Journal of Rheumatic Diseases and Treatment
Massive Serositis as the Initial Presentation of Systemic Lupus Erythe-matosus: A Report of Two Cases and Review of the Literature
Laura Geraldino-Pardilla1 Yevgeniya Gartshteyn1* and Fabian Mendoza2
1Department of Medicine, Columbia University, College of Physicians & Surgeons, USA
2Department of Medicine, Thomas Jefferson University, USA
*Corresponding author: Yevgeniya Gartshteyn, MD, Department of Medicine, Columbia University, College of Physicians & Surgeons, 177 Fort Washington Ave 8SK 8-004 New York, NY 10032, USA, E-mail: yg2372@cumc.columbia.edu
J Rheum Dis Treat, JRDT-1-028, (Volume 1, Issue 4), Case Series; ISSN: 2469-5726
Received: November 26, 2015 | Accepted: December 29, 2015 | Published: December 31, 2015
Citation: Geraldino-Pardilla L, Gartshteyn Y, Mendoza F (2015) Massive Serositis as the Initial Presentation of Systemic Lupus Erythe-matosus: A Report of Two Cases and Review of the Literature. J Rheum Dis Treat 1:028. 10.23937/2469-5726/1510028
Copyright: © 2015 Geraldino-Pardilla L, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Large volume effusions as a manifestation of active systemic lupus erythematous (SLE) is rare, and when it does occur, it is usually associated with complications of chronic lupus disease, such as nephrotic syndrome, constrictive pericarditis, heart failure or Budd-Chiari syndrome. Massive serositis as a presenting feature of SLE is rare. We de-scribe two adult cases of new onset SLE presenting with massive ascites in the first case, and large bilateral pleural effusions in the second case. The serositis in both patients responded well to high dose steroid therapy with signifi-cant improvement in symptoms. Only a small number of case reports describing massive ascites or large pleural effusions as initial manifestations of new onset SLE have been published. A literature review of these case reports and their treatment outcomes is described.
Keywords
Systemic lupus erythematosus, Lupus pleuritis, Lupus peritonitis, Lupus ascites, Pleural effusion
Introduction
Systemic lupus erythematosus (SLE) is an autoimmune disease with heterogeneous phenotypes. Although serosal inflammation is common in SLE, massive pleural ascites and large volume pleural effusions as presenting features are unusual. Unlike most cases of lupus serositis, patients with these large effusions tend to require aggressive man-agement with high dose steroids and steroid-sparing agents [1].
Methods
Two case reports of SLE presenting as serositis with large volume effusions are described.
A literature review was performed using a Pubmed search (1964-2015) for all reported cases of large volume ascites or pleural effusions as the presenting features of new onset SLE. The following search terms were used: SLE/Lupus serositis, ascites, pleuritis, peritonitis, pleural effusion, peritoneal effusion. Only adult cases in the English language were reviewed.
Case Reports
Case 1
A 50-year-old immigrant from Central America, was admitted with rapidly increasing ascites. Medical problems included hypertension, chronic hepatitis C with cirrhosis and portal hypertension (treated with an 8 month course of PEG-IFN one year prior to admission), and end-stage renal disease (ESRD) status post cadaveric renal transplant 10 years prior but complicated by transplant rejection and new hemodialysis requirement over the last two years.
On presentation, the patient was febrile with cervical lymphadenopathy, accompanied by massive non-tender asci-tes with hemodynamic compromise requiring serial large-volume paracentesis (Figure 1). The serum-ascites albumin gradient (SAAG) was < 1.1, which was inconsistent with portal hypertension ascites or possible nephrotic syndrome given the end stage renal disease. Ascitic fluid WBC counts ranged from 77-675/mm3 with a lymphocytic predomi-nance. Peritoneal fluid bacterial, fungal, and AFB cultures were negative and there were no malignant cells. Serum HIV, rheumatoid factor and cryoglobulins were negative. Tuberculin purified protein derivative (PPD) testing was negative as well. Hepatic or portal vascular thrombosis was ruled out with patent vessels seen on Doppler, and an echocardiogram noted preserved ventricular function. Serum ANA and anti-dsDNA antibodies were 1:2560 and 12,751 IU/mL, respectively (normal dsDNA is < 25 IU/ml). The patient was also leukopenic (WBC-2.7/mm3) and had severe hypocomplementemia (C3 = 12 mg/dL, C4 = 4 mg/dL).
