Journal of Rheumatic Diseases and Treatment
Relapsing Polychondritis with Central Nervous System Involvement Presented as Encephalitis: 7 Cases and Literature Review
Anna Zhou, Xindi Li, Lin Zhao, Yonghong Liu and Xinghu Zhang*
Department of Neurology, Beijing Tiantan Hospital, Capital Medical University, China
*Corresponding author: Xinghu Zhang, Department of Neurology, Beijing Tiantan Hospital, Capital Medical University, No.6 Tiantanxili, Dongcheng District, Beijing, 100050, China, Tel: +86-13911-296676, E-mail: xhzhtiantan@hotmail.com
J Rheum Dis Treat, JRDT-3-045, (Volume 3, Issue 1), Research Article; ISSN: 2469-5726
Received: October 03, 2016 | Accepted: February 10, 2017 | Published: February 13, 2017
Citation: Zhou A, Li X, Zhao L, Liu Y, Zhang X (2017) Relapsing Polychondritis with Central Nervous System Involvement Presented as Encephalitis: 7 Cases and Literature Review. J Rheum Dis Treat 3:045. 10.23937/2469-5726/1510045
Copyright: © 2017 Zhou A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objectives: This study aims to describe the clinical manifests, CSF features and brain MRI characters of patients with relapsing polychondritis (RP) and central nervous system (CNS) involvement presented as encephalitis.
Methods: Seven cases with RP and CNS involvement were enrolled from 2011 to 2015. RP was diagnosed upon the modified McAdam criteria, and CNS dysfunction secondary to RP was decided by clinical manifests, CSF analysis and brain MRI.
Results: Of 7 cases, 3 were confirmed RP, and 4 probable. All of these RP patients with CNS involvement presented as encephalitis. The common clinical features of CNS involvement were fever and headache. Brain MRI findings were in diversity. The CNS symptoms were relieved after steroid.
Conclusions: CNS involvement in RP has no specific findings both in symptoms and in brain MRI findings. When one patient presenting with encephalitis has extra-CNS manifestations such as eye and ear abnormalities, CNS involvement of RP should be suspected.
Keywords
Relapsing polychondritis (RP), Central nervous system (CNS), Encephalitis
Introduction
Relapsing polychondritis (RP) is a rare autoimmune systemic inflammatory disease characterized by recurrent episodes of inflammatory and progressive destruction of the cartilaginous structures of the nose, ears, joints and tracheobronchial tree, it also affected eyes, inner ear, kidneys bloods vessels [1]. It was first described by Jaksch-Wartenhorst in 1923 and was named by Pearson in 1960. The annual incidence of the disease is about 3.5 cases per million, with greater than 600 cases worldwide, and the average age when diagnosis is 44-51 years old [2].
Clinically, the disease can involve the CNS and lead to neurological dysfunction. CNS involvement manifests in diversity including encephalitis. In 2004, Ohta reported the first case of RP with non paraneoplastic limbic encephalitis, which presented fever, headache, mental disorder, epilepsy, weakness, dizziness and so on, easily misleading to encephalitis. The reports about CNS involvement of RP are relatively rare. Here, we reported 7 cases with RP who presented clinical manifestations similar to encephalitis in order to explore clinical presentation, CSF and brain MRI characters of RP patients with CNS involvement.
Materials
In this series, 7 RP patients were diagnosed as CNS involvement in Department of Neurology, Beijing Tiantan Hospital from January 2011 to December 2015. RP was diagnosed upon McAdam modified criteria which was set up in 1976. McAdam criteria suggests that a diagnosis of RP is almost certain if three out of the following six criteria are fulfilled : (a) bilateral auricular chondritis; (b) nasal chondritis; (c) respiratory tract chondritis; (d) non-erosive seronegative polyarthritis; (e) ocular inflammation; (f) audiovestibular damage [3]. Later, McAdam criteria were modified. Upon modified criteria, RP can be diagnosed if fulfilling one of the following criteria: (a) at least three of the clinical criteria stated in McAdam criteria; (b) chondritis at two or more separate anatomic locations with response to steroids [4]. CNS involvement of RP was judged by mainly CNS symptoms besides fulfilling the modified McAdam criteria.
Clinical information
Seven cases with RP and CNS involvement were included in this study. Among them, four cases were definite RP who fulfilled all the modified McAdam criteria, and 3 cases were probable RP who only fulfilled 2 out of the 6 criteria. The average age of onset of RP was 42.3 (range 26-51) years old, female-to-male ratio was 1:6. The duration of symptoms before diagnosis ranged from fifteen days to two years. The clinical manifestations of these 7 cases are summarized in table 1.
![]()
Table 1: Summary of the clinical information, CSF and blood results in 7 RP cases with CNS involvement.
