Journal of Rheumatic Diseases and Treatment
Department of Health, Physical Education & Gerontological Studies and Services, City University of New York, York College, USA
*Corresponding author: Prof. Ray Marks, Departments of Health, Physical Education & Gerontological Studies and Services, City University of New York, York College; Health and Behavior Studies, Columbia University, Teachers College, New York, USA, Tel: 1-212-678-3445, Fax: 1-212-678-8259, E-mail: rm226@columbia.edu
J Rheum Dis Treat, JRDT-1-015, (Volume 1, Issue 3), Review Article; ISSN: 2469-5726
Received: June 07, 2015 | Accepted: June 30, 2015 | Published: July 03, 2015
Citation: Marks R (2015) Anxiety and its Impact on Osteoarthritis Pain: An Update. J Rheum Dis Treat 1:015. 10.23937/2469-5726/1510015
Copyright: © 2015 Marks R. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Anxiety is a very common psychological syndrome occurring in the adult population either as a trait or specific condition, and/or in response to a variety of situations, especially adverse health conditions. This narrative review examines the extent to which anxiety may preside among adults with a diagnosis of osteoarthritis, regardless of site, and its linkage to the pain experience. Drawn from the English language peer reviewed work over the last 35 years, articles that focused on the topic of anxiety among cases with osteoarthritis were examined. Although very limited in quantity, these data showed, a sizable proportion of adults with osteoarthritis may present with comorbid anxiety problems, as well as excess anxiety in response to their situation. In most cases, those with any form of anxiety experience more pain, and have less optimal outcomes than those without anxiety. It is concluded that more attention to this correlate in the research and clinical realm will enable a more favorable outlook for the osteoarthritic patient, regardless of joint site, or disease duration.
Keywords
Anxiety, Osteoarthritis, Outcomes, Treatment
Introduction
Psychological conditions, such as anxiety, are highly prevalent among adults in general, as well as adults with a variety of health conditions [1-3]. Frequently associated with depression [3,4], anxiety, which may occur independently in different forms, including preexisting trait anxiety, generalized anxiety disorder, and state anxiety, commonly affects the individual's physical, as well as their overall health status significantly and adversely [5]. Although frequently found among one third of individuals with various forms of painful disabling arthritis, especially those with depression [6], the condition rarely receives the same attention as the physical correlates of the disease, even though these are inextricably linked.
This article provides an overview concerning the presence of anxiety and its impact in the context of osteoarthritis, a highly prevalent and painful disabling rheumatic disease, especially among older adults. It also highlights the implications of this information in the context of optimizing the outcomes for adults with this condition, regardless of disease stage.
Methods
To provide a comprehensive understanding of this topic, all relevant papers published between 1980 and June 2015 in the major data bases were extracted and reviewed. These data were specifically explored to examine whether anxiety is an important osteoarthritis disease correlate, and if so, whether pain, the problem of most concern to people with osteoarthritis, is likely to be significantly heightened by the presence of excessive anxiety as observed early on by Lunghi et al. [7].
To this end, the author reports data embedded in the Academic Search Complete, PubMed, Scopus, Web of Science, Science Citation Index, and PsychInfo data bases using the key words, anxiety and osteoarthritis. Only English language peer reviewed publications were deemed acceptable and all selected papers had to focus on osteoarthritis patients, rather than other forms of rheumatic disease. The key findings were categorized into three key topics: the clinical syndromes of anxiety and osteoarthritis, the evidence connecting anxiety and osteoarthritis, and the implications of the presence of preexisting and/or state anxiety on the pain experienced by the adult diagnosed as having osteoarthritis. No meta-analyses were conducted due to the limited number of publications in this realm, and the mixed samples in most studies that address anxiety in the context of joint replacement surgery. However, all forms of reports were examined, provided they discussed osteoarthritis and some aspect of anxiety, and all types of osteoarthritis were considered. That is, the narrative review presented here was constituted by information deemed relevant to the key topics of interest, especially the extent of anxiety symptoms and their impact on pain among patients with osteoarthritis of any joint.
Results
Over the course of time, when utilizing the key words anxiety and osteoarthritis, the numbers of studies located in: Academic Search Complete were 123, PsychInfo had 127 articles listed, Science Citation Index cited 307 items, Web of Science listed 340 items, Scopus listed 740 items, and numbers in PubMed as of May 30, 2015 were 316. Types of studies included: cross-sectional clinical studies, presurgical, post-surgical, treatment, and rehabilitation studies. Joints studied included the hip, knee, hand, and temporomandibular joints. Instruments used to assess anxiety were the Hospital Anxiety and Depression Scale, the State-Trait Anxiety Inventory, the Mental Health Inventory, the Beck Anxiety Inventory, the Profile of Mood States Inventory, Jung Depression and Anxiety Inventory, and a categorical assessment of the presence or absence of anxiety on the patient's chart. Despite quite large number of possible sources of information, many articles accessed were not related to present topic in any way.