.
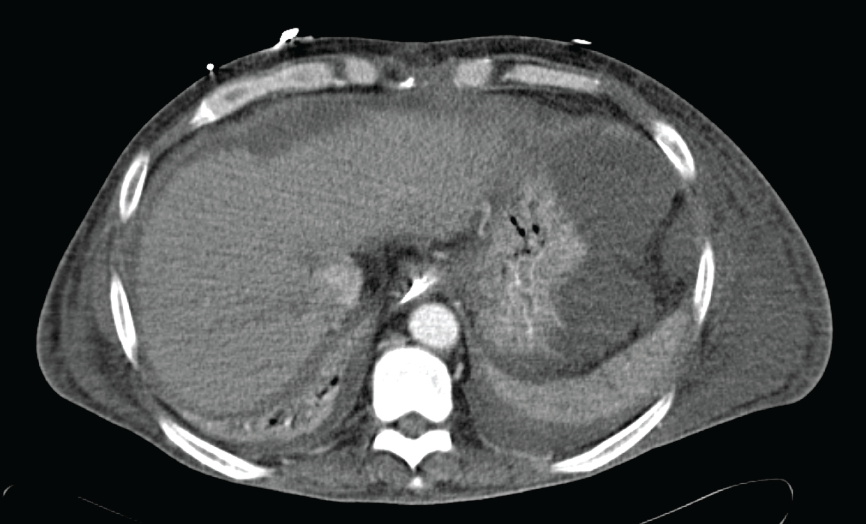
Figure 1: Axial, contrast enhanced computed tomography (CT) image of the abdomen showing ascites.
View Figure 1
A diagnosis of SLE with lupus peritonitis was made and treatment initiated with intravenous methylprednisolone 500 mg/day for a week followed by prednisone 1 mg/Kg/day and hydroxychloroquine 400 mg daily. This resulted in hemodynamic stability, significant improvement of the ascites, rise in complement levels and lowering anti-DNA titers. The small volume ascites that remained revealed a SAAG >1.1 which was then attributed to the known portal hypertension.
Case 2
An 80-year-old patient with history of congestive heart failure (CHF) and breast cancer in remission after a left rad-ical mastectomy, radiation and chemotherapy presented with dyspnea. On arrival the patient required emergent mechanical ventilation for respiratory failure due to massive bilateral pleural effusions and ascites. Pleural fluid analysis was exudative with negative cultures and cytology negative for malignant cells. An echocardiogram showed preserved ventricular function and a small pericardial effusion. A CT scan of the chest confirmed large bi-lateral pleural effusions. V/Q scan was low probability for pulmonary embolism. Bronchoscopic lavage had no growth from cultures and was negative for malignant cells. A right-sided heart catheterization was normal. After diuresis, the patient was extubated but required emergent chest tube placement for pleural fluid drainage.
Serologies revealed a positive serum ANA (1:320), anti-ds-DNA (119), and borderline complement levels (C3 = 89, C4 = 14). Acute renal failure subsequently developed and a renal biopsy revealed Class IV/V lupus nephritis (LN). After no response to prednisone 60 mg/day, methylprednisolone 500 mg/day for 3 days was started followed by a steroid taper, hydroxychloroquine 400 mg daily and mycophenolate mofetil titrated to 2 g/day. The renal function improved over the subsequent days and the pleural and peritoneal effusions resolved.
