Journal of Rheumatic Diseases and Treatment
Effect of Etanercept on Anti-Carbamylated Protein Antibodies in Patients with Rheumatoid Arthritis
Francesca Romana Spinelli, Arbi Pecani, Fulvia Ceccarelli, Cristiano Alessandri and Fabrizio Conti*
Department of Internal Medicine and Medical Specialties - Rheumatology, Sapienza University of Rome, Italy
*Corresponding author: Conti Fabrizio, Department of Internal Medicine and Medical Specialties - Rheumatology, Sapienza University of Rome, Viale del Policlinico 155 - 00161 Rome, Italy, Tel: +39.06 49974631, Fax + 39.06 49974670, E-mail: fabrizio.conti@uniroma1.it
J Rheum Dis Treat, JRDT-1-013, (Volume 1, Issue 2), Research Article; ISSN: 2469-5726
Received: April 07, 2015 | Accepted: May 18, 2015 | Published: May 23, 2015
Citation: Spinelli FR, Pecani A, Ceccarelli F, Alessandri C, Conti F (2015) Effect of Etanercept on Anti-Carbamylated Protein Antibodies in Patients with Rheumatoid Arthritis. J Rheum Dis Treat 1:013. 10.23937/2469-5726/1510013
Copyright: © 2015 Spinelli FR, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Rheumatoid Arthritis (RA) is a systemic, chronic inflammatory disease characterized by inflammation of synovial joints and production of autoantibodies such as Rheumatoid Factor and antibodies directed against modified proteins - i.e. anti-citrullinated peptides antibody (ACPA). Carbamylation, as a post translational modification, has been recently associated to RA since anti-carbamylated protein antibodies (anti-CarP) have been detected in the sera of RA patients. The effect of treatment on anti-CarP level has been never addressed before.
Through this study we aimed to investigate the short term effect of anti-TNF treatment with Etanercept on anti-CarP.
We enrolled consecutive RA patients before starting treatment with Etanercept. Clinical data and serum samples were gathered from each patient at baseline and after 3 months of treatment. Disease activity was assessed at baseline and after 3 months by using the C-reactive protein - Disease Activity Score (DAS) 28. Sixty-three age and sex matched healthy donors served as controls. Anti-Car-P antibodies were investigated by immune-enzymatic assay.
We enrolled 17 RA patients (F:M 15:2, mean age 44.1 ± 10.7 years, mean disease duration 7.9 ± 5.8 years). Six patients (35.3%) were positive for anti-CarP antibodies at baseline while three months after only 4 patients (23.5%) remained positive. Mean serum level of anti-CarP antibodies at baseline and after 3 months were: 253.0 ± 139.8AU/ml and 271.0 ± 132.4AU/ml respectively. Considering the persistently anti-CarP positive patients, the mean antibody titre increases from 386.2 ± 49.3AU/ml at baseline to 421.8 ± 144.0AU/ml at follow up.
The effect of anti-TNF treatment on autoantibody status is still controversial; in particular, data on ACPA variation during treatment are discordant. In our cohort of long standing RA patients, a short term course of Etanercept did not affect the anti-CarP status.
In conclusion, this pilot study demonstrated a slight reduction in the percentage of anti-CarP positive patients but an overall increase of antibody titres unrelated to the clinical response to TNF blockade was observed.
Keywords
Rheumatoid arthritis, Anti-TNF, Anti-carbamylated protein antibodies
Introduction
Rheumatoid Arthritis (RA) is a systemic, chronic inflammatory disease mainly affecting the synovial joints, leading to cartilage and bone erosion. A distinctive feature of RA is the production of autoantibodies such as Rheumatoid Factor (RF) and antibodies directed against modified proteins - i.e. anti-citrullinated peptides antibody (ACPA).
Post-translational modifications encompass several enzymatic or chemical reactions that modify and modulate protein functions. Among the others, carbamylation of proteins, leading to the production of homocitrulline, have been recently associated to RA. Anti-carbamylated proteins (anti-CarP) antibodies have been proposed as an additional biomarker of RA, especially in seronegative subjects and even in pre-clinical stage. As previously demonstrated for ACPA [1], anti-CarP antibodies seems to have a prognostic role since their presence is associated to a more severe and aggressive disease course [2].
The effect of treatment of anti-Car-P in RA patients has never been addressed up to now. In the present study our objective was to investigate the short term effect of anti-TNF treatment on anti-CarP serum levels.
Patients and Methods
Consecutive RA patients who were due to start treatment with Etanercept were enrolled. Patients with known cardiovascular disease (CVD) or kidney failure were excluded. Serum samples were collected at baseline and after 3 months of therapy, aliquoted and stored at -20�C until tested.
Disease activity was assessed at baseline and after 3 months by C-reactive protein (CRP) - Disease Activity Score (DAS)28.
