Journal of Hypertension and Management
Usefulness of Morning Home Blood Pressure Measurements in Non-Obese and Obese Japanese Patients with Type 2 Diabetes Mellitus: Results of a 10-Years, Prospective and Longitudinal Study
Kyuzi Kamoi*
Department of Medicine, Ojiya General Hospital, Ojiya, Niigata 947-8601, Japan
*Corresponding author:
Dr. Kyuzi Kamoi, Department of Medicine, Ojiya General Hospital 3-4-36 Hanazono Nagaoka, Niigata 940-0845, Japan, Tel: +81-0258-36-3986; Fax: +81-0258-36-3986; E-mail: kkam-int@echigo.ne.jp
J Hypertens Manag, JHM-1-004, (Volume 1, Issue 1), Original Article; ISSN: 2474-3690
Received: September 07, 2015 | Accepted: November 03, 2015 | Published: November 05, 2015
Citation: Kamoi K (2015) Usefulness of Morning Home Blood Pressure Measurements In Non-Obese and Obese Japanese Patients with Type 2 Diabetes mellitus: Results of a 10-Years, Prospective and longitudinal Study. J Hypertens Manag 1:004. 10.23937/2474-3690/1510004
Copyright: © 2015 Kamoi K. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abbreviations
BP: Blood pressure, BMI: Body mass index, CBP: Clinic blood pressure, CI: Confidence intervals, CHD: Coronary heart diseases, CVD: Cerebrovascular diseases, DBP: Diastolic blood pressure, HbA1c: Glycated hemoglobin A1c, HBP: Home blood pressure, HDL: High density lipoprotein, HT: Hypertension, LDL: Low density lipoprotein, NGSP: National gycohemoglobin standardization program, NT: Normotension, PAO: Peripheral artery obstruction, SBP: Systolic blood pressure, T2DM: Type 2 diabetes mellitus, TC: Total cholesterol, TG: Triglyceride, UAER: Urinary albumin excretion rate
Abstract
Aim: It was demonstrated that home blood pressure (HBP) has a stronger predictive power for death, micro- and macrovascular complications than clinic blood pressure (CBP) in patients with type 2 diabetes mellitus (T2DM). This study investigated which of these measurements offers predicatively stronger power for outcomes over 10 years in non-obese and obese patients with T2DM.
Methods: At baseline and end-point, 400 Japanese patients with T2DM were classified as having non-obesity or obesity with hypertension or normotension. Body mass index with < 25.0 kg/m2 and ≧25.0 kg/m2, and same thresholds of systolic blood pressure with ≥ 130 mmHg and < 130 mmHg are defined as non-obesity and obesity, and hypertensions and normotensions, respectively. Mean survey duration was 95 months. Primary and secondary outcomes were death, and new or worsened micro- and macrovascular events, respectively. Differences in outcomes for end-point were analyzed using Kaplan-Meier survival curves and log-rank testing. Associated risk factors were assessed using Cox proportional hazards analysis.
Results: Based on HBP, incidences in death, and micro-and macrovascular events were significantly higher in obesity than in non-obesity. However, based on CBP, there were no significant differences of incidences in their vascular events between obesity and non-obesity. One risk-factor associated with obese patients with elevated HBP was therapy for hypertension.
Conclusions: This 10-years study of patients with T2DM demonstrated that elevated HBP is more predictive death and micro- and macrovascular complications in obesity than in non-obesity.
Introduction
It was demonstrated that home blood pressure (HBP) measured in the morning at upon-awakening has better predictive power for death and micro- and macrovascular complications in patients with type 2 diabetes mellitus (T2DM) than casual/clinic blood pressure (CBP) measured [1-3].
Since early time, it is known that obesity in patients with T2DM has a risk-factor for hypertension (HT) measured on CBP [4-6], which influences vascular complications. The study examined whether CBP or HBP measurements provided stronger predictive power for outcomes by comparing cumulative events between non-obese and obese patients with T2DM with either HT or normotension (NT) over 10 years.