Prevalence of Anxiety in Adults with Osteoarthritis
In terms of the prevalence of anxiety among cases with osteoarthritis, a recent observational study by Castano et al. [8] indicated almost 25% of 1258 cases of patients in a primary care setting who had a diagnosis of osteoarthritis, also reported anxiety as a comorbid condition. In an earlier study, Axford et al. [9] found that among 54 patients with osteoarthritis, the majority of whom were women, the prevalence of clinically significant anxiety and/or depression was 40.7%. Marks [10] showed approximately nine percent (92 cases) of 1000 disabled hip osteoarthritis cases awaiting surgery had a prior mental health disorder, and among these patients, 5.5% (44 cases) reported trait anxiety histories, alone or in combination with trait depression. Among the 112 cases reporting either the presence of trait and/or state anxiety, nine cases reported both of these conditions, and a further nine with depression histories reported state anxiety. However, most of the 90 cases experiencing state anxiety had no prior anxiety history. According to Wesseling et al. [11] the presence of self-reported comorbidities, very prevalent among people with osteoarthritis heightens the chances of mental health issues such as anxiety. There are however, very few distinct reports on this topic. Most studies dealing with osteoarthritis either do not focus on mental health issues at all, or focus on mental health in general, depression specifically, fear, and centrally mediated symptoms. Those that have assessed anxiety prevalence in an osteoarthritic sample commonly used the data to predict outcomes or to assess associations with other variables, rather than to examine epidemiological trends. In these studies, anxiety served as predictor variable to ascertain its relevance in regards to disease outcomes, such as the degree of wellbeing and pain.
Relationship of Anxiety and Osteoarthritis Pain
Studies examining the influence of anxiety on the pain experienced by adults with osteoarthritis have generally found a positive correlation, regardless of study design or sample, or anxiety instrument used. For example, in support of the findings by Marks [10] who noted higher pain scores among cases with trait anxiety than those with no such history, Summers et al. [12] who examined cases of primary hip or knee osteoarthritis using outpatient department computer lists showed higher levels of state anxiety were significantly correlated with higher pain scores on all dimensions of the McGill Pain Questionnaire, except the evaluation dimension. In addition, high levels of trait anxiety were significantly associated with higher levels of affective pain and pain intensity scores. State anxiety was also significantly and positively correlated with all measures on the Sickness Impact Profile Inventory, and high levels of trait anxiety were associated with greater functional impairment on several of the Sickness Impact Profile subscales, and the overall score. This research was consistent with findings by Salaffi et al. [13] who examined the relationship between disability and psychological variables of anxiety and depression among 61 women with symptomatic knee osteoarthritis. Using an anxiety inventory, and a pain and disability index, they found disability and pain correlated with the degree of psychological involvement.
Similarly, a more recent paper that focused on psychological factors and their relation to osteoarthritis pain in a sample of 266 cases with hip and/or knee osteoarthritis, revealed a strong association between worsened measures of mental health and pain and risk of pain flares [14]. This finding was consistent with work by Creamer et al. [15]. This group examined the relationship of anxiety and depression among cases with knee osteoarthritis and found trait anxiety as assessed using the Speilberger State Trait Anxiety Inventory was associated with self-reported disability as measured using the Western Ontario Measurement Assessment tool.
While Creamer et al. [15] felt it was unclear from their cross-sectional study whether anxiety raises the risk of subsequent disability or whether disability itself is the reason why subjects become more anxious, pain and fear can clearly trigger the onset of anxiety or increase the prevailing of any comorbid anxiety. In this regard, Rolfson et al. [16] found patients with arthritis undergoing surgery who were less anxious also had less pain and were more satisfied with their surgical procedures and its outcome than those with higher anxiety levels. Similarly, although the population studied was not clearly defined, Badura-Brzoza et al. [17] who conducted a longitudinal investigation concerning the relation between some psychological and psychiatric factors and their influence on health-related quality of life in 102 patients after total hip replacement, found trait anxiety was significantly associated with postoperative mental as well as physical performance.
Likewise, Smith and Zautra [18] who examined the effects of anxiety on pain in women with osteoarthritis and rheumatoid arthritis found anxiety was related to elevations in current and forthcoming pain estimates, suggesting anxiety is important in explaining the progression of the disease. In particular, when studying the differential effects of depression and anxiety on pain, it was noted that the effects were nearly twice as large for anxiety compared to depression, suggesting the mechanism of action is unique.
