Journal of Musculoskeletal Disorders and Treatment
Medial Epicondylitis and Medial Elbow Pain Syndrome: Current Treatment Strategies
Christina Brady and Anil Dutta*
Department of Orthopedic Surgery, University of Texas Health Sciences Center San Antonio, USA
*Corresponding author:
Anil Dutta, Associate Professor, Department of Orthopedic Surgery, University of Texas Health Sciences Center San Antonio, USA, Tel: 210 567-5135, E-mail: duttaA@uthscsa.edu
J Musculoskelet Disord Treat, JMDT-2-014, (Volume 2, Issue 2), Review Article
Received: February 25, 2016: Accepted: May 31, 2016: Published: June 03, 2016
Citation: Brady C, Dutta A (2016) Medial Epicondylitis and Medial Elbow Pain Syndrome: Current Treatment Strategies. J Musculoskelet Disord Treat 2:014.
Copyright: © 2016 Brady C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use,
distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Medial elbow pain is a common complaint in the active population. The most frequent muscular or tendinous condition to cause medial elbow pain is Medial Epicondylitis (ME). The disorder is classically described as "Golfer's elbow" due its association with elbow pain caused by excessive eccentric force across the common flexor origin encountered during the golf swing. In the working population, the condition is frequently associated with repetitive use and is seen in manual laborers who require forceful wrist flexion and pronation along with grasping. Medial Epicondylitis is frequently accompanied by additional medial sided elbow pathology such as ulnar neuritis, ulnar collateral ligament injury, flexor pronator strain, and snapping medial triceps. Treatment is directed towards addressing tendon degeneration at the common flexor tendon origin. The mainstay of treatment is non-operative with stretching, rest, activity modification, therapy, and injections. Intermediate techniques include extracorporeal shockwave therapy (ECSW), ultrasound (US), platelet-rich-plasma (PRP) injections, and newer techniques of ultrasound guided fasciectomy. Surgical treatments are tailored to the severity of the pathoanatomy and need to be inclusive of concomitant pathology. The patient who presents with medial elbow complaints requires a broad differential diagnosis. It is appropriate to consider medial epicondylitis a primary etiology within the larger concept of "Medial Elbow Pain Syndrome" as the presence of ME does not exclude other origins of medial elbow pain.
Keywords
Medial epicondylitis, Ulnar neuritis, Flexor pronator strain, Cubital tunnel syndrome
Abbreviations
ME: Medial Epicondylitis, CFT: Common Flexor Tendon, US: Ultrasound, ECSW: Extracorporeal Shockwave Therapy, UCL: Ulnar Collateral Ligament, PT: Pronator Teres, FCR: Flexor Carpi Radialis, FCU: Flexor Carpi Ulnaris, PL: Palmaris Longus, PRP: Platelet Rich Plasma
Introduction
While Medial Epicondylitis (ME) classically is described in golfers; it is a common condition and frequently found in the setting of manual laborers and individuals who require repetitive use of the elbow, forearm, and wrist [1,2]. The medial epicondyle is the origin of the common flexor tendon (CFT), which includes the pronator teres (PT), the palmaris longus (PL), the flexor carpi radialis (FCR), and flexor carpi ulnaris (FCU). The mechanism of injury is largely eccentric loading of the flexed and pronated forearm, accompanied by valgus stress to the elbow. While most patients ultimately respond to non-operative treatment, it can be a disabling and chronic condition. Refractory cases may require surgical treatment. ME has a particularly close relationship to pathology of the ulnar nerve and the presence of ulnar nerve symptoms impact treatment and prognosis. It is critical to identify variations in presentation and address additional pathologies particularly during surgical intervention. As such, in many ways the diagnosis of ME should be made within the larger paradigm of medial elbow pain and its variations.
Epidemiology
Medial Epicondylitis is significantly less common than lateral epicondylitis with lateral epicondylitis reported at up to 10 times as frequently [3]. ME typically occurs in the 4th to 6th Decade of life and is a common occupational disorder [3]. The prevalence is 0.3 to 1.1% with a slightly higher prevalence in women [4]. In the labor force the prevalence can be as high as 5% [5]. Comparatively, medial-sided elbow pain from cubital tunnel syndrome is common in athletes, manual laborers, and workers exposed to repetitive motion. The incidence of cubital tunnel syndrome is quite high and is reported at a rate of 0.8% per person year in laborers [6-8].