Materials and Methods
Subjects
Subjects comprised 400 Japanese patients with T2DM enrolled between 1999 and 2005 [3], who were divided into two groups with non-obesity and obesity [7].
Subjects were followed up for all-cause morbidity and mortality. All participants visited our clinic regularly and were followed until March 31, 2013. T2DM was diagnosed according to World Health Organization criteria [8], which is required that glycated hemoglobin (HbA1c) level is greater than 6.5% as national glycohemoglobin standardization program (NGSP). All HbA1c values were converted to NGSP values according to the Japan Diabetes Society [9].
Baseline characteristics of participants have been described as table 1. At the beginning of study, 329 patients (82%) were receiving treatment with oral hypoglycemic drugs and/or insulin regimens for T2DM and 196 patients (49%) were receiving treatment with various anti-hypertensive drugs for HT [3]. All patients were fully informed on purposes and procedures for the study and provided oral consent at enrolment and the approval of local ethical committee. This study was a registered clinical trial (Clinical Trial reg. no. NCT00760110)
![]()
Table 1: Clinical characteristics of non-obese and obese patients with type 2 diabetes mellitus on blood pressure measured at basal and end-point, respectively.
View Table 1
Methods
Chemical laboratory data: All chemical laboratory data were obtained at each clinic visit in a non-fasting state for each 3-month. A single specimen was used to assess levels of blood HbA1c, serum creatinine, serum lipid and urinary albumin excretion rate (UAER) based on 2009 guidelines of the American Diabetes Association [10]. Briefly, HbA1c was measured by high-performance liquid chromatography [1-3,11] and expressed as NGSP equivalent [9]. Serum levels of creatinine (mg/dl) and triglyceride (TG) (mg/dl) were measured by enzyme color methods [1-3,11]. Serum levels of total cholesterol (TC) (mg/dl), high density lipoprotein (HDL) (mg/dl) and low density lipoprotein (LDL)(mg/dl) were measured by direct methods [1-3,11]. Albumin concentration in random spot urine was measured by latex agglutination photometric immunoassay method [1-3,11]. Micro albuminuria and clinical albuminuria were defined as UAER ≥ 30 mg/g creatinine and ≥ 300 mg/g creatinine, respectively [10].
BMI: A definition of obesity on BMI is different between the Japan, and the U.S.A. and the Europe [7]. In the Japan, < 25.0 kg/m2 and ≧ 25.0 kg/m2 in BMI are defined as non-obesity and obesity, respectively, whereas in the USA and the Europe, from ≧ 25.0 kg/m2 to < 30.0 kg/m2 in BMI is defined as overweight [7].
Blood Pressure: CBP and HBP were assessed for the values measured once in each clinic visit and in the same morning at each clinic visit within 10 minutes after awakening in the sitting position, respectively [1,3]. Systolic blood pressure (systolic BP) with ≥ 130 mmHg was defined as HT of CBP or HBP, whereas systolic BP with < 130 mmHg was defined as NT of CBP or HBP [1]. The reason underlying that same threshold used for CBP and HBP was based on criteria of the 1999 World Health Organization-International Society of Hypertension guidelines [12], because of starting in 1999. HT of CBP and NT of HBP were defined as white coat HT [13-15], whereas NT of CBP and HT of HBP were defined as masked HT [13-15].
Based on CBP, subjects were divided into patients with HT and NT, and use of anti-hypertensive drug was determined in each group [3,13-15]. Sustained HT and sustained NT were defined from baseline to end-point, respectively [13-15]. In addition, based on HBP or CBP, subjects were divided into patients with HT and NT [3]. Recent guide-lines of HT indicated the different thresholds of NT, that is, systolic HBP is less than 125 mm and systolic CBP is less than 130 mmHg [1,13-15].