These data were further substantiated by Axford et al. [9] who examined the interrelationships between the severity of osteoarthritis, pain, disability, anxiety and depression, using the Hospital Anxiety and Depression Scale (HADS), along with a structured clinical interview. Among the 54 patients studied, this group found pain correlated with the prevailing anxiety and depression scores and disability was greater in patients with a combined depression and anxiety history. More recently Sinikallio et al. [19], who examined cases with knee osteoarthritis found elevated anxiety was associated with pain, and that the osteoarthritis cases reported high levels of anxiety.
Clinical Implications
As outlined above, sufficient past and emerging evidence supports the view that anxiety may prevail in cases with osteoarthritis and that its presence may heighten pain levels. Pain in turn, may invoke anxiety, and increased fear, and a spiral of adverse functional outcomes. The psychological wellbeing of the osteoarthritis patient, in turn, has a strong bearing on the pain experience, as well as on the disease process, including its management, and outcomes. Not surprisingly, Davis et al. [20] who examined the associations of various health indicators and the psychological well-being of adults with and without radiographic knee osteoarthritis found self-reported knee pain correlated significantly with the presence of psychological distress, rather than visible joint destruction. Similarly Van Baar et al. [21] found that after controlling for other characteristics, the psychological characteristics of patients with osteoarthritis, such as anxiety contributed as much as the more traditional kinesiological measures to the patient's disability. Not unexpectedly, a related prospective study by Dieppe et al. [22] found adults with osteoarthritis examined over an eight year period generally had a poor outcome with high levels of physical disability, as well as anxiety, especially if they had knee osteoarthritis. As shown in Table 1, the collective evidence over the past 15 years shows anxiety when assessed in the context of osteoarthritis, is a significant mediator or moderator of disease presentation and outcomes, regardless of instrument used to assess anxiety.
![]()
Table 1: of key findings linking anxiety to osteoarthritis outcomes over the past 15 years.
View Table 1
These data clearly stress the importance of not only examining the physical status of adults with osteoarthritis in routine clinical settings, but that primary care providers should go beyond their usual medical history to identify and diagnose the presence of psychological symptoms such as anxiety especially among their osteoarthritis patients in pain [23]. Similar assessments of the patient's needs and characteristics conducted in the context of the surgical setting, followed by tailored and targeted interventions with follow-up visits to re-examine levels of anxiety would also be highly desirable as outlined by Montin et al. [24]. Those with trait anxiety histories who are more likely to experience state anxiety [24], those who are overweight, those who exhibit excessively high anxiety levels [25], as well as those using narcotics might be specifically targeted.
Indeed, it seems imperative to do this for two reasons. First, because research shows a high proportion of adults with osteoarthritis do suffer from one or more forms of anxiety and that those who do are more likely to experience worse outcomes than those who are not anxious, as well as higher current and future pain levels [18,24,26]. Second, pre-operative state anxiety, which is associated with post-operative state anxiety is a significant predictor of pain among patients undergoing knee or hip replacements [27], and those who exhibit state anxiety are also likely to recover more slowly after surgery in the absence of intervention. As argued by Summers et al. [11] anxiety in any form is likely to have a highly negative impact on the adult with osteoarthritis, especially because anxiety may reduce pain tolerance, thus contributing to an ongoing cycle of inactivity and further pain.
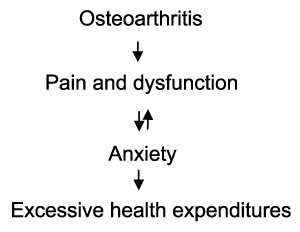
Anxiety and depression can also co-exist among adults with osteoarthritis and this could have an even greater influence on their ability to function physically than those with only one of these conditions, as identified by Axford et al. [9]. This link between anxiety, pain, and disability in people with osteoarthritis, which was also observed by Marks [28] in almost 9.5% of end-stage hip osteoarthritis cases suggests ample numbers of adults with disabling osteoarthritis may have mood and/or anxiety disorder histories that may often go undetected or overlooked in the treatment schedule being offered. An equal number may exhibit prevailing symptoms of emotional distress that may occur simultaneously or independently, either before or after surgery, or both, as well, and this can magnify pre-operative osteoarthritis disability and slow the post-operative recovery process [29]. Indeed, even though surgery for osteoarthritis is usually successful, it has been observed that even the presence of moderate trait anxiety can significantly impair the hip osteoarthritis surgical candidate's health quality of life both before, as well as after surgery [24], even though this is often believed to return the patient to optimal function. The cumulative effect of anxiety on osteoarthritis outcomes is conceptualized in Figure 1.
.
Figure 1: Schematic representation of problems heightened by anxiety among cases with osteoarthritis.