Anti-CarP antibodies were investigated by a "home-made" ELISA as previously reported [2] using carbamylated Fetal Calf Serum (FCS) (Car-FCS) and unmodified FCS as antigens. A titration curve of two positive reference sera with medium-high ELISA immunoreactivity for anti-Car-FCS was carried out in order to show the performance of the test and to transform the absorbance of Car-FCS to arbitrary units per milliliter (aU/mL). The cut-off was established as the mean value + 3 standard deviation of 63 healthy donors.
The objective of this study was exploratory and no appropriate information to base a sample size was available. Data presented a normal distribution and were expressed as mean ± standard deviation. Differences in quantitative variables were analysed by the Student's t test while Pearson's correlation coefficient was used to assess correlation between other variables. P values < 0.05 were considered statistically significant.
Results
In this pilot study we enrolled 17 patients with long standing RA fulfilling the 2010 ACR criteria [3]. Concomitant therapy remained stable throughout the 3 months of follow-up in all the patients. Table 1 reports demographic and clinical data of the cohort.
![]()
Table 1: Demographic and clinical data of the 17 RA patients
View Table 1
At baseline, 6 patients (35.3%) were positive for ant-CarP antibodies; at follow-up, 4 patients were still positive (23.5%) while 2 patients turned negative. Mean serum level of anti-CarP antibodies in the whole cohort was 253.0 ± 139.8 AU/ml at baseline and 271.0 ± 132.4 AU/ml at the third month of Etanercept treatment. (Figure 1). Considering the sub-population of anti-CarP positive patients, the mean antibody titre was 386.2 ± 49.3 AU/ml at baseline and increased to 421.8 ± 144.0 AU/ml after 3 months (Figure 1). After 3 months of anti-TNF treatment with Etanercept we detected a significant decrease of DAS28 (5.14 ± 1.3 to 3.73 ± 1.3, p=0.003).
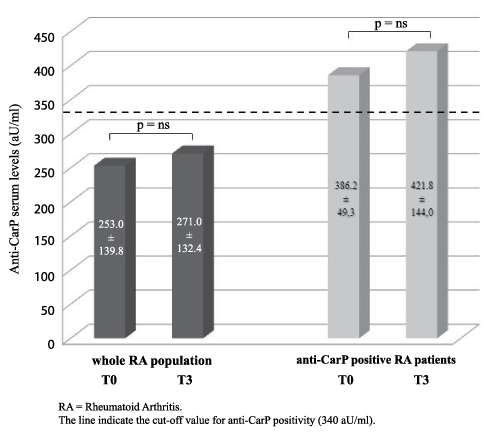
.
Figure 1: Variation of anti-CarP serum levels during Etanercept treatment in the whole cohort of patients with Rheumatoid Arthritis (left) and in the sub-group of positive patients (right).
View Figure 1
At baseline, anti-CarP positive patients presented with a high disease activity (DAS28=5.9 ± 1.2). All the 4 patients persistently positive for anti-CarP showed a clinically meaningful reduction of DAS28 (-2.8 ± 2.3) and were considered EULAR moderate responders; one of them was considered in remission, another one showed a low disease activity and the remaining two a moderate disease activity. We did not find any correlation between anti-Car-P serum level and DAS28 at baseline nor at follow-up.
Discussion
This pilot study is the first attempt to investigate a possible effect of anti-TNF treatment on anti-CarP status. A short term course of Etanercept seems not to affect anti-CarP serum levels in a small cohort of RA patients.
Post-translational modifications of self-antigens are responsible for the formation of neo-epitopes that give rise to (auto)-antibodies formation. Besides RF and ACPA, anti-Car-P antibodies have recently gained interest as additional diagnostic and prognostic marker of RA. Carbamylation is a post-translational modification in which cyanate binds to amino or thiol groups; this modification is determined by increase of blood urea nitrogen levels (i.e. kidney failure), inflammation [4] or enzymatic conversion of lysine residues into homocitrulline [5].
Recently, Shi et al. [2] started to investigate the immunogenicity to homocitrullinated peptides in RA. Antibodies to carbamylated proteins were detected both in ACPA positive and ACPA negative patients suggesting that anti-citrullinated peptide and anti-homocitrullinated peptides are two separate families of autoantibodies; however, the authors did not definitively exclude certain cross-reactivity between the two classes of antibodies [2]. Moreover, anti-CarP showed a strong association with an erosive disease, especially in seronegative patients [2].
Like RF and ACPA [6,7], even anti-CarP can precede the clinical onset of RA. Reactivity to carbamylated-FCS was detected in 39% of patients with inflammatory arthralgia who develop an overt RA within a median time of 12 months [8]. Moreover, anti-CarP (FCS and fibrinogen) were detected in sera collected from healthy subjects many years before the development of RA. The detection of anti-CarP in pre-clinical and early stage of the disease suggests a role - still not fully elucidated - for these antibodies in the pathogenesis of RA.