Microvascular complications: Microvascular complications included nephropathy, neuropathy and retinopathy. Severity of nephropathy was determined based on albuminuria using 4 categories: normal, 0 points; microalbuminuria, 1 point; clinical albuminuria, 2 points; and dialysis, 3 points [3]. Severity of neuropathy was categorized using 2 categories: normal, 0 point; sensorimotor distal symmetric polyneuropathy and/or cardiac autonomic neuropathy, 1 point. Severity of retinopathy was determined using 4 categories: normal, 0 point; simple, 1 point; pre-proliferative, 2 points; and proliferative, 3 points. Development of new, worsened, or improved micro angiopathy was defined according to a change of at least one step from baseline [1,16,17]
Macrovascular complications: Macrovascular complications included cerebrovascular disease (CVD), coronary heart disease (CHD) and peripheral artery obstruction (PAO). Severity of macrovascular events was categorized using 2 categories: normal, 0 point; and CVD, CHD or OAO, 1 point [3]. New, worsened (recurrent) or improved events were defined based on clinical manifestations and treatment with the study [1,16,17].
Study outcome at end-points: Outcome results considered only the first event in each subject [3]. Primary end-point was death from any cause [3]. Secondary end-points were improved or new and worsened micro- and macrovascular events [1,16,17]. The 6-month interval minimizes bias due to the fall or rise in BP [18].
Risk factors at end-point: Risk-factors at end-point in obese participants related to each outcome were determined, and therapy which was added to baseline therapy used for HT of HBP was recorded at end-point. For ethical reasons, patients were treated with various antihypertensive, anti-diabetic, anti-dyslipidemic, anti-hypercoagulation and anemic agents during course of the study by their own doctors [3].
Statistical analysis
Base-line and end-point of clinical characteristics: All results are presented as means ± SD. Mean values were compared by paired or unpaired student t test. Prevalence of micro- and macrovascular complications or medical treatments in non-obese and obese patients with or without HT at base- and end-points using CBP or HBP were compared [3,13-16]. Fisher's exact test was used, and then hazard ratios and 95% confidence intervals (CI) were calculated [3]. Further, in the obese patients, HT and NT at base-point for various vascular complications were calculated odds ratio and receiving operating characteristics (ROC) curve [1].
Relationship between morning home blood pressure at base- and end-point and body mass index: The relationships between morning HBP (mmHg) at base- and end-point and BMI (kg/m2) were calculated by Pearson methods.
End-points and outcome measures: Differences in primary and secondary outcomes between non-obese and obese patients with HT and NT on CBP or HBP using the same threshold of NT were assessed by Kaplan-Meier survival curves and then compared by hazard rate using log-rank test [3,16], respectively..In addition, events in primary and secondary outcomes between HT and NT using the different thresholds of NT were assessed by the same methods mentioned above. The difference in overweight patients was examined by the same methods
Risk factor assessment for outcomes: Risk-factors determined to be statistically related to outcomes in the obese patients were assessed by Cox proportional hazard analysis [3].
All analysis was performed using the Prism version 6.03 software (GraphPad Software, CA, USA) and the Statistical Package for the Bioscience version 6.67 (ComWorks Co, Tokyo, Japan). Two-tailed values of P < 0.05 were considered statistically significant.
Results
Clinical characteristics of non-obese and obese patients with type 2 diabetes mellitus on blood pressure measured at base-and end-points
Body weight: On base- and end-points, 247 and 284 patients were fulfilled the criteria as non-obesity, respectively (Table 1), whereas 153 and 116 patients were fulfilled the criteria as obesity, respectively (Table 1), whose characteristics showed in table 1. At basal point, 205 (83%) of the 247 non-obese patients were continued and 42 (17%) of them changed into obesity, whereas 74 (48%) of the 153 obese patients were continued and 79 (52%) of them changed into non-obesity.