View Table 1
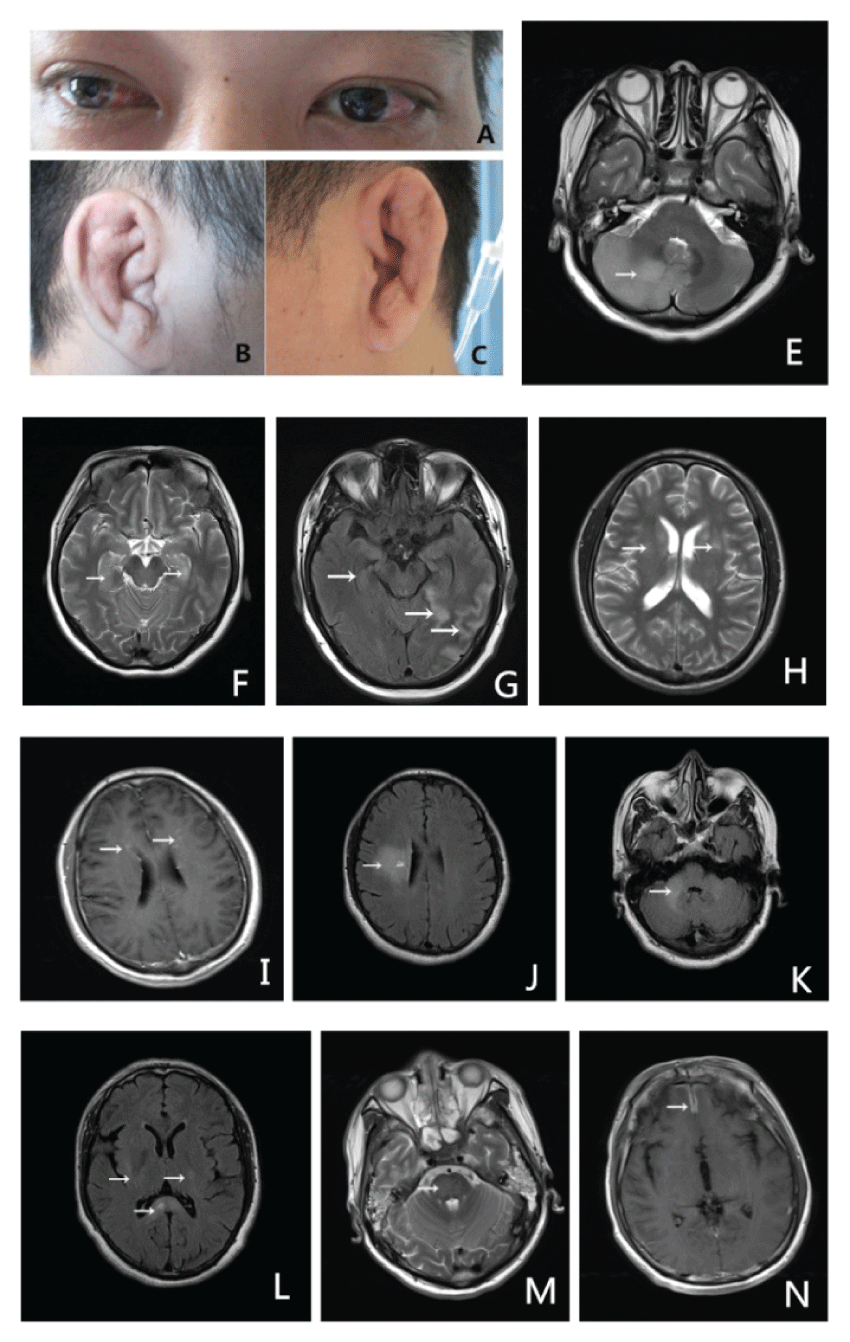
In this series, the most common clinical features of RP were scleriti (n = 7) and auricular chondritis (n = 6) as showed the redness of bilateral eyes and swelling ears (Figure 1). In addition, laryngitis, arthritis, nasal chondritis and bronchomalacia were observed in one or two cases. Skin damage, renal damage or cardiac involvement weren't found. All the symptoms of destruction of the cartilaginous structures of the nose, ears, joints and tracheobronchial tree were relieved after steroid treatment. Heache was found in all cases, with or without fever. The other CNS symptoms included mental disorder, epilepsy, aphasia, and bulbar paralysis, decrease of vision, facial palsy, limb weakness and uroschesis (Table 1).
The CNS symptoms and cartilaginous destruction features were occurred at the same time in two cases, and CNS symptoms appeared before cartilaginous features in four cases. There was also a case that cartilaginous manifests appeared ahead.