Discussion
Although serositis is found in 63% of SLE patients on autopsy, [2] massive ascites and large pleural effusions are uncommon in the lifetime of lupus disease, and are even more rare as the initial manifestation [2-4]. Pleural effu-sions occur in up to 50% of patients with SLE, but it is the presenting feature in only 1-5% of patients, with effu-sions usually small to moderate in size [5]. Unlike pleural involvement, the true prevalence of lupus peritonitis is unknown but presumably low, although probably overlooked despite several cases being published since Metzger's initial case report in 1974 [6].
Large effusions are usually attributed to a complication from CHF, constrictive pericarditis, nephrotic syndrome, portal hypertension, Budd-Chiari, peritoneal carcinomatosis, infectious peritonitis or pneumonia. One of these etiol-ogies is usually cited as the cause for the 8-11% of SLE patients that develop ascites during the lifetime of their dis-ease [7,8]. It is nonetheless important to consider active SLE in the differential, as was the situation in the two cases described that had SLE-related massive ascites and/or large pleural effusions as the initial presentation of SLE. Our patients met the 1997 American College of Rheumatology classification criteria for SLE [9], given positive anti-ANA and anti-ds-DNA antibodies, serositis, as well as leukopenia in case No.1, and lupus nephritis in case No.2. For case No.1, although portal hypertension was present, the low SAAG in the absence of infection, malignancy, or acute portal thrombosis was inconsistent with portal hypertension ascites and suggested peritonitis of unknown eti-ology. Given the positive serum ANA and ds-DNA antibodies, low complement levels, and a significant clinical re-sponse to steroids, SLE remains the most likely diagnosis. Unfortunately, the etiology of the ESRD in this patient could not be determined since the renal biopsy had been performed many years prior in Central America. It is also debatable whether the discontinuation of the immunosuppressants, which the patient had in the past taken follow-ing the renal transplant, now unmasked the SLE, or whether the treatment with PEG-IFN, on the other hand, result-ed in a drug-induced lupus-like illness. In the second case, although the patient had a history of a prior CHF episode, the echocardiogram and right heart catheterization were normal, arguing against CHF as the cause for the large effusions.
Serositis results from fluid and protein leak due to increased permeability of the microvascular circulation that oc-curs with inflammation of the pleural and peritoneal microvessels. The presumed vasculitis is caused by immune-complex deposition and complement activation, described since the 1970s and noted in biopsies of the pleural and peritoneal vessels [2,10-12]. Bitran et al. revealed granular depositions of IgG and complement along the mesothe-lial layer and blood vessels in SLE patients with serositis [13]. In massive ascites, marked serosal exudate in con-junction with a reduced peritoneal absorptive capacity facilitate rapid fluid accumulation.
A review of similar adult cases of massive ascites and severe pleuritis as the presenting features of SLE is summa-rized in table 1 and table 2, respectively [1-5,7,8,10-12,14-18]. Ascites fluid characteristics include a WBC range from 10-1630/mm3 with lymphocytic predominance, [2,7] a SAAG < 1.1, and occasionally positive ANA, anti-dsDNA antibodies, and lupus erythematosus (LE) cells. Pleural fluid characteristics include a WBC 200-3000/mm3 with either a neutrophilic or lymphocytic predominance, high protein and LDH counts, positive ANA, elevated anti-dsDNA titers and presence of LE cells [5,17]. For treatment, most patients required high dose steroids followed by a taper, with complete resolution of serositis noted in some and moderate reduction in others. Additional immuno-suppression was administered in 4 of the 15 reported patients [2,3,5,15]. Chest tube drainage or pleurodesis were rarely required [5].
![]()
Table 1: Case reports of ascites as the presenting feature of SLE.
View Table 1
![]()
Table 2: Case reports ofmassive pleural effusions as the presenting feature of SLE.
View Table 2
Conclusion
Since Dubois stated in 1964 that lupus serositis does not cause significant effusions [19], case reports have been published suggesting that massive lupus serositis does occur and can be the main initial manifestation of the dis-ease. Our case reports and review of the literature emphasize how appropriate evaluation and aggressive immuno-suppressive therapy is often required to assure a positive outcome in these cases.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not- for-profit sec-tors.