Blood pressure: Based on CBP, at base-point, 121 (49%) of the non-obese patients had HT and 126 (51%) of them had NT, whereas at end-point, 147 (51%) of the non-obese patients had HT and 137 (49%) of them had NT. On the hand, at base-point, 120 (78%) of the obese patients had HT and 33 (22%) of them had NT, whereas at end-point, 54 of the obese patients had HT and 62 of them had NT. In them of the non-obese patients, 89 (36%) with HT were continued until end-point and 63 (26%) with NT were sustained until end-point, whereas in them of the obese patients, 69 (45%) with HT were sustained and 25 (16%) with NT were continued. No significant differences in systolic or diastolic CBP at base- and end-points were shown between the non-obesity and the obesity (Table 1 and Table 2). Therapies for HT were insignificantly between the non-obesity and the obesity (Table 1 and Table 3).
![]()
Table 2: Primary and secondary outcomes based on HBP* and CBP** measured at end-point in 116 obese t patients with type 2 diabetes mellitus.
View Table 2
![]()
Table 3: Risk factors for each outcome of events morning hypertensionat end-pointin 116 obese patients with type 2 diabetes mellitus
View Table 3
Based on HBP, at base-point, 161 (65%) of the non-obese patients had HT and 86 (35%) of them had NT, whereas at end-point, 64 (23%) of the non-obese patients had HT and 220 (77%) of them had NT. On the hand, at base-point, 61 (40%) of the obese patients had HT and 92 (60%) of them had NT, whereas at end-point, 39 (34%) of the obese patients had HT and 77 (66%) of them had NT. Fifty one (21%) with HT in the non-obese patients at base-point were sustained and 70 (21%) with NT in them were continued. Whereas 55 (36%) with HT in the obese patients were sustained and 24 (16%) with NT in them were continued. Systolic or diastolic HBP level at base-point was significantly higher in the obesity than in the non-obesity (Table 1). Incidence of patients with masked HT at end-point were significantly (P < 0.001) greater in the obese patients than in the non-obese patients.
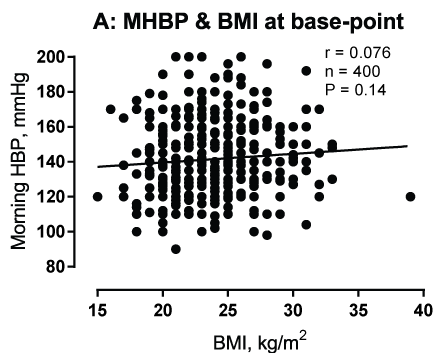
Relationships between HBP at basal and end-point and BMI: The relationships between morning HBP (mmHg) at base- and end-point, and BMI (kg/m2) were described as shown in (Figure 1A and Figure 1B). There was significant relationship between morning HBP at end-point and BMI in 400 patients with T2DM (Figure 1B).
.
Figure 1a: Relationship morning home blood pressure (MHBP) (Y axis) and body mass index (BMI) (X-axis) measured at base-line was shown.
View Figure 1a
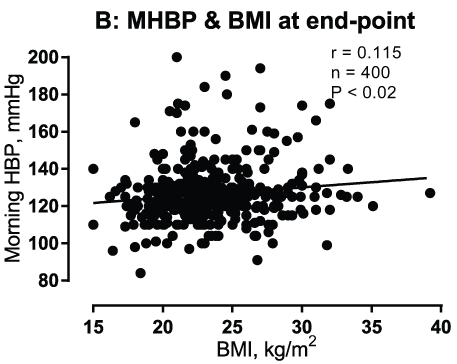
.
Figure 1b: Relationship morning home blood pressure (MHBP) (Y axis) and body mass index (BMI) (X-axis) measured at end-point was shown. The each relationship was calculated by Pearson method.
View Figure 1b
Other variables: Means of age and duration of discovered diabetes mellitus were long (Table 1). The values of TG and UAER at basal point, and HbA1c, HDL and TG at end-point were significantly higher in the obese patients than in the non-obese patients. Therapies for other diseases were insignificantly between the non-obesity and the obesity (Table 1 and Table 3).
