Journal of Rheumatic Diseases and Treatment
Biomechanical Stimulation Therapy - An Efficacious Method for Facial Scleroderma with Reduced Oral Aperture
Walter Berg1, Ingo H Tarner2, Gabriela Riemekasten3, Ulf Müller-Ladner2 and Uwe Lange2*
1Rehabilitative Medicine and Psychosomatic Treatment Center, AHG Hospital, Waren, Germany
2Department of Internal Medicine and Rheumatology, Justus-Liebig-University Giessen, Department of Rheumatology, Clinical Immunology, Osteology and Physical Medicine, Kerckhoff-Klinik, Bad Nauheim, Germany
3Department of Rheumatology and Clinical Immunology, University Hospital, Lübeck, Germany
*Corresponding author: Dr. Uwe Lange, MD, Professorship of Rheumatology, Osteology and Physical Medicine, Department of Internal Medicine and Rheumatology, Justus-Liebig-University Giessen, Department of Rheumatology, Clinical Immunology, Osteology and Physical Medicine, Kerckhoff-Klinik, Benekestrasse 2-8, D-61231 Bad Nauheim, Germany, Tel: +49-6032-996-2100, Fax: +49-6032-996-2104, E-mail:
u.lange@kerckhoff-klinik.de
J Rheum Dis Treat, JRDT-2-030, (Volume 2, Issue 1), Research Article; ISSN: 2469-5726
Received: December 21, 2015 | Accepted: January 23, 2016 | Published: January 26, 2016
Citation: Berg W, Tarner IH, Riemekasten G, Müller-Ladner U, Lange U (2016) Biomechanical Stimulation Therapy - An Efficacious Method for Facial Scleroderma with Reduced Oral Aperture. J Rheum Dis Treat 2:030. 10.23937/2469-5726/1510030
Copyright: © 2016 Berg W, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: To reduce edema and tension of the skin, various physical therapies can be used in patients with systemic sclerosis (SSc). As biomechanical stimulation (BMS) therapy has been identified as an effective physiotherapy method to improve the mobility of joints, legs and the trunk in SSc, the aim of this study was to evaluate the effect of BMS in SSc patients with reduced oral aperture due to facial scleroderma.
Methods: Two patient groups were treated for 3 weeks using different BMS schemes: 16 patients were treated for 20 minutes three times a week (regular BMS), and 12 patients for 30 minutes five times a week (intensive BMS).
Results: Both groups showed a significant increase of their oral aperture as determined by the interlabial distance. Furthermore, comparison between both treatment groups showed a significant superiority of intensive BMS, with a clear dose-effect correlation. No adverse effects were observed.
Discussion: Impaired oral aperture and thus quality of life due to facial scleroderma are improved substantially by BMS, which should therefore be applied to affected SSc patients on a regular basis.
Keywords
Systemic sclerosis, Physical therapy, Biomechanical stimulation
Introduction
Systemic sclerosis (SSc) is a chronic, severe connective tissue disorder characterized by a microangiopathy and excess deposition of connective tissue matrix in the skin and internal organs [1-3]. Skin involvement is the most conspicuous manifestation of SSc, and based on its extent two distinct disease subsets are recognized, diffuse cutaneous (dcSSc) and limited cutaneous systemic sclerosis (lcSSc), with lcSSc affecting only the distal extremities and the face and dcSSc also affecting the proximal extremities and the trunk [1,4,5].
When the face is affected, the cutaneous changes severely impair facial mimicry and oral aperture. A reduced oral aperture due to the tightness of the perioral skin can impair patients’ health and quality of life because eating becomes increasingly difficult and oral access for the purpose of personal dental hygiene and professional dental interventions becomes severely limited. Unfortunately, until today no antifibrotic or immunosuppressive agents have been shown to be of sustained benefit in counteracting the skin changes of SSc.
Physical therapy plays a central role in the therapeutic armamentarium for the treatment of rheumatic diseases including SSc. In addition to manual lymph drainage, biomechanical stimulation (BMS) therapy has been described as a novel physiotherapy method for patients with SSc [6]. BMS applies mechanical vibrations of defined amplitude and frequency to the skin, connective tissue and muscles. Since an improvement of skin score and joint mobility has been achieved by BMS in SSc patients [6] we decided to investigate BMS in SSc patients with facial scleroderma and reduced oral aperture.
