Journal of Musculoskeletal Disorders and Treatment
Mechanical Fatigue Analysis Comparing Two Locking Plates in a Metaphyseal Fracture Model of the Distal Ulna
M Brodbeck1*, A Spiegel2, J Hunt1 and J Gruenert1
1Department of Hand, Plastic and Reconstructive Surgery, Kantonsspital St. Gallen, Switzerland
2Medartis AG research laboratory, Basel, Switzerland
*Corresponding author:
Michael Brodbeck, Department of Hand, Plastic and Reconstructive Surgery Kantonsspital St. Gallen, Rorschacherstrasse 95, 9000 St. Gallen, Switzerland, Tel: +41 71 494 93 64, E-mail: michael.brodbeck@kssg.ch
J Musculoskelet Disord Treat, JMDT-2-018, (Volume 2, Issue 3), Research Article
Received: April 06, 2016; Accepted: August 12, 2016; Published: August 16, 2016
Citation: Brodbeck M, Spiegel A, Hunt J, Gruenert J (2016) Mechanical Fatigue Analysis Comparing Two Locking Plates in a Metaphyseal Fracture Model of the Distal Ulna. J Musculoskelet Disord Treat 2:018.
Copyright: © 2016 Brodbeck M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The purpose of the study was to test the mechanical fatigue properties (fatigue limit and fatigue strength) of two locking plates designed for the distal ulna. Distal Ulna Plate 2.5 (Medartis, Basel, Switzerland) and 2.0 mm LCP Distal Ulna Plate (DePuySynthes, West Chester (PA), USA) were used. A metaphyseal fracture situation was chosen (AO 23-A1.3). Six plate-screw constructs of each design were mounted on custom made fixtures using a Sawbone's 3D ulna model. Testing was performed on monoaxial material testing machines. Endpoints were fatigue strength (load) and fatigue limit (cycles) when the sample fails. Initial load was set at Fmax 10 N. Sinusoidal loading was carried out at 4 Hz. After 50'000 cycles load was increased by 15% and again by 15% after each additional 10'000 cycles. 2.5 mm plates showed median fatigue strength of 40.5 N (range 5.3) and median fatigue limit of 141'307 cycles (range 5'436). 2.0 mm plates 13.2 N (range 5.2) and 67'287 cycles (range 28'718) respectively. Distal Ulna Plate 2.5 showed better mechanical properties.
Keywords
Distal ulna, Fracture, Plate, Fatigue
Introduction
Isolated distal ulnar fractures are extremely rare, but they are much more common in combination with a distal radius fracture. Fractures of the ulnar distal metaphysis are less common and occur in 6% (19/320) of distal radius fractures [1].
In the literature there is still controversy whether these fractures affect wrist function after operative fixation of the distal radius, given that distal ulnar fractures may lead to chronic instability of the distal radio-ulnar joint. These concerns are related to the fact that the radio-ulnar ligaments are primary stabilizers of the distal radio-ulnar joint and attach to the base of the ulnar styloid [2,3]. In addition to the risk of instability McKee et al. reported an association of distal radius fracture nonunion with ulna fracture in elderly women [4].
For displaced metaphyseal distal ulna fractures rates of union exceed 96% with proper fixation techniques [5]. Currently there is no clear evidence that one method of fixation or even operative versus nonoperative treatment is superior in the treatment of distal ulnar shaft and metaphyseal fractures [6]. On the other hand fracture reduction and fixation is indicated for mid and distal ulna shaft fractures with a displacement of more than 50% and angulation greater than 10°. Such fractures may imply disruption of the interosseous membrane (IOM) and cause longitudinal instability of the forearm [7].
Many different plates for open reduction and internal fixation of unstable ulna fractures have been developed and the use of locked plates has become very common. Several studies have shown biomechanical advantages of this technique especially in osteoporotic bone and in metaphyseal fractures [8,9]. A recent biomechanical study by Collins et al. could however not show any clear advantage of locked plating for fractures of the distal ulna [10].
The aim of this study was to test the mechanical properties (fatigue strength and fatigue limit) of two titanium-alloy locking plates commonly used and designed for distal ulnar fractures. Given the high rates of nonunion and instability associated with this injury we hypothesized that stronger mechanical strength of internal fixation would ensure enough time for bony union to occur.