End-points and outcome
Primary outcome: In terms of the primary outcome, mean survey duration until end-point in obese patients was 85 ± 40 months (range, 1-120 months). Eighty one cumulative deaths in the patients were observed over 10 years (Table 2). The causes were cancer, CVD, CHD, respiratory diseases and other diseases in 36, 18, 14, 6 and 7 patients (n = 81), respectively. Among them, 10, 9, 4 and 2 patients (n = 25) at end-point in the obese patients were due to cancer, CVD, CHD and other diseases. On the other hand, there was significant difference in events of death using the different thresholds of HBP and CBP in the obese patients (Table 4), whose incidence of HT of HBP was increased from 47 to 73 persons. Significantly more patients were receiving anti-hypertensive agents in patients using HBP with HT at end-point in comparison with those at baseline. In patients using HBP with sustained HT, 7 patients at baseline refused to use increased doses or new medicines for HT, whereas 32 patients at baseline achieved NT after the treatment. The hazard ratio in death in the obese patients using HBP at end-point was significantly higher in HT than in NT (Table 2), and value of difference was significantly (P = 0.0024) lower in CBP than in HBP (Table 2). Twenty one cumulative deaths in overweight patients were observed over 10 years (Table 6). The causes in 9, 7, 3, 1 and 1 patients (n = 21) in overweight patients were CVD, cancer, hepatic disease and respiratory disease. There were significant differences between with HT and NT using HBP in the overweight patients as the Kaplan-Meier method (Table 6).
![]()
Table 4: Primary and secondary outcomes based on HBP# and CBP## measured at end-point in 116 obese patients with type 2 diabetes mellitus.
View Table 4
![]()
Table 5: Primary and secondary outcomes based on HBP* and CBP** at end-point in 284 non-obese patients with type 2 diabetes mellitus.
View Table 5
Secondary outcomes
a. Microvascular complications: Mean survey duration until the end-point in the 116 obese patients related to microvascular complication was 85 ± 38 months (range 6 -120 months).
The complication was observed in 71 patients in the obese patients over 10 years (Table 2). An improved event was observed in 15 patients including 10 with neuropathy and 5 with nephropathy, whereas 20 patients had new or worsened complications. Forty two patients had no changes until end-point. At end-point, there were significant differences in events of microvascular complication in the obese patients using the same threshold of NT between patients with HT and NT as the Kaplan-Meier method (Table 2). There was no significant difference in the events using the different threshold at end-point in the obese patents, although whose incidence of HT of HBP was increased from 47 to 73 persons. Hazard rate was significantly (2 fold) higher in the obese patients than in non-obese patients (Table 2).Although ROC curve showed that there was no significant difference in the events between HT of and NT using the same thresholds at basal (Table 7) and end-points (Table 8) in the obese patients, the incidence of events in the obese patients had significantly higher in HT than in NT (Table 4 and Table 9). Accordingly, elevated HBP in obese patients may be related to microvascular complications.
![]()
Table 6: Primary and secondary outcomes based on HBP* and CBP** at end-point in 96 overweight patients with type 2 diabetes mellitus.
View Table 6
![]()
Table 7: ROC curve for micro-and macrovascular complications in comparison with morning HBP and CBP at basal point in 153 obese patients with type 2 diabetes mellitus
View Table 7
b. Macrovascular complications: Mean survey duration until end-point related in the 116 obese patients to macrovascular complication was 38.4 ± 30 months (range 7.2-108 months). The events were seen in 25 of the obese patients over 10 years (Table 2). Although cumulative events of macrovascular events were insignificant (P = 0.059) between non-obese patients and obese patients, the incidence in the obese patients had a tendency of high compared with that in the non-obese patients. Among them in the obese patients, no changes were shown in 12 patients and new or worsened events were shown in 14 patients. Events in the obese patients using HBP was also significantly higher in sustained HT than in sustained NT as the Kaplan-Meier method. Further, events based on HBP using the different threshold in the obese patients were significantly higher in HT than in NT (Table 4). In addition, although ROC curves for the events in HBP at base-and end-points using the same thresholds in the obese patients were not significantly different (Table 7 and Table 8), the events in HBP at base-and end-points using the same thresholds were also significantly higher in HT than in NT (Table 9 and Table 10).The hazard rate in the obese patient in HBP using the same thresholds of NT was significantly (3 fold) higher in HT than in NT (Table 2). Accordingly, obese patients with elevated of HBP may be related to macrovascular complications
![]()
Table 8: ROC curve for death, micro- and macrovascular complications for micro- and macrovascular events in comparison with morning HBP and CBP at end-point in 116 obese patients with type 2 diabetes mellitus.