Patients and Methods
A total of 28 SSc patients (25 female; mean age 52, age range 38 - 68 years) with reduced oral aperture were enrolled. The study was conducted according to the Declaration of Helsinki and International Committee on Harmonisation good clinical practices. The protocol was reviewed and approved by the institutional review board. All patients provided written informed consent und fully completed the study. The patients were randomised (computer generated random numbers) into two groups: 16 patients underwent BMS applications for 20 minutes three times a week (regular BMS), and 12 patients were treated for 30 minutes five times a week (intensive BMS). BMS was performed by a trained physiotherapist who was notified of the randomization. The entire treatment period for both groups was three weeks. To prevent communication between the two treatment groups, patients receiving regular BMS were treated on Tuesdays and Thursdays whereas the others were treated on Mondays, Wednesdays and Fridays.
The hand-held BMS unit, which has a fixed amplitude of 4 mm, was set to a vibrating frequency ranging between 23 and 28 Hz as described by Klyscz et al. [6] and was applied to the perioral, sternocleidomastoid muscle and maxillary regions using a dynamic technique of circular movements (Figure 1). By choosing different frequencies, it is possible to obtain different therapeutic effects. The lower frequency range of ≥ 23 Hz improves muscular perfusion and has a pronounced anti-lymphedematous effect [6]. Frequencies of around 28 Hz mediate an analgesic effect [7,8]. During the course of BMS therapy no other treatment was applied.
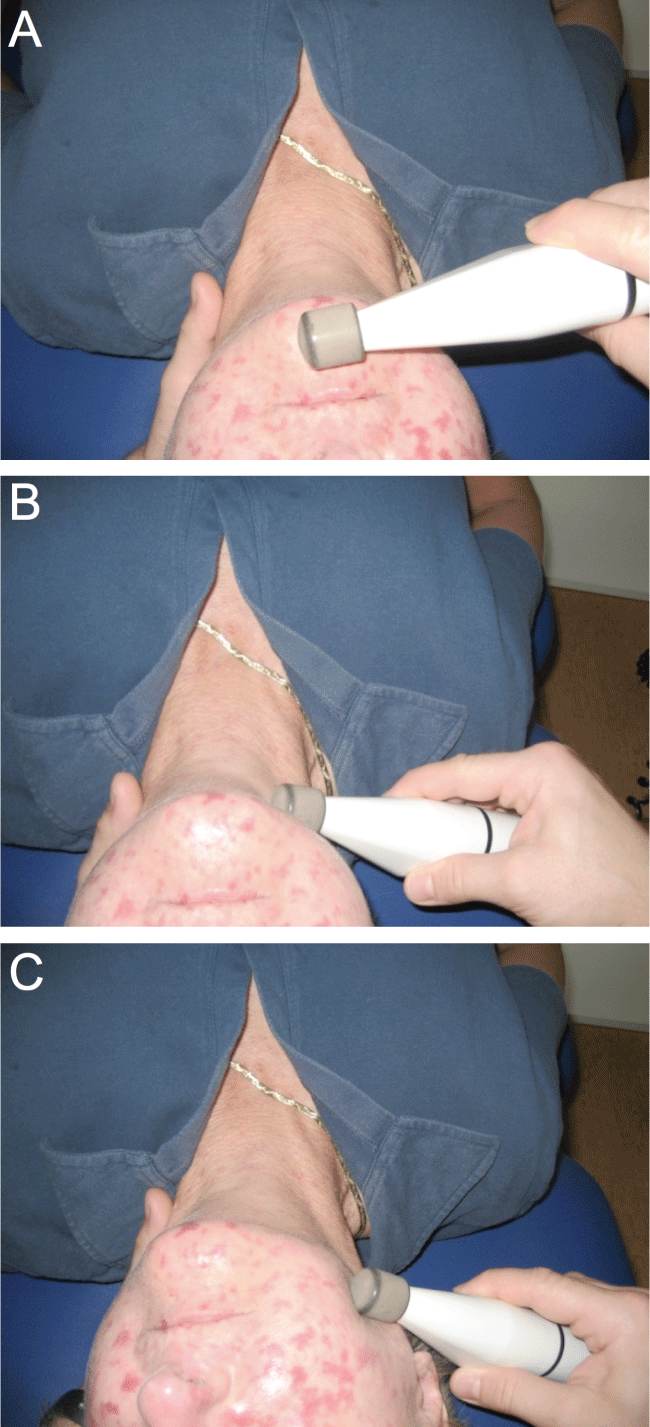
.
Figure 1: Dynamic BMS application technique. The hand-held device is applied to the lower face and the neck in gentle, rotating movements starting in the perioral area underneath the lower lip (A) and continuing from there to the right sternocleidomastoid muscle area (B), the right mandibular area (C), and onward to the perioral area above the upper lip, the left mandibular area, the left sternocleidomastoid muscle area and back to the perioral area underneath the lower lip. This large circle was repeated several times during each treatment session.