Pathology
Medial Epicondylitis involves degenerative changes at the common flexor tendon (CFT), but more specifically involves the pronator teres and the flexor carpi radialis. The pronator teres humeral head origin off the medial conjoined tendon has been implicated as the focal point for the development of ME [9].
Clinical presentation
Typical symptoms are pain along the origin of the common flexor tendon with repetitive wrist flexion, pronation, and valgus stress. Patients may complain of night pain and pain at rest. Clinical presentation shows hyperextension of the wrist or pronation with wrist flexion against resistance can reproduce symptoms along the medial epicondyle. Testing of the cubital tunnel involves elbow flexion and direct pressure on the ulnar nerve. It is important to evaluate for any sensory loss in the ulnar digits or intrinsic weakness in more severe cases.
Classification
Medical Epicondylitis is classified into 2 major subtypes: Type 1 with no ulnar involvement and Type 2: with ulnar nerve involvement. The prognosis for Type 2 ME is worse than the prognosis for Type I and it is for this reason that careful diagnosis and treatment of patients with ulnar nerve symptoms frequently determines outcome [10] (Table 1).
![]()
Table 1: Classification of Medial Epicondylitis [9].
View Table 1
Additional Causes of Medial Elbow Pain
There are many potential causes of medial elbow pain. As such, it is important to include a differential diagnosis. In addition, it is not uncommon for more than one diagnosis to be present at the same time and management must be inclusive of these different elements to be optimal.
Cubital tunnel syndrome/ulnar neuritis
The ulnar nerve is frequently involved in the diagnosis of ME and has a major impact on the prognosis, especially with surgical treatment [10,11]. Cubital tunnel is seen frequently in occupational settings much like medial epicondylitis [6]. The diagnosis of Cubital Tunnel syndrome is made based on clinical symptoms of medial elbow pain with sensitivity in the ulnar nerve distribution. Physical exam findings include a positive Tinel's at the elbow, decreased sensation on Semmes-Weinstein testing, and a positive MacKinnon Test [12]. The "Scratch Test" can be used to determine the location of compression. This is done by scratching differential locations and then resisting shoulder external rotation. Loss of shoulder external rotation strength is considered positive [13]. Motor changes manifest with weakness of interosseous hand muscles, adductor pollicus, and the ulnar lumbrical muscles. EMG/NCV can be confirmatory, but can be negative even in the presence of disease [14]. Attention should also be given to a proximal site of nerve compression. C6 and C7 radiculopathy have been shown to predispose to medial epicondylitis resulting from muscle weakness [15].
Ulnar collateral ligament instability
Injury to the ulnar collateral ligament of the elbow may result in isolated symptoms of pain or frank instability complaints. The UCL is the primary restraint to valgus stress to the elbow. This diagnosis should be considered in the setting of prior elbow dislocation and in overhead athletes such as baseball pitchers who expose the elbow to extreme valgus stress while throwing [16]. Valgus instability in 20 degrees of extension and a positive "Milking Test" or "Moving Valgus Stress Test" [17] along with MRI findings of disruption typically at the ligaments origin are confirmative. Successful reconstruction for the symptomatic patient has been reported with the classical "Tommy John procedure" [18,19].
Flexor pronator strain
The flexor pronator muscle tendon unit can be a source of pain with overuse. Athletes experience high stress during the acceleration phase of throwing [20]. Repetitive stress can result in microtears at the interface of the PT and the FCR. Common sites of strain include the humeral head of the PT, the FCR and the FCU [21,22].
Snapping triceps/Anconeus epitrochlearis
The medial head of the triceps may develop a pattern of "snapping" spontaneously or after surgery [23]. The mechanical symptoms of subluxation can cause pain in isolation. Subluxation of the ulnar nerve can mimic triceps subluxation and should be distinguished. The medial head of the triceps can also cause compression of the ulnar nerve with hypertrophy as seen in weight lifters or in patients with an accessory epitrochleanconeus muscle [24,25]. Resection of the anconeus epitrochlearis has shown to resolve the symptoms [26].
Medial antebrachial cutaneous nerve entrapment
The medial antebrachial cutaneous (MABC) nerve can be an independent source of medial elbow pain with neuropathic symptoms of paresthesia, hypersensitivity, or burning. The MABC can also be present in concert with ulnar neuritis. MABC entrapment has been described after prior surgical procedures, and particular attention must be given to this possibility after prior cubital tunnel release [27,28]. The presentation can also mimic snapping medial triceps with mechanical catching of the nerve with elbow motion [29].