View Figure 1
Discussion
Although anxiety is clearly a possible comorbid condition accompanying osteoarthritis, and osteoarthritis itself can produce feelings of anxiety, unfortunately, as Memel [30] argued more than 10 years ago, general practitioners and other health providers have commonly lacked knowledge about either the importance of and/or the need to assess and treat the presence of anxiety in their osteoarthritis patients. This need to enhance screening efforts and foster optimal psychological health among cases with osteoarthritis is becoming increasingly clear however, as outlined in table 1 and figure 1.
Additionally, data by Vrizekolk et al. [31] provide further support for the importance of examining and diagnosing the presence of an anxiety related syndrome among cases with osteoarthritis, as well as among the general primary care population of adults. This group, who examined the psychological health status of patients with a variety of rheumatic conditions including osteoarthritis, found 64 percent of the sample met criteria for psychological distress at baseline. Although treatment improved this, 69 percent still experienced elevated distress levels and maladaptive illness cognitions after rehabilitation. These data are not surprising given findings that clearly show adults with trait anxiety are likely to experience worse outcomes than those who are not anxious, as well as higher pain levels, poorer coping behaviors, lower levels of physical activity participation, lower levels of social support, and poor sleep patterns, which in turn, could increase their pain and disablement experience adversely [24,26].
Moreover, since distinctive anxiety disorder subtypes prevail among adults with osteoarthritis, the specific type of anxiety disorder may contribute differentially or incrementally to the overall health related situation, plus the extent and rate of recovery.
Conclusion
Anxiety is a serious health condition that may impact the extent of a chronic medical condition [32], as well as life quality and the ability to function optimally. Similarly, osteoarthritis, a progressive joint disease associated with pain and disability among aging adults [33,34] has been linked to poor health outcomes and excessive usage of health resources. Commonly described as a physical problem, premorbid or state-related affective comorbid conditions such as anxiety, which significantly increases the progression of disability among older adults [35] may similarly influence osteoarthritis disease outcomes adversely. In particular, anxiety is commonly associated with poor adherence to self-care regimens and increased symptom burden. These factors can undoubtedly provoke or exacerbate osteoarthritis progression as suggested by findings of Katon et al. [32]. In addition, those with an anxiety disorder histories appear to experience a lower life quality [34], higher rates of pain and disability [9], and a lower ability to recover rapidly after joint replacement surgery when compared to their non-affected counterparts. Consequently, although often neglected in the context of primary care, an increasing body of emerging data stresses the need for routine psychological assessments alongside those commonly conducted for adults with osteoarthritis [36], followed by prompt appropriate treatment, as required.
Yet, in the case of osteoarthritis, it is more common than not for practitioners to focus on the physical aspects of the disease and its medical management rather than on its psychological correlates, and thus no efforts may be forthcoming to implement anxiety reducing treatments that could positively affect functional outcomes later on. This specific situation may need to be remediated at the training level because it may be that primary care providers are unaware of the current research in this area showing psychosocial factors such as anxiety, which can predate the disease or can result from the condition, can determine the extent of the disability that arises over time. They may also be unaware of the methods of assessing anxiety clinically, and of the diverse modes of intervention that can alleviate anxiety. They may also assume that the level of anxiety that may prevail in cases with osteoarthritis of one or more joints is simply to be expected. Similarly, adults with osteoarthritis may be reticent to express their fears, because they believe this is a physical condition, thus remaining undiagnosed and untreated. As outlined by Abrams et al. [37] and Kim et al. [38], because the presence of anxiety is an important predictor of overall well-being, psychometric tests should be routinely applied, and those at risk should be treated accordingly, regardless of clinical or surgical setting [9].
The identification and accurate diagnosis of the presence of anxiety, plus the timely implementation of appropriate interventions to alleviate or minimize anxiety, might not only improve upon current health related outcomes, but might also serve to lower health service utilization and costs associated with the overall management of progressively disabling osteoarthritis. Moreover, timely intervention that maximizes function might also reduce symptoms of pain that independently contributes to osteoarthritis disability. As well, the need for joint replacement surgery may be reduced or delayed by incorporating effective behavioral and psychological approaches into conservative treatment plans [36,39]. Finally, people with advanced osteoarthritis may benefit from joint replacement surgery to a greater extent than those treated solely in the biomedical model-if at the time of hospital referral - those with anxiety histories and those who express pre-surgical anxiety are identified, and precautions are taken to offset these risks as discussed by Giraudet-Le Quintrec et al. [40].