View Figure 1
All patients were examined prior to BMS treatment and after completion of the treatment period by a study physician who was blinded to the treatment group. Oral aperture was measured as mean interlabial distance (in millimetres) based on three measurements per patient using a micro-caliper. Between each measurement, the patients were asked to close their mouth and re-open as wide as possible. As a control-group, the interlabial distance was measured in 20 healthy, age-matched individuals. In addition, patients were asked at the end of the 3-week treatment period about subjective changes of their facial skin according to the corresponding item (delta-skin) of the European Scleroderma Study Group activity score [9].
Data were tested for normal distribution using normal Q-Q plots and the Shapiro-Wilk test. Due to a lack of normal distribution, statistical analysis included the Wilcoxon test for evaluation of the changes of oral aperture before and after therapy in either group and the Mann-Whitney U test for analysis of the differences between the two treatment groups. A p-value < 0.01 was considered as statistically significant. The study’s alpha-level was 0.05. All analyses were done using R for Windows 2.14.
Results
All patients reported that their facial skin felt softer and less tense after completion of BMS therapy, without any adverse effects or increased pain during the treatment. Ten patients (35.7%) reported that during BMS there was an extremely pleasant, soothing sensation of warmth in the treated facial skin areas.
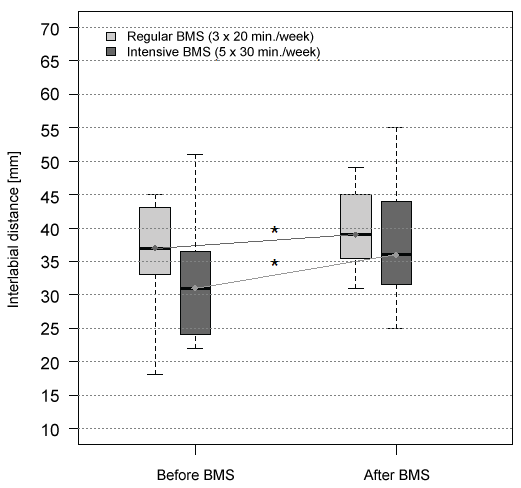
The mean interlabial distance ± standard deviation (SD) at baseline was 54 ± 3 mm in the 20 healthy controls, 36.6 ± 7.2 mm (95% confidence interval [CI] 32.75 ; 40.37) in the regular BMS group and 32.4 ± 9.3 mm (95% CI 26.52 ; 38.31) in the intensive BMS group (Figure 2). The difference between the two BMS groups was not statistically significant (p = 0.137). Both BMS treatment regimens resulted in a significant increase of oral aperture. While the mean ± SD interlabial distance increased by 2.1 ± 1.3 mm (95% CI 1.45; 2.8; p < 0.02) to 38.7 ± 7 mm (95% CI 34.94; 42.43) in the regular BMS group, an even higher increase of 5.7 ± 2.8 mm (95% CI 3.88; 7.45; p < 0.001) yielding 38.1 ± 9.1 mm (95% CI 32.31; 43.86) was achieved in the intensive BMS group (Figure 2). Comparison between the two BMS treatment regimens showed a significant superiority of intensive BMS (p < 0.001).
.
Figure 2: Effects of different BMS application regimens on oral aperture measured as interlabial distance in mm. Significant improvement (*) was achieved by both regular BMS with 3 applications per week for 20 minutes each (light grey boxes; p < 0.02) and intensive BMS with 5 applications per week for 30 minutes each (dark grey boxes; p < 0.001). The rate of improvement of oral aperture was significantly greater in the intensive BMS group (p < 0.001) as depicted by the slope of the light grey lines.
View Figure 2
Discussion
Efficacy of physical therapy in SSc has been suggested by clinical studies [10,11] and positive effects in daily practice. Established physical therapy methods are manual lymphatic drainage, connective tissue massage, carbon dioxide baths, mobilization treatment, and proprioceptive neuromuscular facilitation (PNF) therapy.
In the spectrum of physical therapy, biomechanical stimulation therapy (BMS) is a novel physiotherapy method for SSc [6]. Application of BMS causes tissue structures to vibrate visibly along the longitudinal axis at frequencies between 23-28 Hz. Thus far, the exact mechanisms of the biologic effects of BMS are not completely understood. BMS has been shown to improve joint mobility in healthy subjects and SSc patients and to reduce muscular tone and tissue edema [6,12] without any signs of adverse effects. Furthermore, pain was ameliorated noticeably about 10-15 seconds after initiation of treatment and resulted in a pleasant sensation of warmth in study groups exposed to similar vibration therapies [7,8,13]. A possible explanation for this vibration-induced improvement in flexibility and mobility in terms of a neurophysiological phenomenon could be that the tissue vibration results in a stimulation of the Golgi tendon organs leading to an inhibition of muscle contractions followed by muscle relaxation [14].