Imaging/Diagnostic Testing
Plain radiographs may demonstrate sclerotic changes along the medical epicondyle in cases of long standing disease. An AP and Lateral X-ray are also necessary to rule out alternate diagnoses including medial epicondyle fracture, elbow arthritis, and deformity. Ultrasound has been described to identify tendon degeneration and areas of hypoechoic tissue. Ultrasound can also be used as an adjuvant for guided injections or tissue modulation. MRI is most sensitive and will demonstrate additional damage to the ulnar collateral ligament and ulnar nerve. EMG/NCV adds specificity to the diagnosis and is indicated when ulnar nerve pathology is suspected.
Non-Operative Treatment
Mainstay of treatment is non-operative management of medial epicondylitis. This includes rest, NSAIDs, and physical therapy. This has been reported to be 60 to 90% effective in treating symptoms [30]. Rehabilitation exercises should emphasize stretching of the CFT. This includes wrist supination and extension with the elbow hyper extended. Progressive eccentric strengthening constitutes restoration of the muscle-tendon unit. If a patient does not improve with non-operative treatments, steroid injections and night splinting can be considered. Steroids provide short term relieve of symptoms, specifically pain. However, these effects may not endure long-term [31]. Additionally, the side effects should not be disregarded, including atrophy of the skin and subcutaneous fat tissue with exacerbation of symptoms [32].
Intermediate Treatments
Extracorporeal shockwave therapy (ecswt)
ECSWT has been reported as a potential option for definitive treatment of tendinopathy [33,34]. It was originally introduced to medicine for kidney or common bile duct stone disintegration. Its medical uses have been expanded to include tendinopathy, but the information is currently limited regarding efficacy. ECSWT may be a good alternative when steroid injections are not a viable option. In patients with newly diagnosed medial epicondylitis, initial ESWT is effective for treating symptoms. However, when compared to steroids, steroids provide better initial relief [33]. In other studies, including a randomized control in the setting of lateral epicondylitis, ECSWT proved no improvement when compared to placebo [34]. This may highlight the natural improvement of symptoms frequently seen with medial epicondylitis.
Other injections (PRP/Prolotherapy)
Other injections have been described in the non-operative treatment of medial and lateral epicondylitis including platelet-rich-plasma (PRP) and prolotherapy. PRP is an autologous biological blood-derived product with concentrated platelet-derived growth factors that would ideally enhance healing. In comparison to steroid injections, PRP has shown to be more efficacious in the long term improvement of symptoms in lateral epicondylitis [35]. This finding was also seen in other kinds of tendinopathy [36]. Prolotherapy refers to injecting an irritant, usually hyperosmolar dextrose ormorhuate sodium directly surrounding a tendon or into a joint space. This has thought to initiate healing from the secondary growth factors from an induced inflammatory response. In chronic tendinopathies promising results of efficacy of treatment with results up to 1 year have been reported [37].
Focused tissue aspiration (FAST)
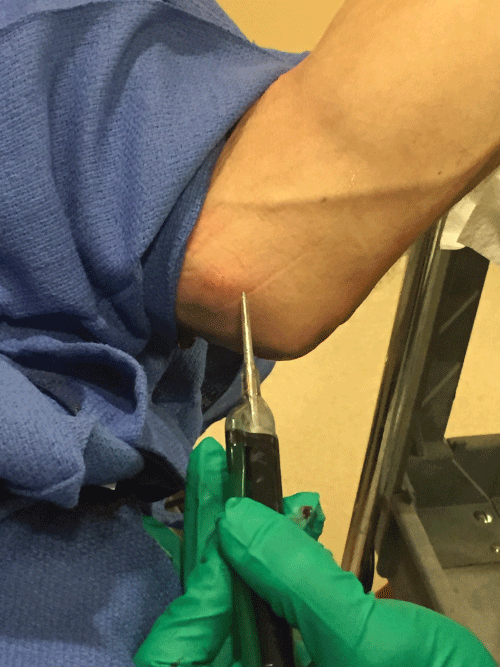
FAST is a technique utilized to accomplish fasciotomy. The technique is a recent innovation in the treatment of ME. An ultrasound probe set at a frequency which is ablative of damaged tissue is applied via US guidance. The damaged tissue is then aspirated out of the patented probe system (Tenex, Rochester, MN) (Figure 1). There have been no reported complications after over 100 procedures. As such this technique may offer a promising alternative to invasive open procedures particularly in patients with Type I ME with minimal nerve involvement. The technique takes advantage of defining the damaged tissue as hypoechoic on ultrasound. FAST technology has proven successful showing 95-100% satisfaction and follow-up studies showing resolution of the hypoechoic tissue [38,39].