In the interim, given that anxiety is commonly associated with chronic physical conditions such as osteoarthritis [27], and that anxiety may contribute to pain, pain-related fears and negative functional outcomes [41], plus low life quality [42], Hill et al. [42] emphasized the need to recognize as well as address the significant additional negative impact anxiety can render on the patients' physical well being. In addition, Dorr and Chao [43] found that the pre-surgical emotional state of the patient undergoing joint replacement surgery affected their feelings of satisfaction after surgery, as did Perruccio et al. [44] and advocated for appropriate pre-operative education to allay any unwarranted negative impact. Dorr and Chao [43] also stressed the need for surgeons to understand the expectations of the patient, and to direct them to realistic goals, in order to allow patients to exceed their expectations.
To offset excess state or situational anxiety and/or distress in the surgical setting educational strategies [45] that can impact both conservative, as well as operative treatment outcomes and reduce health expenditures [46], and fears that impair life quality, physical function, pain, and sleep [47] can be helpful.
To this end, more research conducted on patients with different forms of osteoarthritis is indicated as the evidence for the impact of anxiety on pain and postoperative osteoarthritis outcomes is less than convincing [48-52]. More concerted efforts are also needed to uncover who is likely to be most affected [53], the patient's views about their apprehensions [54], the effects of anxiety on surgical recovery processes [55], and the types of anxiety that most influence key features of the condition [56-63]. A greater ability to minimize pain experienced as a result of osteoarthritis pathology is also indicated at all times, to reduce the possibility of fostering reactive anxiety states and their adverse effects on the existing disease process and its functional outcomes. As well, training clinicians and support staff to recognize and diagnose anxiety disorders, and to utilize valid instruments for assessing anxiety is very crucial to enabling them to better tailor their treatments and evaluate these over the course of time in light of their diagnoses. The use of both pharmacologic as well as non-pharmacologic strategies that can successfully target the mechanisms underlying the prevailing anxiety problem is strongly indicated as well [18].
As outlined by Hill et al. [42] and Perrucio et al. [44], optimal mental well-being is critical for maximizing outcomes for people with osteoarthritis. In this respect, available treatment options for reducing anxiety include the use of video information [45], serotonin-reuptake inhibitors [23], benzodiazepines applied in therapeutic doses, pre-operative education [40], guided imagery [24], anxiety management [27], social rehabilitation [29], and Cognitive Behavioral Therapy [47]. Emotional support [63] interventions designed to reduce psychological distress prior to surgery [64,65], holding frank discussions with patients [66], applying music during surgery [67], and standardizing both routine [68] and pre-operative screening procedures for anxiety [69] may be helpful as well.
In all cases, the mode of intervention selected to minimize anxiety should take into account the diagnostic category of anxiety, as trait anxiety is not the same as the experience of transitory or state anxiety, which can fluctuate [63]. In addition, personal factors must be taken into consideration. Based on the best available evidence, those with trait anxiety histories, as well as those with depression histories, and multiple comorbid conditions including obesity should be targeted preferentially, the optimal timing for effective support programs should be examined empirically, followed by relative program effectiveness [63].
References
-
Fava GA, Porcelli P, Rafanelli C, Mangelli L, Grandi S (2010) The spectrum of anxiety disorders in the medically ill. J Clin Psychiatry 71: 910-914.
-
Sareen J, Jacobi F, Cox BJ, Belik SL, Clara I, et al. (2006) Disability and poor quality of life associated with comorbid anxiety disorders and physical conditions. Arch Intern Med 166: 2109-2116.
-
Scott KM, Bruffaerts R, Tsang A, Ormel J, Alonso J, et al. (2007) Depression-anxiety relationships with chronic physical conditions: results from the World Mental Health Surveys. J Affect Disord 103: 113-120.
-
Burns MN, Siddique J, Fokuo JK, Mohr DC (2010) Comorbid anxiety disorders and treatment of depression in people with multiple sclerosis. Rehabil Psychol 55: 255-262.
-
Paukert AL, Pettit JW, Kunik ME, Wilson N, Novy DM, et al. (2010) The roles of social support and self-efficacy in physical health's impact on depressive and anxiety symptoms in older adults. J Clin Psychol Med Settings 17: 387-400.
-
Murphy LB, Sacks JJ, Brady TJ, Hootman JM, Chapman DP (2012) Anxiety and depression among US adults with arthritis: prevalence and correlates. Arthritis Care Res 64: 968-976..
-
Lunghi ME, Miller PM, McQuillan WM (1978) Psycho-social factors in osteoarthritis of the hip. J Psychosom Res 22: 57-63.
-
Casta�o Carou A, Pita Fern�ndez S2, P�rtega D�az S3, de Toro Santos FJ4; Grupo de estudio EVAL�A (2015) Clinical profile, level of affection and therapeutic management of patients with osteoarthritis in primary care: The Spanish multicenter study EVAL�A. Reumatol Clin .