References
-
Zhou L, Ming Sun C, Li Chen W, Zhang H, Wang P, et al. (2014) Massive and painful ascites as a presenting manifestation of systemic lupus erythematosus flare: a case report and literature review. Rev Med Chil 142: 255-260.
-
Weinstein PJ, Noyer CM (2000) Rapid onset of massive ascites as the initial presentation of systemic lupus erythematosus. Am J Gastroenterol 95: 302-303.
-
Bouros D, Panagou P, Papandreou L, Kottakis I, Tegos C (1992) Massive bilateral pleural effusion as the only first presentation of systemic lupus erythematosus. Respiration 59: 173-175.
-
Hammoudeh M, Siam AR (1995) Recurrent peritonitis with ascites as the predominant manifestation of systemic lupus erythematosus. Clin Rheumatol 14: 352-354.
-
Wan KS (2008) Pleuritis and pleural effusion as the initial presentation of systemic lupus erythematous in a 23-year-old woman. Rheumatol Int 28: 1257-1260.
-
Metzger AL, Coyne M, Lee S, Kramer LS (1974) In vivo LE cell formation in peritonitis due to systemic lupus erythematosus. J Rheumatol 1: 130-133.
-
Forouhar-Graff H, Dennis-Yawingu K, Parke A (2011) Insidious onset of massive painless ascites as initial manifestation of systemic lupus erythematosus. Lupus 20: 754-757.
-
Prasad S, Abujam B, Lawrence A, Aggarwal A (2012) Massive ascites as a presenting feature of lupus. Int J Rheum Dis 15: e15-16.
-
Hochberg MC (1997) Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum 40: 1725.
-
Ishiguro N, Tomino Y, Fujito K, Nakayama S, Koide H (1989) A case of massive ascites due to lupus peritonitis with a dramatic response to steroid pulse therapy. Jpn J Med 28: 608-611.
-
Ito H, Nanamiya W, Kuroda N, Inoue M, Sasaoka A, et al. (2002) Chronic lupus peritonitis with massive ascites at elderly onset: case report and review of the literature. Intern Med 41: 1056-1061.
-
Mitra B, Sengupta P, Saha K, Sarkar N, Pal J (2005) Systemic lupus erythematosus presenting with recurrent pleural effusion without any systemic manifestation. J Assoc Physicians India 53: 1073-1106.
-
Bitran J, McShane D, Ellman MH (1976) Arthritis Rounds: Ascites as the major manifestation of systemic lupus erythematosus. Arthritis Rheum 19: 782-785.
-
Mier A, Weir W (1985) Ascites in systemic lupus erythematosus. Ann Rheum Dis 44: 778-779.
-
Trock D, Voinea A, Wolk J, Majoros S (2005) New-onset lupus presenting as serositis in an 80-year-old woman: does a high-titer ANA in pleural, pericardial, or peritoneal fluid help confirm the diagnosis? J Clin Rheumatol 11: 292-293.
-
Pott Junior H, Amate Neto A, Teixeira MA, Provenza JR (2012) Ascites due to lupus peritonitis: a rare form of onset of systemic lupus erythematosus. Rev Bras Reumatol 52: 116-119.
-
Chang WT, Hsieh TH, Liu MF. Systemic lupus erythematosus with initial presentation of empyematous pleural effusion in an elderly male patient: a diagnostic challenge. J Microbiol Immunol Infect 46: 139-142.
-
Liu R, Zhang L, Gao S, Chen L, Wang L, et al. (2014) Gastrointestinal symptom due to lupus peritonitis: a rare form of onset of SLE. Int J Clin Exp Med 7: 5917-5920.
-
Dubois EL, Tuffanelli DL (1964) Clinical Manifestations of Systemic Lupus Erythematosus. Computer Analysis of 520 Cases. JAMA 190: 104-111.





