Journal of Musculoskeletal Disorders and Treatment
Diaphyseal Femur Fractures in Children: A Preliminary Study Comparing the use of Elastic Stable Intramedullary Nailing (ESIN) Versus Locking Compression Plates (LCP)
Carlos Acosta Olivo*, J Antonio Ibargüengoytia, Felix Vilchez Cavazos, J Fernando de la Garza Salazar, J Alberto Moreno, Victor Peña Martinez and Eloy Cardenas Estrada
Hospital Universitario Dr. Jose E. Gonzalez, Universidad Autonoma de Nuevo Leon, Mexico
*Corresponding author:
Carlos Acosta Olivo, Ph. D., M.D, Universidad Autonoma de Nuevo Leon,
Hospital Universitario Dr. Jose E. Gonzalez, Ave Madero y Gonzalitos s/n. Mitras Centro CP. 64480, Monterrey, N.L, México, North America, Tel: +52-81-8347-6698, E-mail: dr.carlosacosta@gmail.com
J Musculoskelet Disord Treat, JMDT-3-029, (Volume 3, Issue 1), Research Article
Received: July 10, 2016 | Accepted: January 23, 2017 | Published: January 26, 2017
Citation: Olivo CA, Ibargüengoytia JA, Cavazos FV, Salazar JFG, Moreno JA, et al. (2017) Diaphyseal Femur Fractures in Children: A Preliminary Study Comparing the use of Elastic Stable Intramedullary Nailing (ESIN) Versus Locking Compression Plates (LCP). J Musculoskelet Disord Treat 3:029.
Copyright: © 2017 Olivo CA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective: To compare the functional and radiological results of diaphyseal femur fractures in children between the use of ESIN (Elastic Stable Intramedullary Nail) versus LCP (Locking Compression Plates).
Material and methods: We conducted a prospective, longitudinal, randomized clinical trial on patients aged 5-16 years with diaphyseal femur fractures. All patients weighed more than 30 kg and exhibited no evidence of distal neurovascular compromise or severe polytrauma. We evaluated radiographic consolidation and knee flexion and extension mobility.
Results: A total of 22 patients divided into two groups according to the treatment method were included. Of these, 20 patients completed the study (11 in the ESIN group and 9 in the LCP group). At 3 months, the LCP group exhibited significantly better recovery based on consolidation and knee flexion. The other parameters were not significant.
Conclusions: The group of patients treated with LCP exhibited more rapid consolidation and return to their daily activities. Furthermore, patients treated with LCP suffered fewer complications.
Level of evidence: Therapeutic studies level II prospective comparative study.
Keywords
ESIN, LCP, Pediatric femur, Complex fractures
Introduction
Diaphyseal femur fractures in children account for 1.4-1.7% of all fractures, and 7.6% of those involving the long bones. The ratio of diaphyseal femur fractures between males and females is 2.6:1 [1,2]. Different treatments may be applied based on the patient's age, fracture characteristics, and family social situations, as well as, adverse socioeconomic conditions related to high rates of fractures [1-3]. In children between 6 and 9 years of age, these fractures are often caused by being struck by motor vehicles, and can lead to a complex and unstable fracture [3].
Pediatric femur fractures, represent 9.8% of fractures requiring surgical treatment; up to 76% of femur fractures are diaphyseal, and 62% of these are treated with elastic intramedullary nails, whereas only 10% are treated through open reduction and fixation with plates [4]. Surgical treatment of pediatric femur fractures is indicated in the 6-14 years age group, as the treatment can lead to the rapid mobilization of the patient, shorter hospital stays, and more rapid integration into previous school and daily life activities [5-7].