Serum and CSF analysis
Blood WBC counts elevated in 6 cases, ESR increased in 5 cases, and CRP increased in 6 cases (Table 2). In 3 cases, intracranial pressure was high. CSF WBC count increased in six cases and protein elevated in three cases. All the findings in blood and CSF implied the possibility of inflammation in CNS.
![]()
Table 2: The lab results in CSF and blood.
View Table 2
Brain MRI
All cases got brain MRI scanning. MRI finding was in diversity without specific signs. 2 cases had normal MRI. 4 cases had abnormal signals in brain parenchyma (cerebellum: 2 cases (Figure 1E and Figure 1K), pons: one case (Figure 1M), and cerebral cortex: one case (Figure 1G). Moreover, thalamus, basal ganglia, corona radiate and centrum semiovale and corpus callosum could also be involved (Figure 1F, Figure 1H, Figure 1I, Figure 1J and Figure 1L). One case had meningeal enhancement in anterior longitudinal fissure (Figure 1N).
Treatment and follow-up
All of Our patients were given intravenous methylprednisolone (500 mg/d, 5 days) or dexamethasone (20 mg/d, 7 days), then oral prednisone (60 mg/d) followed and tapered gradually. After steroid therapy, both CNS and no CNS symptoms improved remarkably.
Discussion
RP is a rare disease with the incidence of approximately 3.5 per million/year [5]. CNS involvement in RP is estimated to occur with an incidence of 3% RP patients [6]. Encephalitis is one of manifestations of CNS involvement, which was first reported by Ohta, et al. in 2004 [7]. Besides encephalitis, other manifestions of CNS involvement included headache, seizures, hemiplegia, aseptic meningitis, and cerebral aneurysms [5]. In our series, symptoms of CNS involvement included fever, headache, mental disorder, dizziness, weakness or speech difficulty.
Due to the lack of specific biomarkers, the diagnosis of RP is still a challenge. McAdam criteria [3] is now widely accepted, in which RP is mainly diagnosed based on clinical features including auricular and nasal chondritis, ocular inflammation, nonerosive inflammatory polyarthritis, respiratory tract chondritis and audiovestibular damage. A definite RP is made when three of six clinical features are present along with the histological findings of affected cartilage which are loss of basophilic staining of the cartilage matrix, perichondrial inflammation, and eventual destruction of cartilage replaced by fibrotic tissue [7]. In our patients, two cases had three clinical features, and the others had two. All of them lacked of tissue biopsy. It should be stressed that all of our patients had auricular chondritis and ocular inflammation which may be a symbol of RP.
Patients with CNS involvement in RP sometimes have CSF profiles mimicking meningoencephalitis. Wang, et al. described 4 patients with RP who were suspected as meningoencephalitis upon elevated WBC and protein in CSF [8]. All of our patients were considered as viral encephalitis or meningitis at the local hospital based on the elevation of WBC count (4 cases) and increase of protein content (2 cases) in CSF. These findings remind us that encephalitis should be differentiated carefully. One should pay much attention to extra-CNS manifestations which maybe is a clue of final diagnosis, for example, swelling nose, cauliflower ears and redness eyes are helpful to the diagnosis of RP.
The pathogenesis of RP arises from an immunologic reaction to type II collagen, with specific circulating antibodies present in approximately two-thirds of patients with RP [9]. The mechanism of CNS involvement in RP may be related to vasculitis [10]. However, Kashihara, et al. found positive anti-CluR antibodies in sera and CSF of a RP patient with limbic encephalitis [11], thus mechanism of CNS involvement in RP may be complicated.
Brain MRI findings in CNS involvement of RP are no specific. In a report, some RP patients presented with encephalitis had lesions in the temporal lobes on brain MRI [12]. Another paper described a RP patient with bilateral, small disseminated high-intensity signals with vague margins in the medial temporal lobe, hippocampus, and insular cortex [13], which was similar to brain MRI findings in our patient 2. Our patient 4 showed multiple lesions in the thalamus, basal ganglia, corona radiate and centrum semiovale, which were similar to 3 reports [14-16]. Ohta Y, et al [7] reported a 57-year-old man with non paraneoplastic limbic encephalitis whose brain MRI showed hyperintense lesions in bilateral hippocampi, amygdaloidal bodies, left para-ventricular deep white matter, bilateral caudate nuclei and left putamen. Lesions in bilateral hippocampi, amygdaloidal bodies and left putamen were enhanced with Gd-DTPA. Our cases had similar findings (Figure1F, Figure1H, Figure1I and Figure 1G). Ota M, et al. [17] described a RP patient whose brain MRI showed leptomeningeal enhancement in the frontal, parietal, and posterior regions, which was similar to our patient (Figure 1N). Ducci, et al. [18] reported a RP patient with neurological symptoms who had diffuse thickening of the dura in the frontal lobes similar to our patient 3. We also found the lesions in cerebellum hemisphere, cerebellum vermis and corpus callosum which had never been reported in the previously literatures.