Surgical Management
There are number of open surgical options for the treatment of medial epicondylitis. The following procedures are commonly employed and the indications are based on the co-pathologies. It is critical that additional pathologies outlined previously are not neglected. The surgical treatment of those conditions can be included within the scope of any of the procedures described.
Percutaneous release
Simple percutaneous release has shown good results and can be performed in the office setting [40]. However, it runs the risk of complete detachment of the flexor pronator origin and damage to the MABC and ulnar nerve. The procedure can be supplemented with ultrasound guidance [41].
Medial epicondylectomy
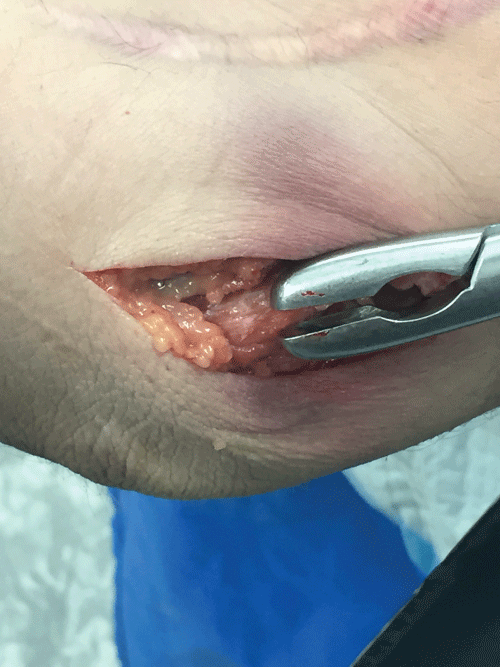
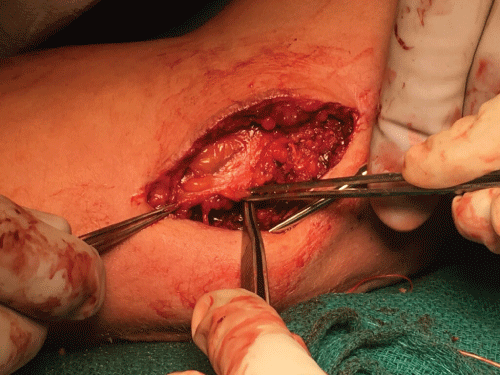
The results of medial epicondylectomy are fairly predictable in the setting of Type IA medial epicondylitis [9,11,42,43]. The elbow is exposed via a small medial incision and care is taken to protect superficial nerves. The CFU is split along the lines of its fibers and the medial epicondyle is exposed. The medial conjoint tendon and the zone of the origin of the FCR and the humeral head of the PT are developed. The degenerative tissue is removed and a portion of the medial epicondyle is removed as necessary (based on its prominence). Care must be taken to not cause iatrogenic subluxation of the ulnar nerve in this process or subluxation of the medial triceps. Some authors have advocated suture anchor repair of the flexor pronator mass [44]. More commonly, the flexor pronator can be repaired over the removed degenerative tissue through bone tunnels (Figure 2).
Medial epicondylectomy with in-situ ulnar nerve release
The medial epicondyle is exposed in the same fashion as in procedure II, but the ulnar nerve is fully exposed via a release of the Osborne's ligament. The medial intermuscular septum is released at the origin of the FCU to ensure full decompression of the ulnar nerve. Simple oblique epicondylectomy is a more extensive removal of the medial epicondyle that can be performed for decompression of the ulnar nerve. The continuum between simple fascial release and epicondylectomy is based on surgeon judgment and preference. The result of simple epicondylectomy alone in athletes has not been shown to be reliable [45]. The nerve is maintained in its position unless it demonstrates evidence of anterior subluxation, in which case an anterior transposition may be indicated. Considerable evidence exists that in the setting of an index procedure for decompression of the ulnar nerve, there is no difference in simple release versus a more extensive transposition procedure [46-49].