The use of elastic intramedullary nails is considered a treatment option for patients between 5 and 11 years old [8]. A minimally invasive approach is performed and allows better management of diaphyseal fractures of the middle third. However, this type of treatment does not control the rotation and shortening of the limb [9]. Carey, et al. [10] reviewed 27 femur fractures treated with elastic intramedullary nails and concluded that this treatment is effective and well-tolerated by patients between 6 and 12 years of age. The body weight of the patient is directly related to the postoperative course of treatment with elastic intramedullary nails [11,12]; therefore, patients with a body weight greater than 49 kg (> 108 pounds) and patients older than 10 years are often associated with poor outcomes, as well as features with unstable patterns. Complications such as varus or valgus misalignment may occur in as many as 11% of cases, recurvatum or antecurvatum in up to 8% of cases, rotation in 8%, and discrepancies in length can occur in up to 32% [9,13,14]. A complication rate of up to 49% has been reported; with 40% reporting pain at the site of insertion of the nails in the distal femur [15].
Another treatment option is fixation with plates, which can be achieved through open reduction and plate fixation or indirect reduction and the application of a bridge plate [16,17]. The advent of locking plates, which has led to the concept of "external fixation internally", allows for better stability and can be applied with minimally invasive techniques [18].
The consolidation time for these fractures ranges from 6 weeks in patients treated with elastic intramedullary nails [19] compared with 13.3 weeks in patients treated with plates [20]. However, the complication rate is lower with plates (3-13%) [20,21] relative to the 6-49% of patients managed with elastic intramedullary nails [14,15]. The objective of our study was to compare locking compression plates (LCP) with intramedullary elastic nails (TENs) for the treatment of complex diaphyseal femur fractures in the pediatric population.
Materials and Methods
We conducted a randomized clinical trial approved by the ethics committee of our hospital. Patients were randomized into two groups. Group one corresponded to treatment with LCP, and group two was composed of patients who were treated with elastic stable intramedullary nails (ESIN). The patients were randomly assigned into either group using the Alea-T-7/33 program.
The inclusion criteria were as follows: patients 5-16 years of age with diaphyseal femur fracture, body weight between 30 and 50 kilograms, and informed consent signed by parents or guardians. We excluded patients with polytrauma, cranioencephalic trauma, open fractures, physeal injury, distal neurovascular compromise, pathologic fracture, active infections and non-ambulatory patients. We eliminated patients who did not complete the minimum monitoring proposed. The fractures were classified according to AO/OTA classification as follows [22]: type A (simple, transverse or oblique cut), type B (middle fragment wedge shaped) or type C (complex with multiple fragments).
Upon admission to the emergency department of our hospital, all of the patients were placed in trans-tibial skeletal traction with 10% body weight, until the implant was ready in our hospital, and underwent operations under general anesthesia according to conventional surgical techniques based on the selected implant. Patients in group 1 underwent operation with ESIN (Synthes®, Paoli, Pennsylvania) while placed in the supine decubitus position on a radiolucent table; under fluoroscopic control, 3 cm incisions were made in the medial and lateral thigh 2 centimeters above the distal femoral physis. The diameter of the nails used corresponded to 40% of the diameter of the medullary canal, and using two nails of the same diameter were used [9]. Patients in group 2 were placed in the supine decubitus position on a radiolucent table. An incision of approximately 10 cm was made, taking into account the center of the fracture, a subvastus approach was performed, and straight 3.5 mm LCPs (Synthes®, Paoli, Pennsylvania) were placed. All of the patients were discharged on the second postoperative day, with free knee and hip mobility based upon pain tolerance. The use of crutches and weight bearing was progressive.
After surgery, patients were assessed on an outpatient basis on postoperative day 12 (± 2). The sutures were removed, and isometric exercises of thigh muscles began. The patients were assessed at 3 and 6 weeks and at 3 and 6 months. During follow-up visits, the radiographic extent of the bony callus was assessed via anteroposterior and lateral radiograph of the thigh, according to Stans, et al. [23]: grade 0, no identifiable bony callus; grade 1, primary bony callus formation with little or no new periosteal bone; grade 2, new periosteal bone formation on two sides of the femur; and grade 3, new periosteal bone formation on three or four sides of the femur. The mobility upon flexion and active knee extension was also evaluated.