Glucocorticoids are effective to RP. Intravenous pulse methylprednisolone (1 g/d for 3 consecutive days) is a common option, then followed by oral prednisone [16]. Our cases improved remarkably after steroid. However, the optimal dose and the duration of steroid are still uncertain. Further study is needed.
Conclusion
In summary, CNS involvement in RP has no specific findings both in symptoms and in brain MRI findings. The diagnosis is still difficult. However, when one patient presenting with encephalitis has extra-CNS manifestations such as eye and ear abnormalities, CNS involvement of RP should be suspected. Immunotherapy including steroids and immunosuppressants may be a choice. Long-term follow-up is necessary.
Conflicts of Interest
There are no conflicts of interest.
References
-
Lahmer T, Treiber M, von Werder A, Foerger F, Knopf A, et al. (2010) Relapsing polychondritis: An autoimmune disease with many faces. Autoimmun Rev 9: 540-546.
-
Adliff M, Ngato D, Keshavjee S, Brenaman S, Granton JT (1997) Treatment of diffuse tracheomalacia secondary to relapsing polychondritis with continuous positive airway pressure. Chest 112: 1701-1704.
-
McAdam LP, O'Hanlan MA, Bluestone R, Pearson CM (1976) Relapsing polychondritis: prospective study of 23 patients and a review of the literature. Medicine (Baltimore) 55: 193-215.
-
Chuah TY, Lui NL (2016) Relapsing polychondritis in Singapore: a case series and review of literature. Singapore Med J.
-
Cantarini L, Vitale A, Brizi MG, Caso F, Frediani B, et al. (2014) Diagnosis and classification of relapsing polychondritis. J Autoimmun 48-49: 53-59.
-
Kent PD, Michet CJ Jr, Luthra HS (2004) Relapsing polychondritis. Curr Opin Rheumatol 16: 56-61.
-
Ohta Y, Nagano I, Niiya D, Fujioka H, Kishimoto T, et al. (2004) Nonparaneoplastic limbic encephalitis with relapsing polychondritis. J Neurol Sci 220: 85-88.
-
Wang ZJ, Pu CQ, Wang ZJ, Zhang JT, Wang XQ, et al. (2011) Meningoencephalitis or meningitis in relapsing polychondritis: four case reports and a literature review. J Clin Neurosci 18: 1608-1615.
-
Childs LF, Rickert S, Wengerman OC, Lebovics R, Blitzer A (2012) Laryngeal manifestations of relapsing polychondritis and a novel treatment option. J Voice 26: 587-589.
-
Hsu KC, Wu YR, Lyu RK, Tang LM (2006) Aseptic meningitis and ischemic stroke in relapsing polychondritis. Clin Rheumatol 25: 265-267.
-
Kashihara K, Kawade S, Takahashi Y (2009) Autoantibodies to glutamate receptor GluRe2 in a patient with limbic encephalitis associated with relapsing polychondritis. J Neurological Sci 287: 275-277.
-
Kao KT, Potrebic S, Evans JR (2007) Relapsing polychondritis presenting as meningoencephalitis with valvular abnormality: a case report. Clin Rheumatol 26: 1985-1988.
-
Fujiki F, Tsuboi Y, Hashimoto K, Nakajima M, Yamada T (2004) Non-herpetic limbic encephalitis associated with relapsing polychondritis. J Neurol Neurosurg Psychiatry 75: 1646-1647.
-
Massry GG, Chung SM, Selhorst JB (1995) Optic neuropathy, headache, and diplopia with MRI suggestive of cerebral arteritis in relapsing polychondritis. J Neuroophthalmol 15: 171-175.
-
Hatti K, Giuliano V (2014) Central nervous system involvement in relapsing polychondritis. J Clin Rheumatol 20: 396-397.
-
Choi HJ, Lee HJ (2011) Relapsing polychondritis with encephalitis. J Clin Rheumatol 17: 329-331.
-
Ota M, Mizukami K, Hayashi T, Sumida T, Asada T (2005) Brain magnetic resonance imaging and single photon emission computerized tomography findings in a case of relapsing polychondritis showing cognitive impairment and personality changes. Prog europsychopharmacol Biol Psychiatry 29: 347-349.
-
Ducci RD, Germiniani FM, Czecko LE, Paiva ES, Teive HA (2016) Relapsing polychondritis and lymphocytic meningitis with varied neurological symptoms. Rev Bras Reumatol.