Medial epicondylectomy with subcutaneous ulnar nerve transposition
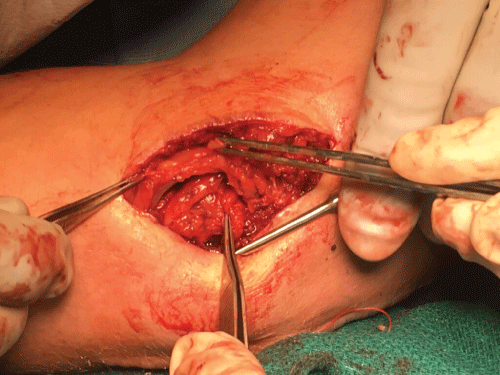
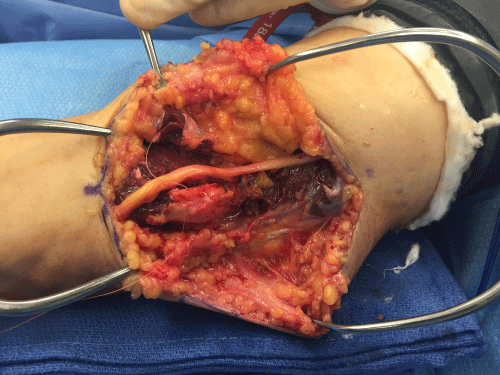
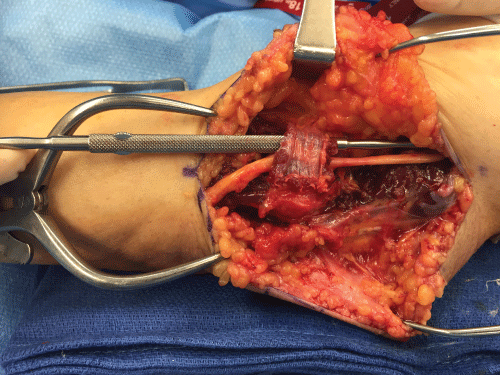
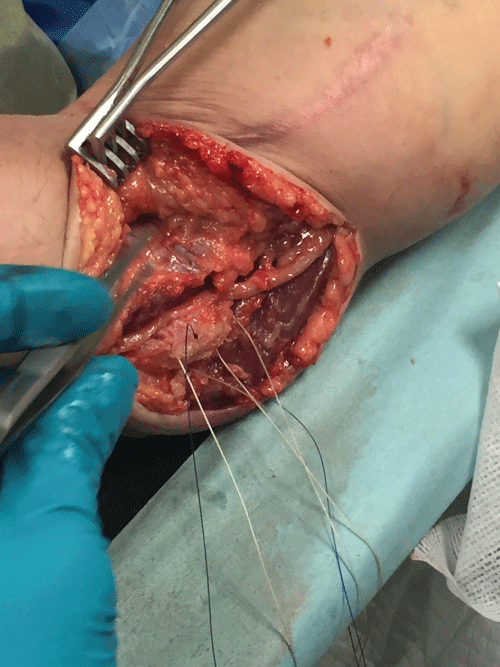
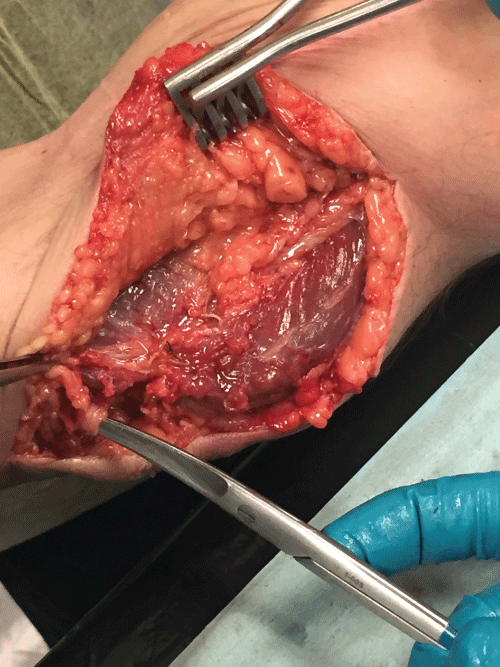
The medial epicondyle is exposed and debrided with minimal release of the CFT as described in procedure I. The ulnar nerve is fully exposed and released, then transposed anteriorly. A fascial sling is used to maintain the ulnar nerve in an anterior position over the flexor pronator fascia. The CFT is repaired over the medial epicondyle as described in Procedure I. When the ulnar nerve is unstable, the transposition is clearly indicated. Care must be taken to release all sites of compression including the Arcade of Struthers, the intermuscular septum, Osborne's ligament, and the flexor carpi ulnaris (Figure 3 and Figure 4).