Materials and Methods
Specimen preparation
Two different plates that cover the same indications were compared in our test; a simple fracture model (see Test Set-Up explained below) was employed. In our clinic we use the Distal Ulna Plate 2.5 (Medartis, Basel, Switzerland). For comparison we chose the 2.0 mm LCP Distal Ulna Plate (DePuySynthes, West Chester (PA), USA) since it is also a locking plate. Both plates are made from titanium-alloy and indicated for distal ulnar fixation. The detailed specifications are given in table 1. Only the short Medartis plate (46 mm) was used in current study.
![]()
Table 1: Plate specifications.
View Table 1
Testing was performed on monoaxial material testing machines Thelkin (Winterthur, Switzerland) and Zwick-Roell (Ulm, Germany) at the Medartis AG research laboratory in Basel (Switzerland). Fatigue strength was defined as the load at which failure occurs, whereas the fatigue limit was defined as the number of load cycles when the sample fails.
The plates were mounted on the fracture model according to the manufacturer supplied surgical techniques [11,12]. Six plate-screw constructs were tested each.
Test set-up
The designs of the various subject plates, including their shapes and dimensions, precluded static and dynamic testing as described in ASTM F382 - Standard Specification and Test Method for Metallic Bone Plates [13] which describes a simple four-point bend test. Instead, a test set-up was chosen according to the following criteria:
• Loading of the plate must be based on an in-vivo loading scenario.
• The set-up must also represent a worst case scenario of loading to replicate possible outcomes.
• Design must not favour one plate design over another.
Accordingly a system test simulating a comminuted metaphyseal fracture situation without ‘bony support' was chosen. This type of fracture is named as an AO 23-A1.3 fracture or a Q3 fracture in combination with a distal radial fracture in the most frequently cited AO Comprehensive Classification System [14]. Fractures of the distal ulna associated with fractures of the distal radius are classified according to a Q modifier [15]. This setup is considered to be clinically relevant, biomechanically unfavourable (i.e., worst case) and highly reproducible.
The actual set-up is shown in figure 1: Six plate-screw constructs of each design were mounted lateral (ulnar) on custom-made fixtures (Figure 2) using Sawbone's Inc.'s (Vashon Island, Washington) 3D ulna model. Using CAD software the models were modified to include clamping and load transfer points, the osteotomy as well as drill holes; additionally, the model was ‘hollowed out' to represent the cortical part of the bone only. Fixtures were then printed in glass fiber-reinforced polyamide using rapid prototyping technology and the central cavity filled with polyurethane foam to simulate cancellous bone. Load is transferred at a defined distance from the proximal fragment using a parallel and a ball bearing to minimize shear forces (Figure 1, marks 2 and 3). To make sure that plate, screw and locking mechanism are all tested, a distance of 1 mm was maintained between plates and substrate in the distal fragment (Figure 2, right). By maintaining the point of load transfer at a fixed distance from the proximal fragment for all tests and independent of the hardware used, identical bending moments are guaranteed. Screw-hole usage is based on fracture location and company-provided literature [11,12] (Figure 2).

.
Figure 1: Test set-up with clamped sample. (1) parallel; (2) ball bearing; (3) Arrow indicates the monoaxial (radial-ulnar) load application.
View Figure 1

.
Figure 2: Samples mounted for test. top: Medartis plate, bottom: DePuySynthes plate.
View Figure 2
Testing protocol
Based on the plates' indication we assume that the maximum time of load bearing varies somewhere between 6 and 12 weeks after which the bone should have consolidated; typically, bony consolidation is expected within 6 weeks post-operatively [16]. This time roughly corresponds to 50'000-100'000 load cycles (assuming a recuperating person performs 500-1'000 load cycles per day).