The present study shows that regular BMS application for three weeks results in a significant improvement of oral aperture in facial scleroderma without causing any adverse effects. Furthermore, comparison between two treatment regimens with different intensities of BMS application reveals a significant superiority of intensive BMS with 30 minutes of treatment applied five times per week. The achieved increase in oral aperture of 5.6 mm can be of critical importance for allowing oral access with a spoon when eating, a tooth brush for oral hygiene or a dental instrument. In addition, 36% of patients experienced the treatment to be very pleasing and soothing and all patients felt an amelioration of skin tension, the importance of which cannot be overestimated, particularly regarding facial skin. Thus, taken all benefits together, BMS therapy substantially improves the patients’ quality of life. Of note, application of this treatment method can be learned by patients relatively easily after detailed instruction by an experienced physiotherapist. Thus, BMS is suitable for convenient, daily self-application by SSc patients. We conclude that BMS is an effective, easy-to-use and safe technique which should be used as part of a multimodal therapy in SSc patients on a regular basis. Our pilot study provides the basis for further studies which should compare BMS to other physical therapy modalities such as active exercise, connective tissue massage and ultrasound in order to further confirm its efficacy and to develop optimal combination strategies.
Key messages
• Facial scleroderma and reduced oral aperture represent significant impairment in the quality of life in patients with SSc.
• Thus far, there is no effective, evidence-based treatment option for impaired oral aperture.
• Biomechanical stimulation therapy is a highly effective, safe, easy-to-use and low-cost treatment option that provides significant improvement of oral aperture and relief of facial skin tension in patients with SSc.
References
-
LeRoy EC, Black C, Fleischmajer R, Jablonska S, Krieg T, et al. (1988) Scleroderma (systemic sclerosis): classification, subsets and pathogenesis. J Rheumatol 15: 202-205.
-
Walker UA, Tyndall A, Czirják L, Denton C, Farge-Bancel D, et al. (2007) Clinical risk assessment of organ manifestations in systemic sclerosis: a report from the EULAR Scleroderma Trials And Research group database. Ann Rheum Dis 66: 754-763.
-
Hunzelmann N, Genth E, Krieg T, Lehmacher W, Melchers I, et al. (2008) The registry of the German Network for Systemic Scleroderma: frequency of disease subsets and patterns of organ involvement. Rheumatology (Oxford) 47: 1185-1192.
-
Krieg T, Takehara K (2009) Skin disease: a cardinal feature of systemic sclerosis. Rheumatology (Oxford) 48 Suppl 3: iii14-18.
-
Czirják L, Foeldvari I, Müller-Ladner U (2008) Skin involvement in systemic sclerosis. Rheumatology (Oxford) 47 Suppl 5: v44-45.
-
Klyscz T, Rassner G, Guckenberger G, Jünger M (1999) Biomechanical stimulation therapy. A novel physiotherapy method for systemic sclerosis. Adv Exp Med Biol 455: 309-316.
-
Klyscz T, Ritter-Schempp C, Jünger M, Rassner G (1997) [Biomechanical stimulation therapy as physical treatment of arthrogenic venous insufficiency]. Hautarzt 48: 318-322.
-
Lundeberg T, Nordemar R, Ottoson D (1984) Pain alleviation by vibratory stimulation. Pain 20: 25-44.
-
Valentini G, Della Rossa A, Bombardieri S, Bencivelli W, Silman AJ, et al. (2001) European multicentre study to define disease activity criteria for systemic sclerosis. II. Identification of disease activity variables and development of preliminary activity indexes. Ann Rheum Dis 60: 592-598.
-
Berg W (2008) Sklerodermie. In: Lange U, (ed) Physikalische Medizin in der Rheumatologie unter Berücksichtigung evidenzbasierter Daten. Stuttgart: Ligatur, 99-106.
-
Müller-Eschner M, Albrecht K, Saar P, Müller-Ladner U, Strunk J, et al. (2008) Therapieeffekt von Bastian (CO2)-Handbädern auf die akrale Durchblutung bei Patienten mit systemischer Sklerose. In: Lange U, ed. Physikalische Medizin in der Rheumatologie unter Berücksichtigung evidenzbasierter Daten. Stuttgart: Ligatur, 151-154.
-
Nazarov V, Spivak G (1987) Development of athlete`s strength abilities by means of biomechanical stimulation method. Theory and Practice of Physical Culture (Moscow) 12: 37-39.
-
Atha J, Wheatley DW (1976) Joint mobility changes due to low frequency vibration and stretching exercise. Br J Sports Med 10: 26-34.
-
Issurin VB, Liebermann DG, Tenenbaum G (1994) Effect of vibratory stimulation training on maximal force and flexibility. J Sports Sci 12: 561-566.