Medial epicondylectomy with flexor pronator z- lengthening
The standard technique of submuscular anterior nerve transposition requires the nerve to be positioned underneath the elevated flexor pronator mass. The concern for this technique is the potential pressure of the restored flexor pronator mass on the ulnar nerve [50]. The technique of flexor pronator Z-lengthening provides the benefits of a muscular protective layer over the anterior positioned ulnar nerve without the negative effects of scarring and excessive pressure on the nerve created by the standard submuscular transposition [51] (Figure 5 and Figure 6).
Medial epicondylectomy with submuscular ulnar nerve transposition
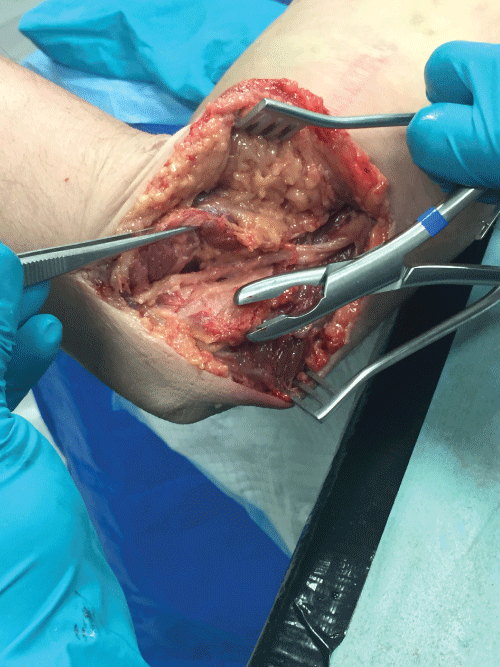
The authors consider this the most aggressive technique for treatment of refractory medial epicondylitis as they often employ this technique after failed prior surgery. Anterior transposition of the ulnar nerve is recommended in the setting of failed prior ulnar nerve surgery [49]. The addition of a full fascial release of the flexor pronator origin and removal of the prominent medial epicondyle is the most comprehensive surgical treatment in these refractory cases (Figure 7, Figure 8 and Figure 9).
References
-
Amin NH, Kumar NS, Schickendantz MS (2015) Medial epicondylitis: evaluation and management. J Am Acad Orthop Surg 23: 348-355.
-
Bennett JB (1994) Lateral and medial epicondylitis. Hand Clin 10: 157-163.
-
Descatha A, Dale AM, Jaegers L, Herquelot E, Evanoff B (2013) Self-reported physical exposure association with medial and lateral epicondylitis incidence in a large longitudinal study. Occup Environ Med 70: 670-673.
-
Shiri R, Viikari-Juntura E (2011) Lateral and medial epicondylitis: role of occupational factors. Best Pract Res Clin Rheumatol 25: 43-57.
-
Descatha A, Leclerc A, Chastang JF, Roquelaure Y; Study Group on Repetitive Work (2003) Medial epicondylitis in occupational settings: prevalence, incidence and associated risk factors. J Occup Environ Med 45: 993-1001.
-
Descatha A, Leclerc A, Chastang JF, Roquelaure Y; Study Group on Repetitive Work (2004) Incidence of ulnar nerve entrapment at the elbow in repetitive work. Scand J Work Environ Health 30: 234-240.
-
da Costa JT, Baptista JS, Vaz M (2015) Incidence and prevalence of upper-limb work related musculoskeletal disorders: A systematic review. Work 51: 635-644.
-
Mondelli M, Giannini F, Ballerini M, Ginanneschi F, Martorelli E (2005) Incidence of ulnar neuropathy at the elbow in the province of Siena (Italy). J Neurol Sci 234: 5-10.
-
Gabel GT, Morrey BF (2009) Medial Epicondylitis the Elbow and its Disorders 4th Edition. 643-649.