In addition, we evaluated complications, which were divided into minor and major complications. Minor complications were those that did not exhibit important clinical significance for postoperative outcomes, surgical complications resolved transoperatively, varus/valgus less than 10° in children 6-10 years old and less than 5° in those over 10-years-old, recurvatum-antecurvatum less than 15° in children 6-10 years old and less than 10° in those over 10 years old, shortening < 10 mm, and pain at the surgical scar.
Major complications were those in which an unplanned surgery was required, and those that involved persistent lameness, hip or knee rigidity, malunion, nonunion, deep infection, or persistent nerve damage (excluding asymptomatic implant removal).
Statistical analysis
The Student's t-test was used for parametric distributions, whereas the Mann-Whitney test was used for non-parametric distributions, with a 95% confidence interval. The STATA/IC™ 10 software was used.
Results
A total of 22 patients were included. Two were eliminated due to a lack of minimum follow-up. The study ended with 20 patients: 11 in the LCP group and 9 in the ESIN group; all fractures were closed. No differences in the treatment groups were observed with respect to demographic data. The gender distribution was 13 male and 7 female patients. The average age of all patients was 8.5 years (5-12 years). Demographic data has shown in (Table 1).
![]()
Table 1: Demographic data.
View Table 1
The AO/OTA international classification for the classification of fractures was used. The distribution and treatment has shown in (Table 2 and Table 3).
![]()
Table 2: Distribution of fractures according OTA/AO classification.
View Table 2
![]()
Table 3: Distribution of patients about OTA/AO classification and treatment.
View Table 3
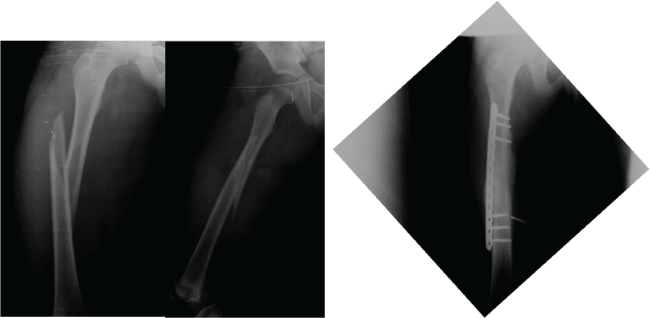
During the first evaluation at 12 days, both groups of patients were evaluated and placed at grade 0. At the three-week evaluation, all patients in the LCP exhibited grade 2 consolidations, whereas all of the patients managed with ESIN were at grade 1. At the sixth week of evaluation, both groups of patients maintained the same consolidation grade as during the previous evaluation. At the 3-month evaluation, all patients with the LCP plate exhibited complete consolidation, placing them in grade 3, whereas all patients using ESIN were at consolidation grade 2. At the end of the six-month evaluation, all patients in both groups were at grade 3 consolidations (Figure 1 and Figure 2).
.
Figure 1: Eleven year old, male patient, treated with LCP at 6th month we observed a complete ossification.
View Figure 1
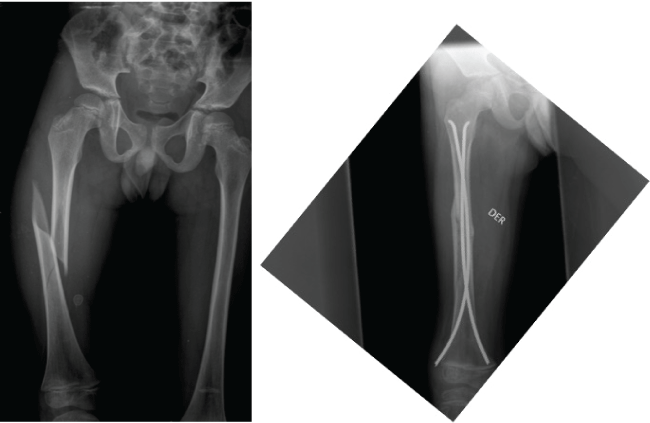
.