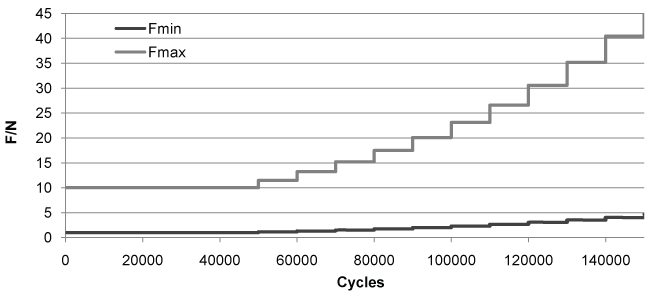
Based on preliminary tests the initial load for fatigue testing was set at Fmax 10 N. Sinusoidal loading was carried out at 4 Hz following a modified Locati approach [17,18]. After 50'000 cycles load was increased by 15% and again by 15% after each additional 10'000 cycles (Diagram 1). The advantage of the Locati approach compared to other methods such as Wöhler diagrams or staircase testing is that testing always occurs in the device's ‘critical load range' as all tests lead to fracture. Therefore a lot of information can be gained with relatively few samples and load cycles. While the results are not directly comparable to results obtained with methods such as Wöhler diagrams, the results are valid and generally accepted [17]. When comparing two devices the Locati method is in our view preferable to a Wöhler diagram since more informative value can be obtained with fewer samples. The load ratio, R (Fmin to Fmax), was 0.1. Ending criterion was mechanical failure (plate or screw fracture).
Results
Load and displacement were recorded. Fatigue strength for an individual sample is defined as the load at which failure occurs; the fatigue limit is defined as the number of load cycles when the sample fails. Median and range of fatigue strength (N) and fatigue limit (cycles) are calculated for both plates (Table 2).
![]()
Table 2: Summary of bending tests until plate failure.
View Table 2
The fatigue strength of the six Medartis plates has a median value of 40.5N (range 5.3), and the fatigue limit has a median value of 141'307 cycles (range 5436). For the six DePuySynthes plates the fatigue strength has a median value of 13.2N (range 5.2), and the fatigue limit a median value of 67'287 cycles (range 28'718). Power analysis shows a statistical power of 100% for fatigue strength and fatigue limit with a confidence interval of 95% each. And the Mann-Whitney U test proves significance with a P value of 0.003 (fatigue strength) and 0.004 (fatigue limit) respectively. All plates failed at the level of the screw hole over the fracture site in between the proximal and the distal screw (Figure 3).
Discussion
The lack of bone for fixation in the distal end of the fractured ulna often represents a challenge to hold the reduction in place. Despite the newest findings by Collins et al., which put in question any advantage of locked plating for fractures of the distal ulna [10] in our opinion the head screws in particular offer such an advantage as cannot penetrate the second cortex due to the distal radioulnar joint (DRUJ) to avoid an intra articular position of the screw.
There is no clear evidence that one method of fixation or even operative versus nonoperative treatment is superior in the treatment of distal ulnar shaft and metaphyseal fractures [6]. However previous studies have indicated a risk for nonunion with distal ulnar fractures [4,19]. The surgical approach to the distal ulna places the dorsal sensory branch of the ulnar nerve at risk. This branch emerges from the deep fascia approximately 1 to 4 cm proximal to the ulnar styloid [20]. Neurapraxia of these nerve branches has been reported in up to 40% of patients, although it is often transient and resolves completely [21].
Issues related to hardware prominence of a lateral plate location result in a second surgery for hardware removal in 30-35% [21,22]. Nevertheless several authors report good to excellent results after open reduction and internal plate fixation of unstable distal ulnar fractures with concomitant distal radial fractures [23-25].
In our study we were able to simulate a repetitive radial-ulnar bending force on the plates, similar to in vivo stresses. Given the risk of nonunion in distal ulnar fractures, using plates with a stronger strength profile may be indicated. Considering the repetitive monodirectional load in this experimental set-up and the fact that the wrist in a below elbow splint without any load bearing during the time of recuperation would hardly be exposed to a force of > 10N 1500-3000 times per day both plates would probably not reach mechanical failure during bony consolidation. By using a glass fiber reinforced polyamide 3D Ulna model we were able to simulate an ideal bone quality even in the distal fragment, which provides maximal grip to the ‘monocortical' head-screws. In comminuted or osteoporotic bone the distal part might present the weakest part of the system and it would rather fail by screw loosening than plate breakage.
The limit of this study is that the two plates are similar in term of material (titan) but different in thickness (1.6 mm vs. 1.3 mm) and screw size (2.5 mm vs. 2.0 mm) respectively.
Conclusion
According to results of our testing in the above described near clinical setup, the Distal Ulna Plate 2.5 (Medartis, Basel, Switzerland) showed better mechanical properties compared to the 2.0 mm LCP Distal Ulna Plate (DePuySynthes, West Chester (PA), USA).
Acknowledgement
None.
