format that can be uploaded to any computer with the proper imaging software and allows both patient information in the form of a header, and imaging data in viewable form to be accessible at the same time. The purpose of this study is to perform a practice management comparison of CD-ROM imaging before and after our department purchased Digital Imaging and Communications in Medicine (DICOM) viewer software (DICOM, Rosslyn, VA) to help load outside images into our GE Picture Archiving and Communications System (PACS).
Materials and Methods
Two pediatric orthopaedic surgeons, who regularly see patients with outside images, aggregated data on their experience with CD-ROMs and PACS. Thirty-three consecutive patients who presented to the pediatric orthopaedic clinic for a new consult with images on a CD-ROM before and thirty-three consecutive patients after the addition of DICOM viewer software to our GE Centricity Imagecast 2012 PACS system were compared. Data collected for each patient included the site of origin of the CD-ROM, the time in minutes spent by the surgeon trying to access the images (measured by wristwatch), the number of computers tried until images were successfully viewed (each exam room is equipped with one computer, additionally there are several networked workstations available to the surgeons), any cases of failure to view the images, the quality of the images rated on a 1-5 Likert scale by the pediatric orthopaedic surgeon (5 - excellent quality, 3 - sufficient for diagnosis, 1 - poor/unreadable quality), image modality (X-ray, MRI, CT), the need to take repeat images at our clinic, whether a radiology report was included on the imaging disc, and the final diagnosis. Descriptive statistics were used in the analysis. Images from any CD-ROM were stored on a webserver and deleted after 2 years per hospital protocol. This study was approved by the Penn State College of Medicine IRB.
Results
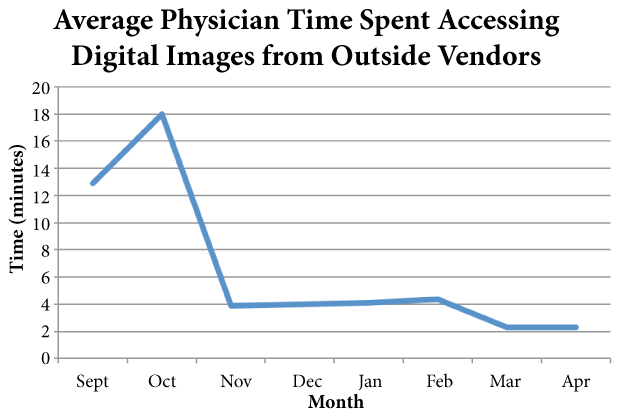
Prior to the application of the DICOM viewer software to our PACS the average time to access the images was sixteen minutes (range 2-35 minutes), the average number of computers that the disc was placed into until successful viewing of the images was two (range 1-4). The images could be viewed on the first attempted computer in only eight cases (24.2%). The quality of the images averaged 2.8 (range 1-4). A radiology report was included with the CD-ROM in eight cases. Images included twenty-six radiographs, seven MRIs, and two CTs. In seven cases, repeat images were indicated due to inability to view the images on the CD-ROM (3 cases) and poor image quality (4 cases). The most common orthopaedic issue diagnosed on the digital images was a fracture, ten cases (30%). Figure 1 shows the monthly average time invested into image retrieval by the physician throughout the course of the study. Images originated from 20 hospitals.
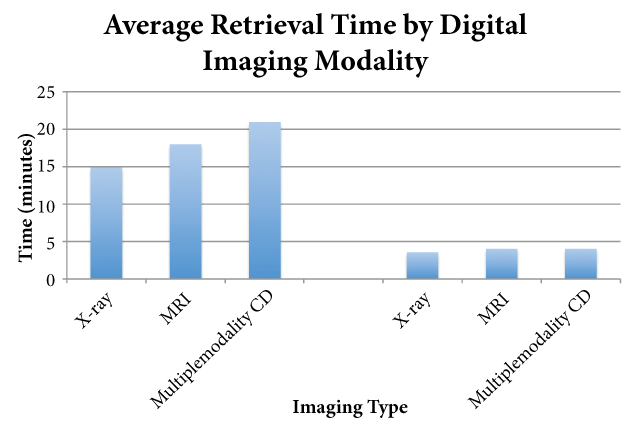
After introduction of the DICOM software to the PACS system, the average time to view the images was 3.5 minutes - an average reduction in time of 12.5 minutes (range 2-40 minutes). In 90% of cases, the digital images were successfully retrieved and accessed on the first attempted computer. In only three cases were additional computers needed to view time images. The quality of the images averaged 3.8 (range 1-4). A radiology report was included in only one case. Images included twenty-four X-rays and thirteen MRIs. Repeat images were indicated in five cases: three cases of inability to view images and two cases of poor image quality. The most common diagnosis was fracture, in ten cases (30%). Images originated from 17 outside hospitals. The five unreadable disks in the study originated from five different outside institutions (Figure 2, Table 1).