View Table 8
![]()
Table 9: Evaluations with morning HBP or CBP between HT and NT at end-point for death, and micro- and macrovascular events in 116 obese patients with type 2 diabetes mellitus.
View Table 9
Risk factor assessment for outcomes
Death, age, UAER, macrovascular complications and therapy for hyper coagulation or HT using HBP and the same threshold of BP were significant risk-factors in the obese patients, although the hazard rate of therapy for HT was less than 1.0 (Table 3). Events of micro- and macro vascular complications and therapy for dyslipidemia or HT were also significant risk-factors in the obese patients (Table 3), although hazard rate of therapy for HT was also less than 1.0.
![]()
Table 10: Evaluations with morning HBP or CBP between HT and NT at basal point for micro- and macrovascular events in 153 obese patients with type 2 diabetes mellitus.
View Table 10
Discussion
Ages in patients with non-obesity and obesity were old. Subsequently, many patients had HT [4]. Recent guidelines have recommended that BP of threshold for HBP should be lower by 5-10 mmHg than that for CBP [13-15]. In this study, the same threshold of NT for CBP and HBP groups were used based on guidelines in place when this study began [12]. Nevertheless, cumulative events of death were significantly higher in the obese patients than in the non-obese patients.
Cumulative events of microvascular complications were also significantly higher in the obese patients than in the non-obese patients, and using HBP, there was significantly higher in HT than in NT, while no significant difference using CBP was seen. Cumulative events of macrovascular complications in the obese patients using HBP was significantly higher in HT than NT, although no significant difference using CBP at end-point was seen. This study also showed that the obese patients at base-point had high TG and increased UAER compared with the non-obese patients. The findings are consistent with finding previously reported [4-6,9-22].Furthermore, it demonstrated first that incidences of dead and cumulative vascular events in patients with HT using HBP at end-point were higher in obesity than in non-obesity. In the overweight patients according to guideline of the U.S.A. and the Europe [7], there were significantly more differences in micro- and macrovascular events using the same thresholds at end-point in HT than in NT. Therefore, although definition of obese is different between Japanese and non-Japanese patients with T2DM [7], the finding may be given to non-Japanese patients with T2DM.The significant relationship between morning HBP at end-point and BMI was supported this view.
Death and cumulative event of microvascular complications were related to occurring events of macrovascular disturbances and were decreased by therapy for HT of HBP and therapy treated with anti-coagulation in the obese patients. Hazard rates of primary and secondary outcomes in the obese patients using HBP were higher in HT than in NT. Measurement HBP has no gratification in not only patients also staffs of medical facilities, because that it has a nuisance or a troublesome [23-26]. However, it is demonstrated that measurement of HBP in obese patients with T2DM is necessary as this study.
All findings indicated that incidences of death and cumulative events of micro-and macrovascular complications were significantly higher in obesity than in non-obesity, and those in the obese patients were strongly related to HT of HBP and were similar to results of the Ohasama study [18,19], supporting the view that HBP in the obese patients has a strongly prognostic value compared in the non-obese patients. Based on the results of the present study, obesity with HT of HBP may be added to the list of risk factors in patients with T2DM [5,6].