Figure 2: Ten year old, male patient, with espiroid fracture. Treatment with ESIN, AP radiograph shown consolidation at sixth month.
View Figure 2
Knee mobility
In all evaluations, better ranges of flexion were observed in patients treated with LCPs, with these results exhibiting statistical significance. When assessing the knee extension of patients, no significant difference between the treatment methods was observed; however, the results were better for the plates. At the end of the evaluation, all patients achieved complete extension (Table 4 and Table 5).
![]()
Table 4: Results of knee flexion. Value of p ≤ 0.05.
View Table 4
![]()
Table 5: Results shown the extension of the knee. The value of 0 is equal to a complete extension.
NS: Non Significance.
View Table 5
Minor complications were noted in all of the patients in the ESIN group (9 patients). In one patient who exhibited a fracture with long spiroid features, external rotation of 10° and antecurvatum of 10° were noted with an overcorrected gait. One patient exhibited a type C3 fracture feature with femoral shortening of 1 cm, asymptomatic. One patient exhibited varus deformity of 8° without symptomatology. In addition, six patients presented with mild pain at the site of nail insertion. This symptom disappeared after removing the implants. In the patients in the LCP group, only one patient suffered a minor complication. A drill bit that broke during the positioning of the plate was found in the posteromedial thigh compartment without associated symptomatology (Table 6).
![]()
Table 6: Complications of procedures.
View Table 6
Two patients in the ESIN group presented major complications. Two patients, one with a B3 type fracture and one with a C3, did not exhibit improvement in mobility of the knee, requiring mobilization under anesthesia. One patient, in LCP group, exhibited a fracture associated with an accident, one year after the initial fracture, and this fracture was managed with an open reduction and osteosynthesis with another plate (Table 6).
Discussion
The treatment of femur fractures in school-aged is preferably surgical, but there is controversy over the ideal treatment. The most frequently used options are LCPs or elastic nails. Elastic nails have an advantage over the placement of plates, as the technique requires minimal invasion of the soft tissues, but the principal disadvantage is a higher percentage of complications relative to LCP.
In an assessment of the use of elastic intramedullary nails in 16 consecutive patients between 5-15 years of age, relative to a similar retrospective group handled with plaster cast immobilization, the elastic intramedullary nails group exhibited a significantly earlier union than the plaster cast group (6 vs. 8 weeks). Furthermore, in the plaster cast group, there were more complications, such as increased angulation in the coronal plane, poor rotational alignment, limb length discrepancy, longer immobilization time, more delay in bearing weight, and increased school absences [19]. A retrospective review was performed on 60 diaphyseal femoral fractures in 58 patients treated with submuscular plates, with an average age of 9 years. Forty of the fractures were classified as unstable (67%). All of the fractures healed, and all patients returned to full activity. Two of the 58 patients (3%) suffered a major complication: an implant failure and a deep infection in an exposed fracture. None of the patients exhibited clinically significant misalignment or limb length discrepancy. All of the patients underwent implant removal without complications [20]. We performed a comparison of treatments in complex femoral fractures in pediatric patients to determine differences in clinical outcomes and improvements between locked compression plates (LCPs) and elastic stable intramedullary nails, assessing radiographic evolution to determine the time of bone consolidation, knee mobility, and complications associated with the use of either method of treatment.