Declaration of Conflicting Interests
All named authors hereby declare that they have no conflicts of interest to disclose. Implants used for testing were donated by Medartis AG (Basel, Switzerland). The results and interpretation were not influenced by commercial interests of the hosting company.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
References
-
Biyani A, Simison AJ, Klenerman L (1995) Fractures of the distal radius and ulna. J Hand Surg Br 20: 357-364.
-
Garcia-Elias M (1998) Soft-tissue anatomy and relationships about the distal ulna. Hand Clin 14: 165-176.
-
Lindau T (2005) Treatment of injuries to the ulnar side of the wrist occurring with distal radial fractures. Hand Clin 21: 417-425.
-
McKee MD, Waddell JP, Yoo D, Richards RR (1997) Nonunion of distal radial fractures associated with distal ulnar shaft fractures: a report of four cases. J Orthop Trauma 11: 49-53.
-
Anderson LD, Sisk D, Tooms RE, Park WI 3rd (1975) Compression-plate fixation in acute diaphyseal fractures of the radius and ulna. J Bone Joint Surg Am 57: 287-297.
-
Richards TA, Deal DN (2014) Distal ulna fractures. J Hand Surg Am 39: 385-391.
-
Dymond IW (1984) The treatment of isolated fractures of the distal ulna. J Bone Joint Surg Br 66: 408-410.
-
Claes L (2011) Biomechanical principles and mechanobiologic aspects of flexible and locked plating. J Orthop Trauma 25: 4-7.
-
Egol KA, Kubiak E, Fulkerson E, Kummer FJ, Koval KJ (2004) Biomechanics of locked plates and screws. J Orthop Trauma 18: 488-493.
-
Collins M, Hart A, Hines J, Steffen T, Harvey EJ, et al. (2014) Distal ulna fractures: A biomechanical comparison of locking versus nonlocking plating constructs. J Orthop Trauma 8: 470-475.
-
(2012) Medartis Surgical Technique-Step by Step; Distal Radius/Distal Ulna 2.5. Basel, Switzerland: Medartis AG.
-
http://www.synthes.com/MediaBin/International%20DATA/036.000.494.pdf.
-
(2008) American Society for Testing and Materials (ASTM). Standard Specification and Test Method for Metallic Bone Plates. ASTM F 382-399 e1.
-
Marsh JL, Slongo TF, Agel J, Broderick JS, Creevey W, et al. (2007) Fracture and dislocation classification compendium-2007. Orthopaedic Trauma Association classification, database and outcomes committee. J Orthop Trauma 21: 1-133.
-
Mueller ME, Nazarian S, Koch P, Schatzker J (1990) The comprehensive classification of fractures of long bones. Berlin: Springer-Verlag.
-
Rammelt S, Heineck J, Zwipp H (2004) Metatarsalfractures. Injury 35: 77-86.
-
Rotem A (1981) Accelerated fatigue testing method. Int J Fatigue 3: 211-215.
-
Zhang O, Poirier J, Barr J (2003) Modified Locati Method in Fatigue Testing. SAE Technical Paper.
-
Kim JK, Yun YH, Kim DJ, Yun GU (2011) Comparison of united and nonunited fractures of the ulnar styloid following volar-plate fixation of distal radius fractures. Injury 42: 371-375.
-
Handoll HH, Pearce PK (2004) Interventions for isolated diaphyseal fractures of the ulna in adults. Cochrane Database of Systematic Reviews 2.
-
Pomerance J (2005) Plate removal after ulnar-shortening osteotomy. J Hand Surg Am 30: 949-953.
-
Loh YC, Van Den Abbeele K, Stanley JK, Trail IA (1999) The resultsof ulnar shortening for ulnar impaction syndrome.J Hand Surg Br 24: 316-320.
-
Dennison DG (2007) Open reduction and internal locked fixation of unstable distal ulna fractures with concomitant distal radius fracture. J Hand Surg Am 32: 801-805.
-
Lee SK, Kim KJ, Park JS, Choy WS (2012) Distal ulna hook plate fixation for unstable distal ulna fracture associated with distal radius fracture. Orthopedics 35: 1358-1364.
-
Ring D, McCarty LP, Campbell D, Jupiter JB (2004) Condylar blade plate fixation of unstable fractures of the distal ulna associated with fracture of the distal radius. J Hand Surg Am 29: 103-109.