.
Figures 2: Shows the time to retrieve the image based on type of image before and after introduction of DICOM software.
View Figures 2
![]()
Table 1: Results before and after DICOM introduction.View Table 1
Discussion
Most hospitals now use digital imaging. Greater than 91% of physicians prefer digital imaging to film but the transfer of digital imaging between hospitals can be challenging due to incompatibility of computer software [4]. Currently the trend is to exchange digital imaging via CDs because they are easy for hospitals to create and for patients to transport between facilities [2]. Transfer of images via the Internet may be the next advance in image exchange; however today, concerns about privacy of network transfer and HIPPA violations have prevented this practice. The current study focuses on efficacy and practical issues when using CD-ROM based images in the outpatient orthopaedic clinic.
In the outpatient orthopaedic clinic, obstacles exist when using a computer system to view digital images. For example, storage of images on CD-ROM also has incompatibility issues. One challenge in the exchange of information via CD-ROM from other institutions is errors of information. Erickson reported that when using CD-ROM to share images, about 1% of CD-ROMs have an incorrect patient name, 1% of CD-ROMs are unreadable after multiple attempts on multiple computers, 1% has data for the wrong patient, and 1% has data for more than one patient [2]. Sending a disk with the wrong patient information or with information of two patients is a HIPAA violation and carries consequences for the hospital under the Patient Safety and Quality Improvement Act of 2005.
Storage of patient information on CD-ROMs also poses a problem for the hospital system. If the host institution decides to keep the actual CD-ROM in a filing system as backup, an optimal storage environment must be created that keeps the disks in a dark room, with a constant temperature of 25°C, and 40% humidity [5]. The study by Stinson et al. showed that 95% of CD-ROMs stored under these optimal conditions will have a shelf life of 217 years, but van Ooijen demonstrated that at an average of 9.5 years, 2% of the CD-ROMs randomly sampled had disk read errors that led to loss of data [5,6]. In the current study, seven disks (21.1%) were unreadable prior to the advent of the DICOM imaging software. However, even after utilization of modern imaging software three disks (9%) were still unreadable by our computer system at presentation in our clinic.
Today, multiple computer systems and software companies are competing for the medical market. Incompatibility between software systems is common. The transfer of images on CD-ROMs can lead to incompatibility. Although most CD-ROMs are equipped with a dedicated viewer, these viewers are different per vendor and thus, users need to learn to operate many different software packages. Some of the software packages require installation on the local workstation, but installation is not always possible due to security reasons [7]. Reports and information other than images are not included in many CD-ROMs. In the current study only nine of sixty-six CD-ROMs included a report. Some vendors have radiology reports on their CD-ROMs in text files in different formats that are not readable by all computers.
Many physicians view digital imaging as an advance in the field of radiology; however, some orthopaedic surgeons view digital imaging as a nuisance [8,9]. For example, Juenemann published an elegant study examining the time it takes for orthopaedic residents to read conventional radiographs compared with digital radiographs [9]. Ten sets of six X-rays were prepared on print film and in digital format on CD-ROMs. The computer was turned on, no password was needed, and the same viewing software was used on all digital images. Six senior level orthopaedic residents were tested. Time in seconds needed to read the radiographs were measured. The evaluation of conventional radiographs took twenty-one seconds (range 14-29 seconds) while reading the digital images took ninety seconds (range 63-117 seconds) (P < 0.001). Digital images took an average of sixty-nine seconds longer compared to standard radiographs. Juenemann concluded that, despite ideal conditions, the use of digital images had a negative impact on the economics and logistics of daily practice [9]. Dr. Juenemann does not suggest turning back the clock of time and use only conventional x-rays; rather, Dr. Juenemann recommends that improvements need to be made in software systems to speed up the process. The present study included images that originated from thirty different hospitals or emergency rooms. In only 16% of the cases, the digital images were successfully viewed by the pediatric orthopaedic surgeon on the first computer tried. Prior to the utilization of DICOM imaging software, the time to load and view the images on CD-ROM averaged sixteen minutes (2-35 minutes). Following introduction of DICOM imaging software the time to load and view images improved to 3.5 minutes (2-40 minutes). We did not compare the time to view standard images in this study. The time needed for review of digital images depends on the computer system, the software, and the origin of the CD-ROM. The five unreadable disks in the study originated from five different outside institutions.