The effect of treatment on anti-CarP status is still not known. To the best of our knowledge, the present study is the first one aimed to investigate the short term effect of TNF inhibition on anti-CarP serum levels. It was not possible to observe a significant variation of anti-CarP levels in the 17 long-standing RA patients treated with Etanercept. Data on the effect of anti-TNF drugs on ACPA and relationship between decrease of ACPA and clinical response are somehow controversial. In 2004, Alessandri et al were among the first to investigate the effect of TNF inhibition on ACPA and demonstrate a decrease titres of RF and ACPA in patients showing clinical improvement [9]. In the last decade, many authors addressed the same topic showing contrasting results: some authors identified a reduction of ACPA levels while other did not detected any effect of anti-TNF drugs on ACPA titre [10].
Unexpectedly, in our cohort we observed an increase of anti-CarP serum levels, not correlating with the disease activity. The relationship between anti-CarP titres and response to treatment is still unknown. The results of this pilot study suggest a dissociation between serum levels of anti-CarP and reduction of disease activity even in patients who showed an increase of antibody titres after anti-TNF treatment.
Disease duration seems to be one of the factors affecting ACPA response during anti-TNF therapy: shorter disease duration (less than one year) was more likely associated to autoantibodies negativization [10]. The long disease duration of the cohort described in the present study might have influenced the low variation of anti-CarP during the follow-up. The results of this study should be interpreted cautiously since this is a pilot study on a small cohort of patients. Moreover, the short term of the observation could be insufficient to catch a modification of antibody titre.
In conclusion, this pilot study aimed at evaluating the short term effect of anti-TNF on anti-CarP serum levels and status showed a slight reduction of percentage of positive patients but an overall increase of antibody titres unrelated to the clinical response to TNF blockade.
Ethical Statement
All procedures of the study were conducted following the ethical standards on human experimentation. Informed consent was obtained from all the patients for being included in the study.
References
-
Aggarwal R, Liao K, Nair R, Ringold S, Costenbader KH (2009) Anti-citrullinated peptide antibody assays and their role in the diagnosis of rheumatoid arthritis. Arthritis Rheum 61: 1472-1483.
-
Shi J, Knevel R, Suwannalai P, van der Linden MP, Janssen GM, et al. (2011) Autoantibodies recognizing carbamylated proteins are present in sera of patients with rheumatoid arthritis and predict joint damage. Proc Natl Acad Sci USA 108: 17372-17377.
-
Aletaha D, Neogi T, Silman AJ, Funovits J, Felson DT, et al. (2010) 2010 rheumatoid arthritis classification criteria: an American College of Rheumatology/European League Against Rheumatism collaborative initiative. Ann Rheum Dis 69: 1580-1588.
-
Wang Z, Nicholls SJ, Rodriguez ER, Kummu O, Horkko S, et al. (2007) Protein carbamylation links inflammation, smoking, uremia and atherogenesis. Nat Med 13: 1176-1184.
-
Carter AL, Eller AG, Rufo S, Metoki K, Hommes FA (1984) Further evidence for a separate enzymic entity for the synthesis of homocitrulline, distinct from the regular ornithine transcarbamylase. Enzyme 32: 26-36.
-
Rantapaa-Dahlqvist S, de Jong BA, Berglin E, Hallmans G, Wadell G, et al. (2003) Antibodies against cyclic citrullinated peptide and IgA rheumatoid factor predict the development of rheumatoid arthritis. Arthritis Rheum 48: 2741-2749.
-
Bos WH, Wolbink GJ, Boers M, Tijhuis GJ, de Vries N, et al. (2010) Arthritis development in patients with arthralgia is strongly associated with anti-citrullinated protein antibody status: a prospective cohort study. Ann Rheum Dis 69: 490-494.
-
Shi J, van de Stadt LA, Levarht EW, Huizinga TW, Toes RE, et al. (2013) Anti-carbamylated protein antibodies are present in arthralgia patients and predict the development of rheumatoid arthritis. Arthritis Rheum 65: 911-915.
-
Alessandri C, Bombardieri M, Papa N, Cinquini M, Magrini L et al. (2004) Decrease of anti-cyclic citrullinated peptide antibodies and rheumatoid factor following anti-TNFalpha therapy (infliximab) in rheumatoid arthritis is associated with clinical improvement. Ann Rheum Dis 63: 1218-1221.
-
Modi S, Soejima M, Levesque MC (2013) The effect of targeted rheumatoid arthritis therapies on anti-citrullinated protein autoantibody levels and B cell responses. Clin Exp Immunol 173: 8-17