Limitations
First, numbers of the non-obese and the obese patients, and events occurring over 10 years were heterogeneous and small, respectively. Therefore, we were unable to survey outcomes and compare differences among groups of patients with HT and NT of CBP or HBP at baseline as a cohort study, which would have provided clinically valuable information.
Second, there was no evening or 24-hour BP measurement. We classified patients into HT or NT groups based on CBP and HBP at baseline and end-point, and compared differences in cumulative events between these groups. These patients' classifications obviously overlapped.
Third, for ethical reasons, most patients received treatment with antihypertensive agents and other medications during follow-up. Conventionally, antihypertensive drugs are prescribed based on CBP values, but currently, we prescribe those drugs at bedtime based on values of morning HBP [3]. However, some patients refused dosage increases or changes in medications for HT identified based on values of morning HBP. Reasons for refusal were not due to high costs or side effects of medication, but rather to patients' and physicians' lack of acceptance of HBP values for medication adjustments. In addition, some patients may be prescribed both morning and evening doses for antihypertensive agents. If a patient takes the evening dose, the morning HBP may be controlled, but during the day, as that dose wears off, BP levels may rise again. However, we did not have BP readings based on ambulatory blood pressure monitoring. Accordingly, we were unable to examine outcomes without changing treatment from baseline over 10 years to determine the influence of these drugs. Therefore, it can be argued that it is not appropriate to classify patients who have been taking antihypertensive drugs into groups with HT or NT.
Fourth, prognostic values of CBP and HBP should be assessed as not only categorical data but also continuous data. The analysis using continuous variables may give more significant meaning, but in this study, BP as a continuous variable showed high fluctuations and the numbers of participants was small.
Conclusion
This prospective study of patients with T2DM for 10 years demonstrated that elevated morning HBP measured is significantly predictive death, and events of micro- and macrovascular complications in obese patients than in non-obese patients, suggesting that elevated HBP in patients with T2DM, in particular obese patients may be needed to decrease for preventing death, and micro and macrovascular complications.
Acknowledgments
There was no funding for this study.
References
-
Kamoi K, Miyakoshi M, Soda S, Kaneko S, Nakagawa O (2002) Usefulness of home blood pressure measurement in the morning in type 2 diabetic patients. Diabetes Care 25: 2218-2223.
-
Kamoi K, Ito T, Miyakoshi M, Minagawa S (2010) Usefulness of home blood pressure measurement in the morning in patients with type 2 diabetes: long-term results of a prospective longitudinal study. Clin Exp Hypertens 32: 184-192.
-
Kamoi K (2015) Usefulness of morning home blood pressure measurements in patients with type 2 diabetes mellitus: results of a 10-year, prospective, longitudinal study. Clin Exp Hypertens 37:122-127.
-
Stone MC (1980) Hypertension. The influence of age, sex and other risk factors. J R Coll Gen Pract Occas Pap 6-10.
-
Colosia DA, Palencia R, Khan S (2013) Prevalence of hypertension and obesity in patients with type 2 diabetes mellitus in observational studies: a systematic literature review. Diabetes Metab Syndr Obes 6: 327-338.
-
Richard NR (2009) Obesity-related hypertension. Ochsner J 9:133-136.
-
Examination Committee of Criteria for 'Obesity Disease' in Japan; Japan Society for the Study of Obesity (2002) New criteria for 'obesity disease' in Japan. Circ J 66: 987-992.
-
(1999) Definition, diagnosis and classification of diabetes and its complications. Part 1: diagnosis and classification of diabetes mellitus. World Health Organization, Department of Noncommunicable Disease Surveillance, Geneva.
-
Seino Y, Nanjo K, Tajima N, Kadowaki T, Kashiwagi A, et al. (2010) Report of the committee on the classification and diagnostic criteria of diabetes mellitus. Diabetology International 1: 2-20.
-
American Diabetes Association (2009) Clinical practice recommendations 2009: standards of medical care-2009. Diabetes Care 32: S13-S61.