The time of onset of bone consolidation, has been reported to average from 5.4 weeks until observing a bony callus of 3 or 4 cortical layers at 14 weeks with the use of plates; with the use of elastic intramedullary nails, a mean of 7.6 weeks (± 1.5 weeks) for consolidation was observed [17,24-26]. Bony consolidation was significantly correlated with age and the shape of the fracture but not with the level, or mechanism of the fracture [26]. Samora, et al. [27] studied the use of submuscular plates for unstable pediatric diaphyseal fractures, including 32 patients with 33 fractures. The mean time to support weight was 8.1 weeks (3-17.6 weeks). All of the patients in the assessment consolidated at 12 weeks, without transoperative complications. In our results, we noted an onset of fracture consolidation at 3 weeks in the group of plates. At 12 weeks of evolution, consolidation was observed in 3 or 4 cortical layers in all patients treated with LCPs, whereas in the patients treated with ESIN, consolidation was observed beginning at 6 weeks. However, for these patients, consolidation of 3 or 4 cortical layers was not observed until 24 weeks of the study.
Furthermore, in our patients, in the motion of the knee, flexion was significantly greater in patients treated with LCP, whereas extension exhibited no differences between groups in all assessments during the study, and at the end of which all patients showed a full extension.
The complications that were presented during the various treatments for unstable diaphyseal femur fractures in children were divided into minor and major complications, depending on whether a second operation to resolve the complication was required. With respect to minor complications, angular deformities, such as valgus and antecurvatum, superficial wound infection, and transient nerve palsy have been reported in the literature [20]. Additionally, shortening of the limbs has been reported in some series with the use of plates [24]. In our results, we noted minor complications associated with elastic intramedullary nails in all nine patients, pain at the entry site of the nails in 6 patients, and three patients exhibited angular, rotational or limb shortening deformities.
Major and minor complications associated with plate fixation in pediatric diaphyseal femur fractures have been described in up to 13% of cases in skeletally immature patients (6-15 years) with a mean age of 10.2 years. A total of 85 patients were examined (83% male, with a mean age 10.2 years). Complications were observed in 11 patients (13%). Major complications, defined as those resulting in an unplanned surgical procedure (excluding removal of asymptomatic plate implants and/or screws) occurred in 5 patients (6%). Minor complications (those not requiring unplanned surgery) were observed in 6 patients (7%). Rates of 6% for major complications and 7% for minor complications were observed. Most complications occurred after 4 months post-operation, with major complications occurring later [21].
The major complications noted in our study included two patients in the ESIN group exhibiting limitations in knee mobility with disabling pain that had to be managed with mobilization under anesthesia and re-education of gait. A patient in the LCP group exhibited a pathological fracture due to osteoporosis, which was managed with open reduction and plate fixation.
The patients treated with LCP exhibited the best results with respect to consolidation and joint mobility. The results of our study confirm that for the management of diaphyseal femur fractures with complex features in patients between 5 and 11-years-old, one of the best options is the use of locking plates, as it is easier to control rotational and angular deformities and initial shortening of the fracture.
References
-
Sahlin Y (1990) Occurrence of fractures in a defined population. A 1-year study. Injury 21: 158-160.
-
McCartney D, Hinton A, Heinrich SD (1994) Operative stabilization of pediatric femur fractures. Orthop Clin North Am 25: 635-650.
-
Hinton RY, Lincoln A, Crockett MM, Sponseller P, Smith G (1999) Fractures of the femoral shaft in children. Incidence, mechanism, and sociodemographic risk factors. J Bone Joint Surg Am 81: 500-509.
-
Ward WT, Rihn JA (2006) The impact of trauma in an urban pediatric orthopaedic practice. J Bone Joint Surg Am 88: 2759-2764.
-
Karn MA, Ragiel CA (1986) The psychological effects of immobilization in the pediatric orthopaedic patient. Orthop Nurs 5: 12-17.
-
Hughes BF, Sponseller PD, Thompson JD (1995) Pediatric femur fractures: effects of spica cast treatment on family and community. J Pediatr Orthop 15: 457-460.
-
Kirby RM, Winquist RA, Hansen ST (1981) Femoral shaft fractures in adolescents: a comparison between traction plus cast treatment and closed intramedullary nailing. J Pediatr Orthop 1: 193-197.
-
Kocher MS, Sink EL, Blasier RD, Luhmann SJ, Mehlman CT, et al. (2009) Treatment of Pediatric Diaphyseal Femur Fractures. J Am Acad Orthop Surg 17: 718-725.