-
Axford J, Butt A, Heron C, Hammond J, Morgan J, et al. (2010) Prevalence of anxiety and depression in osteoarthritis: use of the Hospital Anxiety and Depression Scale as a screening tool. Clin Rheumatol 29: 1277-1283.
-
Marks R (2009) Comorbid depression and anxiety impact hip osteoarthritis disability. Disabil Health J 2: 27-35.
-
Wesseling J, Welsing PM, Bierma-Zeinstra SM, Dekker J, Gorter KJ,et al. (2013) Impact of self-reported comorbidity on physical and mental health status in early symptomatic osteoarthritis: the CHECK (Cohort Hip and Cohort Knee) study. Rheumatol (Oxford) 52: 180-188.
-
Summers MN, Haley WE, Reveille JD, Alarc�n GS (1988) Radiographic assessment and psychologic variables as predictors of pain and functional impairment in osteoarthritis of the knee or hip. Arthritis Rheum 31: 204-209.
-
Salaffi F, Cavalieri F, Nolli M, Ferraccioli G (1991) Analysis of disability in knee osteoarthritis. Relationship with age and psychological variables but not with radiographic score. J Rheumatol 18: 1581-1586.
-
Wise BL, Niu J, Zhang Y, Wang N, Jordan JM, et al. (2010) Psychological factors and their relation to osteoarthritis pain. Osteoarthritis Cartilage 18: 883-887.
-
Creamer P, Lethbridge-Cejku M, Hochberg MC (2000) Factors associated with functional impairment in symptomatic knee osteoarthritis. Rheumatology (Oxford) 39: 490-496.
-
Rolfson O, Dahlberg LE, Nilsson JA, Malchau H, Garellick G (2009) Variables determining outcome in total hip replacement surgery. J Bone Joint Surg Br 91: 157-161.
-
Badura-Brzoza K, Zajac P, Brzoza Z, Kasperska-Zajac A, Matysiakiewicz J, et al. (2009) Psychological and psychiatric factors related to health-related quality of life after total hip replacement - preliminary report. Eur Psychiatry 24: 119-124.
-
Smith BW, Zautra AJ (2008) The effects of anxiety and depression on weekly pain in women with arthritis. Pain 138: 354-361.
-
Sinikallio SH, Helminen EE, Valjakka AL, V�is�nen-Rouvali RH, Arokoski JP (2014) Multiple psychological factors are associated with poorer functioning in a sample of community-dwelling knee osteoarthritis patients. J Clin Rheumatol 20: 261-267.
-
Davis MA, Ettinger WH, Neuhaus JM, Barclay JD, Segal MR (1992) Correlates of knee pain among US adults with and without radiographic knee osteoarthritis. J Rheumatol 19: 1943-1949.
-
van Baar ME, Dekker J, Lemmens JA, Oostendorp RA, Bijlsma JW (1998) Pain and disability in patients with osteoarthritis of hip or knee: the relationship with articular, kinesiological, and psychological characteristics. J Rheumatol 25: 125-133.
-
Dieppe P, Cushnaghan J, Tucker M, Browning S, Shepstone L (2000) The Bristol 'OA500 study': progression and impact of the disease after 8 years. Osteoarthritis Cartilage 8: 63-68.
-
Wu LR, Parkerson GR Jr, Doraiswamy PM (2002) Health perception, pain, and disability as correlates of anxiety and depression symptoms in primary care patients. J Am Board Fam Pract 15: 183-190.
-
Montin L, Leino-Kilpi H, Katajisto J, Lepist� J, Kettunen J, et al. (2007) Anxiety and health-related quality of life of patients undergoing total hip arthroplasty for osteoarthritis. Chronic Illn 3: 219-227.
-
Daltroy LH, Morlino CI, Eaton HM, Poss R, Liang MH (1998) Preoperative education for total hip and knee replacement patients. Arthritis Care Res 11: 469-478.
-
Dekker J, van Dijk GM, Veenhof C (2009) Risk factors for functional decline in osteoarthritis of the hip or knee. Curr Opin Rheumatol 21: 520-524.
-
Feeney SL (2004) The relationship between pain and negative affect in older adults: anxiety as a predictor of pain. J Anxiety Disord 18: 733-744.
-
28. Marks R, Allegrante JP (2002) Comorbid disease profiles of adults with end-stage hip osteoarthritis. Med Sci Monit 8: CR305-309.
-
Badura-Brzoza K, Zajac P, Kasperska-Zajac A, Brzoza Z, Matysiakiewicz J, et al. (2008) Anxiety and depression and their influence on the quality of life after total hip replacement: preliminary report. Int J Psychiatry Clin Pract 12: 280-284.