Multiple studies in both the emergency and family practice settings have shown that increased wait times leads to decreased Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) score and decreased perceived quality of care [10-12]. Picture Archiving and Communication System (PACS), a standard digital platform used across many medical centers, was implemented in our department as a major step towards the upgrade of the outpatient setting [4]. The implementation of the DICOM viewer improved the abilities of our PACS to read outside CD-ROMs. Workflow, physician productivity, and potentially patient satisfaction also improved. In the current study, the new DICOM software decreased wait times by 12 minutes.
The improvement in time occurred for CD-ROMs containing either X-rays or MRI. Furthermore, after implementation of DICOM imaging, almost all images could be viewed on the first attempted computer. In addition, Erickson suggested using a CD support person at the check-in desk to load the CDS and confirm accurate information [2]. We have implemented this practice since the conclusion of this study.
Conclusion
Digital imaging and PACS have gained wide acceptance for handling of radiology studies in clinical practice. However, many patients are referred with prior exams recorded on CD-ROMs. The handling of these exams can be difficult due to variations in the software used to decode and display images. To remedy this, clinics, hospitals and medical centers have introduced centralized handling of CD-ROMs where the disks are read and copied to the PACS system by a small number of trained staff rather than burdening the busy clinicians who attend to the referral patients with this task. The current study demonstrates that advances in computer software including the DICOM viewer can improve workflow and physician productivity. However, despite the use of the DICOM viewer, three CD-ROMs (9%) were still unreadable by our PACS and these images could not be viewed. Standardization of software between all vendors of digital imaging systems is clearly needed. Although digital images minimize processing and storage issues common with film, additional advances in digital radiology technology must evolve before one can conclude that patient care and physician productivity are optimized in the outpatient pediatric orthopaedic clinic when using CD-ROM images.
Study Limitations
This study has multiple limitations including; small sample size, single clinic and PACS system, small number of observers, and use of subjective measures for image quality.
References
- van Ooijen PM, Roosjen R, de Blecourt MJ, van Dam R, Broekema A, et al. (2006) Evaluation of the use of CD-ROM upload into the PACS or institutional web server. J Digit Imaging 19 Suppl 1: 72-77.
- Erickson BJ (2011) Experience with importation of electronic images into the medical record from physical media. J Digit Imaging 24: 694-699.
- Sodickson A, Opraseuth J, Ledbetter S (2011) Outside imaging in emergency department transfer patients: CD import reduces rates of subsequent imaging utilization. Radiology 260: 408-413.
- Chan L, Trambert M, Kywi A, Hartzman S (2002) PACS in private practice--effect on profits and productivity. J Digit Imaging 15 Suppl 1: 131-136.
- Stinson D, Ameli F, Zaino N (1995) Lifetime of KODAK writable CT and photo CD media, Eastman Kodak Company.
- van Ooijen PM, Viddeleer AR, Meijer F, Oudkerk M (2010) Accessibility of data backup on CD-R after 8 to 11 years. J Digit Imaging 23: 95-99.
- van Ooijen PM, Guignot J, Mevel G, Oudkerk M (2005) Incorporating out-patient data from CD-R into the local PACS using DICOM worklist features. J Digit Imaging 18: 196-202.
- Wade FA, Oliver CW (2004) Living with digital imaging. Clin Orthop Relat Res: 25-28.
- Juenemann S, Hasler C, Brunner R (2009) Digital imaging data on CD-R: a time trap for orthopaedic surgeons in outpatient clinics. J Child Orthop 3: 59-62.
- Bleustein C, Rothschild DB, Valen A, Valatis E, Schweitzer L, et al. (2014) Wait times, patient satisfaction scores, and the perception of care. Am J Manag Care 20: 393-400.
- Trout A, Magnusson AR, Hedges JR (2000) Patient satisfaction investigations and the emergency department: what does the literature say? Acad Emerg Med 7: 695-709.
- Howard M, Agarwal G, Hilts L (2009) Patient satisfaction with access in two interprofessional academic family medicine clinics. Fam Pract 26: 407-412.