-
Gabel GT, Morrey BF (1995) Operative treatment of medical epicondylitis. Influence of concomitant ulnar neuropathy at the elbow. J Bone Joint Surg Am 77: 1065-1069.
-
Kurvers H, Verhaar J (1995) The results of operative treatment of medial epicondylitis. J Bone Joint Surg Am 77: 1374-1379.
-
Novak CB, Lee GW, Mackinnon SE, Lay L (1994) Provocative testing for cubital tunnel syndrome. J Hand Surg Am 19: 817-820.
-
Cheng CJ, Mackinnon-Patterson B, Beck JL, Mackinnon SE (2008) Scratch collapse test for evaluation of carpal and cubital tunnel syndrome. J Hand Surg Am 33: 1518-1524.
-
Tapadia M, Mozaffar T, Gupta R (2010) Compressive neuropathies ofthe upper extremity: update on pathophysiology, classification, and electrodiagnostic findings. J Hand Surg Am 35: 668e677.
-
Lee AT, Lee-Robinson AL (2010) The prevalence of medial epicondylitis among patients with c6 and c7 radiculopathy. Sports Health 2: 334-336.
-
Schwab GH, Bennett JB, Woods GW, Tullos HS (1980) Biomechanics of elbow instability: the role of the medial collateral ligament. Clin Orthop Relat Res: 42-52.
-
O'Driscoll SW, Lawton RL, Smith AM (2005) The "moving valgus stress test" for medial collateral ligament tears of the elbow. Am J Sports Med 33: 231-239.
-
Jobe FW, Stark H, Lombardo SJ (1986) Reconstruction of the ulnar collateral ligament in athletes. J Bone Joint Surg Am 68: 1158-1163.
-
Rohrbough JT, Altchek DW, Hyman J, Williams RJ 3rd, Botts JD (2002) Medial collateral ligament reconstruction of the elbow using the docking technique. Am J Sports Med 30: 541-548.
-
Hamilton CD, Glousman RE, Jobe FW, Brault J, Pink M, et al. (1996) Dynamic stability of the elbow: Electromyographic analysis of the flexor pronator group and the extensor group in pitchers with valgus instability. J Shoulder Elbow Surg 5: 347-354.
-
Davidson PA, Pink M, Perry J, Jobe FW (1995) Functional anatomy of the flexor pronator muscle group in relation to the medial collateral ligament of the elbow. Am J Sports Med 23: 245-250.
-
Chen FS, Rokito AS, Jobe FW (2001) Medial elbow problems in the overhead-throwing athlete. J Am Acad Orthop Surg 9: 99-113.
-
Spinner RJ, Gabel GT (2001) Latrogenic snapping of the medial head of the triceps after ulnar nerve transposition. J South Orthop Assoc 10: 236-240.
-
Gervasio O, Zaccone C (2008) Surgical approach to ulnar nerve compression at the elbow caused by the epitrochleoanconeus muscle and a prominent medial head of the triceps. Neurosurgery 62: 186-192.
-
Spinner RJ, Wenger DE, Barry CJ, Goldner RD (1999) Episodic snapping of the medial head of the triceps due to weightlifting. J South Orthop Assoc 8: 288-292.
-
Li X, Dines JS, Gorman M, Limpisvasti O, Gambardella R, et al. (2012) Anconeus epitrochlearis as a source of medial elbow pain in baseball pitchers. Orthopedics 35: e1129-1132.
-
Dellon AL, MacKinnon SE (1985) Injury to the medial antebrachial cutaneous nerve during cubital tunnel surgery. J Hand Surg Br 10: 33-36.
-
Masear VR, Meyer RD, Pichora DR (1989) Surgical anatomy of the medial antebrachial cutaneous nerve. J Hand Surg Am 14: 267-271.
-
Cesmebasi A, O'driscoll SW, Smith J, Skinner JA, Spinner RJ (2015) The snapping medial antebrachial cutaneous nerve. Clin Anat 28: 872-877.
-
Ciccotti MC, Schwartz MA, Ciccotti MG (2004) Diagnosis and treatment of medial epicondylitis of the elbow. Clin Sports Med 23: 693-705.
-
Stahl S, Kaufman T (1997) The efficacy of an injection of steroids for medial epicondylitis. A prospective study of sixty elbows. J Bone Joint Surg Am 79: 1648-1652.