-
Memel DS, Kirwan JR, Sharp DJ, Hehir M (2000) General practitioners miss disability and anxiety as well as depression in their patients with osteoarthritis. Br J Gen Pract 50: 645-648.
-
Vriezekolk J, Eijsbouts A, Evers A, Stenger A, Van Den Hoogen F, et al. (2010) Poor psychological health status among patients with inflammatory rheumatic diseases and osteoarthritis in multidisciplinary rehabilitation: need for a routine psychological assessment. Disabil Rehabil 32: 836-844.
-
Katon W, Lin EH, Kroenke K (2007) The association of depression and anxiety with medical symptom burden in patients with chronic medical illness. Gen Hosp Psychiatry 29: 147-155.
-
Hochberg MC, Kasper J, Williamson J, Skinner A, Fried LP (1995) The contribution of osteoarthritis to disability: preliminary data from the Women's Health and Aging Study. J Rheumatol Suppl 43: 16-18.
-
Hopman-Rock M, Kraaimaat FW, Bijlsma JW (1997) Quality of life in elderly subjects with pain in the hip or knee. Qual Life Res 6: 67-76.
-
Brenes GA, Guralnik JM, Williamson JD, Fried LP, Simpson C, et al. (2005) The influence of anxiety on the progression of disability. J Am Geriatr Soc 53: 34-39.
-
Keefe FJ, Smith SJ, Buffington AL, Gibson J, Studts JL, et al. (2002) Recent advances and future directions in the biopsychosocial assessment and treatment of arthritis. J Consult Clin Psychol 70: 640-655.
-
Abrams TE, Vaughan-Sarrazin M, Rosenthal GE (2010) Influence of psychiatric comorbidity on surgical mortality. Arch Surg 145: 947-953.
-
Kim SH, Kang S, Kim YM, Kim BG, Seong SJ, et al. (2010) Prevalence and predictors of anxiety and depression among cervical cancer survivors in Korea. Int J Gynecol Cancer 20: 1017-1024.
-
Salmon P, Hall GM, Peerbhoy D (2001) Influence of the emotional response to surgery on functional recovery during 6 months after hip arthroplasty. J Behav Med 24: 489-502.
-
Giraudet-Le Quintrec JS, Coste J, Vastel L, Pacault V, Jeanne L, et al. (2003) Positive effect of patient education for hip surgery: a randomized trial. Clin Orthop Relat Res : 112-120.
-
Heuts PH, Vlaeyen JW, Roelofs J, de Bie RA, Aretz K, et al. (2004) Pain-related fear and daily functioning in patients with osteoarthritis. Pain 110: 228-235.
-
Hill CL, Gill T, Taylor AW, Daly A, Grande ED, et al. (2007) Psychological factors and quality of life in arthritis: a population-based study. Clin Rheumatol 26: 1049-1054.
-
Dorr LD, Chao L (2007) The emotional state of the patient after total hip and knee arthroplasty. Clin Orthop Relat Res 463: 7-12.
-
Perruccio AV, Davis AM, Hogg-Johnson S, Badley EM (2011) Importance of self-rated health and mental well-being in predicting health outcomes following total joint replacement surgery for osteoarthritis. Arthritis Care Res (Hoboken) 63: 973-981.
-
Ayral X, Gicquere C, Duhalde A, Boucheny D, Dougados M (2002) Effects of video information on preoperative anxiety level and tolerability of joint lavage in knee osteoarthritis. Arthritis Rheum 47: 380-382.
-
Agarwal P, Sambamoorthi U (2015) Healthcare Expenditures Associated with Depression Among Individuals with Osteoarthritis: Post-Regression Linear Decomposition Approach. J Gen Intern Med .
-
Davis L, Barlow DH, Smith L (2010) Comorbidity and the treatment of principal anxiety disorders in a naturalistic sample. Behav Ther 41: 296-305.
-
Ozcetin A, Ataoglu S, Kocer E, Yazici S, Yildiz O, et al. (2007) Effects of depression and anxiety on quality of life of patients with rheumatoid arthritis, knee osteoarthritis and fibromyalgia syndrome. West Indian Med J 56: 122-129.
-
Scopaz KA, Piva SR, Wisniewski S, Fitzgerald GK (2009) Relationships of fear, anxiety, and depression with physical function in patients with knee osteoarthritis. Arch Phys Med Rehabil 90: 1866-1873.
-
Tallon D, Chard J, Dieppe P (2000) Exploring the priorities of patients with osteoarthritis of the knee. Arthritis Care Res 13: 312-319.