-
Kamoi K, Takeda K, Hashimoto K, Tanaka R, Okuyama S (2013) Identifying risk factors for clinically significant diabetic macula edema in patients with type 2 diabetes mellitus. Curr Diabetes Rev 9: 209-217.
-
(1999) 1999 World Health Organization-International Society of Hypertension Guidelines for the Management of Hypertension. Guidelines Subcommittee. J Hypertens 17: 151-183.
-
Mancia G, De Backer G, Dominiczak A, Cifkova R, Fagard R, et al. (2007) 2007 guidelines for the management of arterial hypertension: the task force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). J Hypertens 25: 1105-1187.
-
Ogihara T, Kikuchi K, Matsuoka H, Fujita T, Higaki J, et al. (2009) The Japanese Society of Hypertension guidelines for the management of hypertension (JSH 2009). Hypertens Res 32: 3-107.
-
Pickering TG, Miller NH, Ogedegbe G, Krakoff LR, Artinian NT, et al. (2008) Call to action on use and reimbursement for home blood pressure monitoring: a joint scientific statement from the American Heart Association, American Society of Hypertension, and Preventive Cardiovascular Nurses Association. Hypertension 52: 1-9.
-
(1993) The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. The Diabetes Control and Complications Trial Research Group. N Engl J Med 329: 977-986.
-
Ohkubo Y, Kishikawa H, Araki E, Miyata T, Isami S, et al. (1995) Intensive insulin therapy prevents the progression of diabetic microvascular complications in Japanese patients with non-insulin-dependent diabetes mellitus: a randomized prospective 6-year study. Diabetes Res Clin Pract 28: 103-117.
-
Ohkubo T, Imai Y, Tsuji I, Nagai K, Kato J, et al. (1998) Home blood pressure measurement has a stronger predictive power for mortality than does screening blood pressure measurement: a population-based observation in Ohasama, Japan. J Hypertens 16: 971-975.
-
Noguchi Y, Asayama K, Staessen JA, Inaba M, Ohkubo T, et al. (2013) Predictive power of home blood pressure and clinic blood pressure in hypertensive patients with impaired glucose metabolism and diabetes. J Hypertens 31: 1593-1602.
-
Burchfiel CM, Laws A, Benfante R, Goldberg RJ, Hwang LJ, et al. (1995) Combined effects of HDL cholesterol, triglyceride, and total cholesterol concentrations on 18-year risk of atherosclerotic disease. Circulation 92: 1430-1436.
-
Chen AH, Tseng CH (2013) The role of triglyceride in cardiovascular disease in asian patients with type 2 diabetes--a systematic review. Rev Diabet Stud 10: 101-109.
-
Toyama T, Furuichi K, Ninomiya T, Shimizu M, Hara A, et al. (2013) The impacts of albuminuria and low eGFR on the risk of cardiovascular death, all-cause mortality, and renal events in diabetic patients: meta-analysis. PLoS One 8: e71810.
-
Wada T, Haneda M, Furuichi K, Babazono T, Yokoyama H, et al. (2014) Clinical impact of albuminuria and glomerular filtration rate on renal and cardiovascular events, and all-cause mortality in Japanese patients with type 2 diabetes. Clin Exp Nephrol 18: 613-620.
-
Stergiou GS, Kalogeropoulos PG, Baibas NM (2007) Prognostic value of home blood pressure measurement. Blood Press Monit 12: 391-392.
-
Blacher J, Halimi JM, Hanon O, Mourad JJ, Pathak A, et al. (2013) Management of arterial hypertension in adults: 2013 guidelines of the French Society of Arterial Hypertension. Ann Cardiol Angeiol 62:132-138.
-
Peterson JC, Pirraglia PA, Wells MT, Charlson ME (2012) Attrition in longitudinal randomized controlled trials: home visits make a difference. BMC Med Res Methodol 12: 178.