-
Beyzadeoglu T, Bekler H, Gokce A (2011) Skin and subcutanous fat atrophy after corticosteroid injection for medial epicondylitis. Orthopedics 34: 570.
-
Lee SS, Kang S, Park NK, Lee CW, Song HS, et al. (2012) Effectiveness of initial extracorporeal shock wave therapy on the newly diagnosed lateral or medial epicondylitis. Ann Rehabil Med 36: 681-687.
-
Haake M, König IR, Decker T, Riedel C, Buch M, et al. (2002) Extracorporeal shock wave therapy in the treatment of lateral epicondylitis : a randomized multicenter trial. J Bone Joint Surg Am 84-84A: 1982-1991.
-
Peerbooms JC, Sluimer J, Bruijn DJ, Gosens T (2010) Positive effect of an autologous platelet concentrate in lateral epicondylitis in a double-blind randomized controlled trial: platelet-rich plasma versus corticosteroid injection with a 1-year follow-up. Am J Sports Med 38: 255-262.
-
Coombes BK, Bisset L, Vicenzino B (2010) Efficacy and safety of corticosteroid injections and other injections for management of tendinopathy: a systematic review of randomised controlled trials. Lancet 376: 1751-1767.
-
Distel LM, Best TM (2011) Prolotherapy: a clinical review of its role in treating chronic musculoskeletal pain. PM R 3: S78-81.
-
Seng C, Mohan PC, Koh SB, Howe TS, Lim YG, et al. (2016) Ultrasonic Percutaneous Tenotomy for Recalcitrant Lateral Elbow Tendinopathy: Sustainability and Sonographic Progression at 3 Years. Am J Sports Med 44.
-
Koh JS, Mohan PC, Howe TS, Lee BP, Chia SL, et al. (2013) Fasciotomy and surgical tenotomy for recalcitrant lateral elbow tendinopathy: early clinical experience with a novel device for minimally invasive percutaneous microresection. Am J Sports Med 41: 636-644.
-
Baumgard SH, Schwartz DR (1982) Percutaneous release of the epicondylar muscles for humeral epicondylitis. Am J Sports Med 10: 233-236.
-
Barnes DE, Beckley JM, Smith J (2015) Percutaneous ultrasonic tenotomy for chronic elbow tendinosis: a prospective study. J Shoulder Elbow Surg 24: 67-73.
-
Ollivierre CO, Nirschl RP, Pettrone FA (1995) Resection and repair for medial tennis elbow. A prospective analysis. Am J Sports Med 23: 214-221.
-
Vinod AV, Ross G (2015) An effective approach to diagnosis and surgical repair of refractory medial epicondylitis. J Shoulder Elbow Surg 24: 1172-1177.
-
Grawe BM, Fabricant PD, Chin CS, Allen AA, DePalma BJ, et al. (2016) Clinical Outcomes After Suture Anchor Repair of Recalcitrant Medial Epicondylitis. Orthopedics 39: e104-107.
-
Osei DA, Padegimas EM, Calfee RP, Gelberman RH (2013) Outcomes following modified oblique medial epicondylectomy for treatment of cubital tunnel syndrome. J Hand Surg Am 38: 336-343.
-
Zlowodzki M, Chan S, Bhandari M, Kalliainen L, Schubert W (2007) Anterior transposition compared with simple decompression for treatment of cubital tunnel syndrome. A meta-analysis of randomized, controlled trials. J Bone Joint Surg Am 89: 2591-2598.
-
Dellon AL (1989) Review of treatment results for ulnar nerve entrapment at the elbow. J Hand Surg Am 14: 688-700.
-
Gervasio O, Gambardella G, Zaccone C, Branca D (2005) Simple decompression versus anterior submuscular transposition of the ulnar nerve in severe cubital tunnel syndrome: a prospective randomized study. Neurosurgery 56: 108-117.
-
Gabel GT, Amadio PC (1990) Reoperation for failed decompression of the ulnar nerve in the region of the elbow. J Bone Joint Surg Am 72: 213-219.
-
Dellon AL (2001) Clinical grading of peripheral nerve problems. Neurosurg Clin N Am 12: 229-240.
-
Dellon AL, Coert JH (2004) Results of the musculofascial lengthening technique for submuscular transposition of the ulnar nerve at the elbow. J Bone Joint Surg Am 86-86A Suppl 1: 169-179.