-
Chen CJ, McHugh G, Campbell M, Luker K (2014) Subjective and Objective Sleep Quality in Individuals with Osteoarthritis in Taiwan. Musculoskeletal Care .
-
Hern�ndez C, D�az-Heredia J, Berraquero ML, Crespo P, Loza E, et al. (2015) Pre-operative Predictive Factors of Post-operative Pain in Patients With Hip or Knee Arthroplasty: A Systematic Review. Reumatol Clin .
-
Jacobs CA, Christensen CP, Karthikeyan T (2015) Chronic non-orthopedic conditions more common in patients with less severe degenerative changes that have elected to undergo total knee arthroplasty. J Arthroplasty 30: 1146-1149.
-
Fujita K, Makimoto K, Hotokebuchi T (2006) Qualitative study of osteoarthritis patients' experience before and after total hip arthroplasty in Japan. Nurs Health Sci 8: 81-87.
-
Hanusch BC, O'Connor DB, Ions P, Scott A, Gregg PJ (2014) Effects of psychological distress and perceptions of illness on recovery from total knee replacement. Bone Joint J 96-96B: 210-6.
-
Judge A, Arden NK, Cooper C, Kassim Javaid M, Carr AJ, et al. (2012) Predictors of outcomes of total knee replacement surgery. Rheumatology (Oxford) 51: 1804-1813.
-
Duivenvoorden T, Vissers MM, Verhaar JA, Busschbach JJ, Gosens T, et al. (2013) Anxiety and depressive symptoms before and after total hip and knee arthroplasty: a prospective multicentre study. Osteoarthritis Cartilage 21: 1834-1840.
-
Vissers MM, Bussmann JB, Verhaar JA, Busschbach JJ, Bierma-Zeinstra SM, et al. (2012) Psychological factors affecting the outcome of total hip and knee arthroplasty: a systematic review. Semin Arthritis Rheum 41: 576-588.
-
Riddle DL, Wade JB, Jiranek WA, Kong X (2010) Preoperative pain catastrophizing predicts pain outcome after knee arthroplasty. Clin Orthop Relat Res 468: 798-806.
-
Vissers MM, de Groot IB, Reijman M, Bussmann JB, Stam HJ, et al. (2010) Functional capacity and actual daily activity do not contribute to patient satisfaction after total knee arthroplasty. BMC Musculoskelet Disord 11: 121.
-
Liddle AD, Judge A, Pandit H, Murray DW (2014) Determinants of revision and functional outcome following unicompartmental knee replacement. Osteoarthritis Cartilage 22: 1241-1250.
-
Ali A, Sundberg M, Robertsson O, Dahlberg LE, Thorstensson CA, et al. (2014) Dissatisfied patients after total knee arthroplasty: a registry study involving 114 patients with 8-13 years of followup. Acta Orthop 85: 229-233.
-
Ayers DC, Franklin PD, Trief PM, Ploutz-Snyder R, Freund D (2004) Psychological attributes of preoperative total joint replacement patients: implications for optimal physical outcome. J Arthroplasty 19: 125-130.
-
Utrillas-Compaired A, De la Torre-Escuredo BJ, Tebar-Mart�nez AJ, As�nsolo-Del Barco � (2014) Does preoperative psychologic distress influence pain, function, and quality of life after TKA? Clin Orthop Relat Res 472: 2457-2465.
-
Hanusch BC, O'Connor DB, Ions P, Scott A, Gregg PJ (2014) Effects of psychological distress and perceptions of illness on recovery from total knee replacement. Bone Joint J 96-96B: 210-6.
-
McHugh GA, Campbell M, Luker KA (2013) Predictors of outcomes of recovery following total hip replacement surgery: A prospective study. Bone Joint Res 2: 248-254.
-
Ottaviani S, Bernard JL, Bardin T, Richette P (2012) Effect of music on anxiety and pain during joint lavage for knee osteoarthritis. Clin Rheumatol 31: 531-534.
-
Hodkinson B, Maheu E, Michon M, Carrat F, Berenbaum F (2012) Assessment and determinants of aesthetic discomfort in hand osteoarthritis. Ann Rheum Dis 71: 45-49.
-
Hirschmann MT, Testa E, Amsler F, Friederich NF (2013) The unhappy total knee arthroplasty (TKA) patient: higher WOMAC and lower KSS in depressed patients prior and after TKA. Knee Surg Sports Traumatol Arthrosc 21: 2405-2411.
-
Badel T, Lovko SK, Podoreski D, Pavcin IS, Kern J (2011) Anxiety, splint treatment and clinical characteristics of patients with osteoarthritis of temporomandibular joint and dental students--a pilot study. Med Glas (Zenica) 8: 60-63.