-
Sink EL, Gralla J, Repine M (2005) Complications of pediatric femur fractures treated with titanium elastic nails: a comparison of fractures types. J Peditar Orthop 25: 577-580.
-
Carey TP, Galpin RD (1996) Flexible intramedullary nail fixation of pediatric femoral fractures. Clin Orthop Relat Res 332: 110-118.
-
Moroz LA, Launay F, Kocher MS, Newton PO, Frick SL, et al. (2006) Titanium elastic nailing of fractures of the femur in children: Predictors of complications and poor outcome. J Bone Joint Surg Br 88: 1361-1366.
-
Leet AI, Pichard CP, Ain MC (2005) Surgical treatment of femoral fractures in obese children: does excessive body weight increase the rate of complications? J Bone Joint Surg Am 87: 2609-2613.
-
Heinrich SD, Drvaric DM, Darr K, MacEwen GD (1994) The operative stabilization of pediatric diaphyseal femur fractures with flexible intramedullary nails: a prospective analysis. J Pediatr Orthop 14: 501-507.
-
Wall EJ, Jain V, Vora V, Mehlman CT, Crawford AH (2008) Complications of titanium and stainless Steel elastic nail fixation of pediatric femoral fractures. J Bone Joint Surg Am 90: 1305-1313.
-
Luhmann SJ, Schootman M, Schoenecker PL, Dobbs MB, Gordon JE (2003) Complications of titanium elastic nails for pediatric femoral shaft fractures. J Pediatr Orthop 23: 443-447.
-
Hedequist DJ, Sink E (2005) Technical aspects of bridge plating for pediatric femur fractures. J Orthop Trauma 19: 276-279.
-
Sink EL, Hedequist D, Morgan SJ, Hresko T (2006) Results and technique of unstable pediatric femoral fractures treated with submuscular bridge plating. J Pediatr Orthop 26: 177-181.
-
Wagner M (2003) General principles for the clinical use of the LCP. Injury 34: 31-42.
-
Saseendar S, Menon J, Patro DK (2010) Treatment of femoral fractures in children: is titanium elastic nailing an improvement over hip spica casting? J Child Orthop 4: 245-251.
-
Abdelgawad AA, Sieg RN, Laughlin MD, Shunia J, Kanlic EM (2013) Submuscular bridge plating for complex pediatric femur fracture is reliable. Clin Orthop Relat Res 471: 2797-2807.
-
May C, Yen YM, Nasreddine AY, Hedequist D, Hresko MT, et al. (2013) Complications of plate fixation of femoral shaft fractures in children and adolescents. J Child Orthop 7: 235-243.
-
Marsh JL, Slongo TF, Agel J, Broderick JS, Creevey W, et al. (2007) Fracture and dislocation classification compendium-2007: Orthopaedic Trauma Association classification, database and outcomes committee. J Orthop Trauma 21: S1-133.
-
Stans AA, Morrissy RT, Renwick SE (1999) Femoral shaft fracture treatment in patients age 6 to 16 years. J Pediatr Orthop 19: 222-228.
-
Kanlic EM, Anglen JO, Smith DG, Morgan SJ, Pesantez RF (2004) Advantages of submuscular bridge plating for complex pediatric femur fractures. Clin Orthop Relat Res 426: 244-251.
-
Oh CW, Song HR, Jeon IH, Min WK, Park BC (2007) Nail-assisted percutaneous plating of pediatric femoral fractures. Clin Orthop Relat Res 456: 176-181.
-
Assaghir YM (2012) Titanium elastic nail in femur fractures as an alternative to spica cast in preschoolers. J Child Orthop 6: 505-511.
-
Samora WP, Guerriero M, Willis L, Klingele KE (2013) Submuscular bridge plating for length-unstable, pediatric femur fractures. J Pediatr Orthop 33: 797-802.